The question of whether choosing organic over conventionally grown foods offers a tangible protective benefit against cancer, particularly concerning the effects of pesticide exposure, has become a focal point for health-conscious consumers and scientific inquiry. Emerging research suggests a complex relationship, with a substantial body of evidence linking pesticide exposure to an increased risk of cancer, though the precise impact of dietary choices remains a subject of ongoing investigation.
The Pervasive Presence of Pesticides and Their Link to Cancer
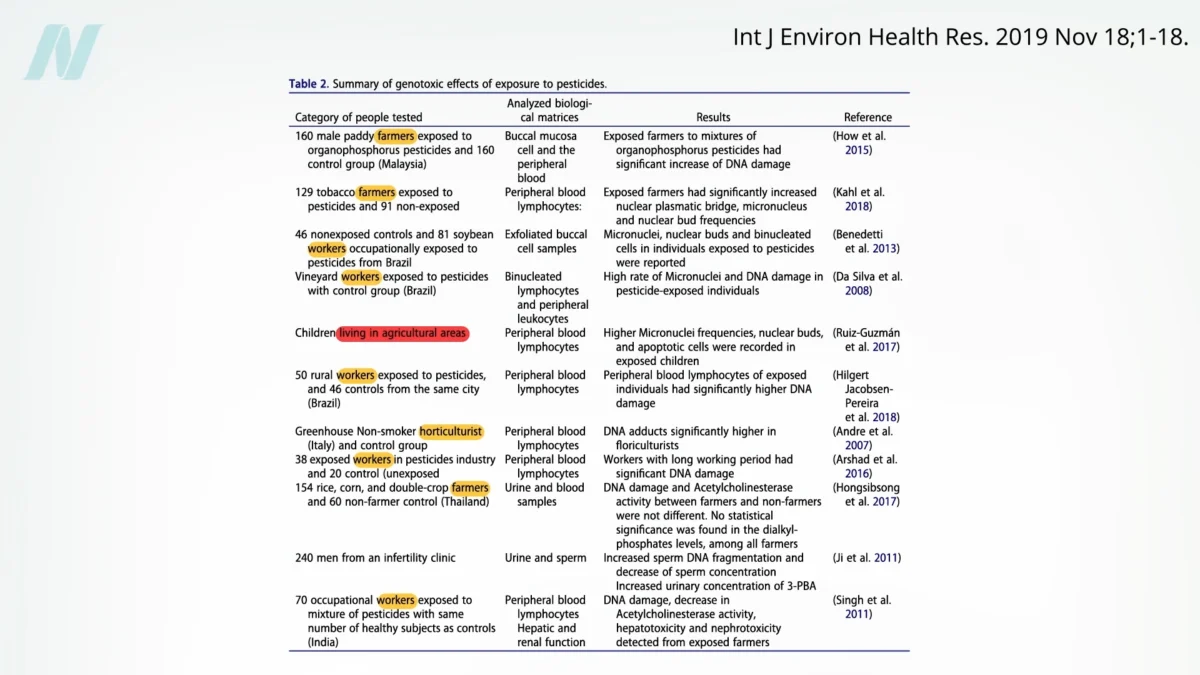
A comprehensive review of human exposure and toxicity of pesticides underscores the significant weight of evidence connecting pesticide exposure to cancer development. Researchers have concluded that the role of pesticides in the genesis of cancer "cannot be doubted." This strong assertion is largely built upon studies examining occupational exposure, such as that experienced by farmers and agricultural workers who handle these chemicals directly. Similarly, individuals residing in areas with high pesticide application rates or those working within the pesticide industry itself have shown increased susceptibility. These high-exposure scenarios provide compelling evidence of the potential for pesticides to induce DNA damage, a critical precursor to cancerous mutations.
While the evidence from occupational settings is substantial, its direct translation to the general population’s dietary exposure requires careful consideration. Non-occupational exposure, primarily through the consumption of food residues, has also been investigated. Some studies have identified a link between non-occupational pesticide exposure and DNA damage, specifically observing single- and double-stranded DNA fragmentation in the sperm of men with elevated pesticide levels in their bodies. However, it is important to note that some of these studies, such as one conducted in China, involved regions where average pesticide concentrations were found to be significantly higher than in many other parts of the world. This highlights the variability in exposure levels across different geographical and agricultural contexts.
Mechanisms of Pesticide Impact on Cancer Development
Beyond direct DNA damage, pesticides may also contribute to cancer development by compromising the body’s natural defense mechanisms. One crucial aspect of this involves the adverse effects on anticancer immunity. Natural Killer (NK) cells, a vital component of the innate immune system, act as a frontline defense against cancer cells and virus-infected cells. Research has demonstrated that exposure to pesticides can impair the function of these critical defender cells, diminishing their ability to effectively eliminate tumor cells.

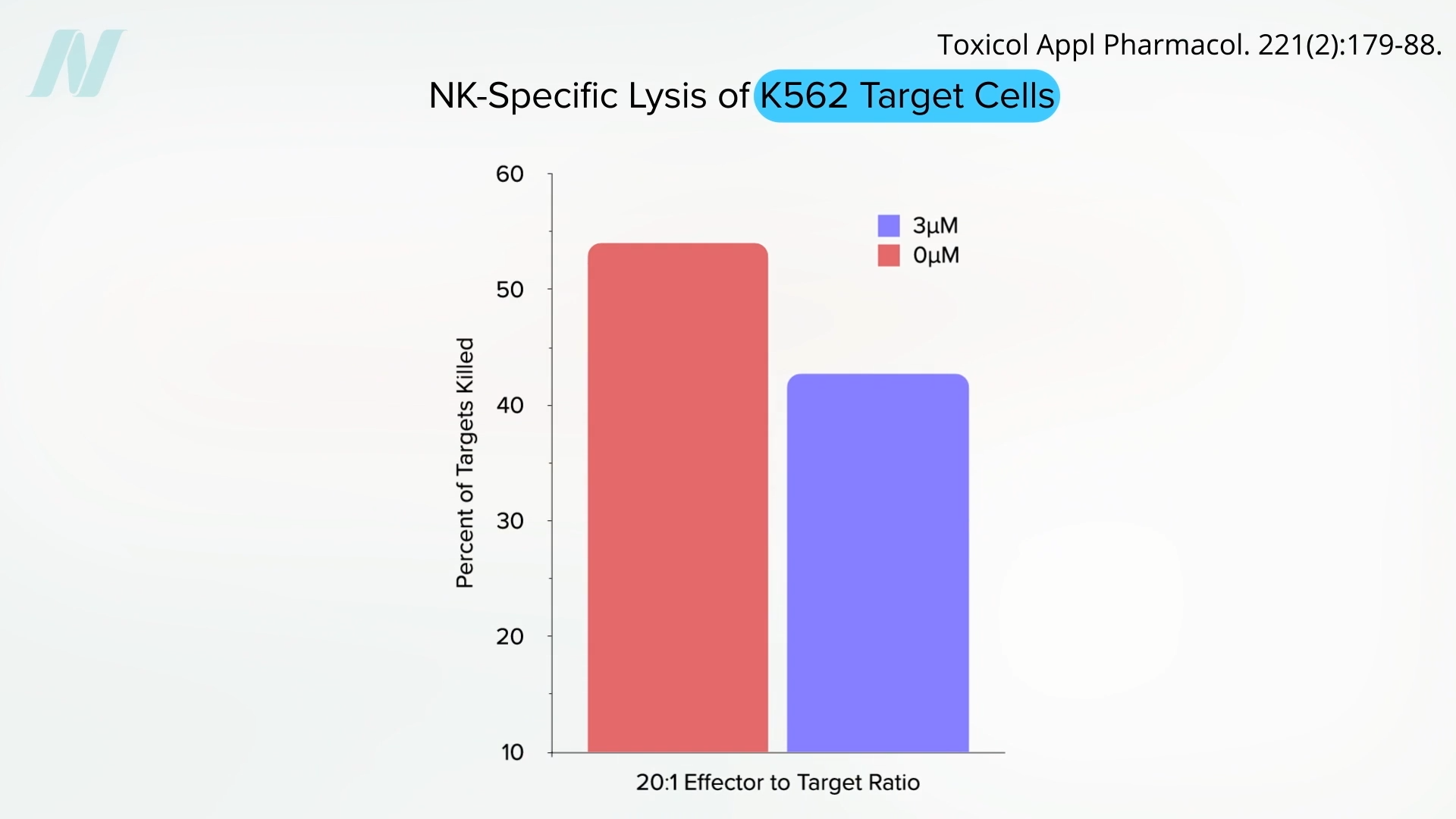
In laboratory settings, studies have illustrated this impact vividly. When NK cells are introduced to human leukemia cells in a petri dish without pesticide exposure, they exhibit a remarkable capacity to destroy a significant portion of the cancer cells. However, upon the addition of even a small amount of pesticide, the NK cells’ effectiveness is severely compromised, leading to a more favorable outcome for the cancer cells. This experimental evidence suggests a potential pathway through which pesticides could facilitate tumor growth by weakening the body’s immune surveillance.
The concentration of pesticides used in these experimental settings often reflects the maximum levels found in individuals actively involved in pesticide application. This raises a pertinent question: what is the impact of the lower, residual levels of pesticides found on conventionally grown produce, and is the choice to purchase organic foods a worthwhile investment for cancer prevention?
Pesticide Residues in the General Population and Dietary Shifts
Pesticide residues are remarkably widespread, with detectable levels found in the blood and urine of over 90% of the U.S. population, irrespective of their occupation or geographical location. This ubiquitous presence strongly suggests that dietary intake is a primary source of exposure for the general public. Crossover trials, where participants switch between consuming conventionally grown and organic foods, provide compelling evidence for this. These studies have demonstrated a rapid and reversible change in urinary concentrations of pesticide metabolites, akin to turning a light switch on and off, as individuals alter their dietary patterns. While this confirms the link between diet and pesticide metabolite levels, it does not definitively prove that these residues are causing harm at typical consumption levels.
The long-term health consequences of ingesting pesticide residues from conventionally grown foods remain an area requiring further elucidation. However, preliminary findings offer intriguing insights.
Investigating the Link Between Organic Food Consumption and Cancer Risk
A recent, large-scale study sought to address this knowledge gap by evaluating the association between the frequency of organic food consumption and cancer risk. This research, considered a significant advancement in its field, controlled for a comprehensive array of potential confounding factors. These included age, socioeconomic status, education level, body mass index, physical activity, meat consumption, and smoking habits. Even after accounting for these variables, individuals who reported consuming organic foods most frequently exhibited a notably lower risk of developing cancer, approximately 25% less than those who rarely or never chose organic options.

The study’s robustness lay in its meticulous control for numerous lifestyle and demographic factors that could influence cancer risk. For instance, researchers accounted for the possibility that organic food consumers might be younger, more affluent, more educated, leaner, more physically active, or less likely to smoke. Despite these adjustments, the observed reduction in cancer risk among frequent organic consumers persisted. Furthermore, the study considered dietary differences beyond organic versus conventional choices, such as overall fruit and vegetable intake or consumption of processed foods. The findings remained consistent: higher organic food consumption was associated with a significantly reduced risk of overall cancer. The researchers concluded that "Our results indicate that higher organic food consumption is associated with a reduction in the risk of overall cancer."
Earlier Studies and Specific Cancer Types
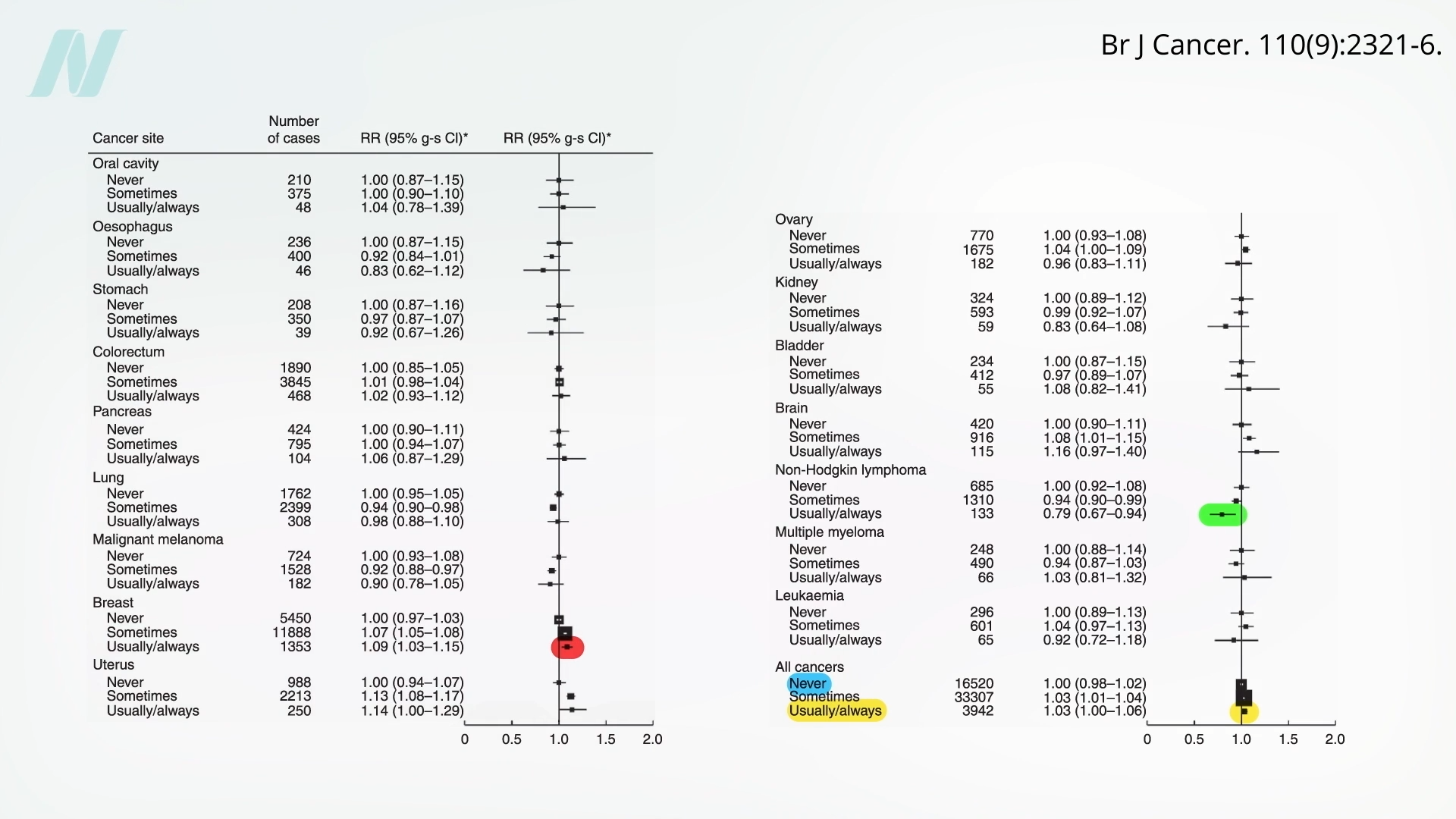
While the aforementioned study represented a sophisticated approach, earlier, larger investigations have also explored this association. One such comprehensive study found limited evidence for a decrease in the incidence of all cancers combined. However, it did identify a potential reduction in the risk of a specific type of blood cancer, non-Hodgkin lymphoma.
Data from this earlier research indicated no significant overall difference in cancer rates between individuals who never consumed organic foods and those who did so regularly. The only statistically significant findings were a lower risk of non-Hodgkin lymphoma and, intriguingly, an increased risk of breast cancer diagnoses among those who frequently chose organic options. The elevated breast cancer diagnosis rate has prompted speculation. One hypothesis suggests that women who prioritize organic foods may also be more diligent about participating in regular breast cancer screenings, potentially leading to earlier detection and diagnosis, rather than an actual increased incidence. However, definitive evidence to support this hypothesis is currently lacking.
Beyond Cancer: All-Cause Mortality and Pesticide-Type Compounds
Beyond the specific concern of cancer, the broader impact on all-cause mortality – the risk of dying prematurely from any cause – is of paramount importance. Research has indicated a significant association between higher blood levels of certain pesticide-type compounds and a shorter lifespan. For instance, elevated levels of beta-hexachlorocyclohexane, a persistent organochlorine pesticide, have been linked to a significantly reduced life expectancy.
Dietary Patterns and Pesticide Load: The Role of Animal Products
Understanding how to mitigate exposure to these harmful compounds is crucial. Historical studies have offered insights into dietary influences on pesticide levels. Decades ago, a study comparing a vegetarian mother and her non-vegetarian sister, both breastfeeding, revealed a notable difference in the levels of beta-hexachlorocyclohexane in their breast milk. The vegetarian sister exhibited approximately one-third lower levels of this pesticide compared to her omnivorous sibling. This finding is consistent with the understanding that chlorinated pesticides, including beta-hexachlorocyclohexane, are lipophilic (fat-soluble) and tend to accumulate in fatty tissues. Consequently, they are found most frequently in foods of animal origin, such as meat, dairy, and eggs.
More contemporary research has continued to explore the link between dietary patterns and pesticide-type compounds. While some recent studies may not have specifically focused on beta-hexachlorocyclohexane, they have examined other concerning chemicals like polychlorinated biphenyls (PCBs). These studies have also found associations between PCBs and increased mortality risk, with these toxins similarly prevalent in eggs, dairy products, and animal fats.
A study investigating PCB levels in individuals with different dietary habits found that vegans had "significantly less polluted" blood compared to omnivores in terms of a range of PCBs linked to increased mortality. However, it is noteworthy that vegans in this study did not exhibit lower levels of beta-hexachlorocyclohexane, suggesting that while a plant-based diet can reduce exposure to certain contaminants, it may not universally eliminate all pesticide-type compounds.
Weighing the Benefits: Produce Consumption and Potential Risks
The cumulative evidence suggests that if reducing exposure to pesticides and similar compounds is a health priority, decreasing the intake of animal products may be a prudent strategy. However, when it comes to fruits and vegetables, the prevailing scientific consensus leans towards the significant health benefits of consumption, likely outweighing potential risks from pesticide residues.
Concerns about pesticide residues on conventionally grown produce should not deter individuals from increasing their intake of fruits and vegetables. The nutritional advantages derived from consuming a wide variety of these foods are substantial and offer significant health benefits. In contrast, the potential lifelong damage from average pesticide exposure on fruits and vegetables has been estimated to reduce lifespan by only a few minutes, a negligible amount when compared to the profound positive impact of a diet rich in fruits and vegetables.
Therefore, the message is clear: maximizing the consumption of fruits and vegetables, regardless of whether they are conventionally grown or organic, is a critical step towards improving overall health and potentially reducing cancer risk. The decision to opt for organic produce may offer additional benefits in reducing pesticide exposure, but the fundamental act of eating more fruits and vegetables remains a cornerstone of a healthy lifestyle.

Doctor’s Note
Further exploration into the benefits and considerations of organic foods can be found in related posts and scientific literature. The ongoing research in this field aims to provide clearer guidance for consumers seeking to make informed choices for their health and well-being.


