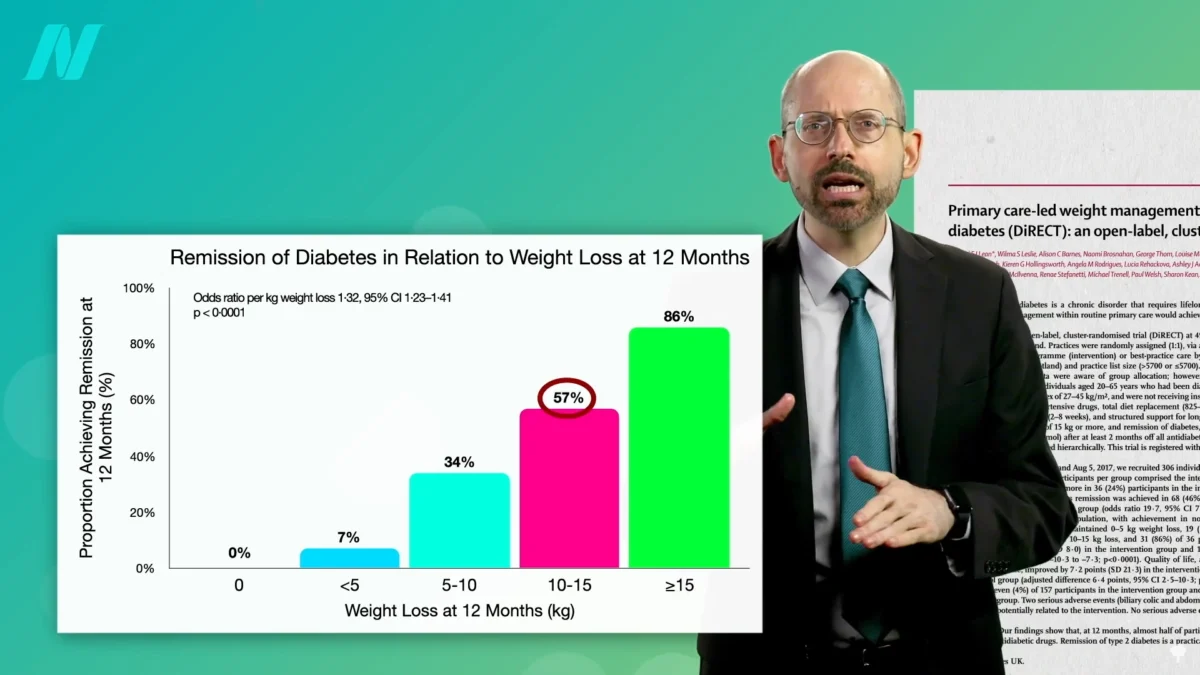
The escalating global health crisis of type 2 diabetes, a condition affecting over half a billion adults worldwide and projected to increase by 50% within a generation, is increasingly being understood not as an irreversible ailment, but as a reversible condition, particularly when addressed early through significant weight loss and sustained lifestyle modifications. Emerging scientific evidence suggests that achieving a 15% reduction in body weight can lead to remission in nearly 90% of individuals diagnosed with type 2 diabetes for less than four years. This remarkable finding offers a compelling alternative to traditional management strategies and even surpasses the remission rates seen with bariatric surgery in comparable patient groups.
The Historical Context of Diabetes Management: From Fasting to Fat Toxicity
The concept of managing diabetes through dietary restriction is not new; in fact, its roots stretch back over a century, with early proponents suggesting that fasting could rapidly halt the progression of the disease and eliminate its symptoms. Historical accounts from over a century ago indicated that fasting could lead to the swift disappearance of diabetes symptoms within days or weeks. While extreme starvation was acknowledged as ultimately detrimental, the underlying principle of significant caloric reduction and subsequent weight loss as a therapeutic tool has endured, albeit with evolving understanding and methodologies.
Early medical texts and practices reveal a long-standing association between diabetes and lifestyle, particularly diet and physical activity. In the early 20th century, type 2 diabetes was often characterized as a "disease of excess," predominantly afflicting those with sedentary lifestyles and access to abundant food. This perception, dating back to observations made in the early 1900s, suggested that individuals whose environments did not necessitate sustained physical exertion and who consumed more calories than they needed were more susceptible. This historical viewpoint underscores the preventable nature of the disease and hints at its potential treatability through dietary intervention.
The notion of "undereating" to combat the effects of overeating, a central theme in modern diabetes management, was remarkably proposed in ancient Ayurvedic texts approximately 2,000 years ago. These texts suggested rigorous physical activity, such as walking hundreds of miles, or severe dietary restrictions, even including consuming unconventional items, as potential remedies. While these ancient prescriptions are far removed from contemporary medical practice, they reflect an early recognition of the profound impact of lifestyle on diabetes.
Later, in 1797, Dr. John Rollo proposed a diet for diabetes that, while radical and even harmful by today’s standards, focused on severe caloric restriction. His regimen, which included rancid meat and emetics to induce vomiting, achieved temporary relief from diabetes symptoms by drastically reducing food intake. This approach, though lacking a scientific basis for safety and long-term efficacy, highlighted the direct correlation between reduced caloric consumption and symptom amelioration.

The siege of Paris during the Franco-Prussian War provided another historical glimpse into the effects of severe dietary restriction. During this period, individuals with diabetes experienced improvements in their condition due to widespread food scarcity, leading to the advice of "mangez le moins possible" – "eat as little as possible." This principle was later formalized into the Allen starvation treatment by Dr. Frederick M. Allen. Considered a significant advancement in diabetes care prior to the discovery of insulin, "The Allen Era" emphasized keeping patients underweight and restricting dietary fat as core principles for managing the disease. Dr. Allen observed that severe diabetes cases could clear up following "wasting conditions" like tuberculosis or cancer, prompting him to experiment with intentional caloric restriction. He found that even in severe diabetes, urinary sugar could be eliminated within ten days, though maintaining this remission upon resuming food intake proved challenging. His research indicated that consuming even small amounts of fat, such as butter or olive oil, could trigger a resurgence of diabetic symptoms.
Understanding Type 2 Diabetes as a Disease of Fat Toxicity
Modern scientific research has significantly advanced our understanding of type 2 diabetes, increasingly framing it as a condition rooted in "fat toxicity." Studies have demonstrated that infusing fat intravenously can lead to a rapid buildup of fat within muscle cells, observable in real-time using advanced MRI technology. This fat accumulation is accompanied by a corresponding increase in insulin resistance. Similar effects have been observed within hours of initiating a high-fat diet, and in some cases, even after a single day or a single meal.
The mechanism behind this is critical: acute dietary fat intake rapidly exacerbates insulin resistance in muscle tissues. When combined with excess caloric intake, this insulin resistance can trigger a cascade of metabolic disruptions. This includes the accumulation of fat in the liver, followed by fat deposition in the pancreas. Ultimately, this process can lead to the full manifestation of type 2 diabetes. Research now suggests that type 2 diabetes can be understood as a state characterized by excessive fat accumulation in the liver and pancreas, and importantly, this condition remains reversible for at least a decade in the majority of individuals.
The Efficacy of Weight Loss in Achieving Diabetes Remission
The pivotal role of weight loss in achieving remission from type 2 diabetes is supported by robust clinical data. Studies have shown that placing individuals on very low-calorie diets, such as 700 calories per day, can effectively mobilize fat from muscle cells. This process is directly correlated with a significant improvement in insulin sensitivity. As this low-calorie diet is sustained, the excess fat within the liver begins to decrease substantially. If the dietary intervention continues, the accumulated fat in the pancreas also reduces, paving the way for potential diabetes reversal.
Crucially, the degree of weight loss and the duration of the disease significantly influence the likelihood of achieving remission. Research indicates that individuals who have had type 2 diabetes for less than four years and achieve a 15% reduction in body weight have a nearly 90% chance of attaining non-diabetic blood sugar levels. This stands in stark contrast to those who have lived with the disease for longer periods; for individuals with diabetes exceeding eight years, the remission rate may drop to approximately 50%.
Comparative Effectiveness: Weight Loss Versus Bariatric Surgery
The effectiveness of lifestyle-induced weight loss in achieving diabetes remission is further highlighted when compared to bariatric surgery. Studies comparing the two interventions have revealed that patients undergoing bariatric surgery, even those experiencing substantial weight loss, often exhibit lower remission rates for type 2 diabetes. For instance, bariatric surgery patients who lose significant weight have reported remission rates of 62% and 26% in comparable groups, respectively, falling short of the remission rates achieved through lifestyle interventions. This data suggests that "your forks are better than surgeons’ knives" – emphasizing the power of dietary choices and lifestyle changes over surgical procedures for diabetes reversal.
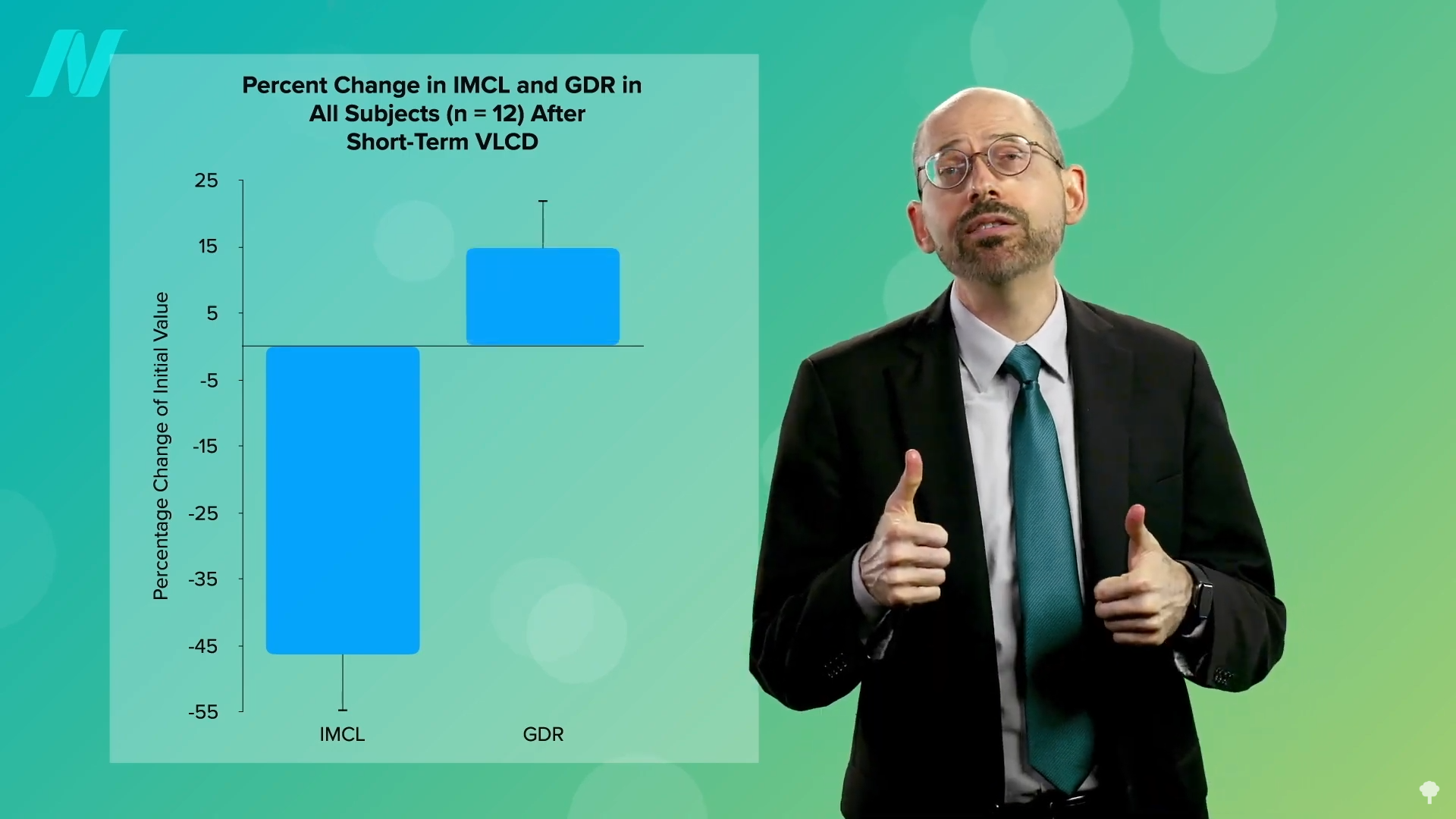
Further evidence supports the profound impact of sustained weight loss on diabetes reversal. A significant proportion of individuals diagnosed with type 2 diabetes for an average of three years can reverse their condition after losing approximately 30 pounds. This outcome underscores the principle that significant, sustained weight loss, achieved through dietary modification and lifestyle changes, is a powerful tool for regaining metabolic health.
The Importance of Sustained Lifestyle Change
While extended periods of physician-supervised, water-only fasting can indeed lead to significant weight loss and diabetes remission, the critical factor for long-term success is the maintenance of this weight loss. Scientific consensus and clinical experience have established a clear correlation: regaining lost weight often leads to the return of diabetes. This underscores the necessity of transitioning from short-term intensive interventions to sustainable, healthy dietary patterns and regular physical activity.
The Evolution of Diabetes Management: From Insulin to Holistic Care
The discovery of insulin in 1921 was a monumental breakthrough, hailed as "medicine’s greatest miracle." It was, and remains, literally life-saving for individuals with type 1 diabetes. However, for those with type 2 diabetes, insulin alone proved insufficient in preventing serious complications such as blindness, kidney failure, stroke, and amputations. This realization led pioneers in diabetes care, like Elliott Joslin, to re-emphasize the importance of self-discipline in diet and exercise, principles that were central to diabetes management in the pre-insulin era. His advocacy highlighted that while insulin provided a crucial therapeutic option, it did not negate the fundamental role of lifestyle in managing and potentially reversing type 2 diabetes.
The Path Forward: Embracing Lifestyle as Medicine
The understanding of type 2 diabetes as a reversible condition, primarily driven by dietary fat accumulation and excess weight, offers a hopeful paradigm shift in its management. The scientific evidence strongly supports the efficacy of significant weight loss, achieved through dietary changes and sustained lifestyle modifications, as a primary strategy for remission. This approach not only rivals but often surpasses the outcomes of more invasive interventions like bariatric surgery.
The implications of these findings are profound. They empower individuals to take an active role in their health, suggesting that by making informed choices about their diet and activity levels, they can significantly improve their metabolic health and potentially reverse a chronic disease. The historical journey from crude fasting methods to a sophisticated understanding of fat toxicity and metabolic pathways illustrates the evolution of medical science. Today, the focus is on evidence-based lifestyle interventions that prioritize sustainable weight loss and address the root causes of type 2 diabetes, offering a path toward long-term remission and improved quality of life.
The ongoing research and clinical validation of these principles are crucial. Public health initiatives and healthcare provider education must increasingly emphasize the potential for diabetes remission through lifestyle changes. This includes promoting balanced diets, encouraging regular physical activity, and providing comprehensive support systems to help individuals achieve and maintain the weight loss necessary for sustained health. The future of type 2 diabetes management lies not solely in pharmacological interventions, but in harnessing the power of lifestyle as a potent form of medicine.