The landscape of type 2 diabetes management is undergoing a significant reevaluation, with emerging scientific consensus highlighting the profound potential for disease remission through substantial weight loss. A pivotal finding suggests that nearly 90% of individuals diagnosed with type 2 diabetes for less than four years may achieve remission by shedding 15% of their body weight. This statistic offers a beacon of hope in the face of a growing global health crisis, as over half a billion adults currently live with diabetes, a figure projected to increase by approximately 50% within the next generation.
Historical Context: Early Understandings of Diabetes and Dietary Intervention
The concept of manipulating diet to manage diabetes is not new; its roots stretch back centuries, predating modern medical understanding. As early as the 19th century, observations during periods of extreme scarcity, such as the siege of Paris during the Franco-Prussian War, led to the rudimentary advice to "eat as little as possible" (mangez le moins possible). This principle was later formalized into the "Allen starvation treatment" by Dr. Frederick M. Allen in the early 20th century. Considered a major advancement before the discovery of insulin, Allen’s approach centered on severe caloric restriction.
Dr. Allen’s work was influenced by clinical reports suggesting that severe diabetes cases could spontaneously improve following debilitating conditions like tuberculosis or cancer, which often lead to significant weight loss. He theorized that inducing a "wasting condition" through extreme dietary limitation might have a similar effect on diabetes. His research demonstrated that even in severe cases, urinary sugar levels could be cleared within ten days through such restrictive diets. However, the challenge, as he observed, lay in maintaining these improvements once patients resumed eating. Allen’s strategy to manage patients involved keeping them underweight and strictly limiting dietary fat, noting that even the consumption of fats like butter or olive oil could trigger a relapse.
Further historical context reveals even more radical, albeit less scientific, early approaches. An Ayurvedic text from approximately 2,000 years ago proposed stark measures for diabetic individuals, including extreme physical exertion like walking hundreds of miles, manual labor such as digging ponds, or consuming highly restrictive and unpalatable substances like cow dung and cow urine. While these methods highlight an early recognition of the link between lifestyle and diabetes, they lack any basis in modern medical science and underscore the desperate search for solutions in the absence of effective treatments.
In a similarly extreme vein, the "Rollo diet" proposed in 1797 by John Rollo, Surgeon General to the Duke of Cumberland, was reportedly composed of rancid meat and utilized emetic drugs to induce severe sickness and vomiting. While these practices did reduce food intake and temporarily alleviate symptoms, their detrimental impact on overall health was undeniable. The underlying principle, however, that reducing food consumption could impact diabetes, persisted through various iterations, demonstrating a consistent, albeit often harsh, understanding of the caloric-overload theory of diabetes.
The Modern Understanding: Diabetes as a Disease of Fat Toxicity
Contemporary research has refined these historical observations, identifying a more specific underlying mechanism: type 2 diabetes is increasingly understood as a condition driven by "fat toxicity." This perspective posits that an excess accumulation of fat, particularly within liver and pancreatic cells, impairs insulin function and leads to insulin resistance.

Studies have shown that infusing fat into the bloodstream can, within hours, lead to observable fat accumulation in muscle cells and a corresponding increase in insulin resistance, detectable via advanced MRI technology. This effect is mirrored in individuals placed on high-fat diets; noticeable increases in insulin resistance can occur within just three days, and in some cases, even a single day or meal can have a significant impact. The rapid increase in insulin resistance following acute dietary fat intake is a critical factor.
When this insulin resistance occurs in muscles, especially in conjunction with excess caloric intake, it can trigger a cascade of metabolic dysfunctions. This can lead to fat accumulation in the liver, followed by the pancreas, ultimately manifesting as full-blown type 2 diabetes. Research indicates that type 2 diabetes can be conceptualized as a state of excessive fat deposition in the liver and pancreas, and crucially, this condition remains reversible for at least a decade in the majority of individuals.
The Power of Weight Loss: Mechanisms of Remission
The critical link between weight loss and diabetes remission lies in the body’s ability to mobilize and reduce excess fat stores. When individuals undergo a very low-calorie diet, such as one restricted to around 700 calories per day, the body begins to draw upon these stored fat reserves. This process leads to a significant reduction in fat within muscle cells, which in turn enhances insulin sensitivity.
Scientific visualization of this phenomenon demonstrates a marked decrease in fat buildup within the liver. As the dietary intervention continues, the excess fat in the pancreas also diminishes. This reversal of fat accumulation in key metabolic organs is the physiological basis for achieving diabetes remission.
Quantifying Remission Success: Weight Loss Benchmarks
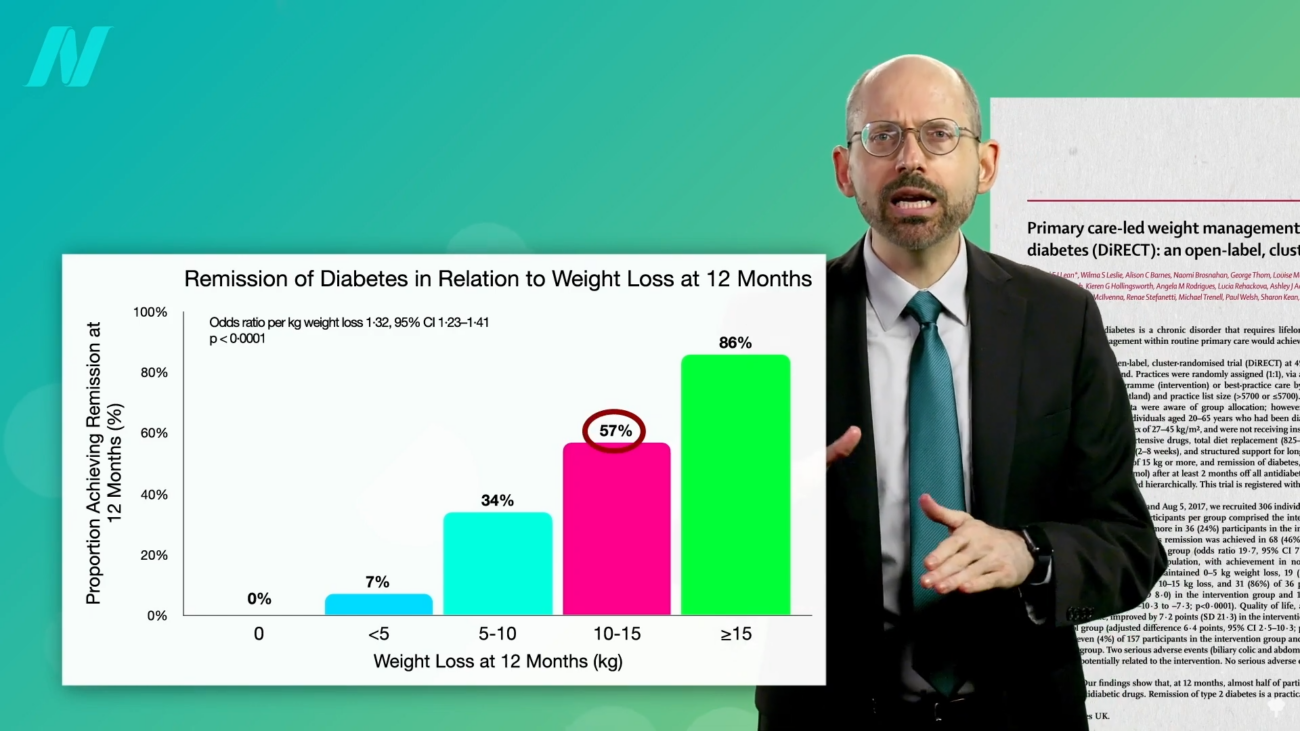
The extent of weight loss required for remission is a crucial metric. Studies reveal a strong correlation between the percentage of body weight lost and the likelihood of achieving non-diabetic blood sugar levels. For individuals diagnosed with type 2 diabetes for less than four years, a weight loss of 15% of their body weight can lead to remission in nearly 90% of cases.
The duration of the disease significantly impacts reversibility. For those who have lived with type 2 diabetes for longer than eight years, the remission rate may decrease to approximately 50% even with substantial weight loss. This underscores the importance of early intervention and diagnosis.
Comparison with Bariatric Surgery
Interestingly, the effectiveness of lifestyle interventions in achieving diabetes remission often surpasses that of bariatric surgery, a procedure typically associated with significant weight loss. Studies have shown that even after undergoing bariatric surgery and experiencing substantial weight reduction, remission rates for type 2 diabetes can be lower than those achieved through dietary changes and weight loss alone. For instance, bariatric surgery patients might see remission rates of 62% for those losing more weight, compared to the nearly 90% achieved by individuals with earlier diagnoses who lose 15% of their body weight through diet. This suggests that the precise mechanisms driving remission through weight loss, particularly the reduction of organ fat, may be more effectively targeted by dietary approaches than by surgery alone. The phrase "Your forks are better than surgeons’ knives" succinctly captures this emerging perspective, emphasizing the power of dietary choices over surgical intervention in managing and potentially reversing type 2 diabetes.
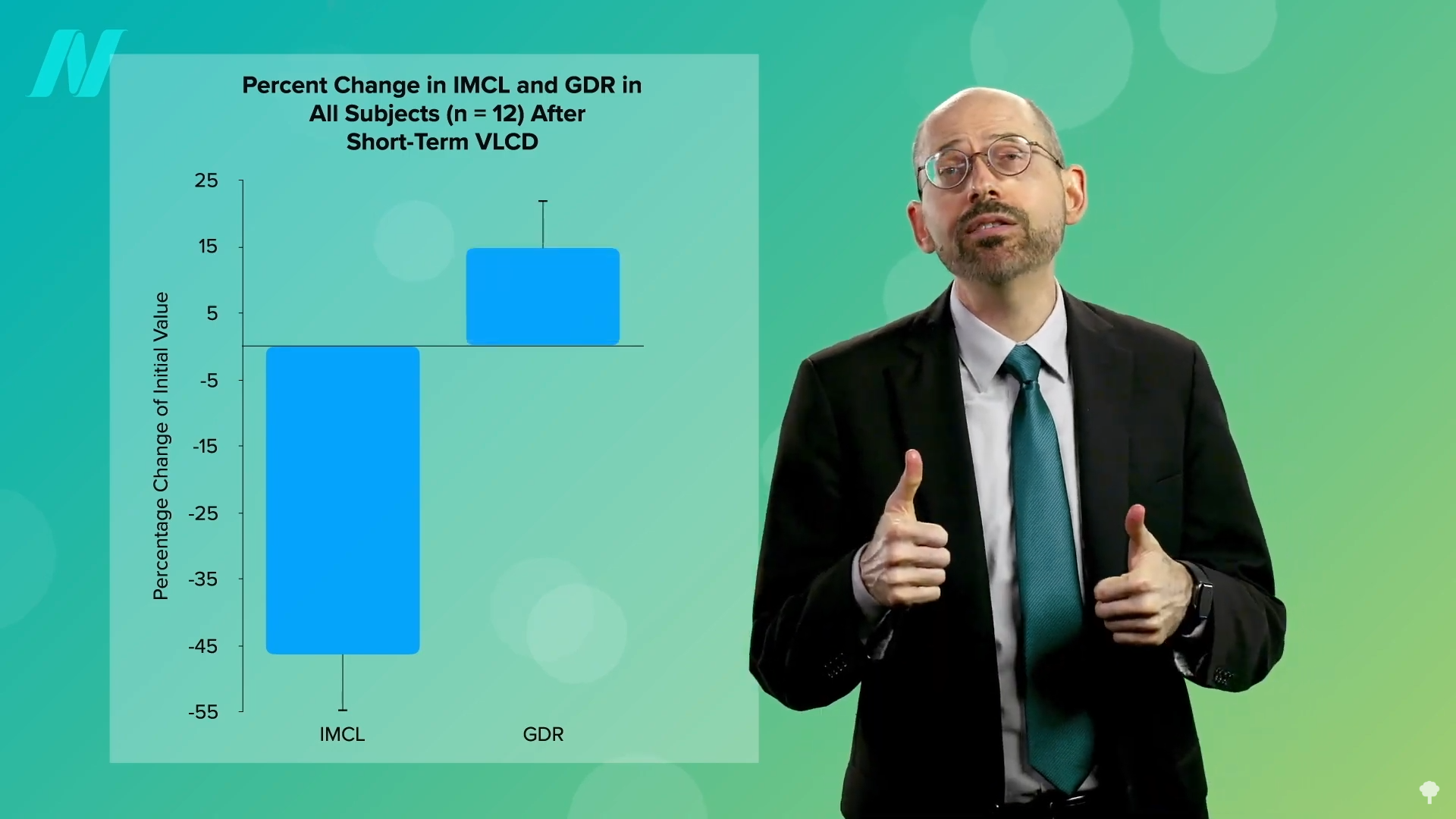
Further data indicates that for individuals diagnosed with type 2 diabetes for an average of three years, losing approximately 30 pounds can lead to disease reversal. This highlights a tangible and achievable goal for many patients seeking to regain control of their metabolic health.
The Role of Fasting and Sustained Lifestyle Changes
While medically supervised, water-only fasting can induce rapid weight loss and contribute to diabetes remission, the critical factor for long-term success is the sustained maintenance of that weight loss. Research has consistently shown that regaining lost weight often leads to the re-emergence of diabetes. Therefore, remission is not merely a temporary outcome of acute intervention but a consequence of sustained lifestyle modifications.
The Evolution of Diabetes Management: From Insulin to Lifestyle
The discovery of insulin in 1921 was a monumental breakthrough, hailed as "medicine’s greatest miracle." It provided a life-saving treatment for individuals with type 1 diabetes and dramatically improved the lives of many with type 2 diabetes. However, the initial euphoria soon gave way to a more nuanced understanding. While insulin could manage blood sugar levels, it proved insufficient on its own to prevent serious long-term complications of type 2 diabetes, such as blindness, kidney failure, stroke, and amputations.
This realization led pioneers in diabetes care, such as Elliott Joslin, to advocate for the continued centrality of lifestyle interventions. Joslin argued that self-discipline in diet and exercise, principles that were paramount in the pre-insulin era, should remain a cornerstone of diabetes management. His perspective underscores that while pharmaceutical advancements are vital, they are most effective when integrated with fundamental principles of healthy living.
Future Implications and Broader Impact
The growing body of evidence supporting diabetes remission through weight loss has significant implications for public health policy, clinical practice, and individual patient empowerment. It suggests a shift in focus from solely managing diabetes as a chronic, progressive disease to actively pursuing its reversal. This approach could lead to reduced healthcare costs associated with diabetes complications, improved quality of life for millions, and a re-evaluation of how diabetes is perceived and treated.
However, achieving and maintaining significant weight loss requires a multifaceted approach. It necessitates comprehensive patient education, accessible resources for dietary guidance, and robust support systems. The success of these interventions hinges on individuals embracing sustained behavioral changes, moving beyond temporary dietary restrictions to adopt a healthier, long-term lifestyle.
The future of type 2 diabetes management appears to be one where early diagnosis, coupled with aggressive weight loss strategies, offers a genuine possibility of remission, transforming a chronic condition into a potentially reversible one. This paradigm shift emphasizes the profound impact of lifestyle choices on metabolic health, empowering individuals to take an active role in their well-being and potentially rewrite their health trajectory.