Millions of Americans grapple with the debilitating effects of arthritis, with osteoarthritis of the knee standing as the most prevalent form and a significant contributor to disability. The complex inflammatory pathways driving these conditions have spurred extensive research into dietary interventions. While certain foods, like strawberries, have demonstrated the ability to reduce specific inflammatory markers, their direct clinical impact on arthritis symptoms has yielded mixed results. For instance, studies on cherry juice, while showing a decrease in C-reactive protein, a marker of inflammation, failed to provide superior symptom relief compared to placebos for knee osteoarthritis. This highlights the crucial distinction between reducing biological markers and achieving tangible clinical improvement for patients.
Exploring Dietary Interventions for Arthritis
The pursuit of natural remedies for arthritis has led researchers to examine a variety of anti-inflammatory foods. Strawberries, for example, have shown an ability to decrease circulating levels of tumor necrosis factor (TNF), a key inflammatory mediator. More compellingly, a randomized, double-blind, crossover trial indicated that dietary consumption of strawberries provided a significant analgesic effect, leading to a notable reduction in pain. This finding contrasts with earlier research on cherry juice, which, despite lowering C-reactive protein, did not translate into significant pain relief for knee osteoarthritis when compared to a placebo. While cherries may offer benefits for other forms of arthritis, such as gout, their efficacy for osteoarthritis remains questionable in clinical practice.

The significant cost of some pharmaceutical interventions, such as TNF inhibitor drugs that can approach $40,000 annually, further amplifies the interest in more accessible and potentially safer alternatives. The severe side effects associated with some potent anti-inflammatory medications, including a rare but fatal form of lymphoma, underscore the importance of exploring the therapeutic potential of dietary components.
Investigating the Anti-Inflammatory Properties of Berries and Extracts
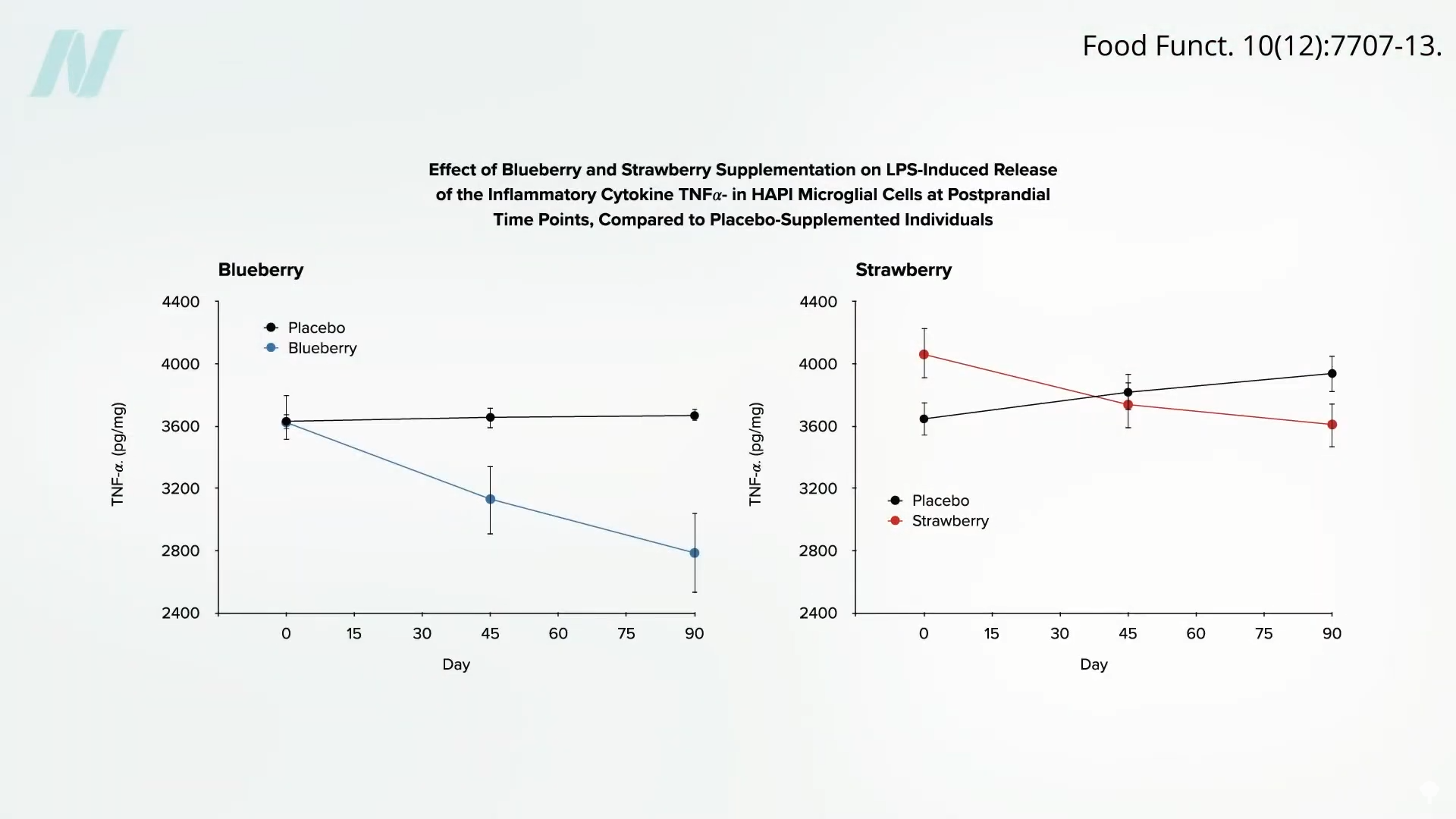
Research has delved into the biological mechanisms by which certain foods might exert anti-inflammatory effects. Studies have shown that when individuals consume the equivalent of one cup of blueberries or two cups of strawberries daily, their blood plasma, when applied to cells in laboratory settings, significantly reduces inflammation compared to plasma from individuals consuming placebo berries. This effect has been observed to increase over time, suggesting that sustained consumption of berries may lead to progressively greater anti-inflammatory benefits.
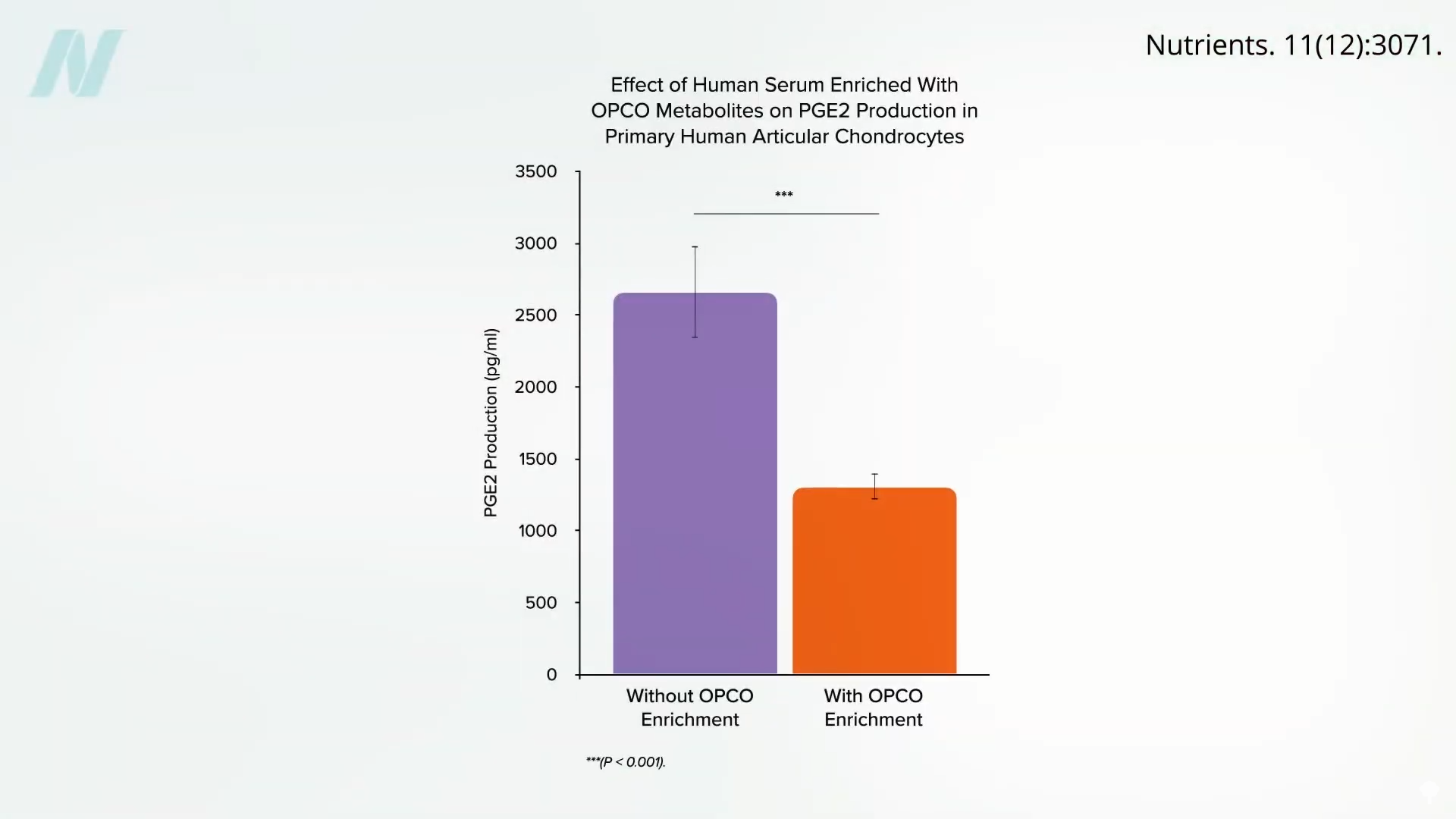
Beyond berries, researchers have investigated the impact of grapeseed and olive extracts on inflammatory processes. In one study, cartilage collected from knee replacement surgeries was exposed to blood samples from volunteers who had consumed a substantial dose of a grapeseed and olive extract. This exposure resulted in a significant reduction in inflammation. While human studies specifically on grapeseed extract for arthritis are limited, an olive extract has demonstrated the ability to alleviate pain and improve daily functioning in individuals with osteoarthritis.
The Nuance of Olive Oil in Arthritis Management
The initial findings regarding olive extracts sparked questions about the potential benefits of incorporating olive oil into one’s diet for arthritis. However, it’s crucial to distinguish between the effects of whole olive components and refined olive oil. The studies showing positive results often utilized freeze-dried olive vegetation water, which contains water-soluble compounds found in olives but absent in olive oil. This highlights that the beneficial components may not be the oil itself, but rather other elements within the olive.
Consuming whole olives, even in moderate amounts like a dozen a day, has been linked to a reduction in inflammatory mediators. However, the high sodium content of olives can be a significant concern, potentially consuming nearly half of the recommended daily intake. Despite claims of "remarkable anti-inflammatory activity" associated with extra virgin olive oil, much of the evidence stems from rodent studies. In human trials, extra virgin olive oil has shown comparable or even less favorable results than other fats like butter or coconut oil in managing inflammation.
While extra virgin olive oil has not consistently demonstrated broad benefits for conditions like fibromyalgia, it has shown some efficacy in alleviating symptoms of inflammatory bowel disease when compared to canola oil. The central question, however, remains: can olive oil compete with conventional arthritis drugs?
Topical Olive Oil: A Surprising Competitor
The breakthrough finding emerged from a double-blind, randomized clinical trial that directly compared topical virgin olive oil with a gel containing an ibuprofen-type drug for osteoarthritis of the knee. In this study, a small amount of topical olive oil – just one gram, equivalent to less than a quarter teaspoon, applied three times daily – proved to be significantly more effective than the ibuprofen-type gel in reducing pain. The daily cost of this topical treatment was remarkably low, under three cents per day.
The trial, which lasted for one month, indicated that topical olive oil was not only effective but superior to the conventional drug in pain management. This raises the intriguing possibility that the benefits of topical olive oil might continue to accrue with longer-term application.
Further research explored the efficacy of extra virgin olive oil in managing morning inflammatory pain in women with rheumatoid arthritis. In a comparative study involving rubbing the oil onto affected areas, compared to using no treatment or an ibuprofen-type gel, the group using extra virgin olive oil demonstrated a greater decrease in disease activity scores. This suggests a tangible benefit for patients experiencing the stiffness and pain characteristic of rheumatoid arthritis, even when applied topically.

Implications and Future Directions
The findings regarding topical olive oil present a significant development in the search for accessible and potentially safer arthritis management strategies. The demonstrated efficacy against an ibuprofen-type drug, coupled with its low cost and minimal side effects, positions topical olive oil as a promising complementary or alternative approach for individuals suffering from osteoarthritis and potentially rheumatoid arthritis.
While the research on topical application is encouraging, further studies are warranted to understand the long-term effects and optimal usage protocols. Investigating the specific compounds within olive oil responsible for its anti-inflammatory and analgesic properties could pave the way for more targeted treatments. Moreover, expanding research to include a wider range of arthritis types and patient populations will be crucial in establishing the full therapeutic potential of this natural remedy.
The contrast between the limited benefits of ingested olive oil for systemic inflammation and the notable success of topical application underscores the importance of delivery methods in therapeutic interventions. This research highlights that while dietary changes can influence inflammation, targeted topical treatments may offer a more direct and potent solution for localized joint pain and inflammation associated with arthritis. The medical community will be closely observing the progression of research in this area, as it holds the promise of offering a more affordable and natural path to pain relief for millions.


