The intricate barrier lining our intestines, a critical component of our overall health, is surprisingly vulnerable. New research indicates that everyday substances, from common medications to dietary choices, can compromise its integrity, leading to a condition colloquially known as "leaky gut" or increased intestinal permeability. This heightened permeability is emerging as a significant factor in disease prevention and a potential target for novel therapeutic strategies.
The Mighty Intestinal Barrier: An Unsung Hero
Our intestinal barrier, a marvel of biological engineering, is responsible for selectively absorbing nutrients while preventing harmful substances from entering the bloodstream. Despite its crucial role, its sheer scale is often underestimated. With its complex folds and villi, the intestinal lining unfurls to an astonishing surface area of over 4,000 square feet – a expanse larger than a tennis court. Maintaining this extensive and vital interface demands a considerable portion of our body’s energy resources, estimated to consume approximately 40% of our total daily energy expenditure. This significant metabolic cost underscores the importance of a robust and functional intestinal barrier.
Unraveling the "Leaky Gut" Concept
The scientific community is increasingly recognizing the disruption of intestinal barrier integrity as a key player in the pathogenesis of a variety of chronic and acute conditions. Growing evidence implicates compromised gut permeability in the development of autoimmune disorders like celiac disease and inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis.
Researchers have employed various methods to assess intestinal permeability. One notable technique involves the use of non-absorbable dyes, such as blue food coloring. In healthy individuals, these dyes are largely confined to the intestinal lumen. However, studies have detected their presence in the bloodstream of severely ill patients, particularly those suffering from sepsis, a life-threatening condition characterized by a systemic inflammatory response and often accompanied by a severely damaged gut barrier. This observation highlights the direct correlation between barrier dysfunction and systemic illness.
Crucially, the development of a "leaky gut" is not exclusive to critical care settings. Even common over-the-counter medications, readily available to the general public, can induce significant intestinal permeability.
The Impact of Common Medications: Aspirin and NSAIDs Under Scrutiny
Non-steroidal anti-inflammatory drugs (NSAIDs), a class of medications widely used for pain relief and fever reduction, have come under particular scrutiny for their potential to disrupt the intestinal barrier. Studies have demonstrated that even a single dose of aspirin can increase intestinal leakiness. For instance, research indicates that taking just two regular aspirin tablets (325 mg each) or two extra-strength aspirin tablets (500 mg each) can measurably increase gut permeability. These findings serve as a stark warning, suggesting that even individuals who consider themselves healthy should exercise caution when using aspirin, as it can lead to gastrointestinal barrier dysfunction.
The notion that buffered aspirin, a combination product designed to mitigate gastrointestinal irritation by including an antacid, might offer a protective advantage has also been challenged. Research has shown that both regular aspirin and buffered aspirin formulations can induce multiple erosions in the delicate inner lining of the stomach and intestines. Endoscopic examinations, where a camera is inserted into the gastrointestinal tract, have revealed extensive redness and erosions in the lining of up to 90% of individuals who took aspirin or buffered aspirin at recommended doses. Alarmingly, this damage can manifest rapidly, occurring within as little as five minutes of ingestion.
Acetaminophen, widely known by its brand name Tylenol in the United States, is often considered a safer alternative for pain relief in terms of gastrointestinal effects. While it may not directly cause the same level of gastrointestinal damage as NSAIDs, it is essential to note its potential for liver toxicity, making it an unsuitable choice for individuals with pre-existing liver conditions.
Interestingly, some research suggests that vitamin C supplements, rather than offering a protective effect, might exacerbate aspirin-induced increases in gut leakiness. This finding adds another layer of complexity to the interplay between common supplements and medication-induced gut damage.
The implications of NSAID-induced gut leakiness extend beyond direct gastrointestinal issues. There is a growing body of evidence suggesting a link between NSAID use and an increased risk of food-induced anaphylaxis, a severe and potentially life-threatening allergic reaction. These drugs are reportedly involved in up to 25% of food-induced anaphylaxis cases, associated with over a tenfold higher risk of such severe allergic attacks. The proposed mechanism involves the increased permeability of the intestinal barrier, allowing minuscule food particles to enter the bloodstream, triggering an exaggerated immune response.
Beyond Medications: Lifestyle Factors and Gut Health
While medications are significant contributors to gut permeability, other lifestyle factors also play a role.

The Demands of Strenuous Exercise
Even strenuous physical activity, while generally beneficial for health, can transiently impact intestinal integrity. An hour of exercise at 70% of maximum capacity, for example, can divert a significant amount of blood flow from the internal organs to the working muscles. This redistribution of blood can lead to temporary injury and mild gut leakiness. This effect can be further compounded if athletes concurrently use NSAIDs, a practice unfortunately not uncommon.
Alcohol Consumption and Gut Barrier Function
Alcohol consumption has also been identified as a risk factor for food allergy attacks, operating through a similar mechanism of increasing gut leakiness. However, studies suggest that abstaining from alcohol can facilitate the healing of the intestinal barrier.
Dietary Fat and the Gut Microbiome
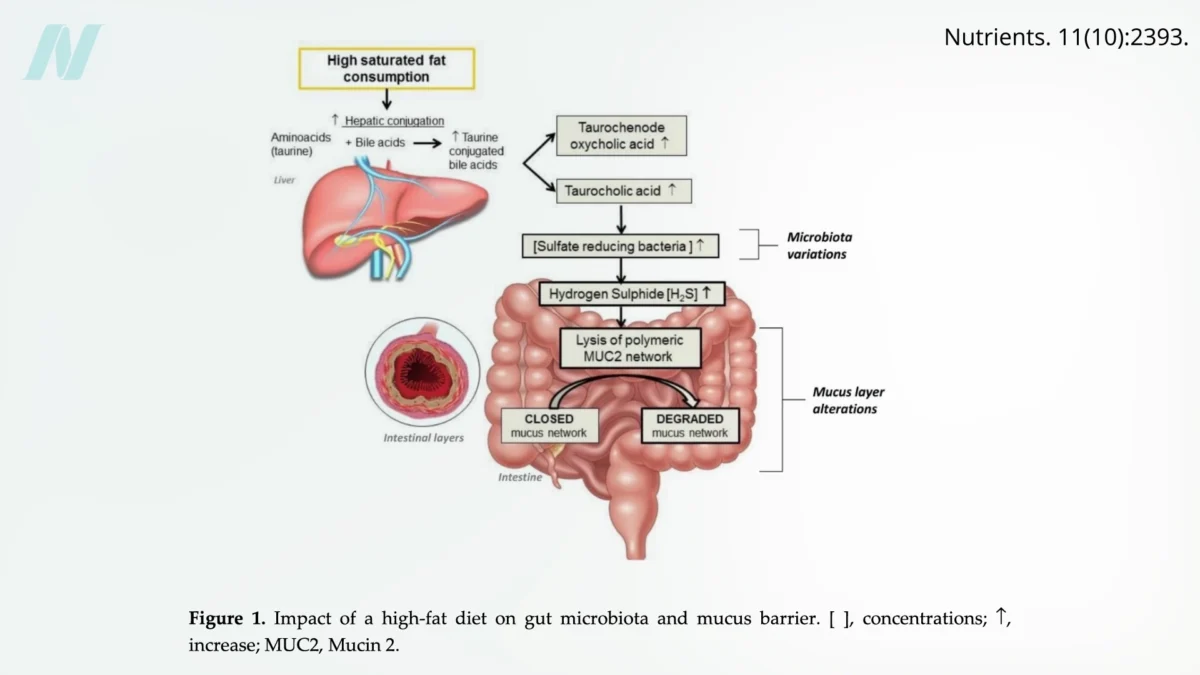
Dietary patterns are increasingly recognized as powerful modulators of gut health. Elevated consumption of saturated fats, prevalent in red meat, dairy products, and many processed "junk" foods, has been linked to detrimental changes in the gut environment. Saturated fats can promote the growth of certain bacteria that produce hydrogen sulfide, a gas with a rotten-egg odor. This gas can degrade the protective mucus layer that lines the intestines, a crucial defense mechanism.
High-fat diets, in general, are understood to negatively impact intestinal health by disrupting the intestinal barrier through various mechanisms. While much of the research in this area has been conducted on laboratory animals or in in-vitro settings, human studies are beginning to provide compelling evidence.
The rise in obesity and cardiometabolic disorders has coincided with a widespread dietary shift from traditional lower-fat diets to higher-fat Westernized diets. A disturbed gut flora, or microbiome, has been demonstrably associated with an increased risk of these same diseases. Rodent studies suggest that high-fat diets can unbalance the microbiome and impair the gut barrier, ultimately contributing to disease development.
To bridge the gap between animal and human studies, comprehensive human interventional trials have been conducted. A six-month randomized controlled feeding trial investigating the effects of dietary fat on gut microbiota provided significant insights. The study found that increased fat consumption was indeed associated with unfavorable alterations in the gut microbiome and elevated levels of proinflammatory factors in the blood. Notably, this effect was observed even when refined carbohydrates were simply replaced with refined fats, such as swapping white rice and wheat flour for soybean oil. These findings carry significant implications, suggesting that countries undergoing dietary transitions towards Westernized patterns should consider advising against increased dietary fat intake, while those already consuming such diets might benefit from reducing their fat consumption.
Implications for Public Health and Future Research
The growing body of evidence linking common lifestyle factors and medications to increased intestinal permeability highlights a critical area for public health intervention and further scientific inquiry. Understanding the mechanisms by which these factors compromise the gut barrier is essential for developing targeted strategies to prevent and manage a range of chronic diseases.
Potential for Disease Prevention and Therapy
The identification of intestinal permeability as a key target opens new avenues for both disease prevention and therapeutic intervention. By understanding which foods, beverages, and medications contribute to a "leaky gut," individuals can make informed choices to protect their intestinal health. Furthermore, this understanding could lead to the development of novel treatments aimed at restoring barrier function and mitigating the downstream health consequences.
The Role of Dietary Interventions
Dietary modifications appear to be a promising avenue for supporting gut barrier integrity. Reducing the intake of saturated fats and processed foods, while potentially increasing the consumption of nutrient-dense, anti-inflammatory foods, could play a significant role in promoting a healthy gut environment. Further research into the specific dietary components that bolster or degrade the intestinal barrier is warranted.
Further Investigation into Medication Safety
The impact of commonly used medications, particularly NSAIDs, on gut health necessitates ongoing research and public awareness. Exploring safer alternatives or developing strategies to mitigate the gastrointestinal side effects of these drugs could significantly improve patient outcomes.
Broader Health Connections
The link between a compromised intestinal barrier and systemic inflammation, autoimmune diseases, and even allergic reactions underscores the interconnectedness of our bodily systems. Addressing gut health may have far-reaching positive effects on overall well-being and the prevention of numerous chronic conditions.
Conclusion
The concept of "leaky gut" is evolving from a fringe idea to a recognized area of significant medical concern. As research continues to illuminate the complex interplay between our diet, lifestyle, medications, and the integrity of our intestinal barrier, the potential for proactive health management and novel therapeutic interventions becomes increasingly clear. By making informed choices about what we consume and how we manage our health, we can actively work towards maintaining a strong and healthy intestinal barrier, a cornerstone of our overall well-being.
Doctor’s Notes and Additional Resources:
For those seeking to delve deeper into the topic of "leaky gut," further information is available. Resources such as "The Leaky Gut Theory of Why Animal Products Cause Inflammation" and "How to Heal a Leaky Gut with Diet" offer comprehensive insights into the mechanisms and dietary strategies related to this condition. Additionally, discussions on gut leakiness have been featured in discussions concerning Small Intestinal Bacterial Overgrowth (SIBO), highlighting its relevance in various gastrointestinal health contexts.