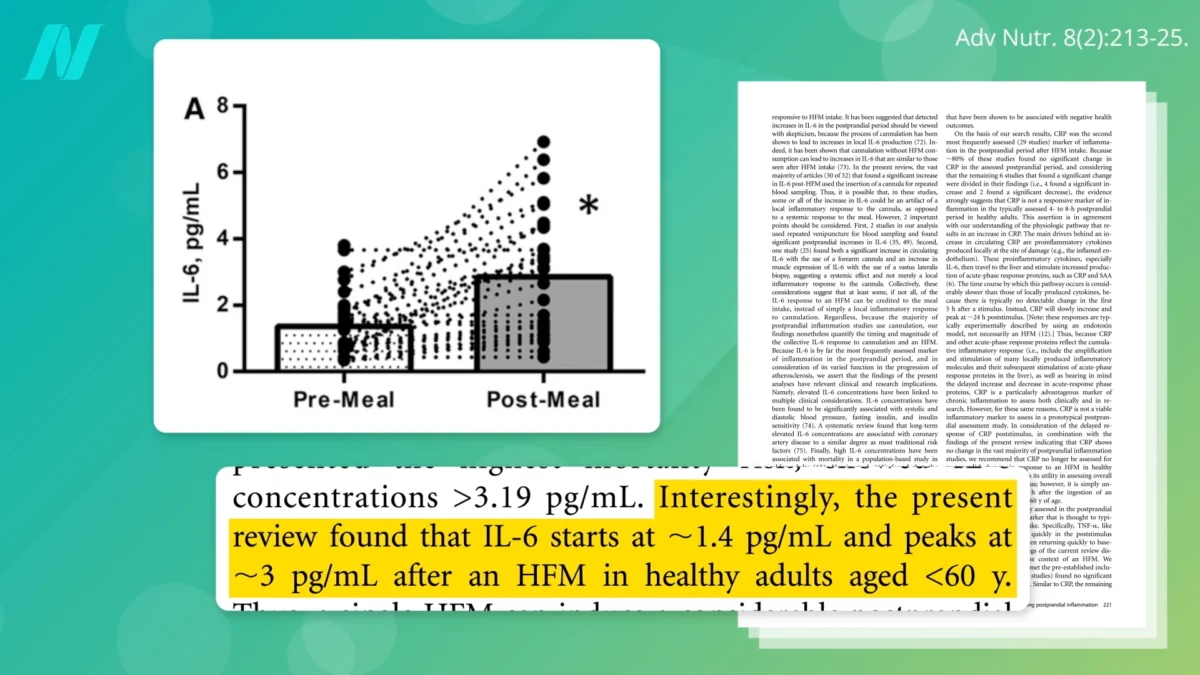
Mounting scientific evidence suggests that the foods we consume can trigger significant inflammatory responses within hours of ingestion, potentially contributing to a range of chronic diseases. Recent research highlights that inflammatory markers, such as interleukin-6 (IL-6), can more than double within a mere six-hour period following the consumption of a single pro-inflammatory meal. This rapid physiological reaction underscores the potent and immediate impact of dietary choices on the body’s inflammatory state, a factor increasingly recognized as a significant contributor to leading causes of death and disability, including type 2 diabetes, obesity, and cardiovascular disease.
The Acute Inflammatory Cascade: Beyond Chronic Consumption
For years, the focus in understanding diet-related inflammation has largely centered on the long-term effects of chronic high-fat diets. However, a growing body of research indicates that the inflammatory repercussions of unhealthy eating are not confined to sustained dietary patterns. Instead, the detrimental effects can manifest acutely, even after the consumption of a single, imbalanced meal. This paradigm shift in understanding the immediate physiological consequences of food intake is critical for public health messaging and individual dietary guidance.
Studies have consistently demonstrated a marked increase in inflammatory markers, particularly IL-6, subsequent to the ingestion of meals characterized by a high fat content. Crucially, these meals often do not solely consist of animal fats but also incorporate refined carbohydrates, such as white flour, and added sugars. This combination of ingredients appears to be particularly potent in triggering an inflammatory cascade.

Unpacking the Culprits: Fat and Sugar’s Role
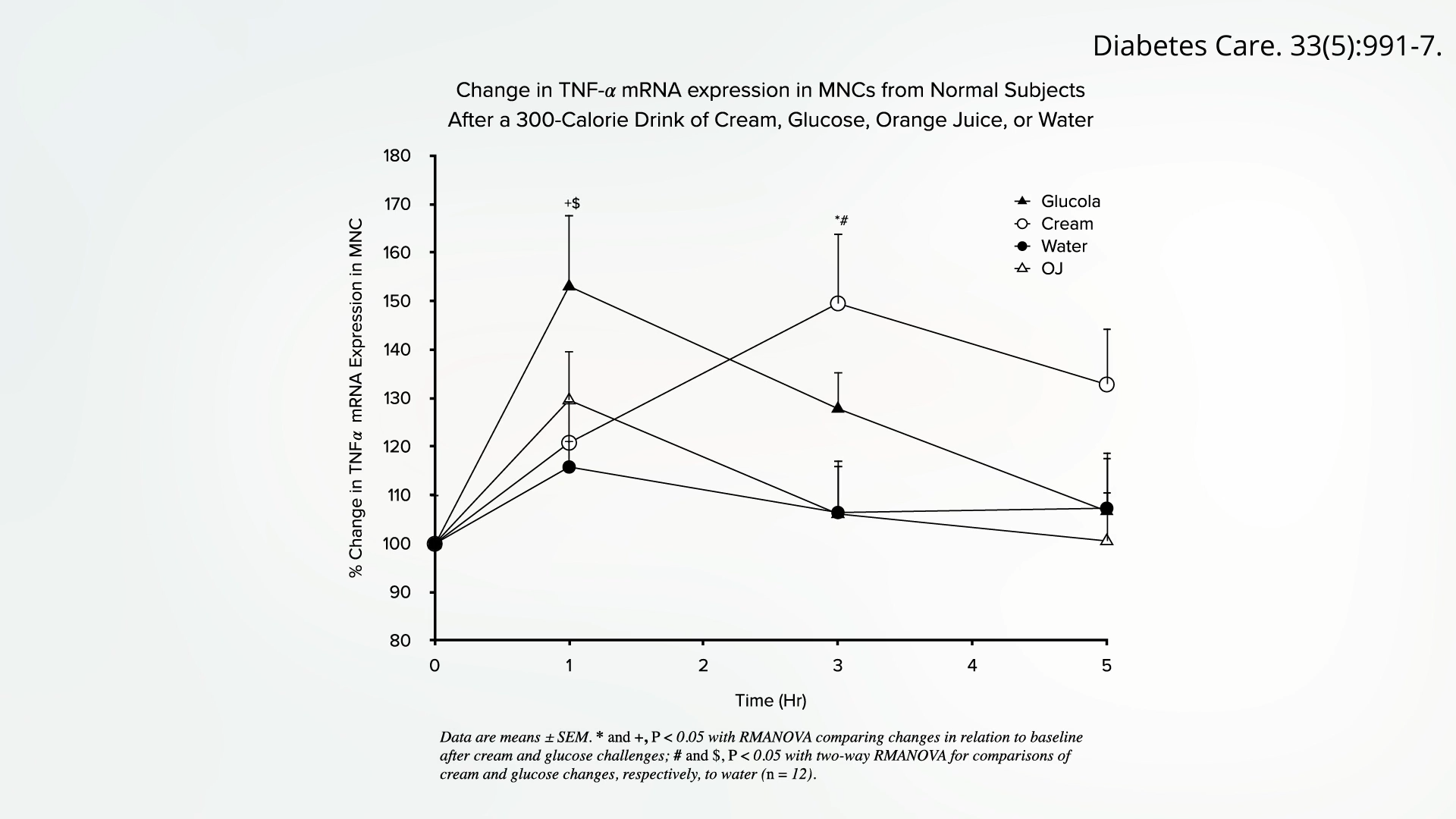
To isolate the specific contributions of different macronutrients, researchers have conducted studies where participants consumed either pure butterfat or a sugar-water solution, devoid of other dietary components. The findings were striking: both pure fat and pure sugar, when consumed in isolation, were shown to elicit a significant spike in inflammation within hours. This provides compelling evidence that both added fats and added sugars independently act as pro-inflammatory agents, contributing to the acute inflammatory response observed after consuming mixed unhealthy meals.
The implications of these findings are substantial. If a single meal can initiate such a rapid inflammatory response, then the cumulative effect of regular consumption of such foods could lead to persistent, low-grade inflammation. This chronic state is a well-established underlying factor in the development and progression of numerous chronic diseases that pose a significant burden on global health systems.
The Significance of Elevated Inflammatory Markers
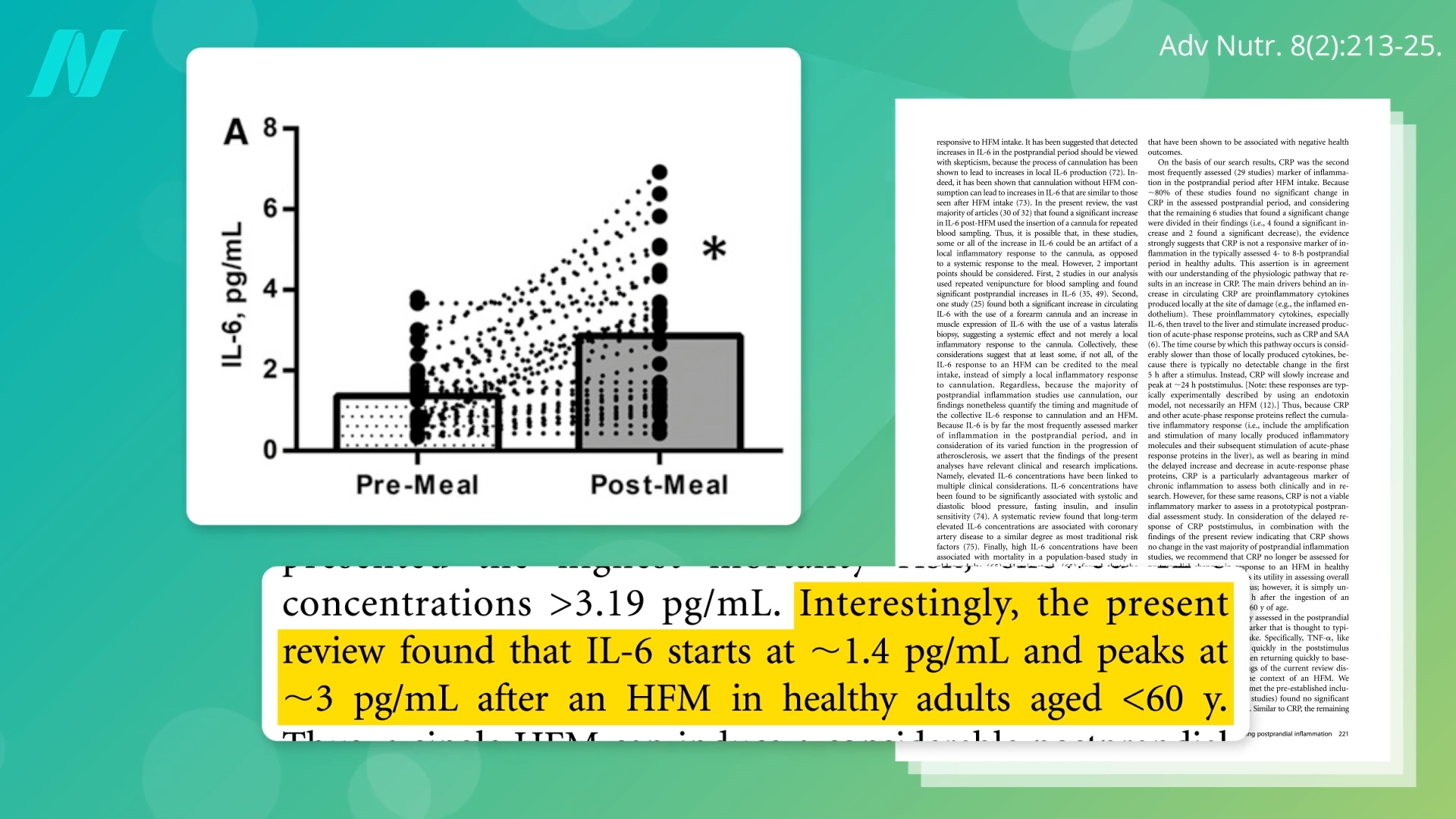
The concern surrounding post-meal inflammation stems from the growing understanding of its link to adverse health outcomes. Elevated levels of IL-6, a key cytokine involved in the inflammatory response, are particularly noteworthy. Research indicates that when IL-6 levels regularly rise to approximately 3 picograms per milliliter (pg/mL), this is associated with a doubled risk of mortality. This association has been observed across a broad spectrum of studies, suggesting a robust and consistent link between elevated IL-6 and increased mortality risk.
Inflammatory Markers and Cardiovascular Risk
The increased risk of death associated with elevated IL-6 is likely multifaceted, but its strong correlation with cardiovascular disease cannot be overstated. Cardiovascular disease remains the leading cause of death for both men and women globally. Studies have found that the association between elevated IL-6 and cardiovascular events is as significant as that observed with other well-established risk factors, such as high cholesterol levels. This highlights inflammation as a critical, and perhaps underestimated, player in the pathogenesis of heart disease.
The immediate post-meal inflammatory surge, therefore, is not merely a transient physiological event but a potential trigger that, when occurring repeatedly, can contribute to the chronic inflammation implicated in the development of these life-threatening conditions.
Not All Fats Are Created Equal: The Role of Whole Foods
While the focus has often been on the pro-inflammatory nature of fats, it is crucial to distinguish between different types of fats and their sources. Emerging research indicates that not all high-fat foods elicit the same inflammatory response. Whole plant-based foods, such as nuts, have demonstrated a remarkable ability to avoid increasing inflammatory markers, even when consumed in significant quantities, such as several handfuls per day. This suggests that the matrix and accompanying nutrients in whole plant foods play a protective role against inflammation.
The Buffering Effect of Healthy Fats
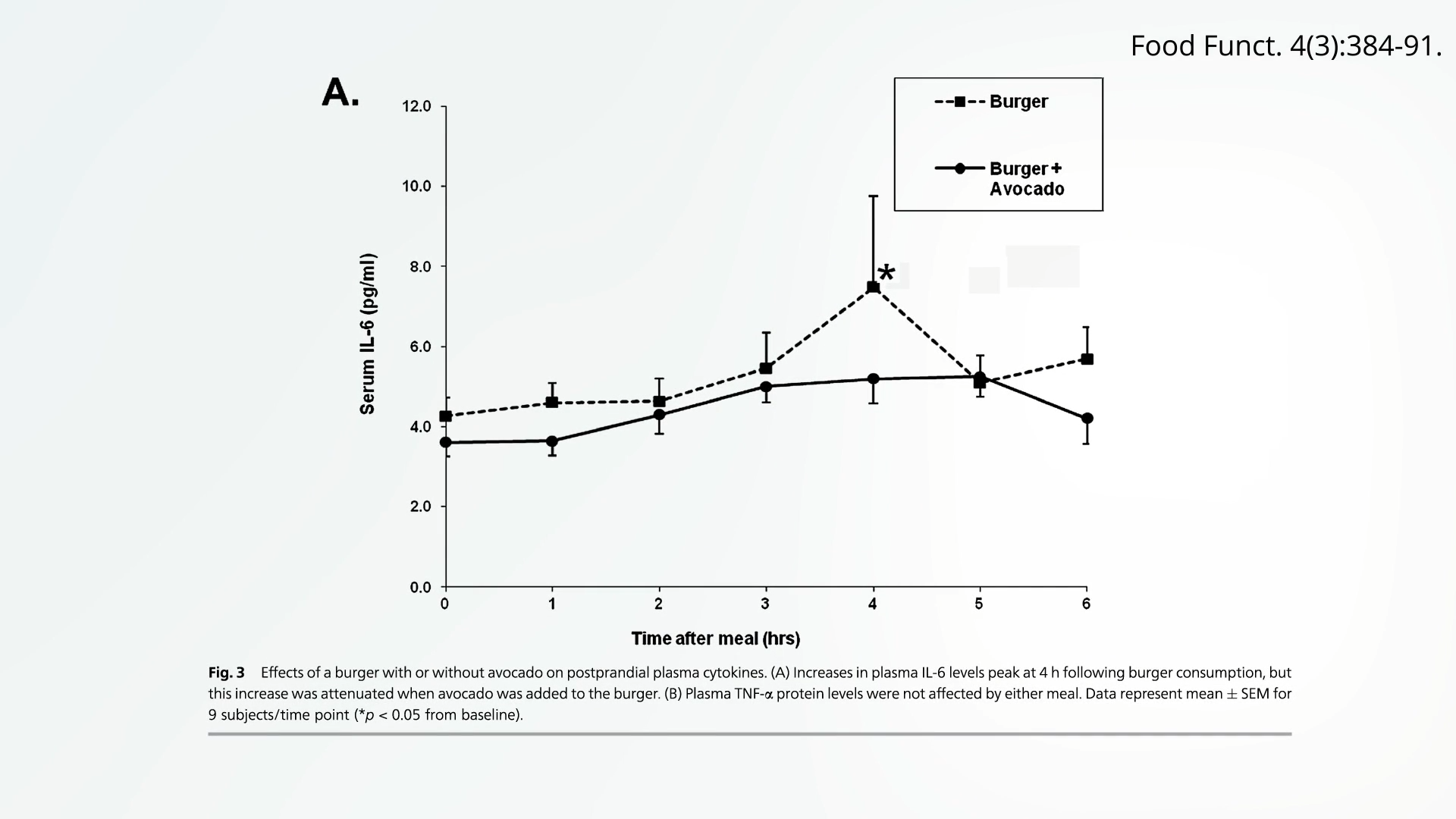
Furthermore, the inclusion of healthy fats in a meal can potentially mitigate the inflammatory effects of other components. For instance, studies have shown that adding half an avocado to a beef burger, even a lean one, can help to blunt some of the inflammatory response triggered by the meat. This finding points towards the synergistic effects of different food components and the potential for strategic food combinations to influence the body’s overall inflammatory response.
The Complexities of Meat and Inflammation
The inflammatory response to meat consumption, even lean varieties, warrants closer examination. While some reviews have suggested a reduction in inflammatory markers after consuming wild game, this is often in comparison to conventionally raised, fattier meats. When individuals consume very fatty meat, there is a demonstrable and rapid increase in inflammatory markers like IL-6, tumor necrosis factor (TNF), and C-reactive protein (CRP). These are all key indicators of systemic inflammation.
Intriguingly, even extremely lean meats, such as kangaroo steak, which are comparable in fat content to elk or moose, can still trigger a significant inflammatory response within hours of consumption. This suggests that factors beyond just fat content, potentially unique proteins or other compounds present in meat, may also contribute to the pro-inflammatory nature of these foods. The speed at which these responses occur, within mere hours, reinforces the idea that the body’s reaction to certain animal proteins can be immediate and pronounced.
A Nuanced Perspective on Meat Consumption
While less inflammatory than some conventional meats, the consumption of even lean game meat can still contribute to an increase in inflammatory markers shortly after eating. This nuanced understanding is vital for individuals seeking to manage their inflammatory load through diet. It suggests that while leaner animal protein sources might be preferable to fattier ones, they may not be entirely devoid of an inflammatory impact.
Broader Implications for Public Health and Dietary Guidance
The scientific findings regarding the immediate inflammatory effects of certain foods have significant implications for public health strategies and individual dietary recommendations. The understanding that a single meal can initiate a pro-inflammatory cascade challenges the notion that only chronic dietary habits lead to inflammation-related diseases.
The Role of Refined Foods and Sugars
The consistent identification of refined carbohydrates and added sugars as significant contributors to inflammation underscores the need for public health campaigns to emphasize the reduction of processed foods, sugary beverages, and refined grain products. These foods are often calorie-dense but nutrient-poor, and their rapid absorption can lead to sharp fluctuations in blood sugar and subsequent inflammatory responses.
Empowering Consumers with Knowledge
By providing clear, evidence-based information about which foods are most likely to trigger inflammation, consumers can be empowered to make more informed choices. This includes understanding that while healthy fats from whole plant sources are generally anti-inflammatory, the fats and refined carbohydrates found in processed and fast foods are key drivers of acute inflammation.
Future Directions in Research
Continued research is essential to further elucidate the complex mechanisms by which different foods influence inflammation. Understanding the specific molecular pathways involved, the role of gut microbiota in modulating inflammatory responses, and the long-term health consequences of repeated acute inflammatory surges will be crucial. Furthermore, developing effective dietary interventions that not only reduce inflammation but are also sustainable and culturally appropriate for diverse populations remains a key public health objective.
The insights gained from studying the immediate impact of food on inflammation offer a powerful lens through which to view the relationship between diet and health. By recognizing the acute, as well as chronic, effects of our food choices, we can move towards a more proactive and personalized approach to preventing diet-related diseases and promoting overall well-being. The science clearly indicates that what we eat, and when we eat it, has a profound and immediate impact on our body’s inflammatory balance.