The landscape of bariatric weight-loss surgery, while offering a powerful tool for individuals struggling with severe obesity, is fraught with potential complications, the severity of which may be significantly influenced by the surgical team’s proficiency. Emerging data and studies indicate that surgeon skill is not merely a qualitative factor but a quantifiable determinant of patient outcomes, directly impacting rates of complications, readmissions, reoperations, and even mortality. This has prompted a closer examination of surgical expertise within the field and a call for greater transparency and standardization.
The Escalating Need for Revision and Associated Risks
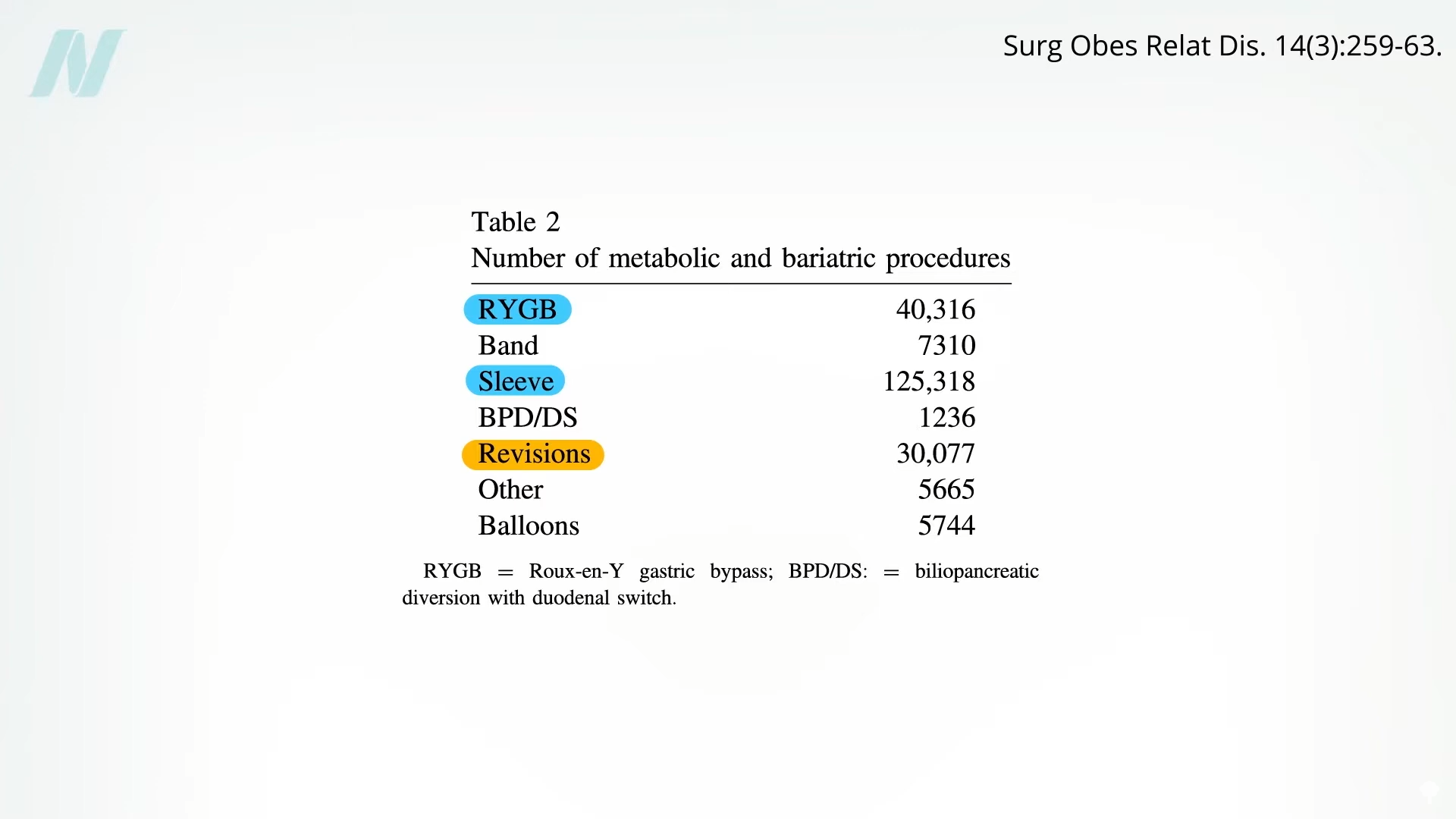
Bariatric procedures, including the widely recognized sleeve gastrectomy and Roux-en-Y gastric bypass, are among the most frequently performed surgeries globally. However, a less publicized, yet significant, reality is the substantial number of patients who require subsequent surgical interventions. In fact, revision procedures to correct issues arising from an initial bariatric operation now stand as the third most common surgical intervention in this domain.
This trend underscores a critical concern: a considerable portion of bariatric patients, estimated to be as high as 25%, are compelled to undergo further operations due to complications stemming from their first bariatric surgery. The implications of these subsequent surgeries are particularly dire. Reoperations carry a demonstrably higher risk profile, with mortality rates potentially ten times greater than those of primary procedures. Furthermore, the success of these revision surgeries is far from guaranteed, presenting a complex challenge for both patients and healthcare providers.
The spectrum of complications following bariatric surgery is broad and can include life-threatening issues such as leaks from surgical staple lines, the formation of abnormal connections between organs (fistulas), the development of painful ulcers, narrowing of the digestive tract (strictures), internal erosion of surgical materials, blockages in the gastrointestinal system, and severe acid reflux.
Surgeon Skill: A Critical Determinant of Patient Safety
A groundbreaking study published in The New England Journal of Medicine shed critical light on the role of surgeon expertise in mitigating these risks. In this research, bariatric surgeons voluntarily submitted video recordings of their surgical procedures for peer review and evaluation. The findings revealed a wide disparity in technical proficiency among surgeons, a variation that directly correlated with patient outcomes.
The study established a clear link between a surgeon’s technical skill and the incidence of post-operative complications, hospital readmissions, the need for reoperations, and mortality rates. Patients operated on by surgeons deemed less competent experienced nearly triple the rate of complications and a five-fold increase in mortality compared to those treated by their more skilled counterparts. This research provided robust empirical evidence that the human element – the surgeon’s dexterity, precision, and understanding of surgical nuances – plays a pivotal role in patient safety.
The Learning Curve: A Necessary Investment in Expertise
The notion that surgical skill is akin to that of a musician or athlete, with inherent talent playing a role, is a perspective shared by some experts. However, the consensus emphasizes the crucial impact of practice and experience in honing surgical abilities. Bariatric procedures, particularly complex ones like gastric bypass, are characterized by a steep learning curve.

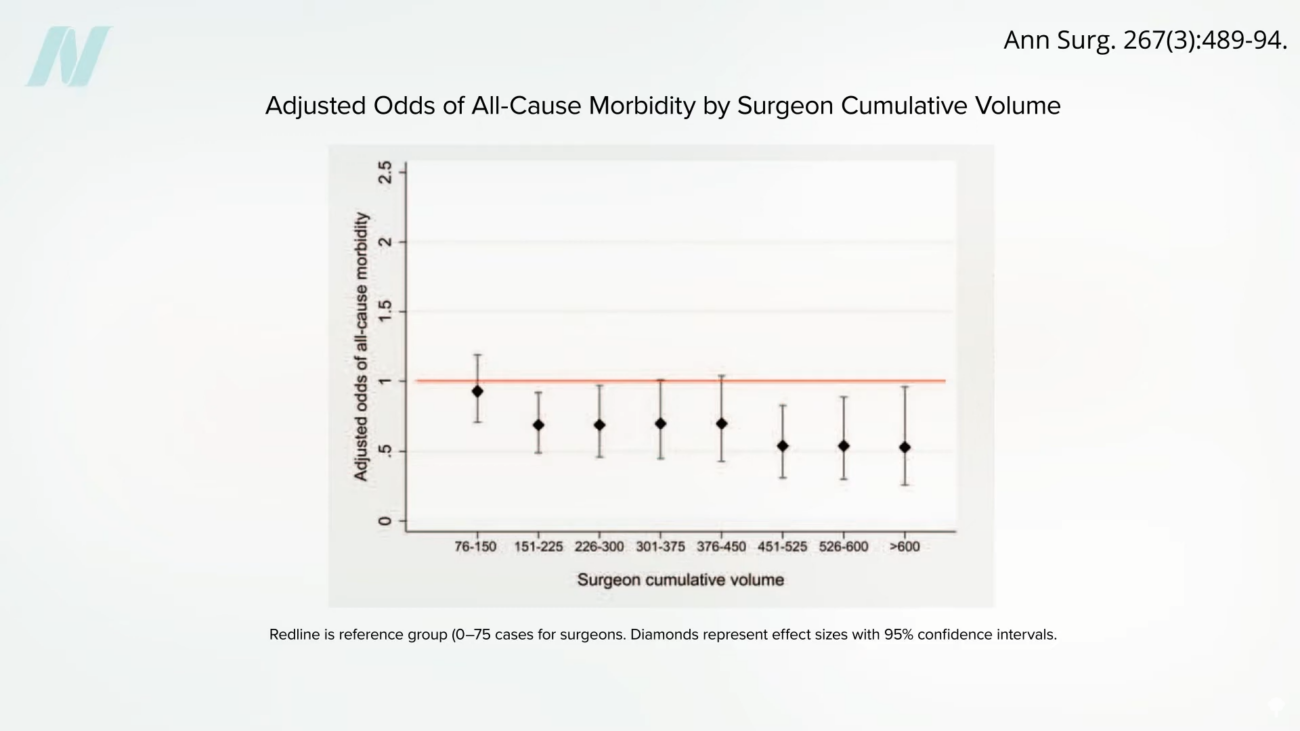
Estimates suggest that a surgeon may need to perform as many as 500 cases to achieve a mastery level of proficiency in gastric bypass surgery. The risk of complications appears to plateau after approximately 500 procedures. Surgeons who have completed more than 600 bypass operations have demonstrated the lowest rates of adverse outcomes.
Data from a comparative analysis illustrates this point starkly: the risk of mortality for patients undergoing surgery with surgeons who have performed fewer than 75 procedures is approximately double that of patients treated by surgeons who have completed more than 450 bypasses. This highlights the critical importance of experience, suggesting that a surgeon’s cumulative caseload is a strong predictor of patient safety and surgical success.
Navigating the Surgical Landscape: Recommendations for Patients
Given the profound impact of surgeon skill on patient outcomes, individuals considering bariatric surgery are strongly advised to engage in thorough due diligence. A key recommendation is to inquire directly with potential surgeons about their experience, specifically asking about the total number of bariatric procedures they have performed. This information can provide valuable insight into their level of expertise.
Furthermore, choosing an accredited bariatric "Center of Excellence" is highly recommended. These centers typically adhere to rigorous quality standards and have demonstrated a commitment to patient safety and optimal outcomes. Studies have indicated that surgical mortality rates at accredited Centers of Excellence are two to three times lower than those at non-accredited institutions, further reinforcing the value of seeking care at specialized, high-quality facilities.
Beyond Surgical Error: The Role of Patient Behavior and Post-Operative Care
While surgeon skill is a critical factor, it is not the sole determinant of bariatric surgery outcomes. Patient behavior and adherence to post-operative guidelines also play a significant role. A cautionary tale, often cited in discussions of surgical complications, involves a patient who, three months after a gastric bypass, consumed an excessive amount of food at an all-you-can-eat buffet without adequate chewing. This led to the rupture of surgical staples and necessitated emergency surgery to remove undigested food, including large chunks of broccoli and whole lima beans, from her abdominal cavity.
This anecdote, while perhaps extreme, serves as a potent reminder of the importance of mindful eating and proper food preparation after bariatric surgery. However, it also prompts a broader reflection: the focus on chewing food thoroughly post-surgery, while important, should not overshadow the fundamental importance of adopting a healthy diet before surgery to prevent the conditions that necessitate such drastic interventions in the first place.
The Lifelong Commitment: Nutritional Deficiencies and Long-Term Management
Even when bariatric surgery is performed flawlessly, the long-term implications for patient health extend far beyond the operating room. These procedures, by design, alter the digestive system to promote weight loss, often through mechanisms that impair nutrient absorption. Consequently, lifelong nutritional replacement and vigilant monitoring are indispensable to prevent serious vitamin and mineral deficiencies.
The consequences of these deficits can be far-reaching, extending beyond common issues like anemia, osteoporosis, or hair loss. Patients are at risk of developing life-threatening deficiencies such as beriberi (thiamine deficiency), pellagra (niacin deficiency), and kwashiorkor (protein deficiency). Nerve damage, potentially leading to vision loss, can manifest years or even decades after surgery due to conditions like copper deficiency.

Tragically, severe deficiencies of essential B vitamins, such as thiamine, have been reported to result in permanent brain damage in nearly one in three affected patients before the condition is identified. This underscores the critical need for comprehensive and ongoing nutritional support and assessment following bariatric surgery.
Understanding the Mechanisms: Malabsorption and "Dumping Syndrome"
Procedures like gastric bypass intentionally induce malabsorption of nutrients by bypassing segments of the intestines. This mechanism, while effective in reducing calorie absorption, comes at the cost of absorbing vital nutrients. Even restrictive procedures, such as stomach stapling, can place patients at risk of life-threatening nutrient deficiencies due to persistent vomiting.
Vomiting is a reported side effect in up to 60% of patients after bariatric surgery, often attributed to "inappropriate eating behaviors," which essentially means attempting to eat in a manner that is no longer compatible with the altered anatomy. This vomiting can contribute to weight loss, functioning similarly to an aversion therapy.
Another significant post-operative phenomenon is "dumping syndrome." A substantial percentage of gastric bypass patients experience symptoms such as abdominal pain, diarrhea, nausea, bloating, fatigue, or palpitations after consuming calorie-rich foods. This occurs because food bypasses the stomach too quickly and empties directly into the intestines. Surgeons often describe dumping syndrome not as a complication, but as an intended consequence, designed to deter patients from consuming energy-dense foods. This behavioral modification, while aiding in weight loss, can significantly impact a patient’s quality of life and dietary choices.
Broader Implications and Future Directions
The growing body of evidence highlighting the impact of surgeon skill on bariatric surgery outcomes has several important implications. Firstly, it reinforces the need for robust training programs and continuous professional development for bariatric surgeons. Standardized assessment tools, similar to those used in the New England Journal of Medicine study, could be integrated into surgical training and practice to ensure a baseline level of competency.
Secondly, it emphasizes the importance of patient education and informed consent. Patients should be fully aware of the risks associated with bariatric surgery and the factors that can influence these risks, including surgeon experience and the choice of surgical facility. Transparency regarding surgeon experience and success rates, where ethically and practically feasible, could empower patients to make more informed decisions.
Finally, the persistent challenge of long-term nutritional deficiencies underscores the need for integrated care models that include dedicated dietitians and endocrinologists specializing in bariatric patient management. Early detection and proactive management of these deficiencies are crucial for preventing severe, irreversible health consequences. As the field of bariatric surgery continues to evolve, a multi-faceted approach that prioritizes surgical excellence, patient education, and lifelong nutritional support will be paramount in ensuring the safety and well-being of individuals seeking to manage severe obesity through surgical intervention.
This article is the second in a four-part series on bariatric surgery. The first installment, "The Mortality Rate of Bariatric Weight-Loss Surgery," is available for review. Future articles will explore "Bariatric Surgery vs. Diet to Reverse Diabetes" and "How Sustainable Is the Weight Loss After Bariatric Surgery?" For those interested in sustainable weight loss strategies, the book "How Not to Diet" offers comprehensive guidance.