The human body’s intricate defense system, inflammation, is a critical process for healing and fighting off infections. However, when this response becomes chronic or excessive, it can contribute to a host of serious health conditions, including type 2 diabetes, obesity, cardiovascular disease, and certain cancers – all leading causes of death and disability globally. New research highlights a startling reality: the inflammatory cascade, often associated with long-term dietary habits, can be significantly triggered by the consumption of a single pro-inflammatory meal, with key inflammatory markers doubling within a mere six hours. This rapid response underscores the immediate and potent impact of certain foods on our physiological well-being.
The Rapid Onset of Inflammation: Beyond Chronic Diets
For years, the focus on diet and inflammation has largely centered on the detrimental effects of chronic high-fat diets. These dietary patterns are well-established contributors to systemic inflammation. However, the latest findings reveal a more immediate threat. The inflammatory effects of unhealthy eating are not solely confined to the cumulative damage of sustained poor dietary choices. Instead, a single, pro-inflammatory meal can elicit a pronounced and measurable inflammatory response shortly after ingestion.

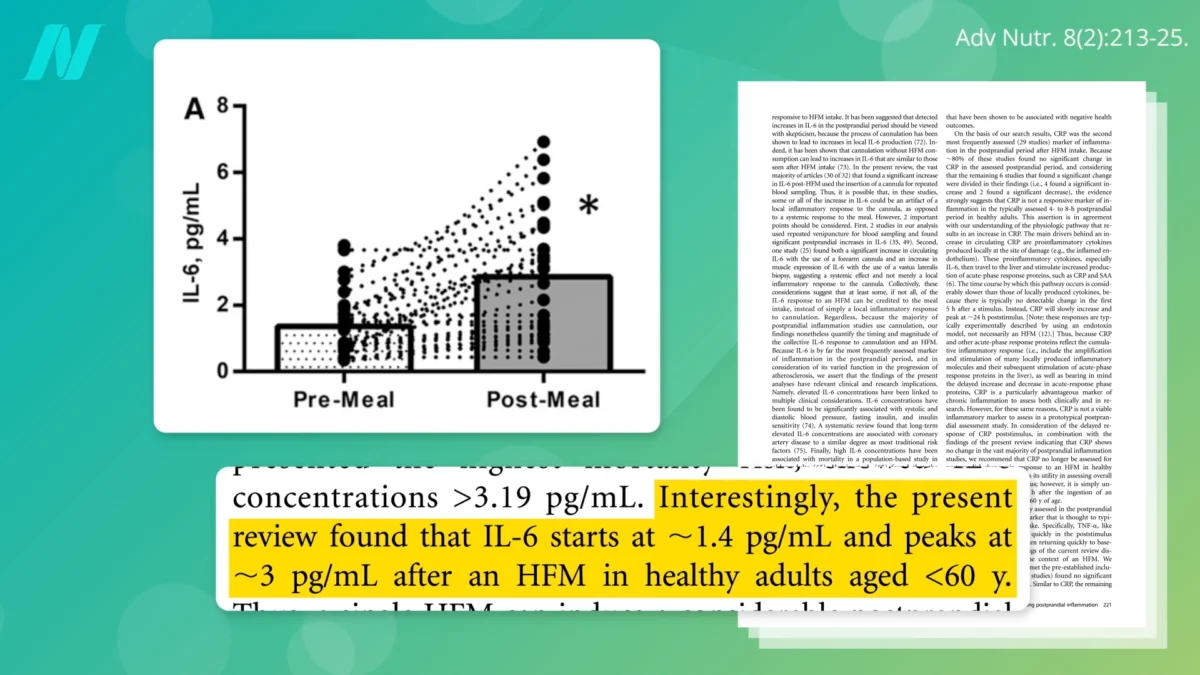
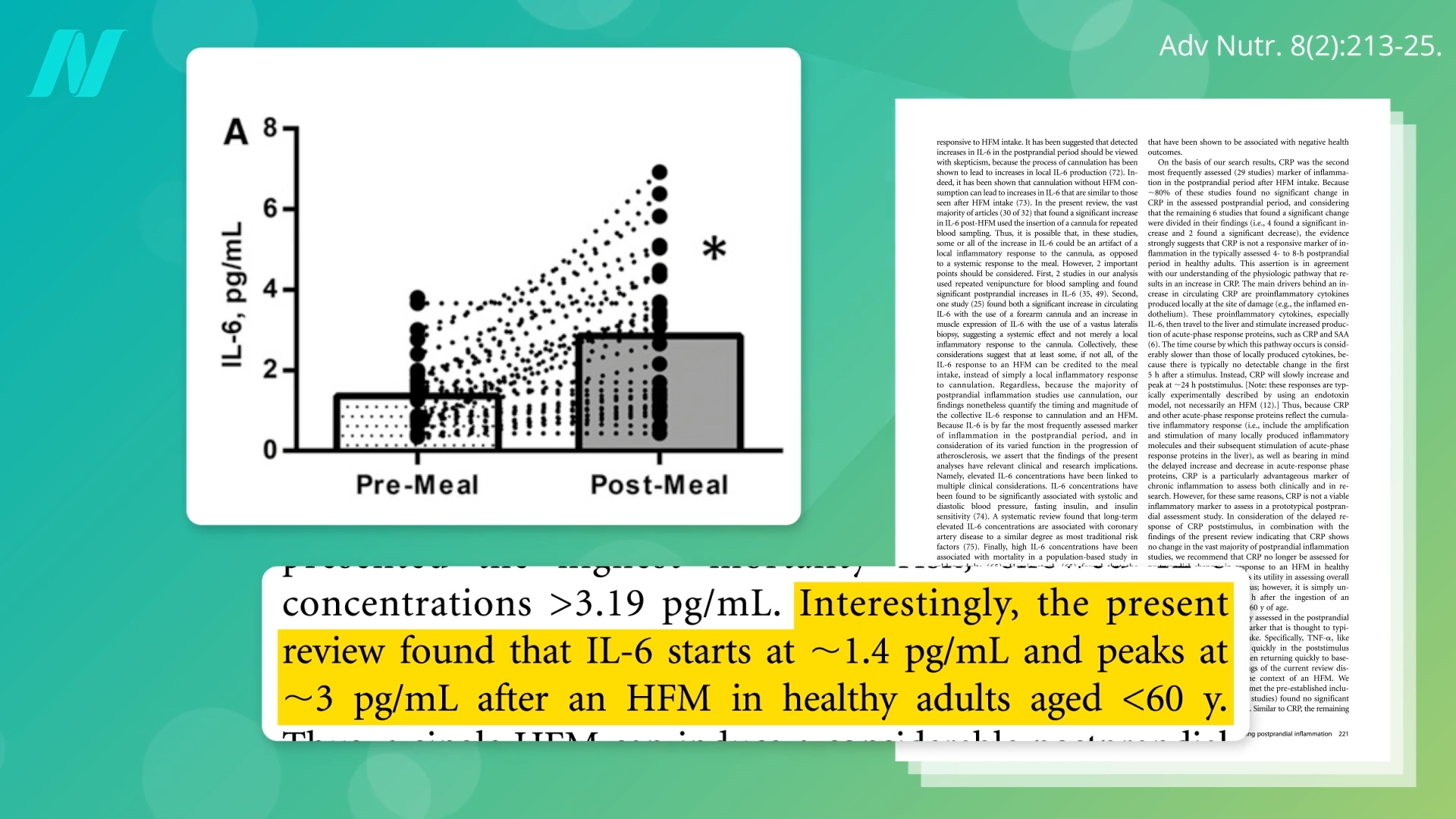
Studies indicate that inflammatory markers such as interleukin-6 (IL-6) can surge dramatically following the consumption of an unhealthy meal. Specifically, IL-6 levels have been observed to double within a six-hour window. While many studies have focused on high-fat meals, the research indicates that the problematic components are not exclusively derived from animal fats. Instead, the tested meals frequently combined high fat content with refined carbohydrates, including white flour and added sugars. This combination appears to amplify the pro-inflammatory effect, demonstrating that both fat and refined sugars independently contribute to this harmful bodily reaction.
Unpacking the Culprits: Fat and Sugar’s Inflammatory Role
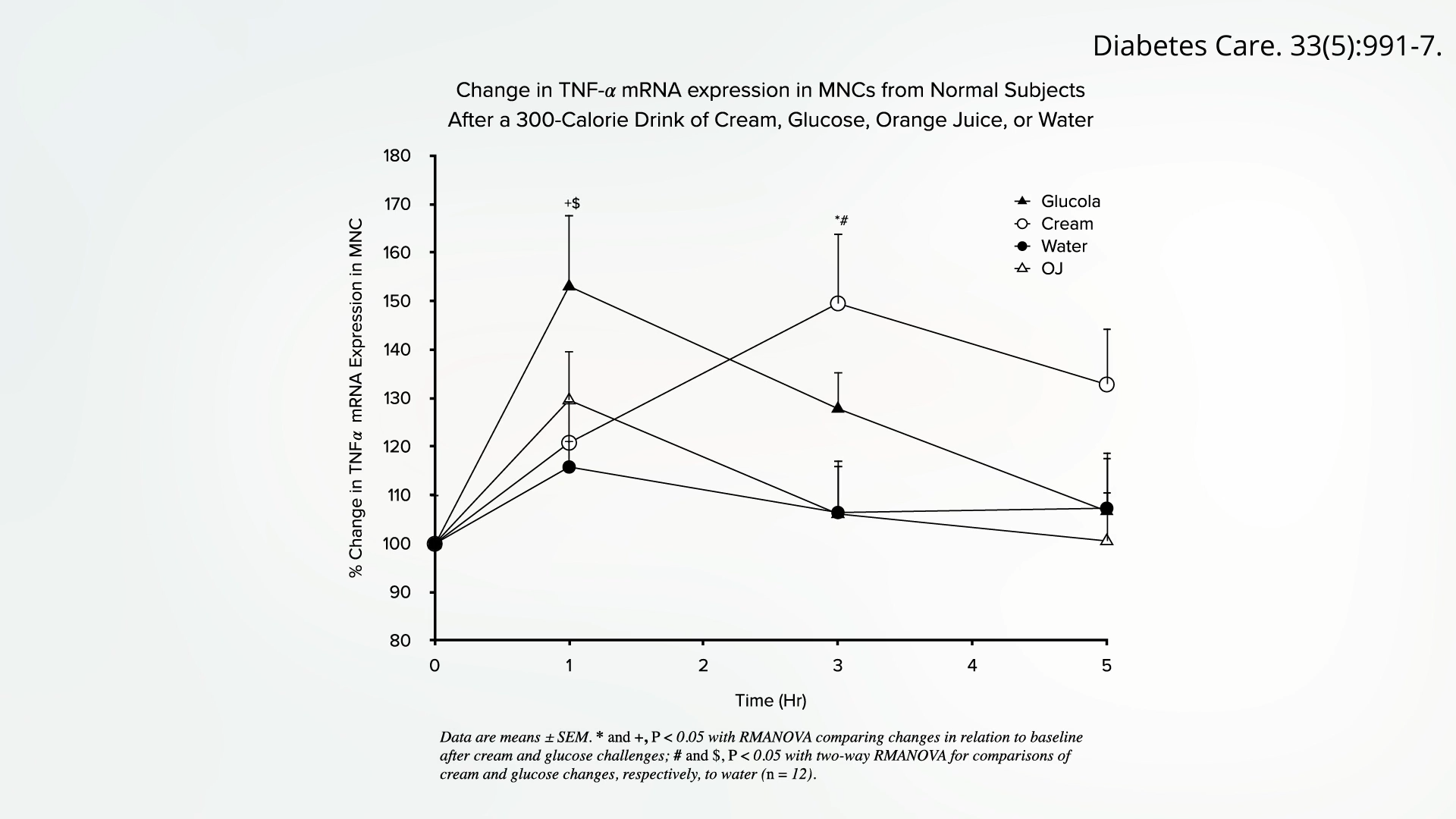
To disentangle the specific contributions of fat and sugar, researchers have conducted targeted studies. In one experiment, participants were given a concentrated dose of pure butterfat, devoid of carbohydrates. The results were significant: a discernible spike in inflammation within hours, confirming the inherent pro-inflammatory nature of added fats. In a parallel study, participants consumed a solution of pure sugar water, again without any fat. This experiment yielded the same outcome – a marked increase in inflammatory markers, proving that added sugars are also potent triggers of inflammation. These findings, visualized in research graphs, clearly illustrate that both macronutrients, when consumed in refined forms, can independently initiate a pro-inflammatory response.
The Serious Health Implications of Post-Meal Inflammation
The concern surrounding these acute inflammatory responses after consuming unhealthy meals stems from their potential long-term consequences. Persistent, low-grade inflammation is increasingly recognized as a fundamental underlying factor in the development and progression of numerous chronic diseases that carry high mortality rates. Diet plays a crucial role, capable of both exacerbating and mitigating this inflammation.
The observed increase in IL-6 levels, often reaching approximately 3 pg/mL after an unhealthy meal, is particularly concerning. When IL-6 levels regularly approach or exceed this threshold, it has been associated with a doubled risk of mortality. This increased risk has been consistently observed across a wide range of studies, likely due to IL-6’s strong correlation with an elevated risk of cardiovascular disease. Cardiovascular disease remains the leading cause of death for both men and women globally, and its link to inflammation is as significant as other well-established risk factors, such as high cholesterol.
Not All Fats Are Created Equal: The Protective Power of Whole Plant Foods
While the focus has often been on the pro-inflammatory nature of certain dietary components, it is essential to distinguish between different types of fats and foods. Emerging research indicates that not all high-fat foods contribute to inflammation. Specifically, whole plant-based foods, such as nuts, have demonstrated a remarkable ability to avoid increasing inflammatory markers, even when consumed in substantial quantities – up to several handfuls per day.
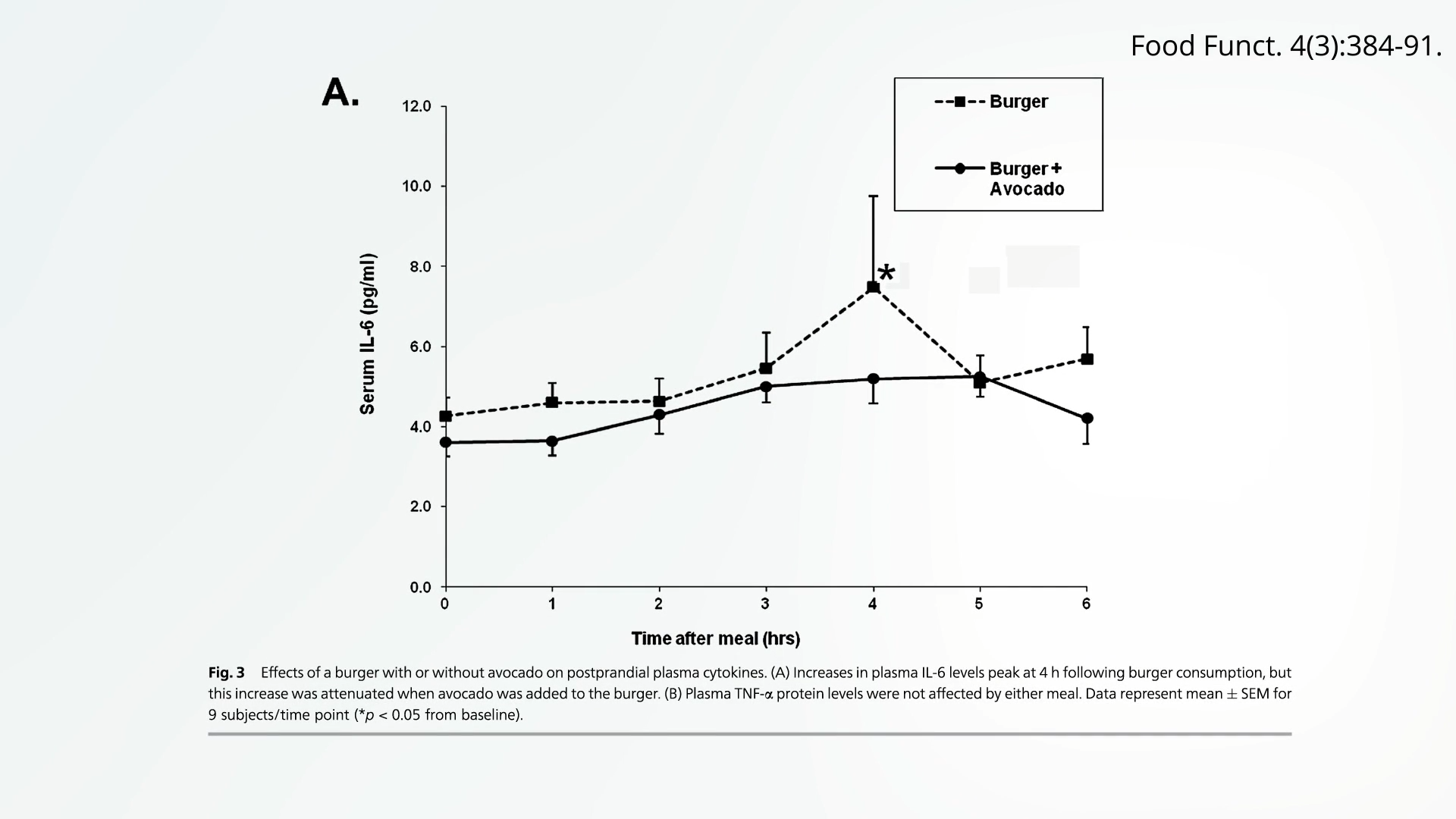
Furthermore, the inclusion of healthy fats from plant sources can potentially counteract the inflammatory effects of other less healthy foods. For instance, studies have shown that adding half an avocado to a beef burger, even a lean one, can help to blunt some of the inflammation triggered by the meat. This suggests a complex interplay where the overall composition of a meal, and the inclusion of anti-inflammatory foods, can significantly modify the body’s response.
The Inflammatory Response to Meat: A Closer Examination
The inflammatory response to meat consumption has been a subject of considerable research, with varying conclusions. Some reviews have suggested a reduction in inflammatory markers after consuming wild game, which is notably lean. However, these findings often represent comparisons to conventionally raised, fattier meats. When individuals consume particularly fatty cuts of meat, a significant surge in IL-6, along with tumor necrosis factor (TNF) and C-reactive protein (CRP) – other key inflammatory markers – is observed within hours.
Intriguingly, the inflammatory response is not solely dictated by fat content. Studies involving extremely lean meats, such as kangaroo steak (comparable in leanness to elk or moose), have also demonstrated a strong inflammatory reaction within hours of consumption. This finding challenges the simplistic notion that leanness alone dictates a food’s inflammatory potential and suggests that other compounds within meat, regardless of fat content, may also contribute to the pro-inflammatory cascade. While potentially less inflammatory than some processed or fattier conventional meats, these leaner meat options still elicit a notable inflammatory response shortly after ingestion.
Broader Impact and Future Directions
The implications of these findings are far-reaching. They underscore the need for a nuanced understanding of dietary inflammation, moving beyond generalized advice to more specific guidance on food choices. The rapid and significant inflammatory response triggered by single meals highlights the importance of mindful eating and the immediate impact of food choices on health.
This research opens avenues for further investigation into the specific mechanisms by which different foods trigger inflammation. Understanding these pathways could lead to the development of more targeted dietary interventions for preventing and managing chronic diseases. The contrast between the inflammatory potential of refined carbohydrates and fats versus the anti-inflammatory or neutral effects of whole plant foods provides a clear direction for dietary recommendations aimed at reducing chronic disease risk.
Key Takeaways:
- Rapid Inflammatory Response: Inflammatory markers like IL-6 can double within six hours of consuming a single pro-inflammatory meal.
- Dual Culprits: Both refined fats and added sugars independently contribute to this rapid inflammation.
- Chronic Disease Link: Persistent low-grade inflammation is a significant factor in leading causes of death and disability, including heart disease and diabetes.
- Protective Plant Foods: Whole plant foods, such as nuts and avocados, do not increase inflammatory markers and can even mitigate inflammation caused by other foods.
- Meat’s Complex Role: While leaner meats may be less inflammatory than fattier options, even very lean meats can trigger a significant inflammatory response.
As public health initiatives increasingly focus on preventative care and lifestyle interventions, understanding the acute effects of diet on inflammation becomes paramount. The evidence suggests that embracing a diet rich in whole, unprocessed plant foods and moderating the intake of refined carbohydrates and certain fats is a critical strategy for maintaining long-term health and reducing the risk of chronic disease. Future research will likely delve deeper into the synergistic effects of food components and the development of personalized dietary strategies to optimize individual inflammatory responses. The immediate impact of our food choices on our internal inflammatory state demands our attention and can serve as a powerful motivator for adopting healthier eating patterns.