The question of whether choosing organic over conventional foods offers protection against cancer and the specific effects of pesticides on cancer risk has become a significant focus in public health discussions. A growing body of scientific evidence suggests a robust connection between pesticide exposure and the development of cancer, prompting a deeper examination of dietary choices and their potential impact on long-term health outcomes.
The Overwhelming Evidence of Pesticide Toxicity
Recent scientific reviews have underscored the substantial evidence linking pesticide exposure to cancer. One comprehensive review, updating the understanding of human exposure and toxicity, concluded that the body of evidence is so extensive that the role of pesticides in cancer development "cannot be doubted." This assertion is built upon decades of research examining the mechanisms by which these chemicals can interact with biological systems.
However, a critical distinction emerges when examining the source of much of this evidence. A significant portion of studies demonstrating DNA damage from pesticides has originated from occupational exposure scenarios. This includes farmers and agricultural workers who are directly involved in the application of pesticides, individuals working within the pesticide industry, and communities residing in areas with high levels of pesticide spraying. These high-exposure groups provide crucial insights into the potential toxicological effects of these chemicals.
While occupational exposure provides a stark picture of pesticide risks, concerns are also mounting regarding non-occupational exposure, which affects the general population through various environmental pathways, including diet. Evidence linking non-occupational pesticide exposure to DNA damage has been observed, such as single- and double-stranded DNA fragmentation in the sperm of men with elevated pesticide levels in their bodies. While one study documenting this effect was conducted in China, where average pesticide concentrations were notably higher than in many other regions, it highlights the potential for widespread impact.

Mechanisms of Pesticide-Induced Harm
Beyond direct DNA damage, pesticides may contribute to cancer development through other mechanisms, notably by compromising the body’s natural defenses. Natural Killer (NK) cells, a crucial component of the immune system’s first line of defense against cancer cells and virus-infected cells, have shown susceptibility to pesticide-induced harm. Research has indicated that exposure to pesticides can impair the function of these vital defender cells, diminishing their ability to effectively eliminate tumor cells.
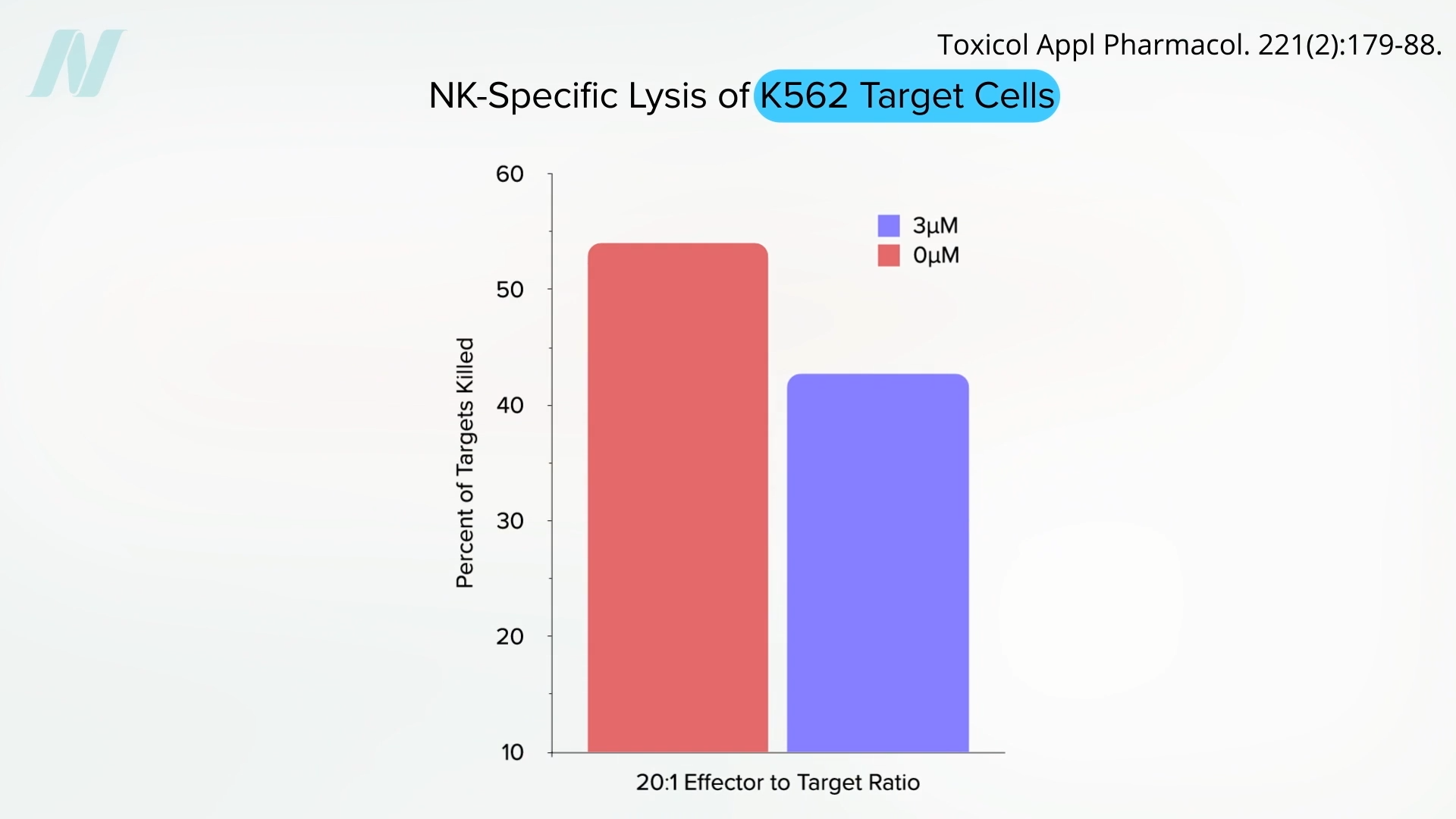
Experimental studies have illustrated this effect vividly. In laboratory settings, NK cells have demonstrated a significant capacity to eliminate a substantial proportion of leukemia cells when introduced in a controlled environment without any pesticide present. However, the introduction of even small amounts of pesticides has been shown to severely disable these NK cells, allowing the cancer cells to proliferate and dominate. This finding suggests a potential pathway through which pesticide exposure could weaken the body’s innate ability to fight off nascent cancers.
The concentration of pesticides used in these experimental studies, while significant, often reflects levels encountered by individuals with direct and intense exposure, such as those actively spraying pesticides. This raises a pertinent question: what are the risks associated with the residual pesticides found on conventionally grown produce, and does choosing organic for cancer prevention justify the potential investment?
The Pervasiveness of Pesticides in the Food Supply
Pesticides are ubiquitous in the modern food system. Studies have consistently detected pesticides in the blood and urine of a vast majority of the U.S. population, irrespective of their occupational or residential circumstances. The primary route of exposure for the general public is through dietary intake. Crossover trials, where participants alternate between consuming conventionally grown and organically produced foods, have demonstrated a direct correlation between dietary choices and urinary concentrations of pesticide metabolites. This "on-and-off switch" phenomenon clearly illustrates the impact of food consumption patterns on internal pesticide levels, though it does not automatically equate to immediate harm.
The long-term health consequences of ingesting these residual pesticide levels from conventionally grown foods remain an area of ongoing scientific inquiry. However, emerging research is beginning to shed light on potential associations.

Organic Food Consumption and Cancer Risk: Emerging Findings
A significant recent study has provided compelling data on the association between organic food consumption and cancer risk. This research, the first of its kind to systematically evaluate this link while controlling for a wide array of confounding factors, found that individuals who reported the highest frequency of organic food consumption exhibited approximately a 25% lower risk of developing cancer.
The study’s robustness lies in its meticulous control for numerous variables that could influence cancer risk. Researchers accounted for factors such as age, affluence, educational attainment, body mass index, physical activity levels, meat consumption, and smoking habits. Even after adjusting for these widespread determinants of health, the association between higher organic food consumption and reduced cancer risk persisted.
Further analysis explored potential dietary confounders. The researchers investigated whether the observed protective effect could be attributed to other dietary differences, such as a generally higher intake of fruits and vegetables or a lower consumption of processed foods among organic consumers. Despite these adjustments, the significantly lower cancer risk in organic consumers remained evident. The study’s conclusion was unequivocal: "Our results indicate that higher organic food consumption is associated with a reduction in the risk of overall cancer."
Earlier Studies and Nuances in Findings
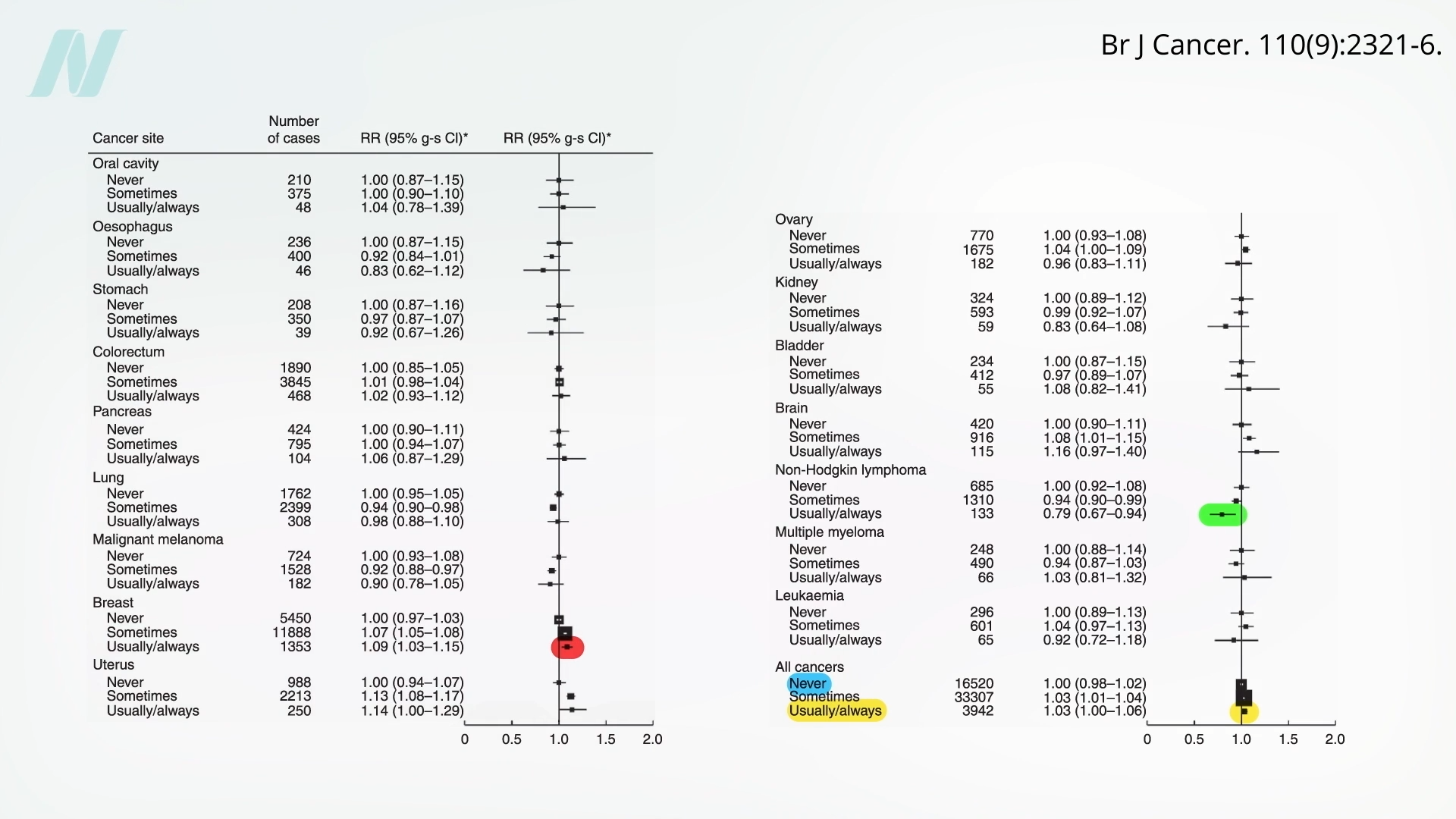
While the recent study offers a strong indication, it is important to consider the broader landscape of research, including earlier investigations. An earlier, larger study examined the association between organic food consumption and cancer incidence. This research found limited evidence for a reduction in overall cancer incidence, with a potential exception noted for non-Hodgkin lymphoma.
However, this earlier study also identified some nuanced findings. When analyzing the data, researchers observed no significant difference in overall cancer rates between individuals who never consumed organic foods and those who consumed them regularly. The only statistically significant associations found were a reduced risk of non-Hodgkin lymphoma and, intriguingly, an increased risk of breast cancer diagnoses.
The potential increase in breast cancer diagnoses among organic consumers in this earlier study warrants careful consideration. Researchers hypothesized whether this observed association could be linked to greater conscientiousness among organic consumers regarding breast cancer screening practices. This heightened vigilance might lead to earlier detection and diagnosis, potentially creating an artificial inflation in the observed incidence rate rather than a true increase in cancer development. This highlights the complexity of epidemiological research and the importance of considering behavioral factors alongside dietary choices.
Beyond Cancer: Pesticides and All-Cause Mortality
The concern surrounding pesticide exposure extends beyond cancer to encompass all-cause mortality, representing the risk of premature death from any cause. Research has indicated that elevated blood levels of certain pesticides are associated with a significantly shorter lifespan. One such pesticide, beta-hexachlorocyclohexane, has been directly linked to this phenomenon.
Understanding how to reduce internal levels of these compounds is crucial. Historical studies have provided insights into dietary patterns and their influence on pesticide accumulation. Decades ago, a study comparing a vegetarian mother to her non-vegetarian sister revealed a notable difference in beta-hexachlorocyclohexane levels in breast milk. The vegetarian mother exhibited approximately one-third lower levels of this pesticide compared to her omnivorous sibling.
This observation is consistent with the chemical properties of certain chlorinated pesticides. These compounds are lipophilic, meaning they are fat-soluble. Consequently, they tend to accumulate in fatty tissues and are found most frequently in foods of animal origin, such as meat, dairy products, and eggs.
More recent investigations have continued to explore the link between dietary patterns and the accumulation of pesticide-related compounds. While not specifically focusing on beta-hexachlorocyclohexane, a contemporary study examined polychlorinated biphenyls (PCBs), another class of persistent organic pollutants. This research found PCBs to be linked to increased mortality risk, with these toxins concentrated in the same types of foods: eggs, dairy products, and animal fats.

The blood of individuals following a vegan diet was found to be "significantly less polluted than omnivores" with respect to a range of PCBs associated with increased mortality. However, this study did not find lower levels of beta-hexachlorocyclohexane in vegans, suggesting that different classes of pesticides may be influenced by dietary choices in distinct ways.
Practical Implications and Dietary Recommendations
The cumulative scientific evidence suggests a clear directive for individuals concerned about the adverse health effects of pesticides and pesticide-like compounds: reducing the intake of animal products may be a prudent strategy. These products appear to be significant reservoirs for certain fat-soluble toxins.
However, when it comes to fruits and vegetables, the landscape shifts. The overwhelming consensus among public health experts and nutritionists is that the benefits of consuming conventionally grown produce likely outweigh any potential risks associated with pesticide residues. The nutritional advantages derived from a diet rich in fruits and vegetables—including essential vitamins, minerals, fiber, and antioxidants—confer substantial health benefits, far exceeding the marginal risks posed by the low levels of pesticides typically found on these foods.
Concerns about pesticide residues on produce should not deter individuals from consuming adequate quantities of fruits and vegetables. The potential lifelong damage from these residues has been estimated to be minimal, shaving off only a few minutes from a person’s life on average. This impact is negligible when contrasted with the profound and well-documented health benefits associated with a diet abundant in fruits and vegetables. Therefore, maximizing the intake of these nutrient-dense foods remains a cornerstone of a healthy lifestyle, irrespective of whether they are conventionally or organically grown.
Future Directions and Ongoing Research
The ongoing research into the complex interplay between pesticide exposure, dietary choices, and health outcomes is vital. Future studies will likely focus on more granular analyses of specific pesticide types, their metabolic pathways within the human body, and their differential impacts on various populations. Furthermore, longitudinal studies that track individuals over extended periods, meticulously documenting dietary habits and health trajectories, will be crucial for solidifying our understanding of these associations. The development of more sophisticated biomonitoring techniques and the integration of advanced data analytics will also play a significant role in unraveling the intricate connections between our food choices, environmental exposures, and long-term well-being. The pursuit of this knowledge is essential for informing public health policies and empowering individuals to make the most informed decisions for their health.


