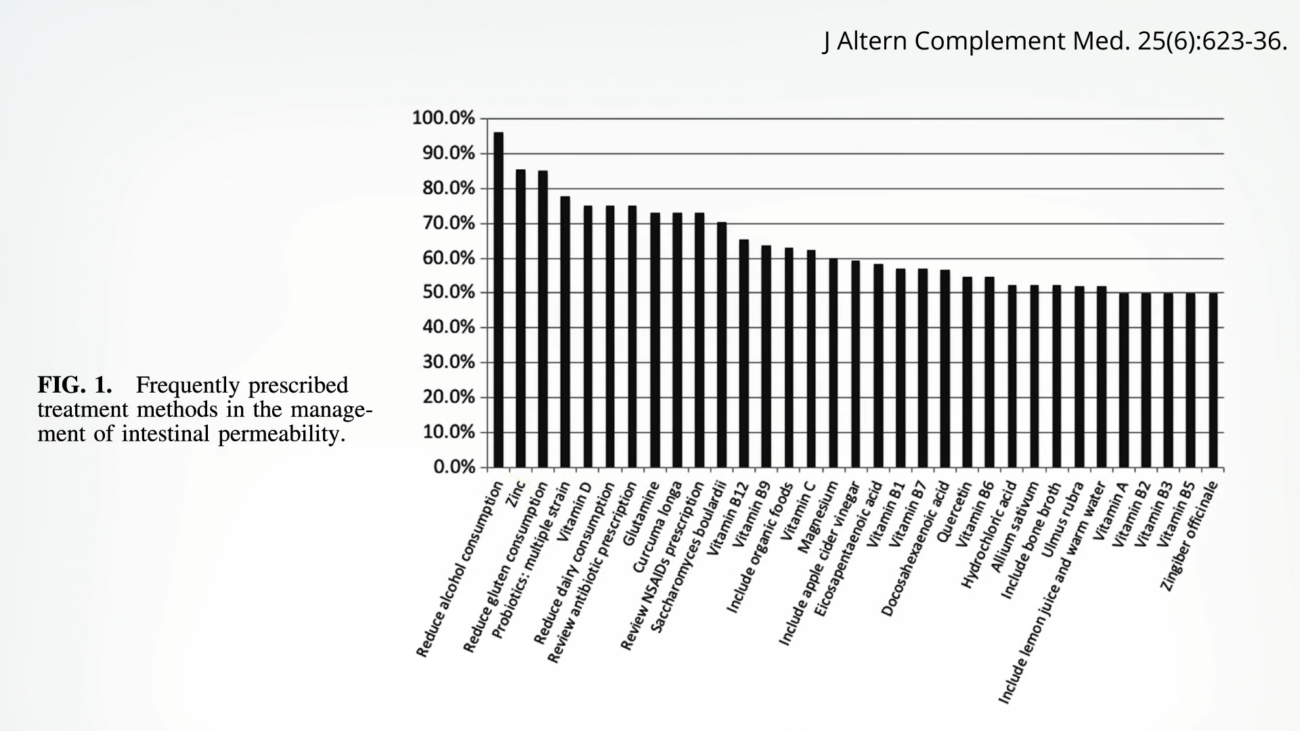
The human intestinal tract, a formidable barrier separating the internal body from the external environment, plays a critical role in regulating nutrient absorption and preventing the entry of harmful substances. This intricate system, responsible for processing a significant portion of our daily environmental exposure, relies on its impermeability to maintain health. However, disruptions to this delicate balance, often exacerbated by dietary choices, can lead to a compromised intestinal barrier, commonly referred to as "leaky gut." This condition allows undigested food particles, microbes, and toxins to permeate the gut lining, potentially triggering systemic inflammation and a cascade of health issues. Understanding the dietary components that can fortify this vital barrier is crucial for preventing and managing leaky gut syndrome.
The Western Diet and Gut Dysbiosis
The prevalence of the Standard American Diet (SAD), also known as the Western diet, has been increasingly linked to the disruption of the gut microbiome, a phenomenon known as gut dysbiosis. This imbalance in the composition and function of gut bacteria can lead to chronic inflammation within the intestinal tract and a weakened intestinal barrier. The consequences of this permeability are far-reaching, as it allows unwanted substances to enter the bloodstream, potentially initiating or exacerbating systemic inflammatory responses.
Historically, the Western diet, characterized by its high intake of processed foods, refined sugars, unhealthy fats, and a low consumption of fruits, vegetables, and whole grains, has been associated with numerous chronic diseases. Research published in journals like Nature and Cell Host & Microbe has consistently highlighted the detrimental effects of such dietary patterns on the gut microbiome. Gut dysbiosis, stemming from this dietary imbalance, is not merely an inconvenience but a significant factor contributing to the rise of conditions such as inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), autoimmune disorders, and metabolic syndrome.
The Power of Plant-Based Nutrition
Emerging research suggests that a predominantly vegetarian diet, rich in plant-based foods, offers a powerful countermeasure against gut dysbiosis and intestinal inflammation. Studies have indicated that individuals adhering to vegetarian diets often exhibit a more balanced gut microbiome, characterized by higher bacterial diversity and enhanced integrity of the intestinal barrier. This is attributed, in part, to the lower levels of harmful uremic toxins, such as indole and p-cresol, commonly found in the digestive systems of vegetarians.
Fiber, a cornerstone of plant-based diets, serves as the primary fuel source for beneficial gut bacteria. When these bacteria metabolize fiber, they produce short-chain fatty acids (SCFAs), such as butyrate, acetate, and propionate. These SCFAs play a crucial protective and nourishing role for the cells lining the intestinal wall, acting as a vital nutrient source that helps maintain the structural integrity of the intestinal barrier. The fermentation of dietary fiber by the gut microbiome leads to the production of these beneficial compounds, underscoring the "prime importance" of plant fiber in preserving gut health.
A landmark study involving patients with non-alcoholic fatty liver disease (NAFLD) provided compelling evidence for the benefits of a plant-rich diet. Over a six-month period, participants who consumed whole grains, beans, lentils, fruits, vegetables, nuts, and seeds experienced a significant reduction in zonulin levels. Zonulin is a protein that plays a key role in regulating the permeability of the intestinal barrier by influencing the tight junctions between intestinal cells. Elevated zonulin levels are considered a primary indicator of a compromised intestinal barrier, making it a valuable biomarker for assessing "leaky gut." The observed reduction in zonulin in this study suggests that a diet abundant in whole, healthy plant foods can effectively help maintain the proper structure and function of the intestinal barrier.

The Role of Dietary Fiber in Intestinal Barrier Function
While the benefits of a plant-rich diet are evident, the specific contribution of dietary fiber to improving gut permeability has been a subject of ongoing scientific inquiry. Early observational studies, while suggestive, often lacked the rigorous controls necessary to establish a definitive cause-and-effect relationship. The aforementioned study on NAFLD patients, for instance, did not include a control group, prompting researchers to cautiously state that "gut permeability might be improved by dietary fiber."
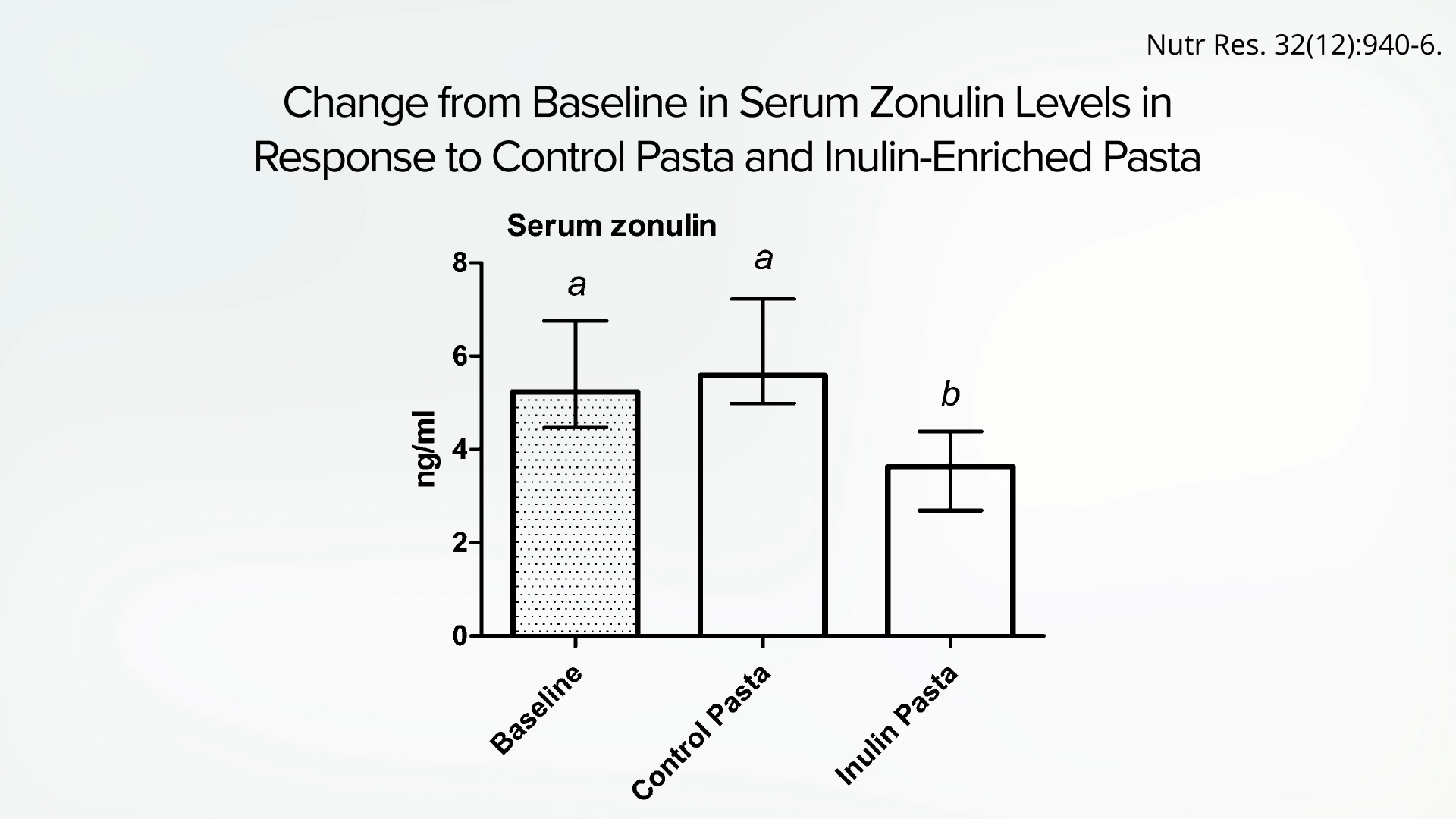
To address this, researchers sought to conduct more definitive studies. A randomized, double-blind, crossover study provided crucial evidence by comparing the effects of pasta with and without added fiber in healthy young men. The results were significant: participants who consumed pasta fortified with added fiber exhibited a notable decrease in zonulin levels compared to their pre-intervention levels and to those in the control group. This robust finding strongly supports the notion that fiber intake directly contributes to reducing intestinal leakiness and enhancing barrier function. This scientific breakthrough, first highlighted in the video "How to Heal a Leaky Gut with Diet," offers concrete evidence for the therapeutic potential of dietary fiber.
The implications of this research are substantial for public health recommendations. As the global burden of chronic inflammatory diseases continues to rise, understanding the precise mechanisms by which diet influences gut health becomes paramount. The consistent demonstration of fiber’s positive impact on zonulin levels suggests that increasing fiber intake through whole grains, legumes, fruits, and vegetables should be a cornerstone of dietary interventions aimed at preventing and managing leaky gut syndrome.
Specific Plant-Based Compounds with Protective Effects
Beyond fiber, certain plant-derived compounds have demonstrated promising capabilities in protecting and repairing the intestinal barrier. Curcumin, the vibrant yellow pigment found in turmeric, has shown remarkable efficacy in preclinical studies. Research on rats indicated that curcumin can help prevent intestinal damage induced by non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen. Similarly, sulforaphane, a compound abundant in cruciferous vegetables such as broccoli, has exhibited protective effects against intestinal damage in mice.
While human studies on broccoli’s direct impact on gut health are still emerging, a notable study involving turmeric consumption in humans provided encouraging results. Participants who consumed the equivalent of two to three teaspoons of turmeric daily for three days experienced a reduction in markers of gastrointestinal barrier damage and inflammation triggered by strenuous exercise. This study, published in Clinical and Translational Gastroenterology, suggests that even moderate doses of turmeric can offer protective benefits. Further research is ongoing to determine the optimal dosage and long-term effects of curcumin and sulforaphane on human intestinal health.
The identification of these specific phytonutrients highlights the complex synergy within whole plant foods. It is not solely the fiber content but also the intricate array of bioactive compounds that contribute to their therapeutic effects. This underscores the importance of consuming a diverse range of plant-based foods to harness the full spectrum of their health-promoting properties.
The Role of Zinc in Gut Barrier Integrity
In the realm of alternative medicine, zinc consistently ranks high on lists of recommended treatments for leaky gut, often cited alongside the reduction of alcohol consumption. Scientific investigation has begun to validate these traditional observations. Zinc is known to possess properties that protect against drug-induced intestinal damage. Studies have shown that in rats, zinc supplementation can mitigate the adverse effects of NSAIDs on the intestinal lining.
A randomized trial involving healthy adults further solidified zinc’s protective role. When participants were administered indomethacin, a potent NSAID known to increase gut permeability, a significant threefold rise in intestinal permeability was observed. However, this increase was entirely prevented when participants also received zinc supplementation. This finding strongly suggests a protective effect of zinc on the small intestine.
While the dose of zinc used in this particular trial was substantial (75 mg per day), nearing twice the tolerable upper daily intake, subsequent research has indicated that even lower doses can be effective. A study published in the Journal of Nutritional Biochemistry found significant improvements in gut leakiness with a dose of just 3 mg of zinc. This suggests that relatively modest zinc supplementation, or even increased dietary intake, could offer meaningful benefits for intestinal barrier function.
For individuals seeking to increase their dietary zinc intake, incorporating zinc-rich foods is a viable strategy. For example, one cup (200g) of cooked lentils can provide an additional 3 mg of zinc to the daily diet. Other excellent dietary sources of zinc include lean meats, poultry, seafood, beans, nuts, and whole grains. Ensuring adequate zinc levels through a balanced diet or targeted supplementation, under professional guidance, can be a key component of a comprehensive strategy for healing a leaky gut.
Broader Implications and Future Directions
The growing body of scientific evidence underscores the profound impact of diet on intestinal barrier function and overall health. The shift from a Westernized diet towards a plant-rich, fiber-sufficient eating pattern, complemented by specific micronutrients like zinc, offers a promising avenue for preventing and managing leaky gut syndrome and its associated inflammatory conditions.
The implications extend beyond individual health, influencing public health policy and dietary guidelines. As research continues to unravel the intricate interplay between the gut microbiome, diet, and disease, a more personalized and preventative approach to healthcare is becoming increasingly feasible. Further research is needed to explore the long-term efficacy of various dietary interventions, optimal dosages of specific nutrients, and the potential for synergistic effects between different food components.
The consistent findings across multiple studies, from observational analyses of vegetarian diets to randomized controlled trials on dietary fiber and zinc, provide a strong foundation for recommending dietary modifications as a primary strategy for promoting gut health. By empowering individuals with knowledge about the foods that strengthen their intestinal barrier, we can collectively move towards a future where chronic inflammatory diseases are more effectively prevented and managed.
Doctor’s Note: For further exploration into preventing gut dysbiosis and leaky gut, readers are encouraged to consult resources such as "Flashback Friday: Gut Dysbiosis: Starving Our Microbial Self" and "Avoid These Foods to Prevent a Leaky Gut," which offer additional insights and actionable advice.