The allure of personalized nutrition, a field promising dietary advice tailored to an individual’s unique biological makeup, is undeniable. Rooted in the intuitive concept that "one size does not fit all," this approach taps into a deep-seated human desire for individuality and special consideration. This inherent appeal has fueled a burgeoning industry, from customized food products to direct-to-consumer genetic testing services offering bespoke dietary recommendations. However, a closer examination reveals a complex landscape where the promise of hyper-individualized diets may overshadow the fundamental importance of personal responsibility for one’s health.
The Allure of Uniqueness and the Rise of Personalized Nutrition
The marketing of personalized nutrition often hinges on the idea that genetic predispositions, microbiome compositions, and other biological markers dictate optimal dietary intake. This resonates deeply with consumers, fostering a sense of empowerment and control over their health outcomes. The concept is so potent that it has spurred innovation in food technology, with 3D food printing emerging as a potential avenue for highly customized meal preparation. The underlying sentiment is that by understanding our unique biological blueprint, we can unlock unprecedented levels of health and well-being.
Legitimate Differences: When Personalization is Essential
It is crucial to acknowledge that genuine individual differences do necessitate tailored nutritional approaches. Severe allergies, such as peanut allergies, require strict avoidance and personalized management plans. Similarly, individuals with celiac disease must meticulously avoid gluten, and those with lactose intolerance require dairy-free alternatives. These are clear-cut examples where personalization is not a luxury but a medical necessity.
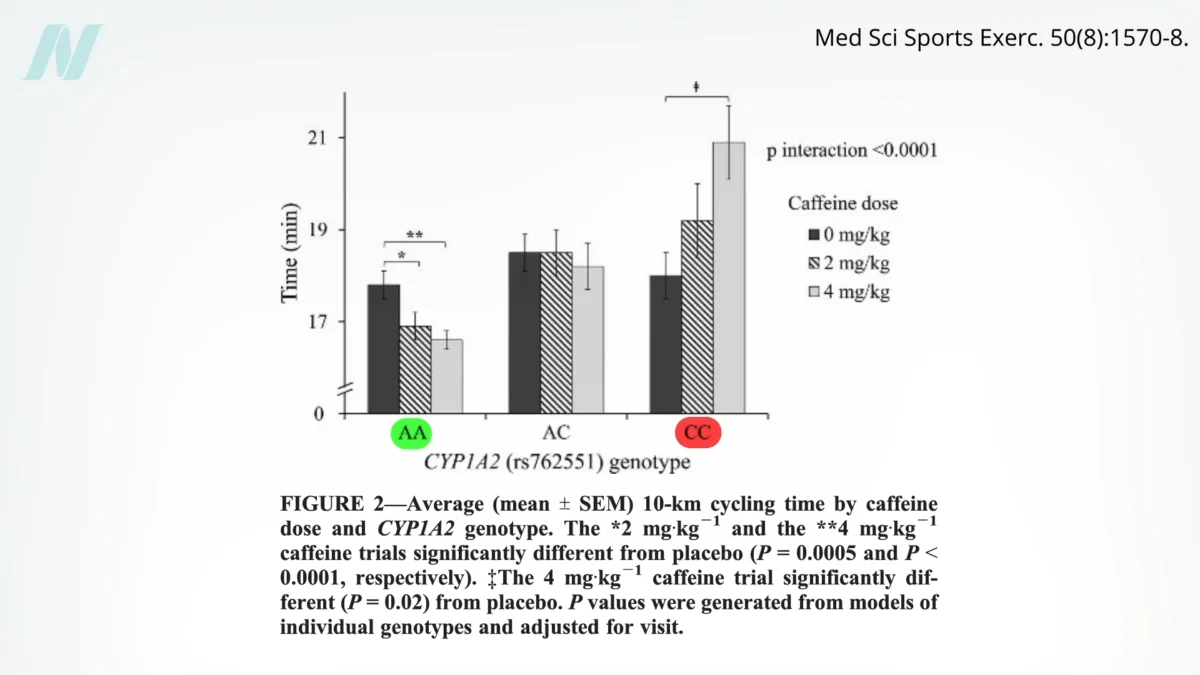
Beyond these well-established conditions, emerging research highlights other areas where genetic variations can influence nutrient metabolism and health benefits. For instance, studies have explored the differences in how individuals metabolize caffeine. Research, including investigations into caffeine metabolism and its impact on athletic performance, suggests that genetic variations in the enzymes responsible for breaking down caffeine can significantly alter its ergogenic effects. Some individuals, classified as "fast metabolizers," may experience performance enhancements, such as improved cycling times, from caffeine consumption. Conversely, "slow metabolizers" might see no benefit or even a performance detriment. These findings, while illustrating a tangible link between genetics and dietary response, represent a specific niche within the broader spectrum of nutritional science.
The Overlap of Similarity: A Foundation for General Health
Despite these legitimate individual variations, it is increasingly apparent that for the vast majority of the population, our physiological similarities far outweigh our differences when it comes to fundamental nutritional needs. The human body, across diverse populations, shares a common architecture and a largely consistent set of requirements for essential macronutrients and micronutrients. This underlying biological commonality forms the bedrock of public health recommendations and evidence-based dietary guidelines.
The Proliferation of Direct-to-Consumer Genetic Testing: Hype or Help?
The surge in direct-to-consumer genetic testing companies offering personalized nutrition advice presents a significant area of concern. These companies often market their services by claiming to optimize micronutrient status based on a limited number of genetic variants. However, scientific consensus suggests that many of these variants explain only a minuscule fraction of the variability in nutrient levels between individuals. The extrapolation of such limited genetic data into broad dietary recommendations can be misleading, creating a false sense of scientific certainty where it may not exist.
Personalized Medicine and the Challenge of Complex Diseases
Personalized nutrition is often framed within the broader context of personalized medicine, also known as precision medicine. This movement is driven by a powerful cultural desire for individual control over health, encompassing diagnosis, treatment, and prevention. While precision medicine holds immense promise for monogenetic diseases – rare conditions caused by a single gene defect, such as hemophilia or sickle cell anemia – its application to complex, multifactorial diseases is considerably more challenging.
Most common chronic diseases, including heart disease, diabetes, and many cancers, arise from a complex interplay between numerous genes and a multitude of environmental factors, including lifestyle. This intricate web of influences poses a significant hurdle for the straightforward implementation of personalized medical and nutritional strategies based solely on genetic information.
Unpacking the Genetics of Complex Traits: Height as a Case Study
The study of complex human traits, such as adult stature, offers a compelling illustration of this complexity. Researchers have identified at least 40 chromosomal locations associated with human height, a trait strongly influenced by genetics. While parental genes account for approximately 80% of the difference in height between individuals, the dozens of identified genes collectively explain only about 5% of this variation. This discrepancy highlights a critical point: identifying genetic associations is a far cry from predicting individual outcomes with high precision.

Genome-wide association studies (GWAS), a common methodology in this field, scan entire genomes to identify statistical links between diseases and specific DNA sequences. While these studies are valuable for understanding broad genetic predispositions, companies marketing genetic susceptibility tests often reinterpret these findings as predictive of individual risk. In reality, these tests typically reveal modest genetic associations with slight increases in disease risk, dwarfed by the more significant contributions of lifestyle behaviors. The scientific community largely agrees that using an individual’s DNA to predict disease risk currently provides "little to no useful information" for guiding preventative strategies.
The Enduring Primacy of Lifestyle: A Universal Prescription
Consider a scenario where genetic analysis indicates a slightly elevated risk for a particular health condition. The advice typically dispensed – to exercise regularly, maintain a healthy weight, moderate alcohol consumption, and consume a diet rich in fruits, vegetables, and whole grains – is sound and universally applicable. These are not personalized recommendations; they are foundational principles of healthy living that benefit everyone, regardless of their genetic makeup.
The stark reality is that the majority of individuals do not consistently adhere to these basic, well-established health recommendations. Nationwide surveys consistently reveal that nearly all populations, including a significant portion of the United States, consume diets that fall short of even modest dietary guidelines. The phrase "almost nobody lives this way" is not an exaggeration but a reflection of widespread adherence challenges to fundamental health practices. This pervasive gap between knowledge and action underscores a critical public health challenge: prioritizing widespread adoption of proven lifestyle interventions over the pursuit of highly personalized, and often unproven, strategies.
The Absurdity of Hyper-Personalization in Public Health
When confronted with the widespread failure to adopt even the most basic, universally beneficial health behaviors, the focus on hyper-personalizing preventive strategies based on genetic risk information begins to appear, as some experts suggest, "on the verge of absurdity." The emphasis should arguably shift from the intricate details of individual genetic code to the fundamental, evidence-based pillars of health: a balanced diet, regular physical activity, adequate sleep, and stress management.
The Caffeine Metabolism Case Study Revisited
To illustrate the nuanced reality of personalized nutrition, consider the video "Friday Favorites: Do the Health Benefits of Coffee Apply to Everyone?" This resource delves into the fascinating differences in caffeine metabolism and its impact on health and athletic performance. As mentioned earlier, the ability to rapidly metabolize caffeine can unlock its ergogenic potential for athletes, leading to measurable improvements in performance. However, for slow metabolizers, the effects can be negligible or even negative.
This example highlights a specific, scientifically validated instance where individual genetic variation plays a direct role in dietary response. It underscores the potential for personalized nutrition in certain well-defined contexts. However, it also serves as a reminder that such clear-cut cases are not the norm for the vast majority of nutritional advice. The video, available on NutritionFacts.org, provides a visual and data-driven exploration of this specific genetic influence on health outcomes.
The Broader Implications: Shifting the Focus
The current discourse surrounding personalized nutrition, while appealing to our desire for individuality, risks diverting attention and resources from foundational public health initiatives. The commercialization of genetic testing for nutritional guidance, often based on limited scientific evidence, raises concerns about consumer exploitation and the potential for misinformation.
Instead of solely pursuing the intricacies of individualized dietary plans, a more impactful approach may involve:
- Reinforcing Evidence-Based Guidelines: Greater emphasis on promoting universally recognized healthy eating patterns, such as those advocated by major health organizations, is essential.
- Addressing Behavioral Barriers: Understanding and overcoming the psychological and societal factors that prevent individuals from adopting healthy lifestyles is paramount.
- Investing in Education: Empowering the public with accurate, accessible information about nutrition and health, dispelling myths, and fostering critical thinking about health claims.
- Targeted Personalization: Focusing personalized approaches on specific, well-researched areas where genetic or other biological factors demonstrably influence health outcomes, such as in the case of severe allergies or specific metabolic disorders.
The future of optimal health likely lies not in a complex, individually tailored genetic code, but in a renewed commitment to the fundamental principles of well-being that have been scientifically validated for decades. The ultimate power to achieve and maintain good health rests not solely on what science can decipher about our unique biology, but on the personal responsibility we take in adopting and sustaining healthy lifestyle behaviors.