The pursuit of a slimmer physique has, throughout history, spurred innovation, but not always in directions that prioritize safety and long-term well-being. In an era saturated with quick-fix promises, a critical examination of various weight-loss methodologies reveals a spectrum ranging from the superficially superficial to the surgically invasive and the neurologically complex. While the desire to shed pounds is a deeply personal and often health-driven endeavor, the methods employed can sometimes venture into territory that raises significant ethical and medical concerns. This exploration delves into some of the more unconventional and often alarming approaches to weight reduction, highlighting their underlying mechanisms, documented outcomes, and the broader implications for public health and medical ethics.
The fundamental challenge in weight management often lies in the delicate balance between caloric intake and expenditure. For an individual of moderate obesity engaging in moderately intense physical activity, such as cycling or brisk walking, the calorie burn can be approximately 350 calories per hour. However, the ease with which high-calorie, low-nutrient foods and beverages are consumed presents a formidable obstacle. A mere five minutes dedicated to snacking on processed items, which can contain around 70 calories (293 kJ) per minute, can effectively negate an entire hour of strenuous exercise. This stark disparity underscores the pervasive difficulty individuals face in achieving a caloric deficit through lifestyle changes alone, and it is this chasm that often drives the search for more radical interventions.
The AspireAssist Siphon: A Surgical Solution to Caloric Intake
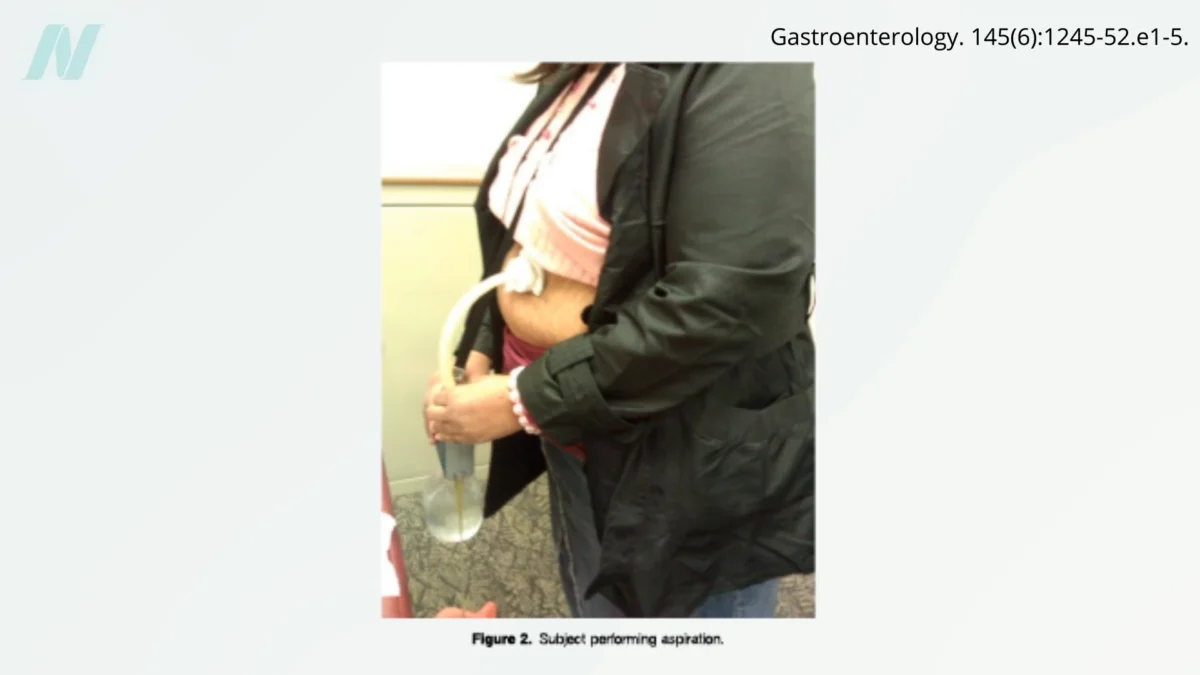
Emerging as a stark example of such radical interventions is the AspireAssist siphon assembly. This device represents a significant surgical undertaking, involving the creation of a percutaneous gastrostomy. In essence, surgeons surgically create an opening in the stomach and establish a tunnel, known as a fistula, through the abdominal wall. This allows individuals, post-meal, to attach a specialized suction device to the opening and directly drain a portion of their stomach contents. The procedure, requiring a surgical intervention to create a direct pathway from the stomach to the exterior, fundamentally alters the body’s natural digestive process.
The implications of such a system are profound, enabling individuals to consume food and then, through the external apparatus, remove a substantial portion of it before full digestion and nutrient absorption can occur. This effectively allows for the consumption of calories followed by their immediate expulsion, a concept that has drawn both fascination and considerable ethical debate. While patients utilizing this method have demonstrated weight loss, the contributing factors are multifaceted. The presence of the fistula may interfere with the natural relaxation of the stomach wall during eating, potentially leading to earlier feelings of fullness. Furthermore, the protocol necessitates significant fluid intake and thorough chewing, behaviors that can aid weight loss by promoting hydration and slowing the rate of consumption. Anecdotal reports also suggest that patients often modify their food choices to avoid the visually unappealing prospect of expelling processed or unhealthy foods, indirectly encouraging healthier eating habits.
However, the medical considerations are substantial. Because stomach juices, rich in essential electrolytes like potassium, are siphoned out, patients must supplement their diet with potassium to prevent deficiencies, a complication also observed in individuals with bulimia nervosa. While serious adverse effects such as abdominal abscesses are reported to be rare, minor wound complications are not uncommon. The primary selling point of the AspireAssist, from a medical device perspective, is that it does not alter the fundamental anatomy of the gastrointestinal tract. In the context of the ever-evolving and sometimes unregulated world of weight-loss procedures, this non-anatomical alteration is presented as a significant advantage.
The Duodenal-Jejunal Bypass Liner: An Invasive Approach to Calorie Absorption
Another intervention that bypasses traditional surgical alterations to the digestive tract, yet introduces its own set of risks, is the duodenal-jejunal bypass liner. Traditional gastric bypass surgery involves the physical removal or rerouting of sections of the digestive system to reduce calorie absorption. In contrast, the duodenal-jejunal bypass liner, such as the EndoBarrier, involves the insertion of a flexible plastic tube, approximately two feet in length, that lines the intestinal walls. The intended mechanism is to create a barrier that prevents the direct contact of food with the intestinal lining, thereby inhibiting nutrient absorption.
The primary challenge with this device lies in its method of fixation. The liner is anchored within the digestive tract using multiple barbed hooks, a design intended to secure it in place. However, these hooks have been implicated in a significant number of adverse events. Data from studies involving over a thousand patients indicate a high incidence of lacerations and other complications directly attributable to these anchoring mechanisms. Nearly nine out of every ten patients have experienced adverse effects, with severe instances, including esophageal perforation and liver abscesses, occurring in approximately one in twenty-seven individuals. These figures highlight the inherent risks associated with introducing a foreign object with mechanical anchoring points into the delicate environment of the human digestive system.
Exploring Other Extreme and Questionable Methods
The landscape of extreme weight-loss techniques extends beyond surgical and device-based interventions, encompassing a range of often dubious and sometimes dangerous practices.

Intestinal "Resurfacing" and Thermal Ablation
Concerns regarding the palatability and efficacy of devices like the AspireAssist have led to investigations into even more drastic endoscopic procedures. Among the most unsettling is a technique referred to as intestinal "resurfacing," which involves the thermal ablation of the superficial duodenal mucosa. In layman’s terms, this procedure entails burning off the lining of the intestines, with the intention of preventing calorie absorption. While proponents may frame this as "resurfacing," the reality is the intentional destruction of a vital mucosal layer, raising profound questions about long-term digestive health and the body’s ability to heal and regenerate such tissue. The potential for scarring, inflammation, and impaired nutrient absorption in the long term remains a significant area of concern.
Botox Injections into the Stomach
In a more recent, albeit ultimately unsuccessful, attempt to curb appetite and slow digestion, researchers have explored the injection of Botulinum toxin (Botox) into the stomach walls of obese individuals. The rationale behind this approach was to partially paralyze the gastric muscles, thereby slowing the emptying of the stomach and promoting a prolonged feeling of fullness. The hope was that this physiological change would lead to reduced food intake and subsequent weight loss. However, clinical trials and subsequent analyses have indicated that this method has not proven effective in achieving significant or sustainable weight reduction in human subjects. The complex interplay of gastric motility, hormonal signals, and satiety is not sufficiently modulated by localized Botox injections to overcome the multifaceted drivers of obesity.
The Inefficacy of Corsets for Weight Loss
Historically, restrictive garments have been employed for aesthetic purposes, and in some instances, proponents have suggested their utility in weight management. A study conducted in Sweden investigated the potential of wearing corsets for extended periods – 12 to 16 hours daily for nine months – as a weight-loss strategy. The findings, however, were largely dismissive of this approach. Participants in the study reported that the corsets were "perceived as uncomfortable," leading to inconsistent adherence. This highlights a fundamental limitation of externally applied restrictive measures: they often fail to address the underlying behavioral and physiological factors contributing to weight gain and are typically abandoned due to discomfort or practicality.
The Perilous Promise of Tapeworms
Perhaps one of the most historically notorious and unequivocally dangerous weight-loss fads involves the ingestion of tapeworm eggs. Advertised as a remedy as far back as the early 20th century, "sanitized tapeworms" were purported to reside in the digestive tract, consuming a portion of ingested calories and thus facilitating weight loss. The disturbing reality is that living tapeworms have been discovered in individuals undergoing bariatric surgery, indicating that infesting oneself with these parasites is not only potentially ineffective but also poses severe health risks. Tapeworms can cause a range of debilitating conditions, including abdominal pain, nausea, diarrhea, malabsorption of nutrients, and, in severe cases, neurological complications if their larvae migrate to the brain. The practice represents a dangerous disregard for health and safety, bordering on self-harm.
Harnessing Disgust as a Weight-Loss Tactic
In a more psychologically driven approach, researchers have explored the use of disgust as a means to reduce the appeal of high-calorie foods. A study titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming" employed subliminal messaging techniques. Participants were exposed to rapid, consciously imperceptible flashes of positive imagery (like kittens) before viewing healthy food items, aiming to create a positive association. Conversely, before being shown images of high-calorie foods, such as ice cream, negative stimuli like cockroaches on pizza, vomit, or burn wounds were flashed. The study reported that subjects subsequently expressed a reduced desire for high-calorie foods, although direct testing of actual consumption was not conducted. The researchers concluded that cultivating subliminal revulsion might offer a novel tactic to counteract the pervasive influence of food cues that promote unhealthy eating habits. This approach, while less physically invasive, taps into the complex relationship between emotion, perception, and dietary choices.
Neurological Interventions and the Quest for Control
The exploration of weight-loss strategies has also ventured into the realm of direct neurological intervention, reflecting a desire to control appetite and food intake at their source.
Electrical Stimulation of the Stomach and Colon
In the United States, significant research has been dedicated to implantable gastric stimulation, involving the insertion of electrodes into the muscular layer of the stomach wall. The aim was to modulate gastric activity and influence satiety signals. However, findings from studies examining this approach have been largely inconclusive or disappointing, failing to demonstrate consistent efficacy in promoting significant weight loss. Following the limited success of gastric stimulation, researchers have also explored electrical stimulation of the colon, though similar challenges in achieving meaningful and sustained weight reduction have been encountered.
Brain Stimulation for Appetite Control
Perhaps the most invasive and ethically contentious area of weight-loss research involves direct brain stimulation. Studies have investigated the effects of repetitive electric brain stimulation on food intake. While placing deep-brain electrodes is an inherently high-risk procedure, scientists have long been intrigued by the possibility of modulating brain activity to reduce appetite. In some experimental approaches, small holes were drilled into the skulls of obese individuals, and electrodes were inserted into specific brain regions. The objective was to identify areas that, when stimulated, could elicit hunger responses. Once such areas were located, researchers applied electrical currents to create lesions, aiming to permanently alter appetite regulation. While this technique showed some promise in animal models like cats and monkeys, its application in obese humans did not result in significant weight loss. This underscores the complexity of the human brain and the intricate biological and psychological factors that govern eating behavior, making direct surgical intervention a risky and often ineffective strategy for weight management.
The Unanswered Question: What Constitutes Sustainable Weight Loss?
The sheer diversity and, in many cases, the extremity of these investigated weight-loss methods highlight a persistent societal challenge: the search for effective and sustainable solutions to obesity. While the allure of rapid results is powerful, the scientific consensus increasingly points towards comprehensive, lifestyle-based approaches. These typically involve a balanced, nutrient-dense diet, regular physical activity, adequate sleep, and effective stress management. The journey to healthy weight loss is rarely a straightforward path and often requires a sustained commitment to behavioral change rather than a reliance on invasive procedures or unproven remedies. As noted by Dr. Greger in his book, How Not to Diet, sustainable weight loss is not a matter of complex brain surgery but rather a consistent application of evidence-based principles. The ongoing exploration of novel interventions, while sometimes yielding scientific insights, must always be balanced against the imperative of patient safety and long-term well-being, ensuring that the pursuit of a healthier body does not lead to undue harm.