Sham surgery trials have revealed that some of the most widely adopted surgical interventions may lack demonstrable efficacy, raising significant concerns about patient care and the evidence base underpinning common medical practices. This investigation delves into the findings of such trials, focusing on procedures like intragastric balloons and orthopedic surgeries, to illuminate the critical need for rigorous, independent evaluation of medical devices and surgical techniques.
The Rise and Fall (and Rise Again) of the Intragastric Balloon
Intragastric balloons, introduced in the 1980s, were heralded as a revolutionary, minimally invasive approach to weight management. These devices were designed to be inserted into the stomach and inflated with air or fluid, occupying a significant portion of the stomach’s volume to promote satiety and reduce food intake. The initial enthusiasm, however, was soon tempered by a stark reality: the surgical device market often sees products launched with insufficient evidence of their effectiveness and safety. The intragastric balloon was a prime example of this pattern.
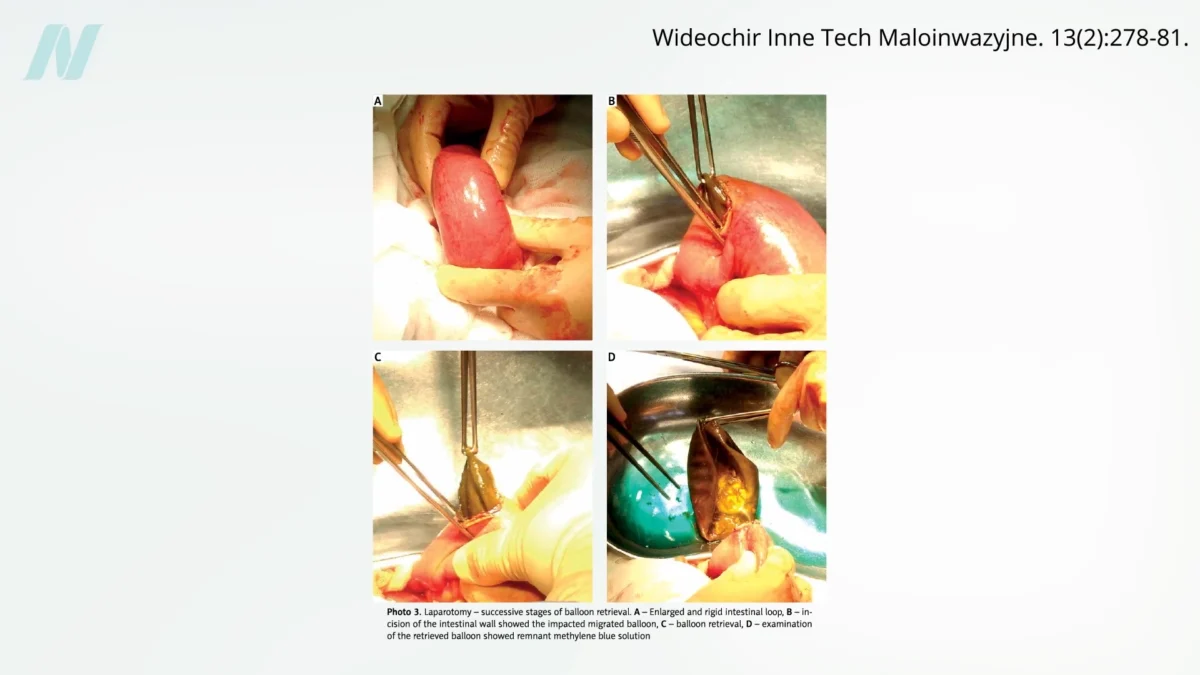
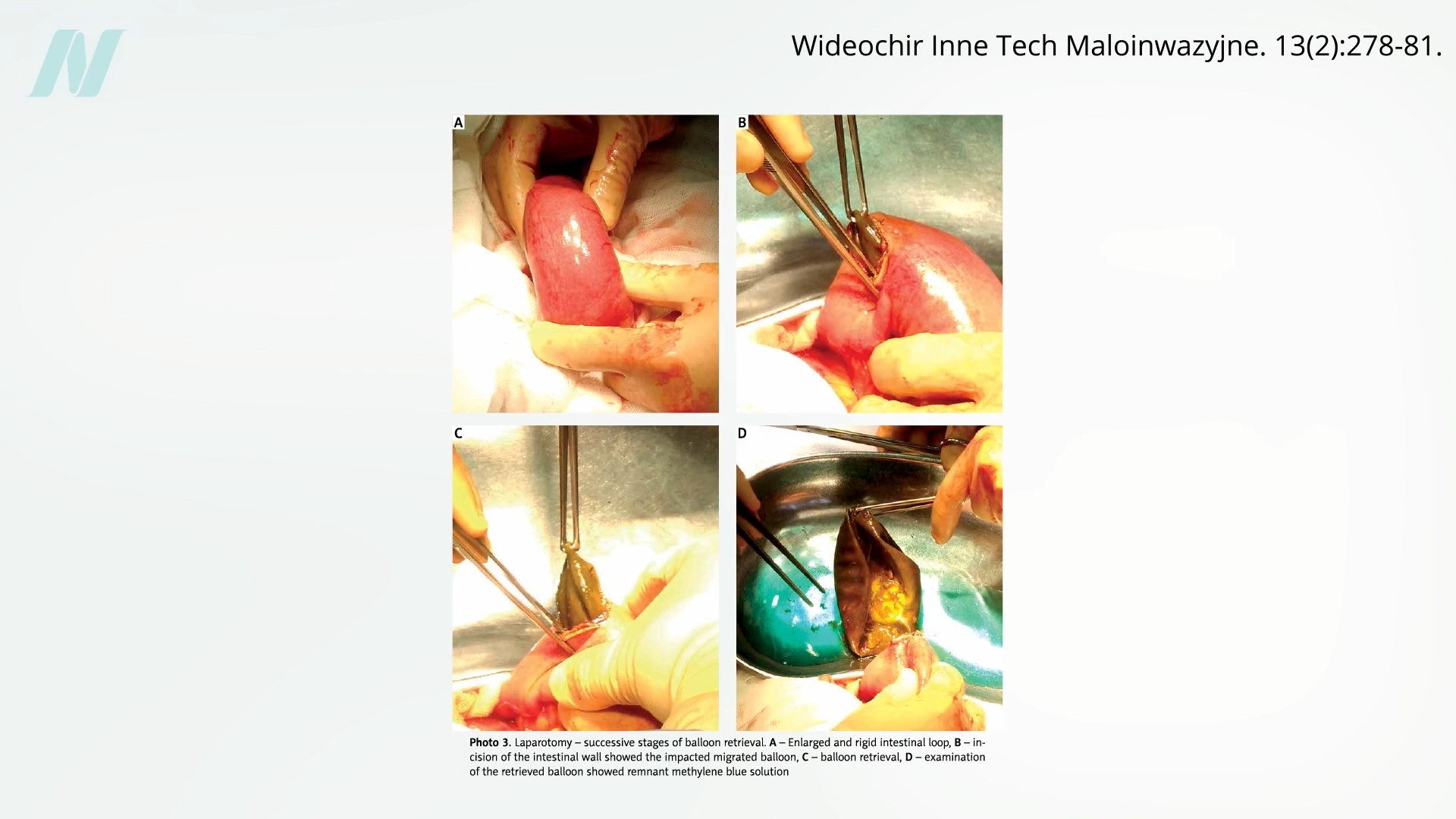
Early studies, including a notable one conducted at the Mayo Clinic, cast a long shadow over the balloon’s purported benefits. This research uncovered a disturbing failure rate, with approximately 80% of the balloons spontaneously deflating. This phenomenon presented a serious, even life-threatening, risk. Deflated balloons could migrate into the intestines, leading to potentially fatal bowel obstructions. Visual evidence from medical imaging and expert commentary, such as that presented in the video "Is Gastric Balloon Surgery Safe and Effective for Weight Loss?", underscores the severity of this complication, highlighting instances where a deflated balloon caused significant intestinal blockage.
Beyond the risk of mechanical complications, the intragastric balloon was also found to be a source of considerable patient distress. Prior to deflation, a significant portion of patients, nearly half, experienced gastric erosions, indicating damage to the stomach lining. More fundamentally, when compared to simpler, non-surgical interventions like dietary changes and behavioral modification strategies, the intragastric balloon failed to demonstrate superior weight-loss outcomes. This lack of clear benefit, coupled with the inherent risks, eventually led to the withdrawal of these devices from the market.

However, the story of intragastric balloons did not end there. Following a hiatus of over three decades, the U.S. Food and Drug Administration (FDA) began approving a new generation of intragastric balloons in 2015. This resurgence coincided with the passage of the Sunshine Act, legislation designed to increase transparency in financial relationships between healthcare providers and the medical industry. The Act mandates the disclosure of payments made by pharmaceutical companies and medical device manufacturers to physicians. While the public has become increasingly aware of the financial ties between doctors and "Big Pharma," the extent of surgeons’ financial relationships with device companies—including those producing devices like gastric balloons—remains a less understood but equally critical issue. Reports indicate that top physicians have received millions of dollars annually from device companies, yet a significant minority of published research originating from these financially intertwined relationships has failed to adequately disclose these conflicts of interest.
While newer intragastric balloons are designed to be reversible, a key advantage over more invasive bariatric surgeries, this reversibility does not equate to safety. The FDA has issued a series of advisories detailing the potential risks associated with these devices, which tragically can include death. The mechanism by which a smooth, rounded object could lead to such severe outcomes is often related to the common and debilitating side effects of nausea and vomiting. In extreme cases, persistent vomiting can exert such pressure that it leads to a rupture of the stomach. These gastrointestinal disturbances are not uncommon, affecting a majority of patients, and may also contribute to life-threatening nutrient deficiencies.
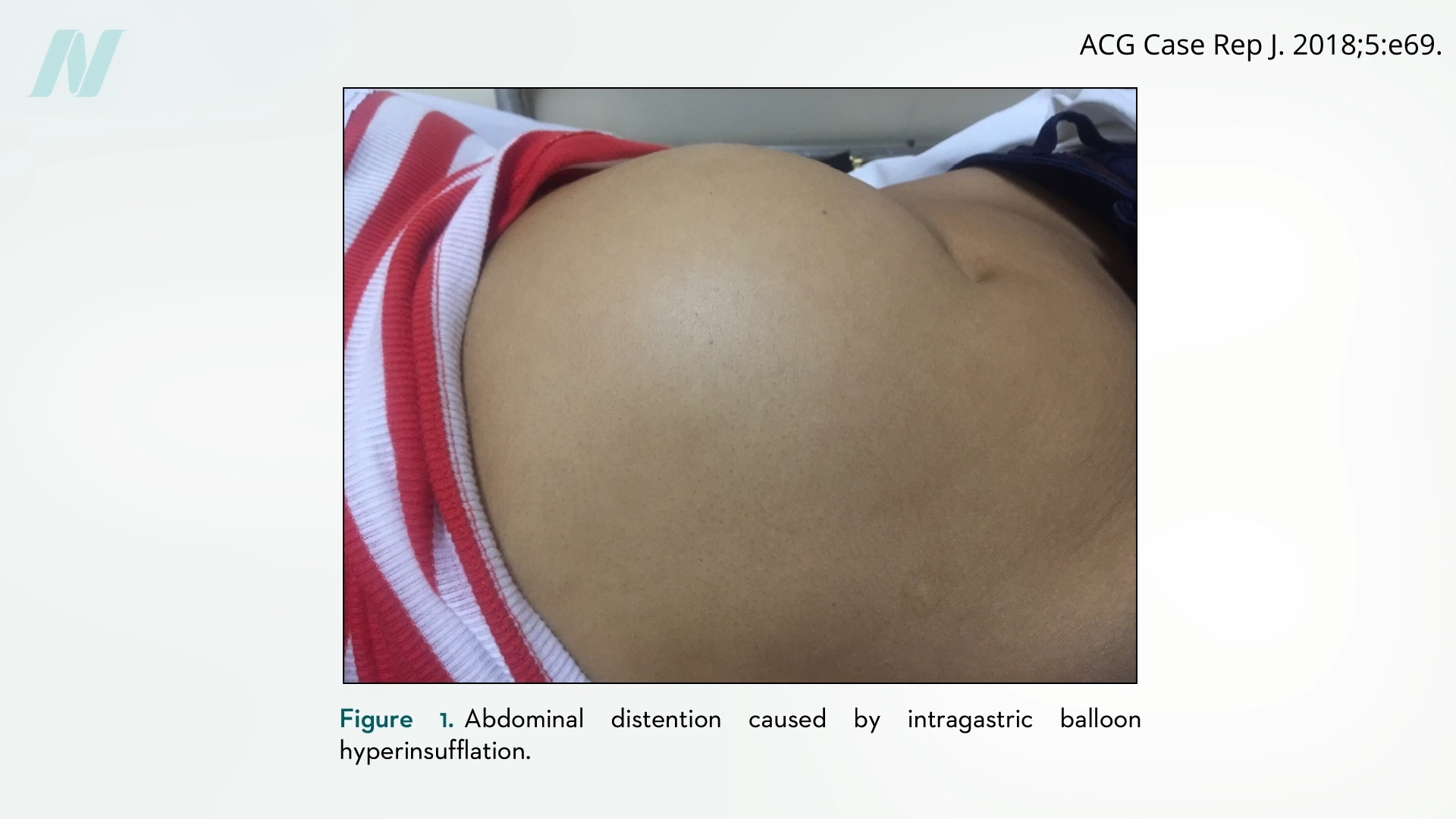
Complications arising from intragastric balloons are not solely linked to deflation. In some instances, devices have been observed to spontaneously overinflate, leading to severe abdominal pain, vomiting, and distention, as illustrated by clinical observations and visual documentation. This phenomenon of spontaneous overinflation, while seemingly counterintuitive for a device designed to occupy space, mirrors earlier concerns raised with other implantable devices, such as breast implants. Reports on "The Phenomenon of the Spontaneously Autoinflating Breast Implant" have documented cases where these devices inexplicably increased in volume, sometimes by over 50%. This "underreported and poorly understood phenomenon" has also been noted in medical literature. Intriguingly, early experimental intragastric balloons were, in fact, developed using principles and designs initially applied to breast implants, highlighting a recurring challenge in medical device innovation.
The Uproar of Sham Surgery Trials: Questioning the Status Quo
The inherent challenge in evaluating the efficacy of surgical procedures lies in isolating the true impact of the intervention from the powerful influence of the placebo effect and the patient-physician relationship. Unlike drug trials, where inert placebos (sugar pills) can be readily administered, surgical interventions present a more complex scenario. To address this, researchers have employed "sham surgery" as a control, a controversial yet informative methodology.
In 2002, a landmark study published in The New England Journal of Medicine scrutinized arthroscopic surgery of the knee, then the most common orthopedic procedure performed globally. Billions of dollars were being invested annually in arthroscopic interventions, involving the insertion of small cameras and surgical instruments to debride damaged tissue in patients suffering from osteoarthritis and knee injuries. The study’s design was audacious: patients experiencing knee pain were randomly assigned to receive either the actual surgical procedure or a sham surgery. In the sham group, surgeons would make incisions into the knee and simulate the surgical steps, including the application of saline to mimic fluid irrigation, without actually performing any therapeutic intervention on the joint.
This trial ignited an immediate and intense controversy within the medical community. Ethical questions were raised about the propriety of exposing patients to the risks of surgery without the intention of providing a therapeutic benefit. Professional medical associations publicly questioned the ethics of the participating surgeons and the sanity of the patients who consented to such a trial. The findings, however, were profoundly illuminating. While patients who underwent the actual surgery experienced improvements, a statistically similar level of improvement was observed in the group that received the sham procedure. This demonstrated that the perceived benefits of arthroscopic knee surgery, at least in this context, were largely attributable to the placebo effect and the natural course of recovery, rather than the surgical intervention itself. The image at 4:42 in the accompanying video visually represents this stark comparison, showing comparable outcomes for both groups.
The implications of this study were far-reaching. It suggested that for a significant number of patients undergoing this ubiquitous procedure, the surgery itself had no discernible therapeutic effect. The study’s findings led to a significant re-evaluation of the indications for arthroscopic knee surgery, with subsequent research and clinical guidelines reflecting a more conservative approach. Today, rotator cuff shoulder surgery is facing a similar crisis of confidence, with sham-controlled trials investigating its efficacy.
Evidence from Intragastric Balloon Trials: A Consistent Pattern of Questionable Benefit
When intragastric balloons were subjected to sham-controlled trials, the results echoed the findings in orthopedic surgery. These rigorous studies revealed that both older and newer iterations of these devices often failed to deliver any statistically significant weight-loss benefit beyond that achieved through placebo effects and associated lifestyle interventions. Even in instances where some weight loss was observed, it was frequently temporary. This is partly attributable to the mandated removal of balloons after six months, a time limit imposed due to escalating deflation risks. Attempts to prolong the use of balloons or to sequentially implant new ones have not yielded improved long-term weight management outcomes. Sham-controlled trials have indicated that any perceived effects on appetite and satiety may diminish over time as the body adapts.
The Broader Implications of "Fake News" in Medicine
The findings from sham surgery trials, when viewed collectively, compel a critical examination of the prevailing medical paradigm. While the medical profession rightly champions evidence-based practice and vigorously counters misinformation, such as the anti-vaccination movement, these trials reveal a concerning susceptibility within medicine to its own form of "fake news" and "alternative facts." When popular surgical procedures, which carry inherent risks and significant financial costs, are demonstrated to be no more effective than placebo interventions, it raises profound questions about the drivers of their continued use.
The financial incentives embedded within the medical device industry, as highlighted by the Sunshine Act disclosures, cannot be overlooked. The substantial payments made to physicians by device manufacturers, coupled with a less-than-perfect record of conflict-of-interest disclosure in published research, create an environment ripe for the perpetuation of potentially ineffective treatments. The medical community’s commitment to scientific rigor and patient well-being necessitates a more robust and transparent system for evaluating the true value of surgical interventions and medical devices.
The implications extend beyond the direct patient impact. The widespread adoption of unproven or marginally effective surgeries diverts significant healthcare resources that could be better allocated to interventions with demonstrable benefits. Furthermore, the erosion of trust that can result from the revelation that popular procedures are, in essence, "shams," can undermine public confidence in the medical establishment.
Moving forward, a greater emphasis on independent, non-industry-funded research, coupled with stringent regulatory oversight and a culture of open disclosure, is paramount. Patients have the right to expect that the medical interventions they undergo are supported by robust scientific evidence of both safety and efficacy. Sham surgery trials, while ethically challenging, have provided invaluable insights into the effectiveness of many common procedures, urging a recalibration of our approach to surgical innovation and patient care.
The subsequent installment of this series, "Extreme Weight-Loss Devices," will further explore the landscape of weight management technologies. For a comprehensive understanding of sustainable weight loss, readers are encouraged to consult resources such as "How Not to Diet," which is dedicated to evidence-based strategies for long-term health.