The landscape of bariatric weight-loss surgery, while offering a powerful tool for individuals struggling with severe obesity, is fraught with potential complications, a significant portion of which may be directly attributable to the surgeon’s proficiency. Recent analyses and studies underscore a critical, yet often overlooked, variable: the surgeon’s technical skill. This factor appears to exert a profound influence on patient outcomes, impacting rates of complications, hospital readmissions, the necessity for reoperations, and even mortality.
The Prevalence of Revisions and Associated Risks
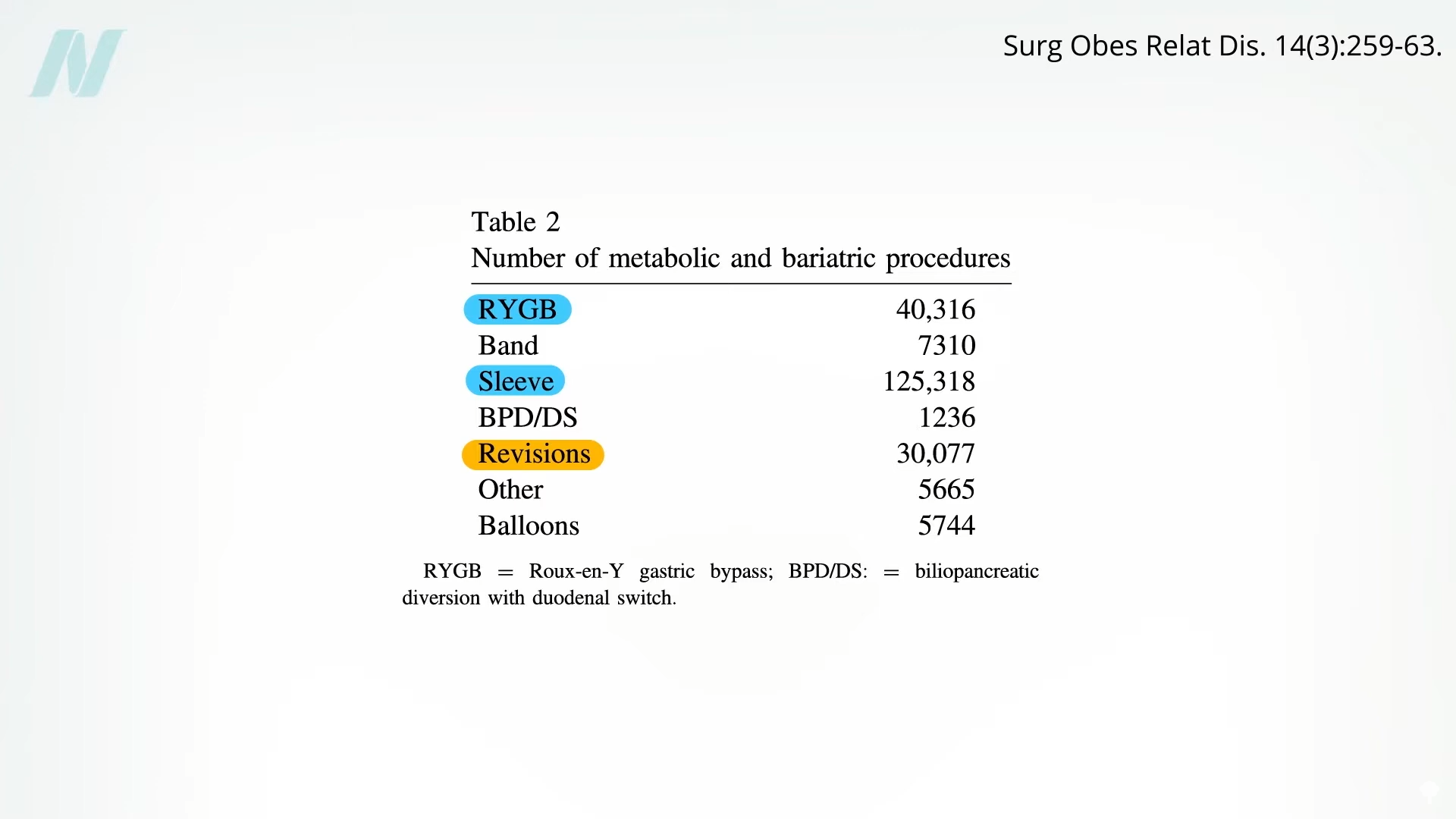
Following the two most common bariatric procedures, sleeve gastrectomy and Roux-en-Y gastric bypass, the third most frequent surgical intervention is a revision to correct issues arising from a prior bariatric operation. This statistic alone highlights the substantial challenge patients face, with an estimated 25% of individuals undergoing bariatric surgery requiring a return to the operating room due to complications from their initial procedure. These subsequent surgeries, or reoperations, carry a significantly elevated risk profile, with mortality rates reported to be up to ten times higher than primary procedures. Furthermore, the success of these revision surgeries is far from guaranteed, leaving patients in a precarious position.
The spectrum of complications following bariatric surgery is broad and can include leaks at the surgical site, the formation of fistulas (abnormal connections between organs), ulcers, strictures (narrowing of passages), erosions, obstructions, and severe acid reflux. While some of these complications can be influenced by patient adherence to post-operative instructions, a substantial body of evidence suggests that surgical expertise plays a pivotal role in their prevention and management.
Surgeon Skill: A Quantifiable Variable in Surgical Outcomes
A landmark study, published in The New England Journal of Medicine, shed crucial light on the impact of surgeon skill. In this innovative research, bariatric surgeons voluntarily submitted video recordings of their surgical procedures to an independent panel of their peers for meticulous evaluation. The findings revealed a wide disparity in technical proficiency among these surgeons. Crucially, this variation in skill was directly correlated with patient outcomes.
The study demonstrated a clear link between surgeon competence and the incidence of adverse events. Patients operated on by surgeons deemed less technically proficient experienced nearly three times the rate of complications and a five-fold increase in their risk of death compared to those treated by their more skilled counterparts. This data suggests that the perceived risks associated with bariatric surgery are not uniform and are significantly influenced by the individual performing the procedure.

The Learning Curve: Mastering Complex Procedures
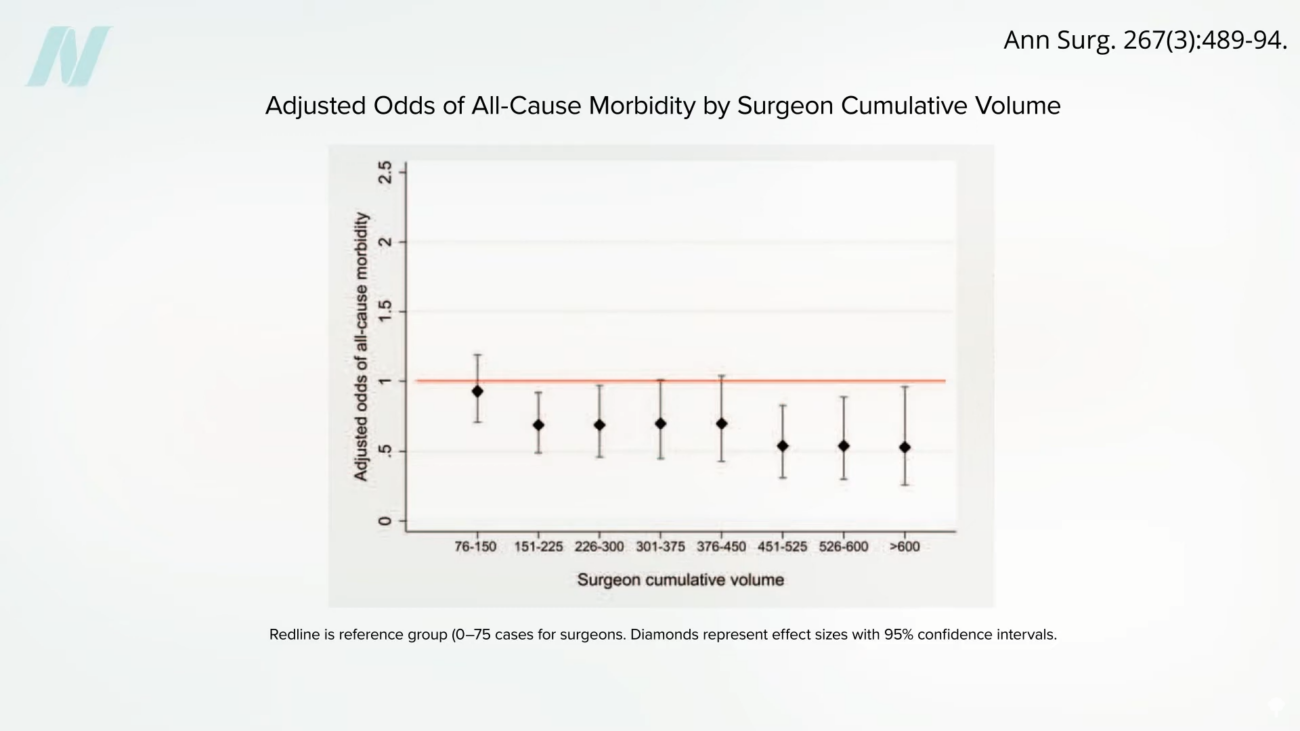
The inherent complexity of bariatric surgeries, particularly procedures like the gastric bypass, necessitates a significant period of learning and skill acquisition for surgeons. Experts suggest that a surgeon may need to perform approximately 500 cases to achieve mastery of the procedure. The data indicates that the risk of complications appears to plateau after a surgeon has completed around 500 procedures. Optimal outcomes, characterized by the lowest rates of complications, are observed among surgeons who have performed more than 600 bypasses.
Analysis of surgical outcomes reveals a stark difference in mortality rates based on surgeon experience. Patients undergoing surgery with surgeons who have performed fewer than 75 procedures face double the risk of mortality compared to those treated by surgeons who have completed more than 450 bypasses. This stark contrast underscores the importance of experience in mitigating the life-threatening risks associated with these complex operations.
Navigating the Choice: Patient Empowerment and Institutional Quality
Given the significant impact of surgeon skill, patients considering bariatric surgery are strongly advised to engage in thorough due diligence. A key recommendation is to inquire directly about the number of bariatric procedures a prospective surgeon has performed. Beyond individual surgeon experience, choosing an accredited bariatric "Center of Excellence" is also a critical step. These accredited institutions have demonstrated adherence to rigorous standards of care and are associated with significantly lower surgical mortality rates – reportedly two to three times lower than non-accredited facilities. This suggests a systemic approach to quality control and patient safety within these specialized centers.
Beyond the Surgeon: Patient Factors and Post-Operative Adherence
While surgeon skill is a paramount factor, it is important to acknowledge that patient behavior and adherence to post-operative protocols also play a significant role in surgical success and complication avoidance. A cautionary tale, albeit an extreme one, highlights this point. In a reported case, a woman three months post-gastric bypass underwent an episode of uncontrolled eating at an all-you-can-eat buffet. Despite selecting healthy foods, she evidently failed to chew them adequately. This led to the rupture of surgical staples and an emergency reoperation. Upon opening her abdomen, surgeons discovered "full chunks of broccoli, whole lima beans, and other green leafy vegetables" within her abdominal cavity. While this serves as an anecdote about the importance of proper chewing, it also indirectly points to the necessity of understanding and adhering to dietary recommendations following surgery. This incident may be interpreted less as a critique of chewing habits and more as a reminder of the profound anatomical and physiological changes that necessitate a complete re-evaluation of eating behaviors.
Lifelong Nutritional Support: An Unavoidable Consequence
Even in cases where the surgical procedure itself is performed without a hitch, bariatric surgery necessitates lifelong nutritional replacement and vigilant monitoring. The procedures, particularly those involving malabsorption, are designed to impair calorie absorption by intentionally bypassing or removing segments of the intestines. This deliberate malabsorption, while contributing to weight loss, simultaneously compromises the absorption of essential vitamins and minerals.
The consequences of these deficits extend far beyond common issues like anemia, osteoporosis, or hair loss. They can manifest as life-threatening deficiencies, including beriberi, pellagra, and kwashiorkor. Furthermore, nerve damage can occur, with vision loss being a potential manifestation of copper deficiency years or even decades after surgery. Tragically, severe deficiencies of B vitamins, such as thiamine, have been reported to result in permanent brain damage in nearly one-third of patients before diagnosis.

Understanding Malabsorptive Mechanisms and Behavioral Modification
The malabsorptive nature of procedures like gastric bypass is a deliberate feature designed to facilitate weight loss. By altering the digestive tract, the body’s ability to absorb calories is significantly reduced. However, this comes at the cost of essential nutrient absorption. Even restrictive procedures, such as stomach stapling, can place patients at risk for life-threatening nutrient deficiencies due to persistent vomiting. Up to 60% of patients report vomiting after bariatric surgery, often attributed to "inappropriate eating behaviors" – essentially, attempting to eat in a manner that is no longer compatible with the altered anatomy. This vomiting, while contributing to weight loss, functions similarly to aversion therapy, where unpleasant physiological responses deter a specific behavior.
"Dumping syndrome" is another mechanism that contributes to behavioral modification post-gastric bypass. A significant proportion of patients experience abdominal pain, diarrhea, nausea, bloating, fatigue, or palpitations after consuming calorie-dense foods. This occurs because these foods bypass the stomach and rapidly enter the intestines. Surgeons often describe dumping syndrome not as a complication, but as an "expected and desired part of the behavior modification caused by gastric bypass surgery," intended to deter patients from consuming energy-dense foods.
Broader Implications for Healthcare and Patient Care
The findings regarding surgeon skill have significant implications for the healthcare system. It highlights the need for robust training programs, continuous professional development, and objective methods for assessing surgical competence. Furthermore, it underscores the importance of patient education and informed consent, ensuring individuals fully understand the risks and the factors that can influence their outcomes.
The long-term management of bariatric surgery patients requires a multidisciplinary approach, involving surgeons, dietitians, endocrinologists, and mental health professionals. This comprehensive care model is essential for addressing the complex nutritional, metabolic, and psychological challenges that can arise following these procedures. As research continues to illuminate the nuances of bariatric surgery, a patient’s ability to make informed decisions, coupled with the expertise of their surgical team, will remain paramount in achieving successful and sustainable health outcomes. The emphasis on surgeon skill serves as a critical reminder that while bariatric surgery can be a life-changing intervention, its success is intricately linked to the precision and experience of the hands that perform it.