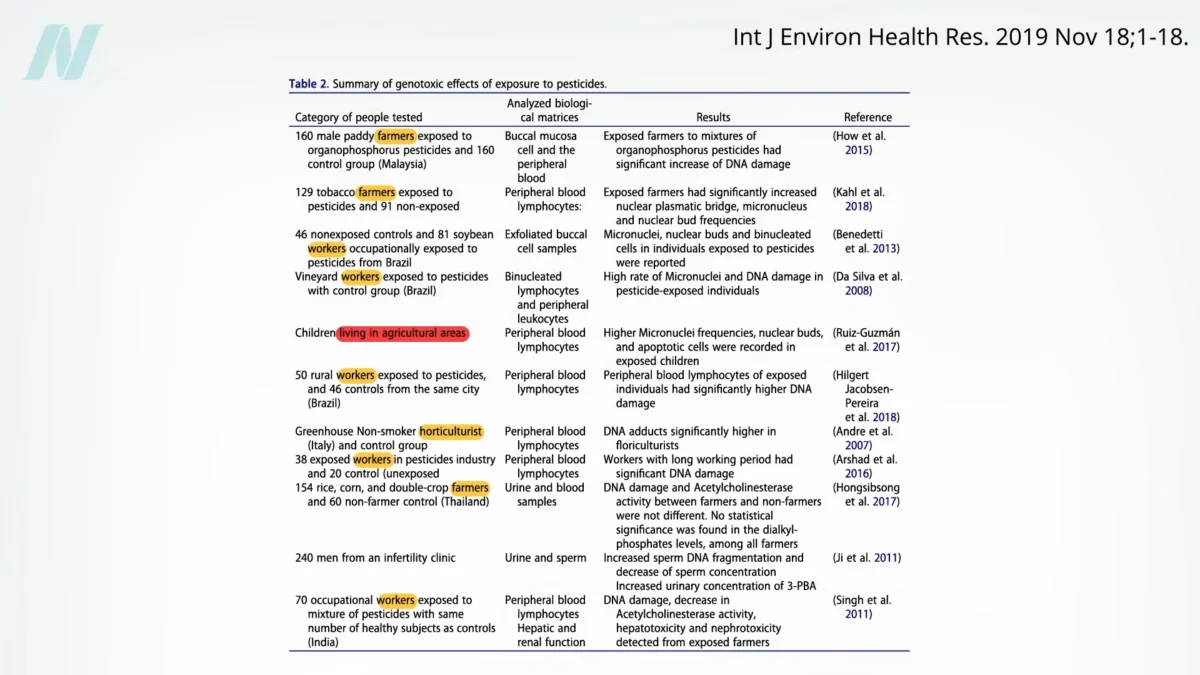
The ongoing debate surrounding the consumption of organic versus conventionally grown foods often centers on the potential health implications, particularly concerning pesticide exposure and its purported link to cancer. A comprehensive review of existing evidence suggests that the connection between pesticide exposure and cancer is substantial, leading some experts to conclude that the role of pesticides in cancer development "cannot be doubted." However, the bulk of research demonstrating DNA damage from pesticides has historically focused on individuals with high occupational exposure, such as farmers and agricultural workers, or those residing in areas with intensive pesticide application.
Understanding Pesticide Exposure and Its Potential Health Impacts
Occupational Exposure: A Well-Documented Concern
Numerous studies have illuminated the risks associated with direct and prolonged exposure to pesticides in agricultural settings. These environments often involve higher concentrations and more frequent contact with a wider range of chemical agents. Research indicates that such occupational exposure can lead to cellular damage, including DNA fragmentation, which is a recognized precursor to various health issues, including cancer. For instance, a review updating evidence on human exposure and toxicity of pesticides underscored the overwhelming body of evidence linking such exposure to an increased cancer risk. This evidence is so robust that it has led to a strong consensus within certain scientific communities regarding the detrimental effects of these chemicals.
Beyond the Fields: Non-Occupational Exposure Pathways
While occupational exposure remains a primary focus, concerns are growing regarding the potential health consequences of lower-level, non-occupational exposure, particularly through dietary intake. Evidence has emerged linking even non-occupational pesticide exposure to DNA damage. A study conducted in China, where average pesticide concentrations are significantly higher than in many other regions, found single- and double-stranded DNA fragmentation in the sperm of men with elevated levels of pesticides in their bodies. This finding, while originating from a region with exceptionally high exposure rates, raises questions about the cumulative effects of chronic, lower-level exposure experienced by the general population through their diet.
Mechanism of Harm: Impairing the Body’s Natural Defenses
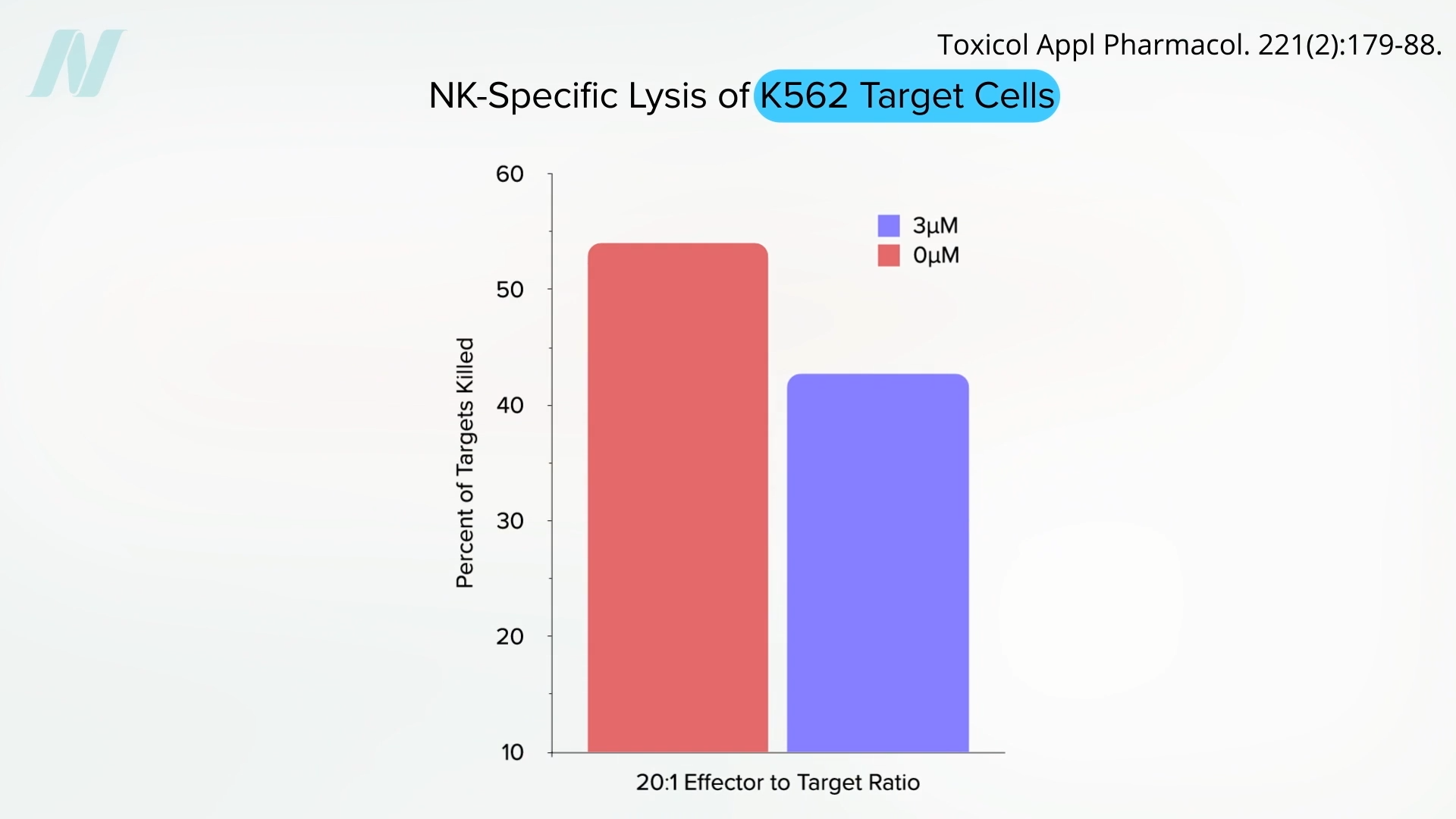
Pesticides may not only directly damage DNA but also potentially compromise the body’s natural defense mechanisms against cancer. Research suggests that these chemicals can adversely affect the function of Natural Killer (NK) cells, a crucial component of the immune system’s first line of defense against cancer and virus-infected cells. Studies have demonstrated that pesticides can impair the ability of NK cells to identify and eliminate cancerous cells. In laboratory settings, NK cells have shown a remarkable capacity to clear a significant portion of leukemia cells. However, when exposed to even small amounts of certain pesticides, their efficacy is dramatically reduced, allowing cancer cells to proliferate. This suggests that chronic exposure to pesticides, even at seemingly low levels, could potentially weaken the body’s ability to combat the development and spread of cancer.

The Dietary Dilemma: Conventional vs. Organic Produce
Given the potential risks associated with pesticide exposure, a natural question arises: does choosing organic foods offer a tangible protective benefit against cancer? The answer, according to current scientific understanding, is complex and evolving.
Residual Pesticides on Conventional Produce
While the studies highlighting severe DNA damage often involve high-level exposure, researchers have also investigated the impact of residual pesticides found on conventionally grown produce. The question of whether the investment in organic food is warranted for cancer prevention hinges on understanding the actual levels of these residues and their cumulative health effects.
Ubiquitous Presence of Pesticides
It is widely acknowledged that pesticide residues are detectable in the blood and urine of a vast majority of the U.S. population, irrespective of their occupation or geographical location. This widespread presence strongly suggests that dietary intake, particularly from conventionally grown foods, is a significant contributing factor. Crossover trials, where participants switch between consuming conventionally grown and organic foods, have provided compelling evidence for this. These studies have shown that urinary concentrations of pesticide metabolites can be turned on and off like a switch, directly correlating with dietary choices. However, the mere presence of these metabolites does not automatically equate to harmful health consequences.
The Unknown Health Consequences of Dietary Residues
The long-term health consequences of ingesting the low levels of pesticide residues commonly found on conventionally grown foods remain a subject of ongoing investigation. While direct causal links are difficult to establish definitively for the general population due to the multifactorial nature of cancer development, emerging research is beginning to shed light on potential associations.
Recent Findings on Organic Food Consumption and Cancer Risk

A significant recent study has provided some of the most compelling evidence to date regarding the association between organic food consumption and reduced cancer risk. This study, the first of its kind to systematically evaluate the link while controlling for a wide array of confounding factors, found that individuals who reported the highest frequency of organic food consumption had approximately a 25% lower risk of developing cancer.
Controlling for Confounding Factors: A Rigorous Approach
The researchers behind this groundbreaking study took meticulous steps to isolate the effect of organic food consumption. They controlled for numerous variables that could potentially influence cancer risk, including age, socioeconomic status, educational attainment, body mass index (BMI), physical activity levels, meat consumption, and smoking habits. Even after accounting for these factors, the association between higher organic food consumption and a reduced cancer risk remained statistically significant.
The study’s authors rigorously addressed potential biases. For instance, they acknowledged that consumers of organic foods might be younger, more health-conscious, or have different lifestyle habits. However, their statistical models accounted for these differences, and the reduced cancer risk persisted. Similarly, factors such as affluence, higher education, lower BMI, increased exercise, reduced meat intake, and less smoking were all factored in, yet the protective association of organic food consumption remained. Even when considering broader dietary patterns, such as higher overall fruit and vegetable intake or lower consumption of processed foods, the observed reduction in cancer risk was still evident. The study’s conclusion was unequivocal: "Our results indicate that higher organic food consumption is associated with a reduction in the risk of overall cancer."
Earlier Research: Mixed Results and Specific Cancer Types
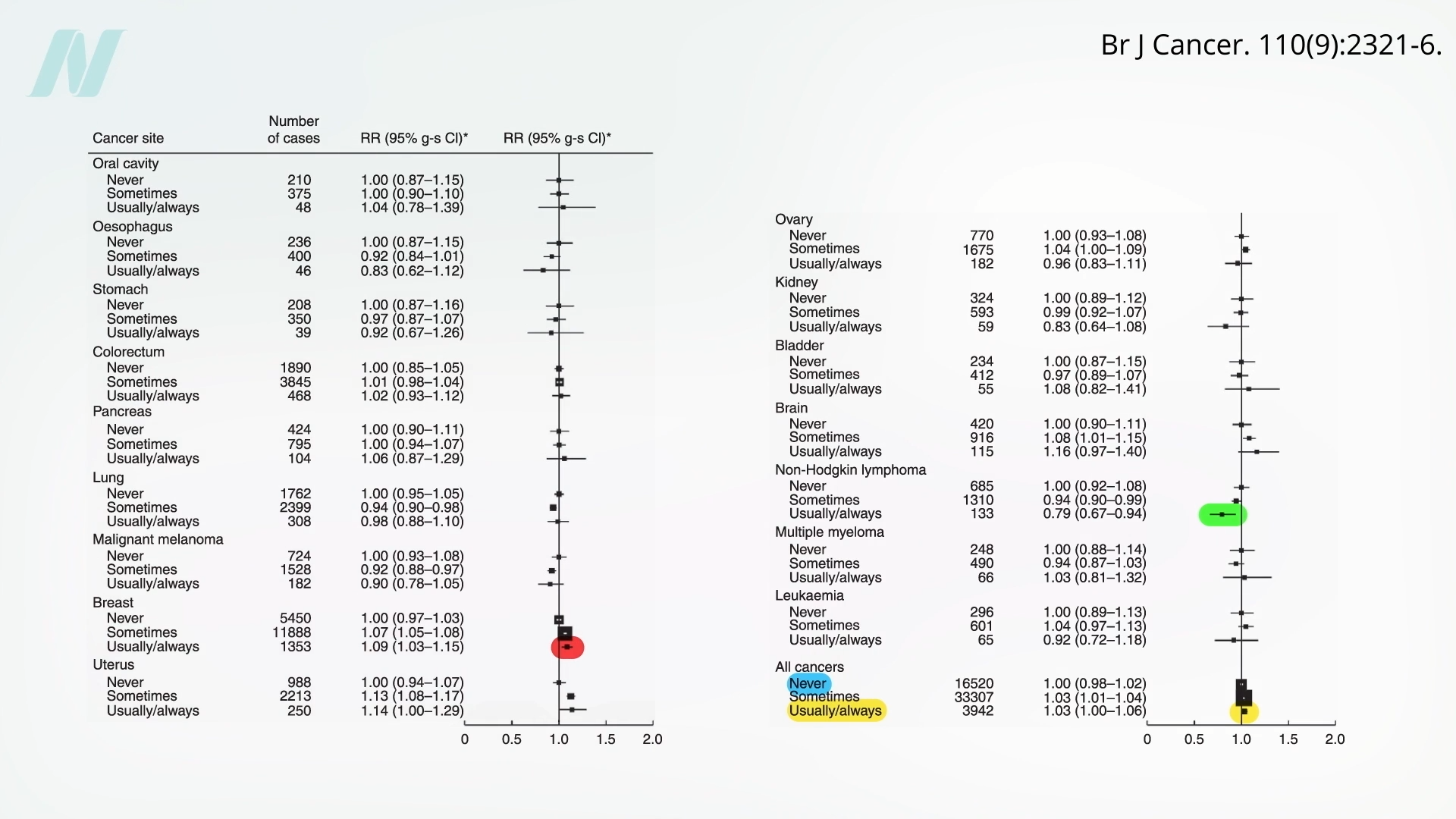
Prior to this comprehensive study, earlier research efforts had yielded more mixed results. One large-scale study, while not finding a significant decrease in the incidence of all cancers, did identify a potential reduction in the risk of a specific type of blood cancer: non-Hodgkin lymphoma. This earlier investigation, however, did not observe an overall reduction in cancer rates among individuals who consistently chose organic foods compared to those who rarely or never did. Interestingly, this study did report a slightly increased risk of breast cancer among organic consumers, a finding for which the researchers could not provide a definitive explanation. They speculated whether increased awareness and adherence to breast cancer screening protocols among organic consumers might contribute to higher diagnosis rates, though this remains a hypothesis.
Beyond Cancer: Pesticides and All-Cause Mortality
The implications of pesticide exposure extend beyond cancer risk to encompass overall mortality. Research has indicated a significant association between elevated blood levels of certain pesticides and a shortened lifespan.
Beta-Hexachlorocyclohexane and Lifespan Reduction
One such pesticide, beta-hexachlorocyclohexane (beta-HCH), has been identified as a potential contributor to reduced longevity. Higher concentrations of this pesticide in the blood have been linked to a significantly shorter life expectancy.
Dietary Patterns and Pesticide Load
Understanding how dietary choices influence the body’s pesticide load is crucial. Decades ago, a study comparing a vegetarian mother with her non-vegetarian sister revealed a notable difference in pesticide levels. The vegetarian sister’s breast milk exhibited approximately one-third lower levels of beta-HCH compared to her omnivorous sibling. This finding is consistent with the understanding that certain classes of chlorinated pesticides, like beta-HCH, are fat-soluble and tend to accumulate in animal products.
Polychlorinated Biphenyls (PCBs) and Mortality Risk
More recent studies have investigated other persistent organic pollutants, such as polychlorinated biphenyls (PCBs), which are structurally similar to some pesticides and are also fat-soluble. Research has found that exposure to PCBs is linked to an increased risk of mortality. These toxins are commonly found in foods of animal origin, including eggs, dairy products, and animal fats.
A study examining PCBs found that individuals following a vegan diet had significantly lower levels of a range of PCBs compared to omnivores. This suggests that reducing or eliminating animal product consumption could lead to a lower overall body burden of these harmful compounds. However, it is important to note that the vegan group in this particular study did not show lower levels of beta-HCH, indicating that dietary strategies for reducing different types of pesticide-related compounds may vary.
Implications for Dietary Choices and Public Health
The cumulative body of evidence suggests that while concerns about pesticide exposure are valid, the practical implications for dietary choices, particularly concerning fruits and vegetables, warrant careful consideration.
The Benefit of Fruits and Vegetables Outweighs Pesticide Risk

For fruits and vegetables, the nutritional benefits of consumption appear to significantly outweigh the potential risks associated with pesticide residues. Even if pesticide exposure from conventionally grown produce were to have a cumulative negative impact over a lifetime, estimates suggest that this impact might reduce lifespan by only a few minutes on average. This is a negligible amount when compared to the substantial health advantages conferred by a diet rich in fruits and vegetables, which are vital for preventing a myriad of chronic diseases. Therefore, public health recommendations should continue to encourage the consumption of these essential food groups, regardless of whether they are organic or conventionally grown.
Reducing Animal Product Intake: A Potential Strategy
For individuals concerned about the adverse health effects of pesticides and related chemical compounds, reducing their intake of animal products may be a prudent strategy. The accumulation of fat-soluble pesticides and pollutants in animal-derived foods suggests that dietary shifts away from these items could lead to lower body burdens of these toxins.
Navigating the Organic Landscape: A Personal Choice
The decision to purchase organic foods is ultimately a personal one, influenced by individual priorities, budget, and risk assessment. While the scientific evidence regarding the direct link between low-level pesticide exposure from conventional produce and cancer is still developing, the findings on occupational exposure and the potential impact of pesticides on immune function underscore the importance of minimizing exposure where possible. The robust findings from recent studies linking higher organic food consumption to a reduced overall cancer risk provide a compelling data point for those seeking to proactively manage their health.
The ongoing research in this field is crucial for informing public health policies and individual dietary choices. As our understanding of the complex interplay between environmental exposures, dietary patterns, and human health continues to evolve, consumers will be better equipped to make informed decisions that promote long-term well-being. The pursuit of a diet that is both nutritious and minimizes exposure to harmful chemicals remains a central tenet of modern health advocacy.


