Parkinson’s disease, a debilitating neurodegenerative disorder affecting millions worldwide, has long been a subject of intense scientific scrutiny. While the precise cascade of events leading to its onset remains complex, emerging research has consistently pointed towards a significant dietary link: milk consumption. This association, robustly supported by multiple large-scale prospective studies, has prompted a deeper investigation into the potential culprits within dairy products that might contribute to the increased risk of developing this progressive brain disorder. Two primary hypotheses have gained traction: the presence of the banned pesticide heptachlor and its epoxide metabolite, and the metabolic breakdown product of milk sugar, galactose. Understanding these potential mechanisms is crucial for public health advisories and individual dietary choices.
The Persistent Association Between Dairy and Parkinson’s Disease
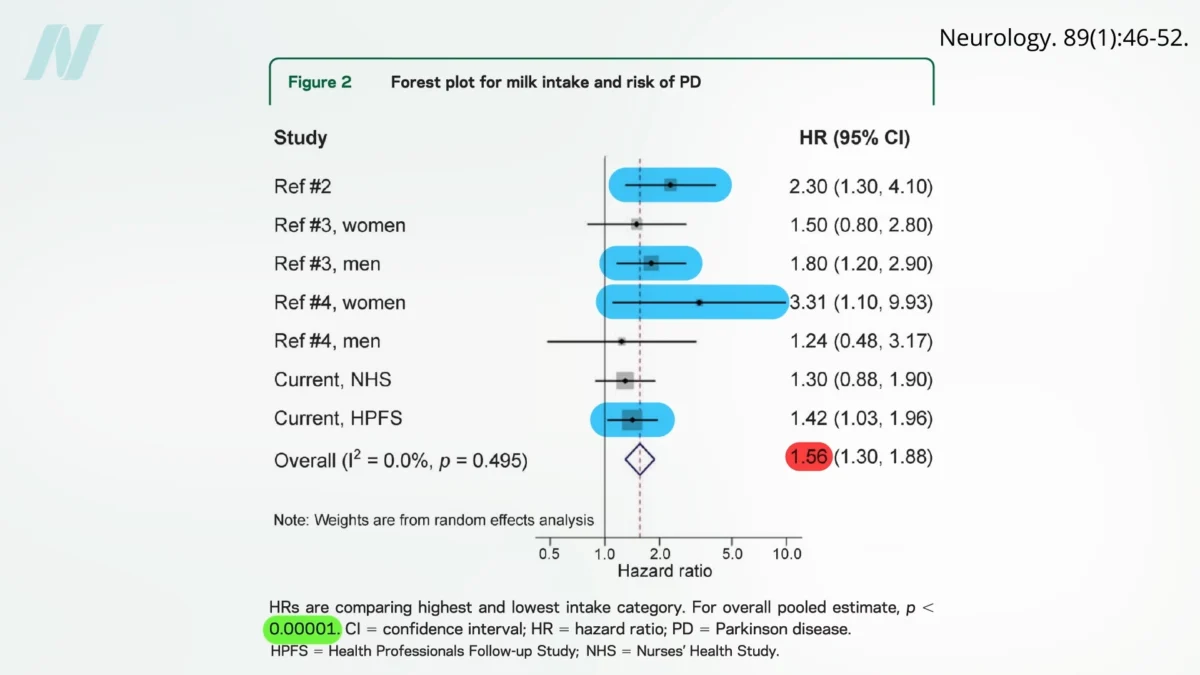
The connection between dairy intake and an elevated risk of Parkinson’s disease is not a new observation, but its significance has been solidified by a growing body of evidence. Five major prospective studies have consistently demonstrated this link, including foundational research from the Harvard cohorts: the Nurses’ Health Study and the Health Professionals Follow-up Study. These extensive investigations, collectively following over 100,000 participants for decades, represent one of the most comprehensive analyses to date of dairy consumption and Parkinson’s disease incidence.
These landmark studies revealed a striking correlation: individuals who consumed the most milk exhibited approximately a 50% increase in their risk of developing Parkinson’s disease compared to those who consumed the least. The statistical significance of this finding is exceptionally high, with a p-value below 0.00001, indicating an extremely low probability of such a result occurring by random chance. This statistical power underscores the robustness of the observed association, suggesting a genuine underlying biological relationship rather than a mere coincidence.
Investigating the Potential Mechanisms: Heptachlor Epoxide
One of the earliest and most compelling hypotheses to explain this association centers on the potential presence of pesticide residues in milk. For years, concerns have been raised about environmental contaminants that can accumulate in the food chain and potentially impact human health. Among these, the organochlorine pesticide heptachlor and its primary breakdown product, heptachlor epoxide, have been identified as potential neurotoxic agents.
A pivotal study, published a year after a review concluded there was "no rational explanation" for the milk-Parkinson’s link, provided a significant clue. This research examined the brains of individuals at autopsy, correlating their reported midlife milk consumption with the density of specific neurons in the substantia nigra, a critical brain region severely affected in Parkinson’s disease. The findings were stark: neuron density was consistently lower in those who consumed the most milk. Even in individuals without a Parkinson’s diagnosis, those drinking as little as two cups of milk daily showed up to a 40% reduction in these vital nerve cells.
Crucially, this study also found a significant correlation between high milk consumption and the presence of heptachlor epoxide residues in the brain. In individuals who were the heaviest milk drinkers, heptachlor epoxide was detected in an astonishing 9 out of 10 brains examined. This high prevalence suggests that milk could act as a significant vector for exposure to this banned pesticide, which has been linked to neurological damage in other contexts. The implication is that chronic exposure to heptachlor epoxide, potentially mediated by milk consumption, could be a direct cause-and-effect contributor to the neurodegenerative processes underlying Parkinson’s disease.
The historical context of heptachlor’s use is important here. Banned in many countries due to its persistence in the environment and potential health risks, residues can still be found in older products or through cross-contamination. Dairy cows, grazing on land where heptachlor may have been applied historically, can absorb these chemicals, which are then secreted into their milk. This pathway highlights the challenges in eradicating environmental contaminants from the food supply.
Exploring the Role of Galactose: A Sweet Neurotoxic Link?
While the pesticide hypothesis offers a plausible explanation, scientific inquiry has also delved into the intrinsic components of milk. Lactose, the primary sugar in milk, breaks down in the body into glucose and galactose. Recent research suggests that galactose itself might play a significant role in neuronal damage and the aging process of the brain, potentially linking it to Parkinson’s disease.

Galactose is known to be rapidly absorbed by the brain shortly after ingestion. Studies indicate that doses exceeding 100 mg/kg of body weight can induce pathological alterations in brain cells, mirroring changes observed in Parkinson’s disease. Alarmingly, consuming just two glasses (approximately 473 mL) of milk daily can easily reach or surpass this threshold, as milk is a primary dietary source of galactose.
What makes galactose particularly concerning for Parkinson’s is its potential to induce oxidative stress. Dopaminergic neurons, the specific type of nerve cells lost in Parkinson’s disease, appear to be especially vulnerable to this oxidative damage. This vulnerability could explain why these particular neurons are disproportionately affected by galactose exposure. The process of experimentally inducing brain aging in laboratory animals often involves the administration of galactose, further underscoring its role in accelerated neuronal decline.
Galactose and Mortality Rates: A Broader Health Impact
The potential neurotoxic effects of galactose may extend beyond Parkinson’s disease, offering an explanation for observations linking high milk consumption to increased mortality rates. While saturated fat content in milk has often been cited as a contributor to cardiovascular issues and reduced lifespan, studies have shown elevated mortality risks associated with milk consumption regardless of fat content. This suggests that factors beyond fat may be at play.
The fact that even skim milk, which is virtually fat-free, still contains lactose and consequently galactose, supports the hypothesis that galactose could be a contributing factor to these broader health concerns. The breakdown of lactose into galactose within the digestive system means that the galactose load remains significant even in reduced-fat dairy products.
Lactose-Free Milk: Not a Guaranteed Solution
The emergence of lactose-free milk products, such as Lactaid, has provided an option for individuals with lactose intolerance. These products are manufactured by adding the lactase enzyme, which breaks down lactose into glucose and galactose. However, from a galactose-exposure perspective, these alternatives may not offer a significant advantage. The enzymatic breakdown occurs in the carton before consumption, meaning that individuals are still ingesting essentially the same amount of galactose as they would from regular milk.
This insight has implications for cognitive health as well. Research indicates that increased milk intake in midlife may be associated with a faster rate of cognitive decline. This correlation is consistent with the established use of D-galactose in animal models to mimic cognitive aging through oxidative stress. Individuals who report drinking more than one glass of milk daily appear to have a higher likelihood of experiencing a decline in global cognitive function compared to those who consume milk infrequently.
Broader Implications and Future Research Directions
The convergence of evidence pointing towards both pesticide residues and galactose as potential contributors to milk-related neurodegeneration presents a complex public health challenge. The robust statistical association between dairy consumption and Parkinson’s disease, coupled with the plausible biological mechanisms, necessitates careful consideration of dietary guidelines and public awareness campaigns.
Further research is imperative to definitively disentangle the relative contributions of heptachlor epoxide and galactose. Studies involving direct measurement of exposure biomarkers and detailed longitudinal tracking of individuals with varying dairy intake and environmental exposures could provide clearer answers. Investigating the synergistic effects of these compounds, or their interactions with other dietary and lifestyle factors, is also crucial for a comprehensive understanding.
Moreover, the implications extend beyond Parkinson’s disease. The potential link between galactose and accelerated brain aging, cognitive decline, and even increased mortality rates underscores the importance of understanding the long-term health consequences of widespread dairy consumption. As scientific understanding evolves, so too must public discourse and dietary recommendations to promote optimal neurological health and longevity. The ongoing investigation into the intricate relationship between milk, its components, and neurodegenerative diseases is a critical step towards mitigating the impact of these conditions on global health.