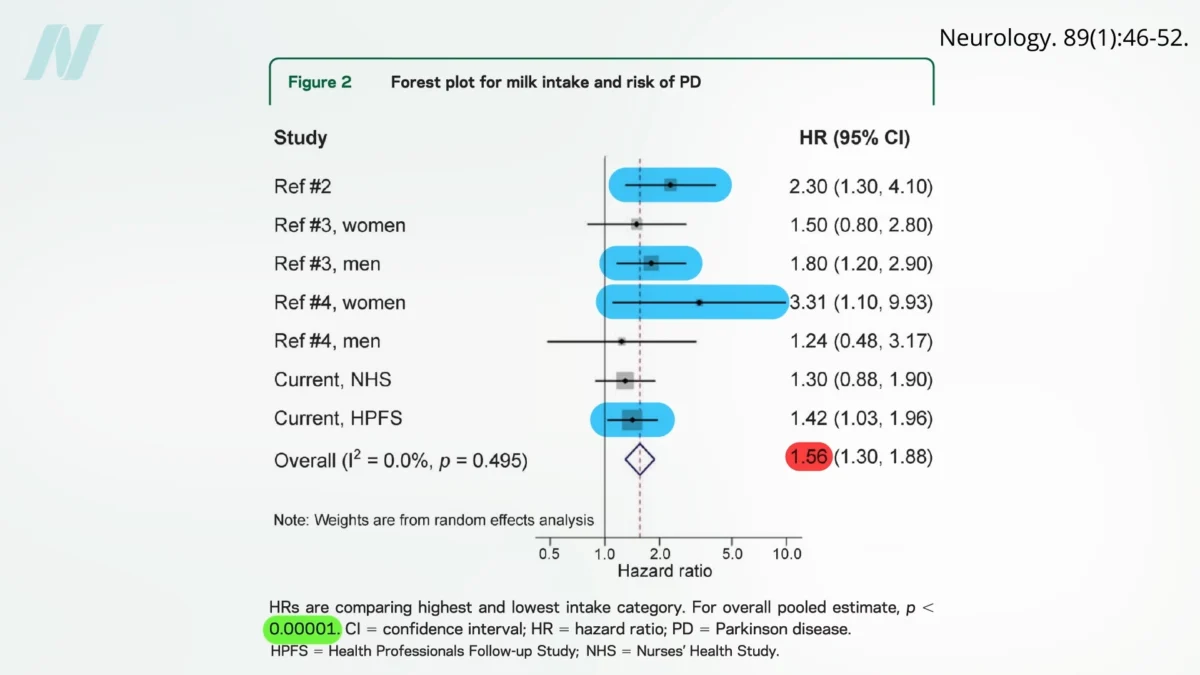
Parkinson’s disease, a relentless neurodegenerative disorder affecting millions globally, has long been a subject of intense scientific scrutiny. While its exact origins remain elusive, a growing body of research points towards lifestyle factors, with dairy consumption emerging as a particularly potent dietary association with an elevated risk of developing this debilitating condition. The strength of this link is underscored by its consistent presence across multiple large-scale prospective studies, including the seminal Harvard cohorts – the Nurses’ Health Study and the Health Professionals Follow-up Study. These landmark investigations, collectively tracking over 100,000 individuals for decades, represent the most comprehensive analyses of dairy intake and Parkinson’s disease to date. Their findings, which examined over 1,000 newly diagnosed Parkinson’s cases, consistently demonstrated an association between dairy consumption and an increased risk. The data revealed a striking pattern: individuals consuming the highest quantities of milk exhibited approximately a 50% higher risk of developing Parkinson’s compared to those who abstained, a finding statistically significant with a p-value below 0.00001, indicating an exceptionally low probability of such an outcome occurring by chance.
The Unanswered Question: What in Milk Triggers the Risk?
Despite these robust epidemiological associations, the precise biological mechanisms underlying the connection between milk and Parkinson’s disease have remained a subject of considerable debate and investigation. For years, a prevailing sentiment among some researchers was a lack of a "rational explanation" for the observed link, as noted in a 2015 review. However, subsequent research has begun to illuminate potential culprits, shifting the focus towards specific components within milk that could be detrimental to neural health.
A pivotal study published in 2016 offered a significant clue by examining the relationship between midlife milk consumption and the density of substantia nigra neurons – the very brain cells critically affected in Parkinson’s disease – at the time of autopsy. Parkinson’s is primarily characterized by the progressive loss of these dopaminergic neurons in a specific region of the brain, with symptoms manifesting only after a substantial portion of these neurons has degenerated. This research meticulously analyzed the milk intake of participants in their 40s, 50s, and 60s and subsequently assessed their brains post-mortem. The findings were stark: neuron density in the substantia nigra was consistently highest in individuals who consumed no milk and lowest in those who were the most avid milk drinkers. Remarkably, even when individuals diagnosed with Parkinson’s were excluded from the analysis, those who consumed approximately two cups (473 mL) of milk daily exhibited up to a 40% reduction in the number of these vital nerve cells in key areas of the brain.
The Pesticide Hypothesis: Heptachlor Epoxide’s Shadow
One compelling theory proposed to explain this neuronal loss centers on the presence of pesticide residues in dairy products. Among the participants who reported the highest milk consumption, residues of heptachlor epoxide, a breakdown product of the banned pesticide heptachlor, were detected in a staggering 9 out of 10 brains examined. This finding suggests a potential causal pathway where the accumulation of this neurotoxic pesticide, ingested through milk, could contribute to the damage and death of dopaminergic neurons, thereby increasing the risk of Parkinson’s disease.
The history of heptachlor in the agricultural landscape is relevant here. Banned in the United States in the late 1970s due to its persistence in the environment and potential health risks, heptachlor was used as an insecticide on a variety of crops, including fruits, vegetables, and grains. However, residues could persist in soil and enter the food chain, particularly through animal products like dairy. Cows consuming contaminated feed could accumulate heptachlor epoxide in their fatty tissues, subsequently transferring it to their milk. The presence of these residues in such a high proportion of brains from heavy milk drinkers provides a tangible link between dairy consumption and a potential neurotoxic insult. The implication is that even though heptachlor itself is banned, historical or ongoing environmental contamination could still be contributing to the problem through the food supply.
The Galactose Factor: A Sugar with a Sinister Role
Beyond the pesticide hypothesis, another significant area of investigation focuses on galactose, a simple sugar derived from the breakdown of lactose, the primary sugar found in milk. Once lactose is consumed, it is broken down into glucose and galactose in the digestive system. Research has indicated that galactose plays a critical role in experimental models of brain aging. When ingested, galactose is readily absorbed by the brain. Studies suggest that for doses exceeding 100 mg/kg of body weight, galactose can induce pathological changes in brain cells that closely mirror those observed in Parkinson’s disease. This threshold can be met or surpassed by consuming just two glasses (approximately 473 mL) of milk daily, positioning milk as a significant dietary source of this potentially neurotoxic sugar.

Crucially, dopaminergic neurons, the specific type of brain cells affected in Parkinson’s, appear to be particularly vulnerable to galactose-induced damage. This heightened susceptibility is attributed to their increased vulnerability to oxidative stress. Oxidative stress, an imbalance between free radicals and antioxidants in the body, is a known contributor to neurodegeneration. Galactose’s ability to exacerbate this stress in these specific neurons makes it a prime suspect in the milk-Parkinson’s link.
Galactose and Mortality: A Wider Impact?
The potential detrimental effects of galactose extend beyond neurodegeneration, offering an explanation for observed links between high milk consumption and increased mortality rates. While saturated fat in dairy has often been cited as a cause for concern regarding cardiovascular health and longevity, studies have revealed elevated mortality risks associated with high milk intake irrespective of the milk’s fat content. This suggests that the impact is not solely due to fat. Even fat-free or skim milk, while lacking saturated fat, still contains lactose, which is broken down into galactose. This implies that the sugar component, galactose, may be a significant contributor to the observed increased mortality, potentially through mechanisms that induce cellular damage and aging.
The Misconception of Lactose-Free Milk
The advent of lactose-free milk, such as Lactaid, has offered a perceived solution for individuals seeking to reduce their lactose intake. However, this innovation does not circumvent the potential problem posed by galactose. In lactose-free milk, the lactase enzyme is added to break down lactose into glucose and galactose while the milk is still in the carton. Consequently, consumers are still ingesting the same quantity of galactose as they would from regular milk. This fact may contribute to the observed correlation between increased milk intake in midlife and a more rapid rate of cognitive decline.
Galactose and Cognitive Decline: A Laboratory Parallel
The role of galactose in accelerating brain aging is well-established in laboratory research. D-galactose, the specific form of galactose found in milk, has been extensively used in animal models to induce cognitive aging. Through mechanisms involving oxidative stress, researchers have successfully mimicked age-related cognitive impairments in these models by administering galactose. Human studies have also shown a correlation: individuals who consume more than one glass (approximately 237 mL) of milk per day appear to be at a higher risk of experiencing a decline in global cognitive function compared to those who rarely drink milk. This reinforces the notion that galactose’s impact on brain health is not confined to Parkinson’s disease but may have broader implications for cognitive function and aging.
Broader Implications and Future Directions
The consistent epidemiological data linking dairy consumption to Parkinson’s disease, coupled with emerging scientific evidence pointing towards both pesticide residues and galactose as potential culprits, necessitates a re-evaluation of dairy’s place in a neuroprotective diet. While dairy products are often promoted for their calcium and vitamin D content, the potential risks associated with their consumption, particularly regarding neurodegenerative diseases and cognitive decline, cannot be ignored.
Further research is warranted to definitively disentangle the relative contributions of heptachlor epoxide and galactose to the observed increased risk of Parkinson’s disease. Understanding the precise dose-response relationships and the long-term effects of chronic exposure to these substances through dairy is crucial. Public health messaging and dietary guidelines may need to evolve to incorporate these findings, offering individuals more nuanced information to make informed choices about their dietary habits. The implications extend beyond individual health, potentially influencing agricultural practices, food processing standards, and regulatory policies concerning pesticide use and dairy production. As science continues to illuminate the intricate connections between our diet and brain health, the case against high milk consumption as a risk factor for Parkinson’s disease appears increasingly compelling, urging a closer examination of the silent threats lurking within seemingly benign dietary staples.