The age-old adage, "All disease begins in the gut," attributed to Hippocrates nearly 2,500 years ago, is gaining increasing scientific validation. Emerging research is shedding light on the profound influence of the gut microbiome – the complex community of microorganisms residing in our digestive tract – on overall health and disease. A key area of focus is trimethylamine N-oxide (TMAO), a compound linked to a growing list of serious health conditions. While plant-based diets appear to offer a protective shield against TMAO’s detrimental effects, a recent investigation into fecal microbiota transplantation (FMT) from vegan donors aimed to explore whether directly altering the gut flora could achieve similar benefits, yielding complex and nuanced results.
Understanding TMAO and its Health Implications
TMAO is produced in the gut when certain bacteria metabolize dietary precursors, primarily choline and L-carnitine, which are abundant in animal products such as red meat, eggs, and dairy. While the body can excrete some TMAO, elevated levels have been increasingly associated with a range of health problems.
Historically, TMAO was primarily recognized for its contribution to cardiovascular diseases. Studies have consistently demonstrated its role in increasing the risk of heart disease and stroke. This link is attributed to several mechanisms, including promoting atherosclerosis (the hardening and narrowing of arteries), increasing blood pressure, and contributing to the formation of blood clots, particularly in individuals with atrial fibrillation. The consequences can be severe, with individuals exhibiting higher TMAO levels often experiencing more debilitating strokes and a significantly increased risk of mortality.
However, the spectrum of TMAO’s influence extends far beyond cardiovascular health. Recent research has expanded its association to include other significant health concerns:
- Inflammatory and Autoimmune Conditions: TMAO has been linked to psoriatic arthritis, a chronic inflammatory disease affecting the skin and joints.
- Metabolic Disorders: Its association with polycystic ovary syndrome (PCOS), a common hormonal disorder among women of reproductive age, highlights its impact on metabolic health.
- Cancer: Perhaps most concerningly, TMAO has been linked to an increased risk of various cancers, which are the second leading cause of death in the United States. While the exact mechanisms are still under investigation, potential pathways include promoting chronic inflammation, inducing oxidative stress, causing DNA damage, and disrupting protein folding – all factors implicated in cancer development.
- Respiratory Illnesses: Chronic obstructive pulmonary disease (COPD), the fourth leading killer, also shows a connection to TMAO. While the direct link is still being elucidated, elevated TMAO levels have been associated with premature death in COPD patients, often due to concurrent cardiovascular complications.
- Neurological Disorders: TMAO has demonstrated the capacity to cross the blood-brain barrier and has been detected in human cerebrospinal fluid. Higher TMAO levels have been observed in individuals with mild cognitive impairment and Alzheimer’s disease dementia. In the brain, TMAO has been shown to induce neuronal senescence (age-related deterioration of brain cells), exacerbate oxidative stress, impair mitochondrial function, and inhibit key signaling pathways like mTOR, all of which contribute to cognitive decline and brain aging.
- Diabetes: Individuals with higher TMAO levels are approximately 50% more likely to develop type 2 diabetes, the seventh leading cause of death.
- Kidney Disease: As the ninth leading cause of death, kidney disease shows a strong correlation with TMAO. Elevated TMAO levels are significantly related to impaired kidney function and can predict fatal outcomes in kidney patients. A longitudinal study revealed a stark contrast: over five years, more than half of chronic kidney disease patients with average or higher TMAO levels died, while nearly 90% of those in the lowest third of TMAO levels remained alive.
The Protective Role of Plant-Based Diets
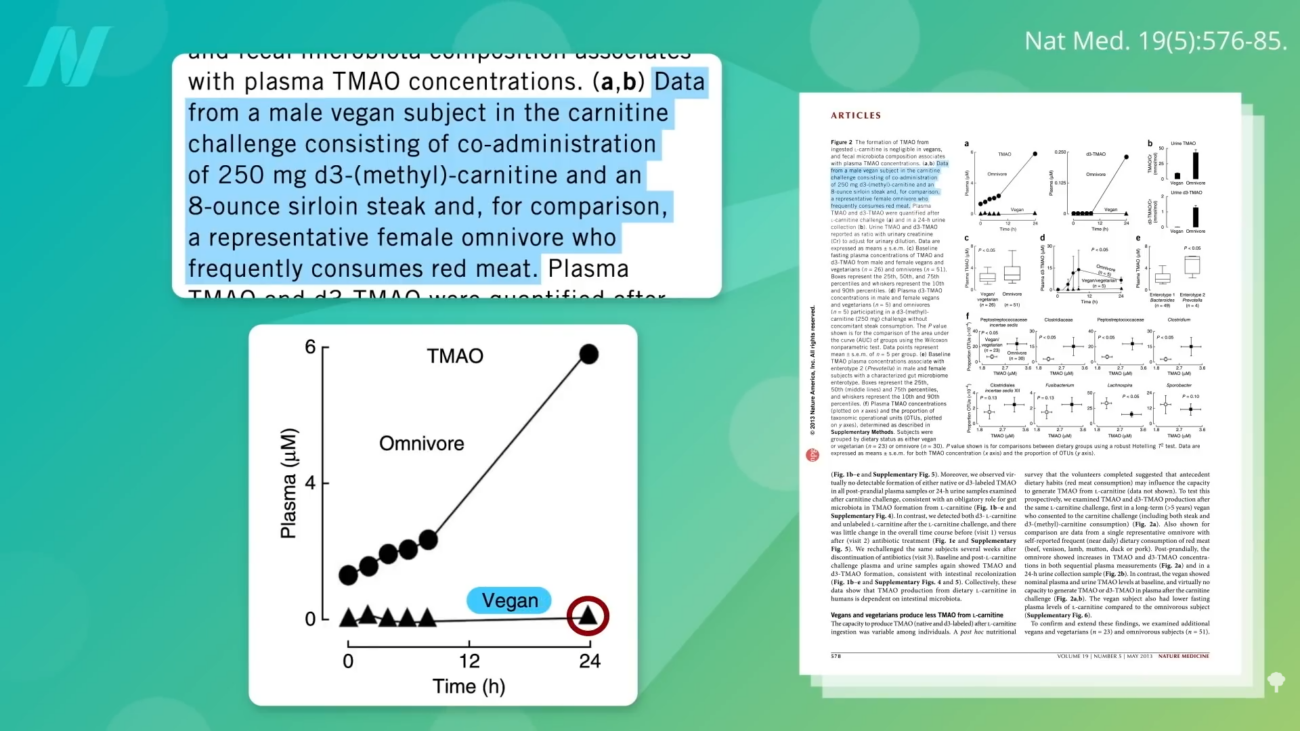
The scientific community has observed a distinct difference in TMAO production between individuals consuming plant-based diets and those with omnivorous diets. Studies suggest that people who adhere to plant-based eating patterns, particularly vegans, produce significantly less TMAO even when consuming foods rich in choline and carnitine, such as steak. This phenomenon is attributed to the differing composition of their gut microbiomes.
Plant-based diets, rich in fiber, cultivate a microbial ecosystem that is less efficient at metabolizing TMAO precursors. Instead, beneficial gut bacteria thrive, producing valuable compounds like butyrate, a short-chain fatty acid that nourishes the gut lining and possesses anti-inflammatory properties. In contrast, diets high in animal products tend to foster a microbiome that readily converts choline and carnitine into trimethylamine (TMA), which is then oxidized in the liver to TMAO.
Exploring Fecal Microbiota Transplantation (FMT) as a Potential Intervention
Given the observed protective effects of a plant-based microbiome, researchers began to explore whether directly transplanting a "healthy" gut flora could offer a therapeutic intervention for individuals with elevated TMAO levels. Fecal microbiota transplantation (FMT), a procedure involving the transfer of fecal matter from a healthy donor to a recipient, has shown promise in treating conditions like recurrent Clostridioides difficile infection. The question arose: could a fecal transplant from a vegan donor, theoretically carrying a microbiome adept at minimizing TMAO production, effectively lower TMAO levels in recipients?
A notable study investigated this very question through a double-blind, randomized, controlled trial. Participants received either fecal matter from vegan donors or their own re-introduced fecal matter via a nasogastric tube. The results, however, were not as straightforward as initially hoped.
Unpacking the Findings of the Vegan FMT Trial
The trial revealed several critical insights that temper immediate enthusiasm for vegan fecal transplants as a universal solution for TMAO reduction.

Discrepancies in Baseline Microbiomes: A key observation was the difference in baseline TMAO production among the vegan donors in this study compared to previous research. In some earlier investigations, vegans were found to produce virtually no TMAO, even when challenged with high-choline meals. This suggested a profound adaptation of their gut flora to a plant-based diet over an extended period. In contrast, the vegan donors in the FMT trial, despite their dietary choices, were still capable of producing TMAO. This suggests that the duration and strictness of adherence to a vegan diet might play a crucial role in shaping a microbiome that is truly resistant to TMAO production. The study did not specify the minimum duration the donors had been vegan, a factor that could be significant.
Limited Impact of the Transplant: Following the vegan fecal transplant, researchers did not observe a significant reduction in TMAO levels in the recipients two weeks after the procedure. This outcome could be attributed to several factors. Firstly, the limited baseline differences in TMAO-producing capacity among the vegan donors meant that the transplanted material may not have introduced a sufficiently distinct microbial profile to overpower the recipient’s existing flora. Secondly, the study’s design, which allowed participants to continue their omnivorous diets post-transplant, likely played a substantial role. The researchers deliberately maintained participants’ usual diets to isolate the effect of the microbiome intervention and avoid confounding variables, acknowledging that diet alone can significantly alter the gut flora.
The Importance of Diet and Microbiome Synergy: The trial’s findings underscore a fundamental principle: the gut microbiome and diet are intrinsically linked. While a fecal transplant can introduce new microbial communities, their long-term colonization and functional impact are heavily influenced by the dietary environment. If recipients continue to consume a diet rich in TMAO precursors, the transplanted microbes may struggle to establish themselves or exert a sustained beneficial effect. The researchers noted that the failure to achieve improvement could be related to the limited baseline microbiome differences and the continuation of an omnivorous diet after the transplant.
The "Vegan Poop" Paradox: The study also highlighted an interesting paradox. The vegan fecal matter used in the transplant appeared to possess some capacity to produce TMAO itself, further complicating the goal of achieving a complete reduction. This suggests that simply identifying as "vegan" may not automatically confer a microbiome that is entirely free of TMAO-producing capabilities. The specific microbial species and their metabolic activities are paramount.
Implications and Future Directions
The results of this vegan fecal transplant study offer a valuable, albeit sobering, perspective. They suggest that there may be no easy shortcuts to mitigating the health risks associated with TMAO. While the concept of a "quick fix" through microbial manipulation is appealing, the findings point towards a more holistic approach.
- Dietary Intervention Remains Paramount: The most consistent and robust evidence for lowering TMAO levels lies in dietary modification. Adopting a whole-foods, plant-based diet appears to be the most effective strategy for cultivating a gut microbiome that naturally minimizes TMAO production and promotes overall health. This aligns with the foundational understanding of gut health, emphasizing that what we feed our gut bacteria directly influences their output.
- The Role of Long-Term Dietary Adherence: The study’s observations suggest that the beneficial effects of a plant-based microbiome on TMAO levels are likely a result of long-term dietary adherence, allowing for significant and stable shifts in microbial composition.
- Personalized Approaches May Be Necessary: Future research might explore more personalized approaches to FMT, potentially involving donor screening for specific microbial profiles known for their TMAO-reducing capabilities and combining FMT with structured dietary interventions.
- Understanding Microbial Adaptation: Further investigation into the complex interactions between diet, genetics, and the gut microbiome is crucial to understanding why some individuals on plant-based diets still produce TMAO and how to best promote a truly protective gut environment.
In conclusion, while the prospect of a "vegan fecal transplant" offered an intriguing avenue for TMAO reduction, the scientific evidence thus far suggests that the most direct and reliable path to a healthier gut microbiome and lower TMAO levels remains through sustained adoption of a whole-foods, plant-based diet. The intricate relationship between our food, our gut microbes, and our health continues to be a vital area of scientific exploration, reinforcing the timeless wisdom that our dietary choices are foundational to our well-being.
Doctor’s Note:
For individuals interested in exploring the possibility of becoming a fecal transplant donor, resources are available to guide you through the process. Information on how to become a fecal transplant super donor can be found through relevant health organizations.
For a deeper understanding of TMAO and its multifaceted health implications, a wealth of related research and articles are accessible through reputable health and nutrition platforms.
To further explore the fascinating world of the microbiome and its impact on human health, consult dedicated topic pages and scientific literature that delve into this rapidly evolving field.