The landscape of health and wellness is increasingly dominated by the concept of personalized nutrition, a field promising tailored dietary advice based on individual characteristics. While the appeal of a one-size-fits-all approach is understandable, particularly in an era that celebrates individuality, a closer examination reveals that a fundamental shift towards personal responsibility for one’s health might be a more impactful, albeit less glamorous, pursuit. The marketing of personalized nutrition often taps into our innate desire to feel special, a psychological driver that fuels its popularity and has spurred innovation in customized food products, with technologies like 3D food printing emerging as promising avenues for individual food customization.
The Nuances of Individuality: When Personalization Matters
Undeniably, there are instances where personalized dietary approaches are not just beneficial but medically imperative. Severe allergies, such as a peanut allergy, can trigger life-threatening anaphylactic reactions, necessitating strict avoidance. Similarly, individuals with celiac disease must meticulously eliminate gluten from their diet to prevent autoimmune damage to the small intestine. Genetic predispositions also play a significant role; for example, lactose intolerance, a common condition, particularly in populations of Asian descent, is due to a genetic mutation affecting lactase enzyme production.
Beyond these well-established conditions, emerging research highlights the impact of genetic variations on how our bodies process nutrients and other compounds. A notable example is the enzyme mutation prevalent in some Asian populations that alters alcohol metabolism. Individuals with this variant metabolize alcohol less efficiently, leading to a buildup of toxic byproducts and a reduced tolerance.
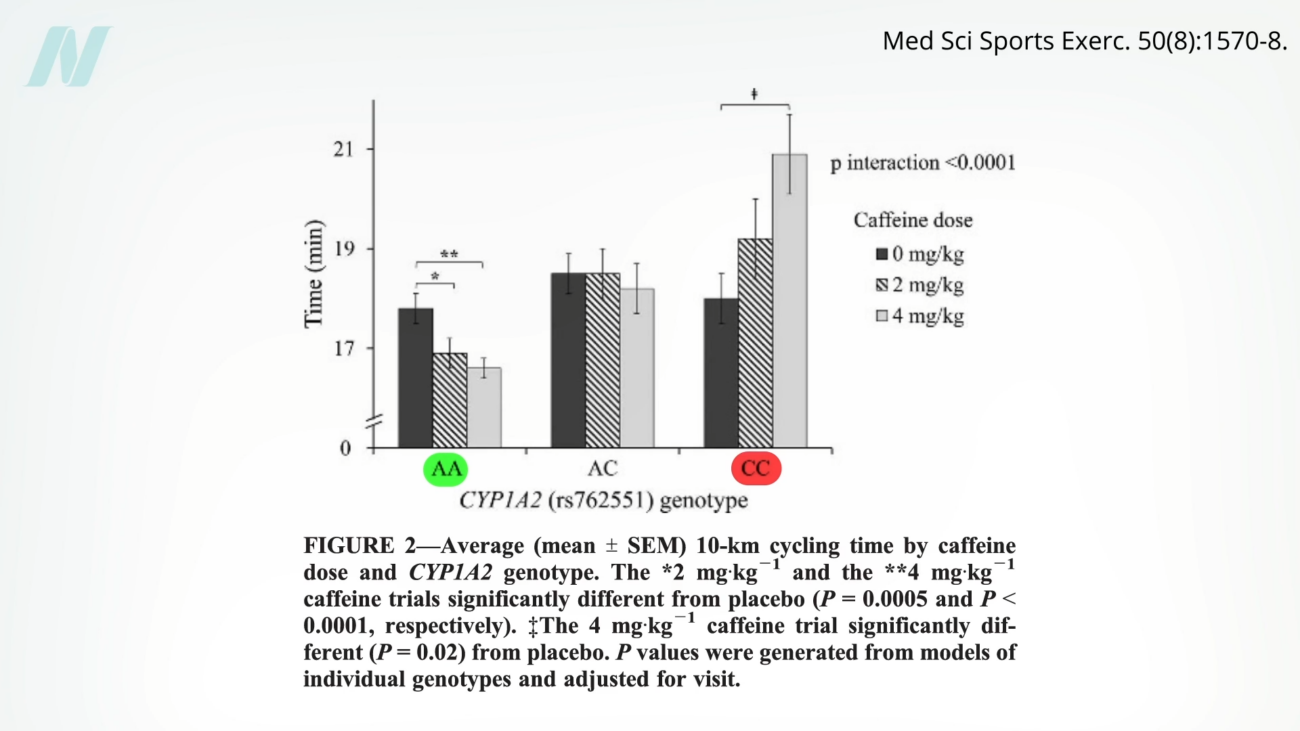
Further illustrating the impact of genetic individuality, research on caffeine metabolism offers compelling insights. A study published in Nature Communications (2016) revealed that the rate at which individuals metabolize caffeine, determined by genetic variations in the CYP1A2 gene, can significantly influence its health benefits and even athletic performance. Fast caffeine metabolizers may experience ergogenic effects, leading to performance enhancements such as shaving over a minute off a 10-kilometer cycling time trial. Conversely, slow metabolizers might see no benefit or even a performance decrease. This phenomenon underscores that while personalization can address specific biological differences, its broad application requires rigorous scientific validation.
The Pervasive Similarity: Beyond the Genetic Blueprint
Despite the compelling examples of genetic individuality, scientific consensus suggests that for the vast majority of the population, fundamental physiological similarities outweigh the differences. While the allure of highly individualized dietary plans is strong, current evidence supporting truly personalized nutrition for the general public remains insufficient. This gap between public perception and scientific reality has been exploited by a burgeoning industry of direct-to-consumer genetic testing companies. These companies often offer personalized nutrition advice, frequently linked to supplement recommendations, based on a limited number of genetic variants. However, studies, such as one published in the American Journal of Clinical Nutrition (2019), indicate that most genetic variants explain only a small fraction of the variance in nutrient levels between individuals, raising questions about the clinical utility of such advice.
The Broader Context: Personalized Medicine and Its Challenges
Personalized nutrition is an integral part of the wider movement towards personalized medicine, often referred to as precision medicine. This approach aims to tailor medical decisions, practices, interventions, and products to the individual patient based on their predicted response or risk of disease. The appeal of personal control over health, from diagnosis and treatment to prevention, is a powerful cultural force driving both demand and commercialization in this sector.
However, the realization of personalized medicine faces significant hurdles. While monogenic diseases, caused by a single gene defect like hemophilia or sickle cell anemia, lend themselves well to targeted genetic interventions, most common diseases are polygenic. These conditions arise from complex interactions between multiple genes and a multitude of environmental factors, making precise prediction and intervention a formidable challenge.

Unpacking the Complexity of Human Traits: The Case of Height
The intricate interplay of genetics and environment is evident even in seemingly straightforward traits like adult stature. Research, including a study in PLoS Genetics (2009), has identified hundreds of chromosomal locations associated with human height, a trait that is strongly heritable. Parental genes account for approximately 80% of the variation in height between individuals. Yet, the dozens of identified genes collectively explain only about 5% of this height variation.
This disparity highlights the limitations of current genetic analysis in predicting complex traits. Genome-wide association studies (GWAS), which scan entire genomes for statistical associations between diseases and specific DNA regions, are valuable research tools. However, companies marketing genetic susceptibility tests often oversimplify and reinterpret these findings as predictive of individual disease risk. The reality is that these identified genetic links typically represent modest associations with a slight increase in disease risk, offering little predictive power when compared to the more significant impact of lifestyle behaviors. Consequently, the practice of using an individual’s DNA to predict disease risk has been widely critiqued, with some research, such as a review in Nature Reviews Genetics (2018), concluding that it currently provides "little to no useful information" for clinical decision-making.
The Unwavering Power of Lifestyle: Foundational Health Strategies
Consider a hypothetical scenario where genetic analysis indicates a slightly elevated risk for a particular health condition. The advice typically rendered is universally sound: exercise regularly, maintain a healthy weight, limit alcohol consumption, and consume a diet rich in fruits, vegetables, and whole grains. This advice, while ostensibly personalized, reflects fundamental public health recommendations that should be adopted by everyone, irrespective of their genetic predispositions.
The critical challenge lies not in identifying the optimal lifestyle, but in its consistent implementation. Numerous studies and national surveys consistently reveal a widespread failure to adhere to even the most basic healthy living principles. For instance, nationwide surveys in the United States have shown that a vast majority of the population consumes a diet that falls short of even the most modest dietary guidelines. The stark reality, as reported in studies such as one in the Journal of the American Medical Association (2010), is that "almost no one in the United States is eating a healthy diet."
Reframing the Health Conversation: Personal Responsibility as the Cornerstone
The persistent gap between recommended healthy living and actual practice leads to a crucial re-evaluation of our focus. While personalized nutrition holds promise for specific medical needs, the broader public health conversation is often distracted by the complexities of genetic profiling. The evidence suggests that for the majority, the most impactful interventions are not found in intricate genetic blueprints but in the consistent application of well-established, fundamental health behaviors.
The obsession with personalizing preventive strategies based on genetic risk information can border on the absurd when the fundamental lifestyle factors are so widely neglected. The real revolution in public health may not come from decoding our DNA, but from empowering individuals to take ownership of their health through consistent, responsible choices regarding diet, exercise, and overall lifestyle. This fundamental shift, from seeking external personalization to embracing internal accountability, is arguably the most critical step in fostering a healthier society.
Doctor’s Note on Caffeine Metabolism and Athletic Performance
Further insight into the impact of individual genetic variations on health outcomes can be found in a video discussing fast versus slow caffeine metabolizers and their differing effects on athletic performance. This exploration, available at Friday Favorites: Do the Health Benefits of Coffee Apply to Everyone?, delves into how genetic makeup influences the ergogenic potential of caffeine, demonstrating that what benefits one individual may not benefit another, and can even have adverse effects.
Broader Implications for Public Health
The commercialization of personalized nutrition, while driven by a genuine desire for improved health, risks overshadowing the proven efficacy of fundamental lifestyle interventions. The focus on genetic predispositions, when not coupled with actionable, evidence-based lifestyle changes, can create a sense of fatalism or an over-reliance on supplements. The implications for public health policy and individual health choices are significant. Resources and public education efforts may be more effectively directed towards promoting adherence to established healthy eating patterns and regular physical activity. The scientific community and health professionals have a crucial role to play in clearly communicating the current limitations of personalized nutrition for the general population and emphasizing the foundational importance of personal responsibility in achieving and maintaining optimal health. The future of health may indeed lie in personalization, but perhaps the most profound personalization is the commitment each individual makes to their own well-being.