The stark contrast between the efficacy of healthy lifestyle choices and pharmaceutical interventions in preventing heart attacks is a critical public health revelation, with evidence suggesting that adopting a healthy lifestyle can reduce the risk of heart attack by as much as 90%, while medications may only achieve a 20% to 30% reduction. This significant disparity underscores the profound impact of long-term dietary and lifestyle habits on cardiovascular health, a finding that challenges conventional approaches to disease prevention and treatment. Atherosclerosis, the progressive hardening and narrowing of the arteries, identified as the leading cause of mortality for both men and women globally, begins its insidious development at an alarmingly young age, often during adolescence, according to extensive research.
The Silent Onset of Atherosclerosis: A Teenager’s Arteries
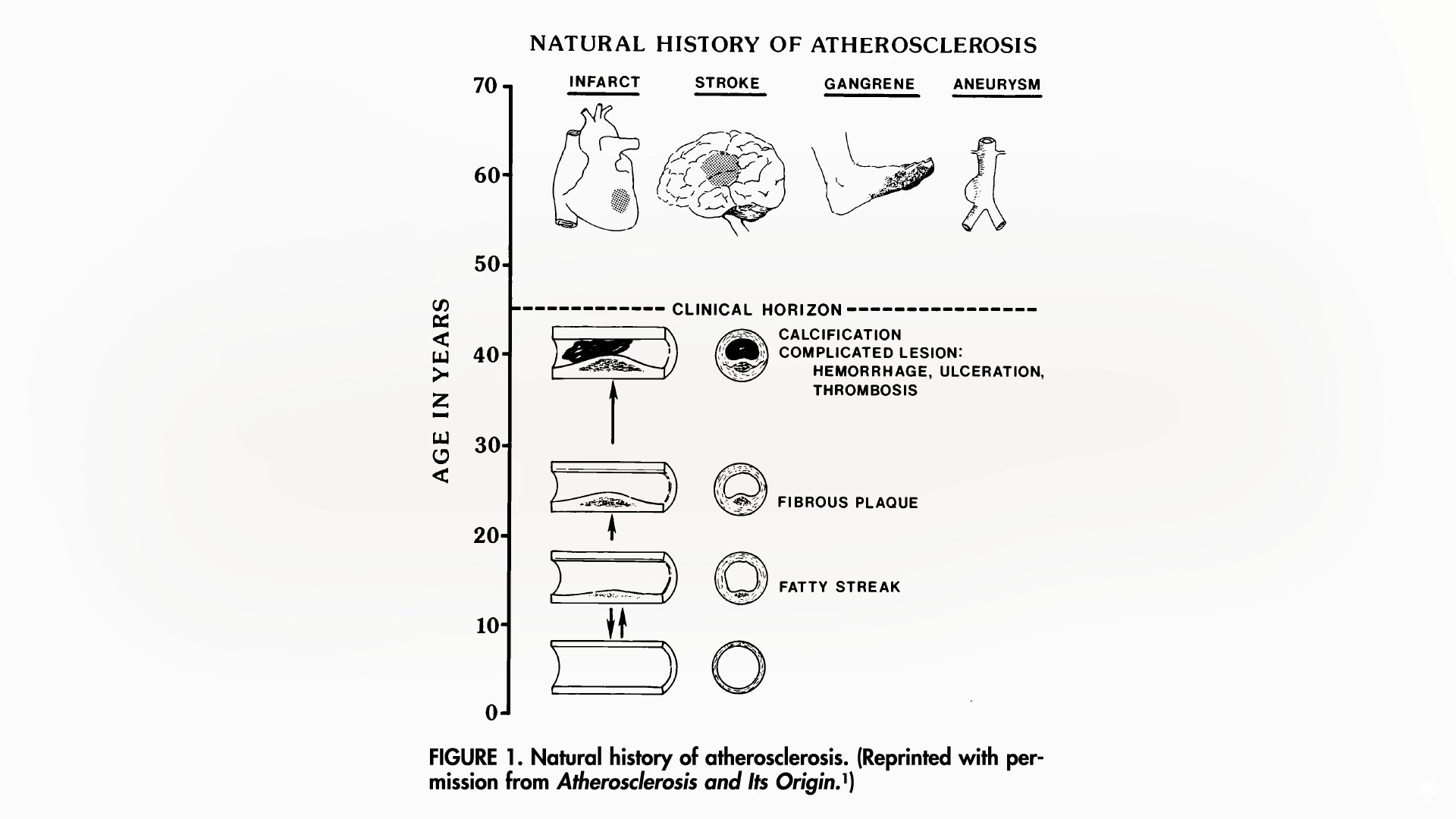
The standard American diet, characterized by its high content of saturated fats, cholesterol, and processed foods, has been identified as a primary driver of early atherosclerotic development. A landmark study involving the examination of approximately 3,000 sets of coronary arteries and aortas from individuals aged 15 to 34 years, who were victims of accidental deaths, homicides, and suicides, revealed a disturbing trend. Investigators discovered that the initial stages of atherosclerosis, known as fatty streaks, can commence forming in the arteries during the teenage years. By the twenties, these fatty streaks evolve into atherosclerotic plaques, which continue to grow and worsen throughout the thirties, ultimately leading to potentially fatal cardiovascular events.
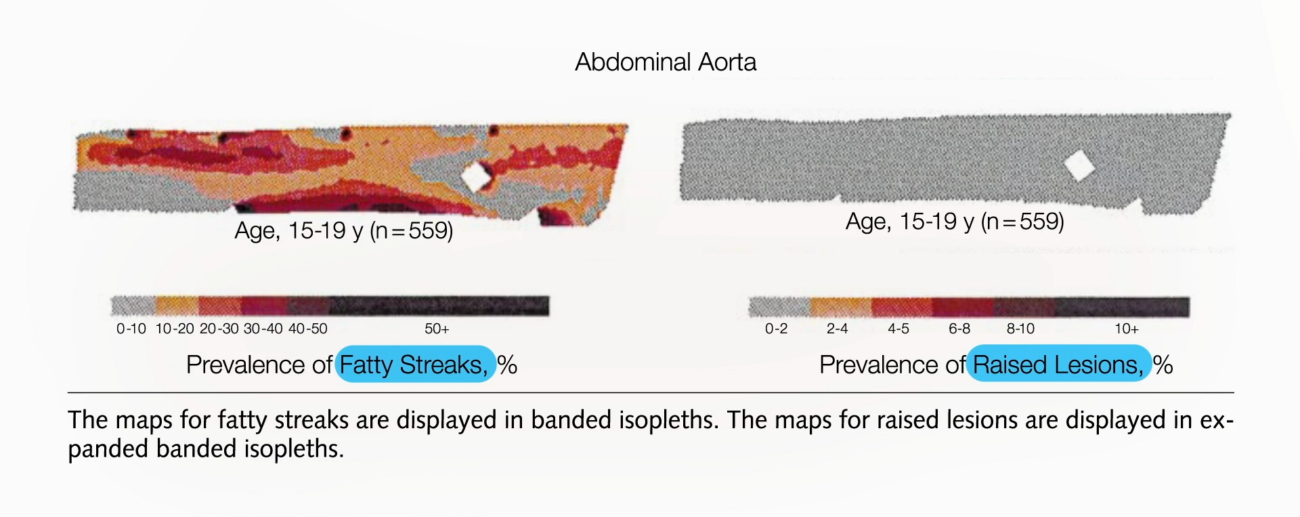
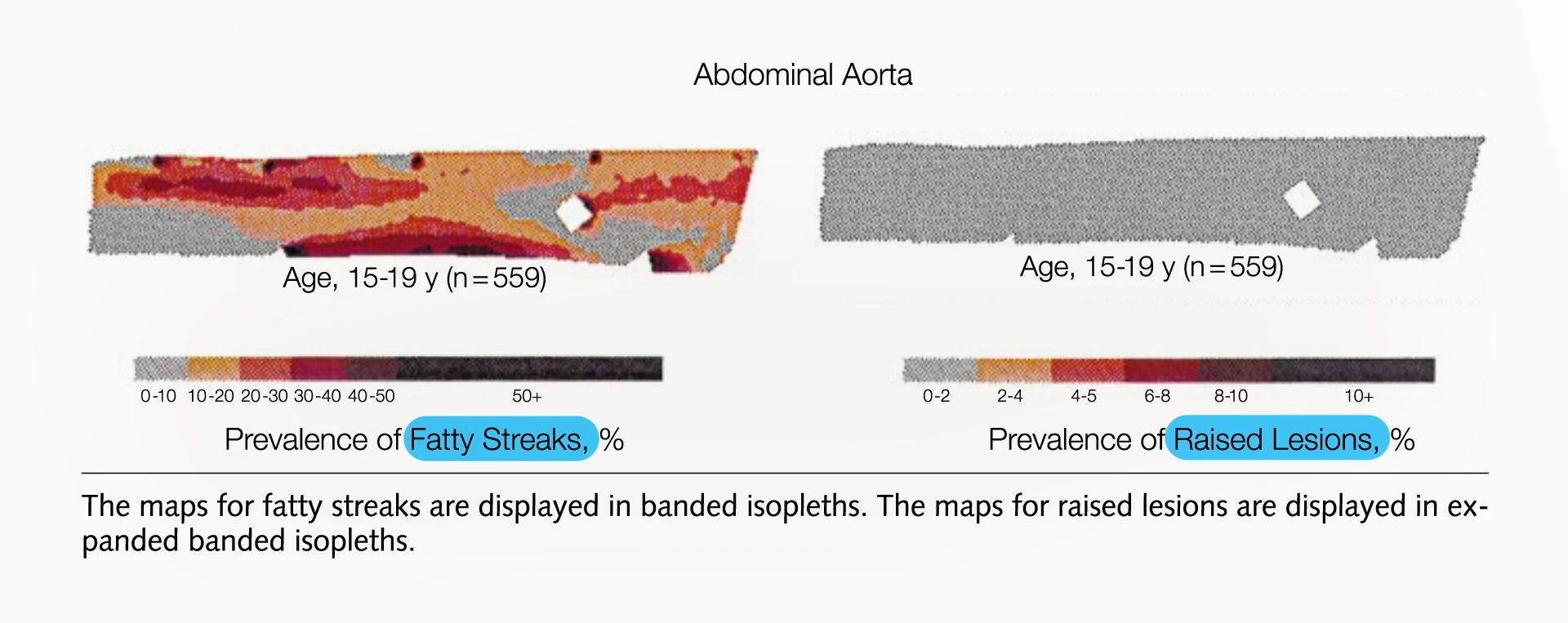
The implications of this early onset are profound. Atherosclerosis in the coronary arteries can precipitate heart attacks, while its manifestation in the brain’s arteries can result in strokes. Visualizations of this progression, often presented in scientific literature and educational materials, depict a clear timeline: from the initial fatty streaks in adolescence to the development of more advanced plaques in early adulthood. For instance, research published in journals such as PubMed has meticulously documented this process. A study focusing on young accident victims between the ages of 15 and 19 found that 100% of them exhibited fatty streaks within their arteries. This prevalence rose sharply in subsequent age groups. By their early twenties, evidence of atherosclerotic plaques began appearing, particularly in the abdominal aorta, the main artery extending from the chest to the pelvis. By their late twenties and early thirties, these plaques had become more widespread and advanced, significantly compromising the arterial lumen.

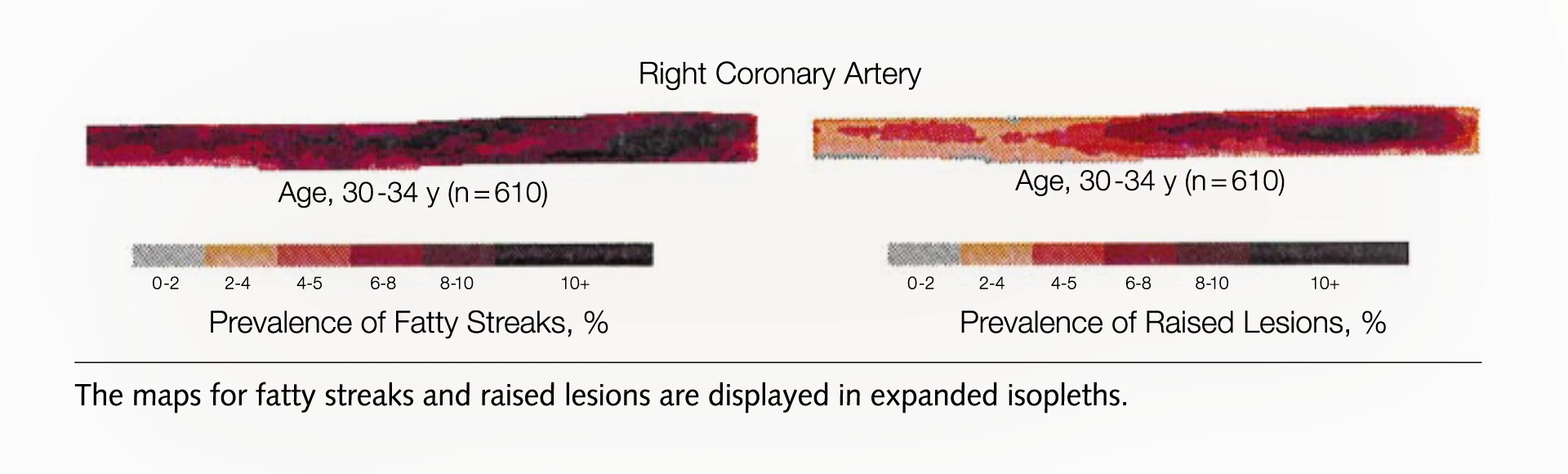
The findings were consistent across different arterial regions. In the coronary arteries, which supply blood to the heart muscle, the pattern mirrored that observed in the aorta. Fatty streaks were prevalent in adolescents, with early signs of plaque formation emerging in individuals in their early twenties. By their early thirties, a significant majority of individuals in the study cohort displayed established plaques within their coronary arteries. This early pathological process, often occurring long before any symptoms manifest, highlights the critical need for preventative strategies to be implemented from a much younger age.
The Early Warning Signs: Atherosclerosis from Adolescence Onward
The chronological progression of atherosclerosis, as documented in scientific investigations, paints a clear picture of its relentless development. Studies have shown that as early as 15 to 19 years of age, the aortas of young individuals, typically considered to be in the prime of their health, already exhibit widespread fatty streaks. These are characterized as the earliest visible lesions of atherosclerosis, appearing as yellowish discolorations on the inner lining of the artery. While these initial lesions do not typically impede blood flow, they represent the foundational stage for the more serious plaque development to come.
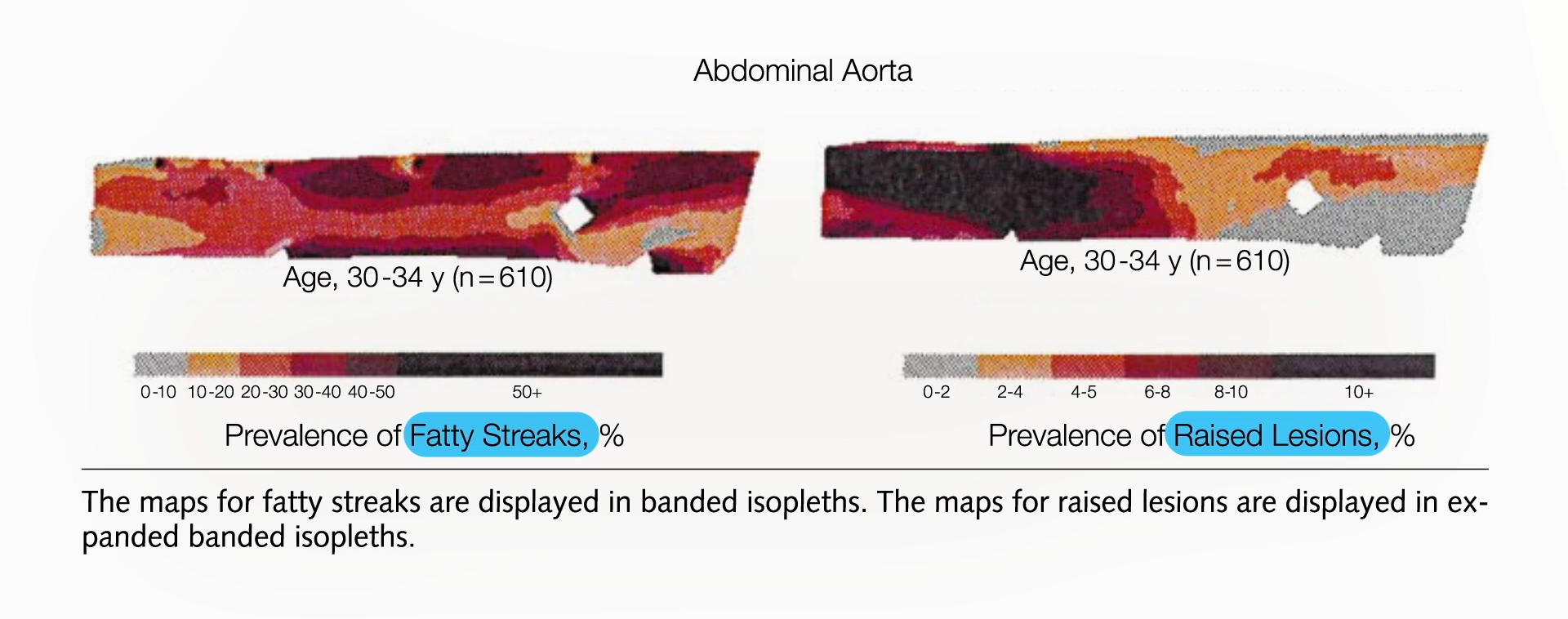
As individuals enter their twenties, the pathological process accelerates. Fatty streaks begin to transition into more complex atherosclerotic plaques. These plaques are composed of lipids (fats), inflammatory cells, smooth muscle cells, and connective tissue. They protrude into the arterial lumen, the inner space through which blood flows, narrowing the passage. Research indicates that by their early twenties, plaques start appearing in the abdominal aorta, and this trend continues to worsen through their late twenties. During this period, the arterial walls undergo significant changes, with the accumulation of plaque material leading to a reduction in the artery’s elasticity and a thickening of its wall.
By the early thirties, the arteries are often described as being in "bad shape." This description refers to the substantial presence of atherosclerotic plaques, not only in the aorta but also in the crucial coronary arteries. The progression from fatty streaks to advanced plaques within a couple of decades underscores the aggressive nature of this disease process when fueled by an unfavorable diet and lifestyle. The absence of symptoms during these formative years often leads to a false sense of security, delaying crucial interventions until significant and potentially irreversible damage has occurred.
The Case for Proactive Prevention: Beyond Symptomatic Treatment
The prevailing medical paradigm often focuses on treating diseases once they become symptomatic. However, the early and silent onset of atherosclerosis fundamentally challenges this approach. Health experts and researchers advocate for a shift towards primordial prevention, a strategy aimed at preventing the development of risk factors and diseases before they even manifest. The analogy of treating a cancerous tumor or advanced diabetes is apt: no one would advocate waiting for a tumor to grow to a significant size or for a diabetic to lose their sight before initiating treatment. Similarly, addressing atherosclerosis requires proactive measures, particularly when its roots are firmly established in adolescence.
The primary mechanism for treating atherosclerosis, as supported by scientific evidence, involves lowering LDL cholesterol levels. This is most effectively achieved through dietary modifications that emphasize a reduction in saturated fat and dietary cholesterol. Such a diet typically involves limiting the consumption of eggs, meat, and dairy products, which are significant sources of these components, and minimizing "junk" food, which often contains unhealthy fats, sugars, and refined carbohydrates.
A Radical Proposal? Rethinking Lifestyle as a Primary Intervention
The call for altering lifestyle habits, beginning in infancy or early childhood, might seem like a "radical proposal" to some, as noted in research discussions. However, when considering that atherosclerosis is the leading cause of death, such a fundamental change in behavior is not only justifiable but essential. The success in curbing smoking rates and subsequently reducing lung cancer incidence serves as a powerful precedent, demonstrating that widespread behavioral change is achievable and can have a dramatic positive impact on public health.
The safety and appropriateness of healthy eating patterns, including strictly plant-based diets, have been affirmed by reputable organizations such as the Academy of Nutrition and Dietetics. They recognize these diets as suitable for all stages of life, commencing from pregnancy. This endorsement provides a strong foundation for advocating for widespread adoption of healthier eating habits from the earliest years.
The "Cure" for Atherosclerosis: A Lifelong Commitment to Low LDL
A pivotal study published in the Journal of the American College of Cardiology declared that "Curing Atherosclerosis Should Be the Next Major Cardiovascular Prevention Goal." This ambitious statement underscores the potential for not just managing but actively reversing or halting the progression of this pervasive disease. The evidence supporting the long-term efficacy of maintaining low LDL cholesterol levels is compelling.
Researchers have identified a genetic mutation in the PCSK9 gene, present in approximately 1 in 50 African Americans, which naturally leads to about a 40% reduction in LDL cholesterol throughout their lives. Individuals with this genetic predisposition exhibit significantly lower rates of coronary heart disease – an impressive 88% reduction in risk compared to those without the mutation. This holds true even when other cardiovascular risk factors are present, such as high blood pressure, overweight or obesity, smoking, and diabetes. This observation powerfully illustrates the protective effect of a lifelong history of low LDL cholesterol.
The crucial insight derived from this genetic anomaly is that a reduction in LDL cholesterol of about 40 mg/dL, achieved through this natural mechanism, correlates with a nearly 90% decrease in coronary heart disease events. This occurred at an average LDL level of 100 mg/dL, compared to 138 mg/dL in the control group. This suggests that sustained low LDL levels, even those not drastically low, can offer profound protection.
Duration vs. Dosage: The Key to Lifestyle’s Dominance
The remarkable difference in risk reduction between the genetically determined low LDL and that achieved with statin drugs raises a critical question: why does a similar reduction in LDL cholesterol yield such vastly different outcomes? The most probable explanation lies in the duration of the intervention. While statin drugs can effectively lower LDL cholesterol, their impact on risk reduction is often limited to 20% to 30% when initiated later in life. In contrast, the genetic mutation provides a lifelong advantage, demonstrating that the length of time LDL cholesterol remains low is a paramount factor.
This principle explains why healthy lifestyle choices can potentially eliminate up to 90% of heart attack risk. By adopting healthy habits early in life and maintaining them consistently, individuals can achieve and sustain lower LDL cholesterol levels for decades. This prolonged period of reduced arterial stress and inflammation allows the body to mitigate the development and progression of atherosclerosis far more effectively than sporadic or late-stage pharmaceutical interventions.
For individuals relying on medication later in life to halt disease progression, achieving an LDL level below 70 mg/dL may be necessary. However, for those who have engaged in healthy eating habits throughout their lives, an LDL level around 100 mg/dL might be sufficient to prevent or significantly slow the progression of coronary atherosclerosis. This aligns with epidemiological data suggesting that heart disease mortality rates tend to bottom out when population-wide average LDL cholesterol levels are around 100 mg/dL.
The Spectrum of Intervention: From Prevention to Reversal
The efficacy of LDL reduction varies depending on the individual’s health status and the timing of intervention. For individuals who have already experienced a heart attack and are at high risk of subsequent events, aggressive LDL reduction may be crucial. In such cases, achieving LDL levels below 70 mg/dL is often recommended. If the aim is to reverse the effects of a lifetime of unhealthy choices through medication, LDL levels might need to drop as low as 55 mg/dL to achieve a near-zero risk of recurrent coronary heart disease events.
For individuals with severe heart disease, aiming for an LDL level as low as 30 mg/dL could not only prevent the formation of new atherosclerotic plaques but also help stabilize existing ones. This stabilization is critical, as unstable plaques are more prone to rupture, leading to blood clots that can cause heart attacks and strokes.
The Safety of Low Cholesterol: A Continuing Inquiry
A vital question that arises in the context of aggressive LDL reduction is the safety of achieving very low cholesterol levels. While the benefits in cardiovascular disease prevention are clear, ongoing research continues to explore whether LDL cholesterol can become "too low" and what potential implications this might have for overall health. This area of inquiry remains a focus for scientists and clinicians, aiming to provide comprehensive guidance on optimal cholesterol management.
Doctor’s Note: Early Intervention is Key
The findings underscore a critical message: heart disease does not begin in adulthood; it originates in childhood. Therefore, preventative measures must also begin at this formative stage. Early adoption of healthy lifestyle choices, particularly dietary habits, can lay the foundation for a lifetime of cardiovascular health. The debate between the actual benefits of diet versus drugs continues to highlight the superior long-term impact of lifestyle modifications. Furthermore, the concept of "primordial prevention" – actively working to maintain a low-risk profile throughout life – is paramount. This proactive approach, focusing on lifestyle, rather than reactive treatment of established disease, represents the most effective strategy for combating the leading cause of death globally. The question of whether cholesterol size matters in cardiovascular risk is also an important consideration, with research indicating that the size and density of LDL particles can play a role in their atherogenicity.