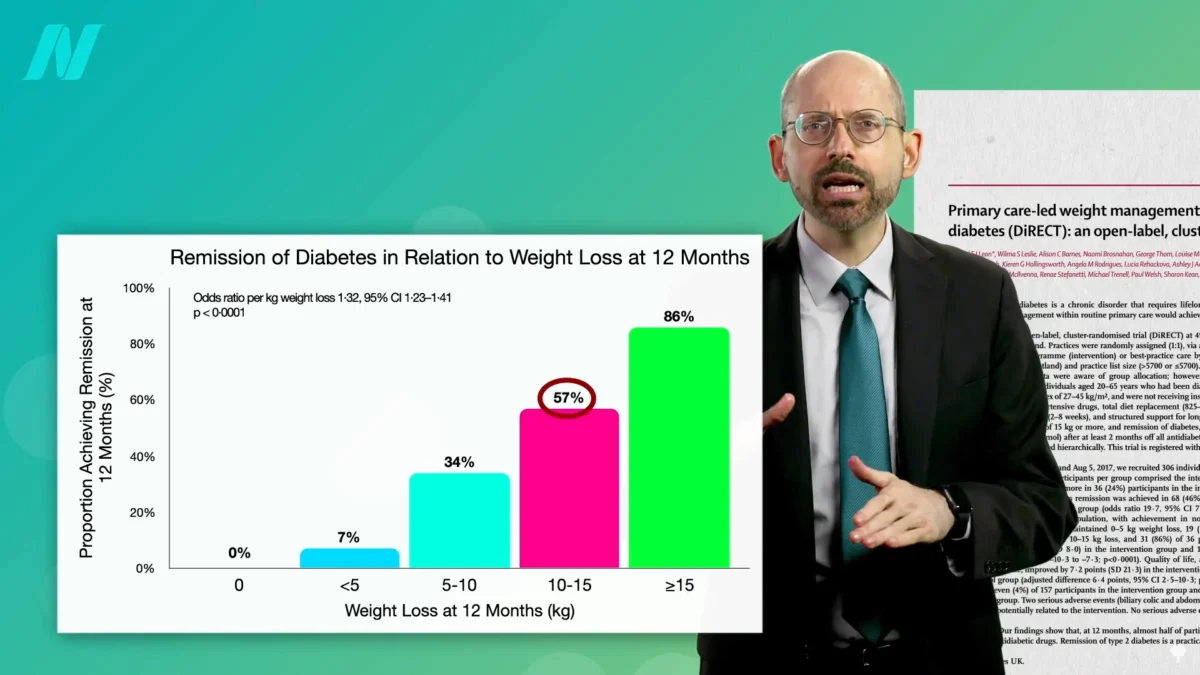
The landscape of type 2 diabetes management is undergoing a significant paradigm shift, with emerging evidence strongly suggesting that substantial weight loss can lead to remission for a vast majority of individuals, particularly those diagnosed in the earlier stages of the disease. Current research indicates that achieving a 15% reduction in body weight can result in remission for nearly 90% of individuals who have lived with type 2 diabetes for less than four years. This finding carries profound implications for public health, especially considering the escalating global prevalence of diabetes.
The Growing Diabetes Epidemic
The World Health Organization estimates that over half a billion adults worldwide currently live with diabetes. Projections indicate a staggering 50% increase in this number within the next generation, placing immense pressure on healthcare systems and individual well-being. Type 2 diabetes, once considered a condition predominantly affecting affluent individuals with sedentary lifestyles and excessive diets, is now a widespread public health challenge. Its preventable nature has long been recognized, and the focus is increasingly shifting towards its treatability and potential for reversal.
Historical Perspectives on Diabetes Treatment
The concept of using dietary restriction to manage diabetes is not new; in fact, historical accounts reveal a long-standing, albeit sometimes extreme, understanding of its efficacy. More than a century ago, fasting was recognized for its potential to halt the progression of diabetes and eliminate its symptoms within days or weeks. Ancient medical texts, dating back approximately 2,000 years to Ayurvedic traditions, proposed radical approaches to managing the disease, suggesting extreme dietary deprivation or strenuous physical activity. One such ancient prescription advised individuals with diabetes to "live like a saint," undertake extensive walking, or even subsist on very limited, unconventional sustenance.
This historical thread of dietary restriction continued through centuries, albeit with varying degrees of scientific rigor and ethical consideration. In 1797, a regimen known as the Rollo diet was proposed, which notably included rancid meat and emetics to induce vomiting. While such methods undoubtedly reduced food intake and temporarily alleviated symptoms, they were largely based on inducing sickness rather than addressing the underlying physiological mechanisms. The unintended consequence of severe food restriction, regardless of its method, was a reduction in caloric intake, which directly impacted blood glucose levels.
During the siege of Paris in the Franco-Prussian War, the extreme scarcity of food led to observations of improved diabetic control among the affected population. This period fostered the principle of "mangez le moins possible" – "eat as little as possible." This philosophy was later formalized into the Allen starvation treatment, developed by Dr. Frederick M. Allen in the early 20th century. Prior to the discovery of insulin, the Allen treatment was considered a monumental advancement in diabetes management. Dr. Allen’s clinical observations revealed that severe diabetes cases often improved following "wasting conditions" such as tuberculosis or cancer, leading him to hypothesize that a controlled state of calorie deprivation could yield similar results.
Dr. Allen’s Groundbreaking Research and the "Allen Era"
Dr. Allen’s meticulous research, documented in leading medical journals of the time, demonstrated that even individuals with the most severe forms of type 2 diabetes could achieve sugar-free urine within ten days through strict caloric restriction. His approach was centered on two core principles: maintaining an underweight status for patients and severely limiting dietary fat. He observed that the reintroduction of even small amounts of fat, such as butter or olive oil, could trigger a rapid return of diabetic symptoms. This period, often referred to as "The Allen Era," underscored the critical link between dietary intake, body weight, and diabetes control before the advent of insulin therapy.

The Role of Fat Toxicity in Type 2 Diabetes
Modern scientific understanding has further illuminated the physiological underpinnings of type 2 diabetes, framing it as a condition of "fat toxicity." Research has demonstrated that infusing fat into the bloodstream, even for a short duration, can lead to the rapid accumulation of fat within muscle cells, impairing insulin sensitivity. This effect is mirrored by consuming high-fat diets, which can induce insulin resistance within days, and in some cases, even after a single meal.
The mechanism is as follows: when the body’s muscle cells become saturated with fat, they become less responsive to insulin, the hormone responsible for facilitating glucose uptake from the bloodstream. This state of insulin resistance, coupled with excessive caloric intake, triggers a cascade of metabolic dysfunctions. Initially, the liver may accumulate excess fat, leading to non-alcoholic fatty liver disease. Subsequently, fat deposition can occur in the pancreas, impairing the function of insulin-producing beta cells. This progressive fat accumulation in key metabolic organs ultimately culminates in the full manifestation of type 2 diabetes.
Crucially, research indicates that type 2 diabetes can be understood as a state of excess fat within the liver and pancreas, and importantly, this condition remains reversible for a significant period, often up to 10 years after diagnosis.
Weight Loss as a Reversal Agent
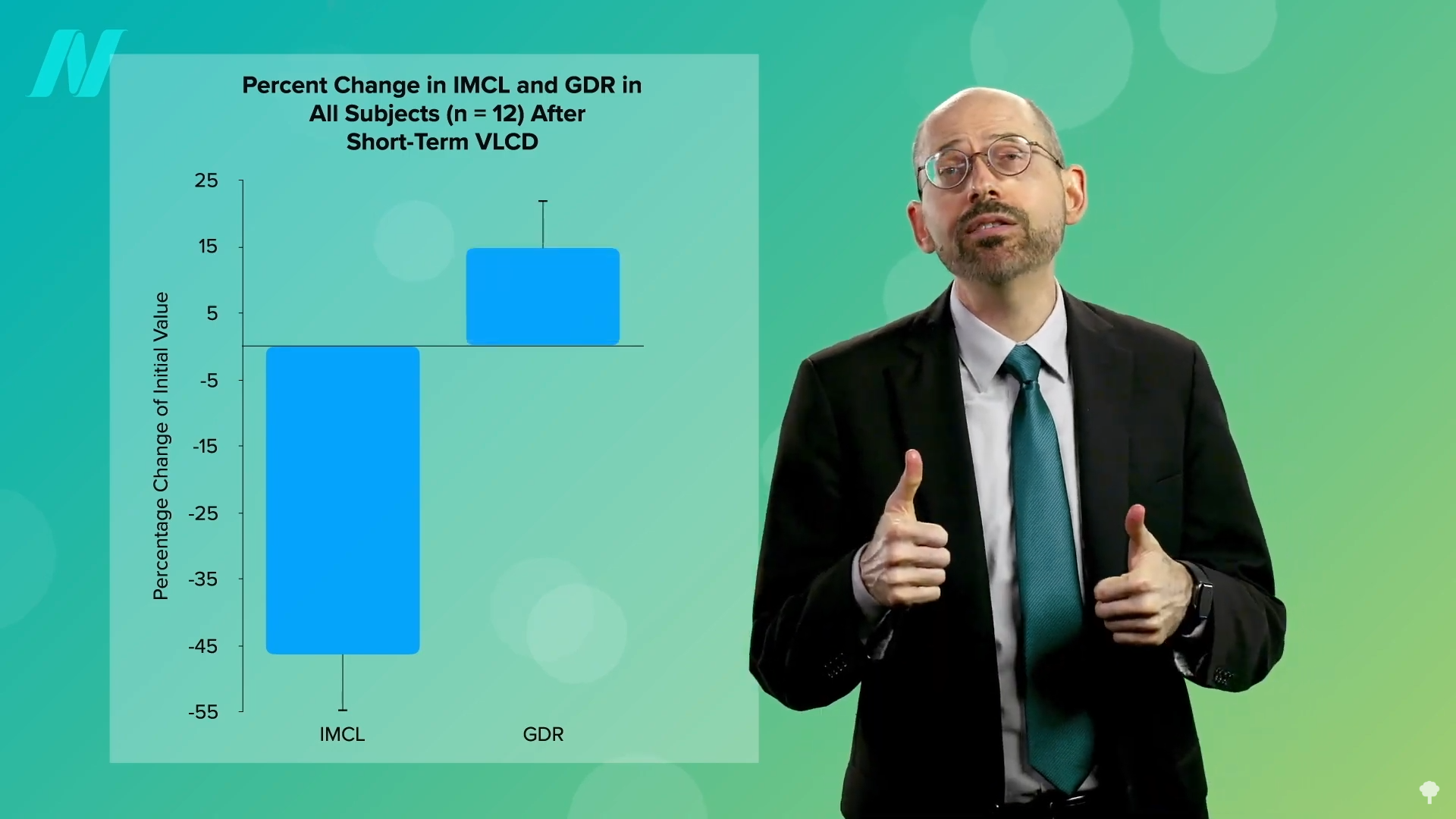
The therapeutic power of weight loss in reversing type 2 diabetes is becoming increasingly evident. Studies employing very low-calorie diets, typically around 700 calories per day, have shown a remarkable ability to mobilize excess fat from muscle cells, leading to a corresponding improvement in insulin sensitivity. This process, when sustained, can result in a substantial reduction of fat accumulation in the liver. If the dietary intervention continues, the excess fat within the pancreas also diminishes, paving the way for potential remission of the disease.
The significance of weight loss is quantified by the degree of body mass reduction. As previously mentioned, a 15% loss of body weight has demonstrated remarkable efficacy in achieving non-diabetic blood sugar levels for nearly 90% of individuals diagnosed with type 2 diabetes within the last four years. This remission rate significantly surpasses the outcomes observed with bariatric surgery, a more invasive procedure. Studies comparing weight loss interventions have found that even when bariatric surgery leads to greater weight reduction, remission rates for type 2 diabetes are lower, around 62% for those achieving substantial weight loss, compared to the much higher rates seen with dietary and lifestyle interventions.
The impact of weight loss is also time-dependent. Individuals who have lived with type 2 diabetes for longer periods may experience less favorable remission rates. For instance, remission may only be achievable in approximately 50% of those who have had the disease for more than eight years. This highlights the critical window of opportunity for intervention and reversal.
Further research indicates that for individuals diagnosed with type 2 diabetes for an average of three years, losing approximately 30 pounds can lead to disease reversal. This underscores the potent therapeutic potential of dietary changes and weight management, suggesting that "your forks are better than surgeons’ knives."
The Role of Fasting and Sustained Weight Management
Extended periods of physician-supervised, water-only fasting have also been shown to induce significant weight loss and facilitate diabetes remission. However, the long-term success of such interventions hinges on the ability to maintain the achieved weight loss. Scientific consensus holds that weight regain is directly correlated with the recurrence of diabetes. This emphasizes that the reversal of type 2 diabetes is not a temporary fix but a commitment to sustained healthy lifestyle choices.
The Evolution of Diabetes Management: Beyond Insulin
The discovery of insulin in 1921 was hailed as one of medicine’s greatest miracles, offering a life-saving treatment for individuals with type 1 diabetes. However, for those with type 2 diabetes, while insulin provided crucial management, it did not inherently prevent long-term complications such as blindness, kidney failure, stroke, and amputations. This realization led prominent diabetes care pioneers, such as Elliott Joslin, to advocate for the continued centrality of diet and exercise in managing type 2 diabetes, even in the era of insulin. His argument was that the self-discipline required for dietary adherence and physical activity, as practiced before insulin’s availability, remained fundamental to effective diabetes management.
Analyzing the Implications
The growing body of evidence supporting weight loss as a primary driver for type 2 diabetes remission has profound implications for public health policy, clinical practice, and individual patient care.
- Shift in Treatment Paradigms: This research challenges the traditional view of type 2 diabetes as an irreversible, progressive disease. It empowers healthcare providers to offer more optimistic prognoses and implement aggressive weight management strategies as a cornerstone of treatment.
- Preventive Health Focus: The strong link between excess weight and type 2 diabetes reinforces the importance of public health initiatives focused on preventing obesity and promoting healthy lifestyles from an early age.
- Cost-Effectiveness: Non-invasive interventions like dietary changes and weight loss are generally more cost-effective than long-term medication use and the management of diabetes-related complications. This could lead to significant savings in healthcare expenditure.
- Patient Empowerment: Understanding that type 2 diabetes can be reversed empowers individuals to take an active role in their health, fostering a sense of agency and motivation to adopt sustainable lifestyle changes.
- Future Research Directions: Continued research is needed to identify the most effective and sustainable weight loss strategies for diverse populations, explore the long-term durability of remission, and understand the precise biological mechanisms that govern the reversibility of type 2 diabetes.
Doctor’s Note on Fat Toxicity
For a deeper understanding of the underlying causes of type 2 diabetes, particularly its relationship with fat accumulation, consulting resources on "Diabetes as a Disease of Fat Toxicity" is highly recommended. These resources provide detailed scientific explanations of how excess dietary fat contributes to insulin resistance and pancreatic dysfunction.
The Broader Impact on Weight Management and Disease Prevention
The insights gained from studying diabetes reversal also inform broader discussions on weight management and disease prevention. While extended fasting can be a powerful tool for initiating weight loss, it is not universally the most effective or sustainable method for long-term weight management. The optimal approach to weight loss and overall disease prevention typically involves a balanced, nutrient-dense diet and regular physical activity, as detailed in resources discussing "The Best Diet for Weight Loss and Disease Prevention." The key takeaway is that sustained weight loss, achieved through consistent healthy habits, is the critical factor in both reversing and preventing type 2 diabetes and a host of other chronic diseases.