The global quest for a slimmer physique has, throughout history, driven individuals to explore a bewildering array of approaches, some grounded in science, others veering into the realm of the bizarre and the potentially dangerous. While established methods like diet and exercise remain the cornerstones of healthy weight management, the allure of rapid results has fueled the development and promotion of radical interventions. This article delves into the safety and efficacy of several such methods, from invasive surgical procedures and device-assisted interventions to historically questionable practices, offering a critical examination of their scientific basis, potential risks, and the broader implications for public health.
The stark reality of modern dietary habits often undermines even the most diligent efforts at calorie expenditure. Consider a moderately obese individual engaging in moderate physical activity, such as cycling or brisk walking. For an hour, they might burn approximately 350 calories. However, the caloric density of many contemporary food and beverage items presents a formidable challenge. A mere minute spent consuming processed snacks or sugary drinks can easily account for 70 calories (293 kJ). This means that a mere five minutes of indulgence can negate an entire hour of strenuous exercise, illustrating the uphill battle many face in achieving a caloric deficit through activity alone. This imbalance has, in part, paved the way for more extreme interventions.
The AspireAssist Siphon System: A Controversial Intervention
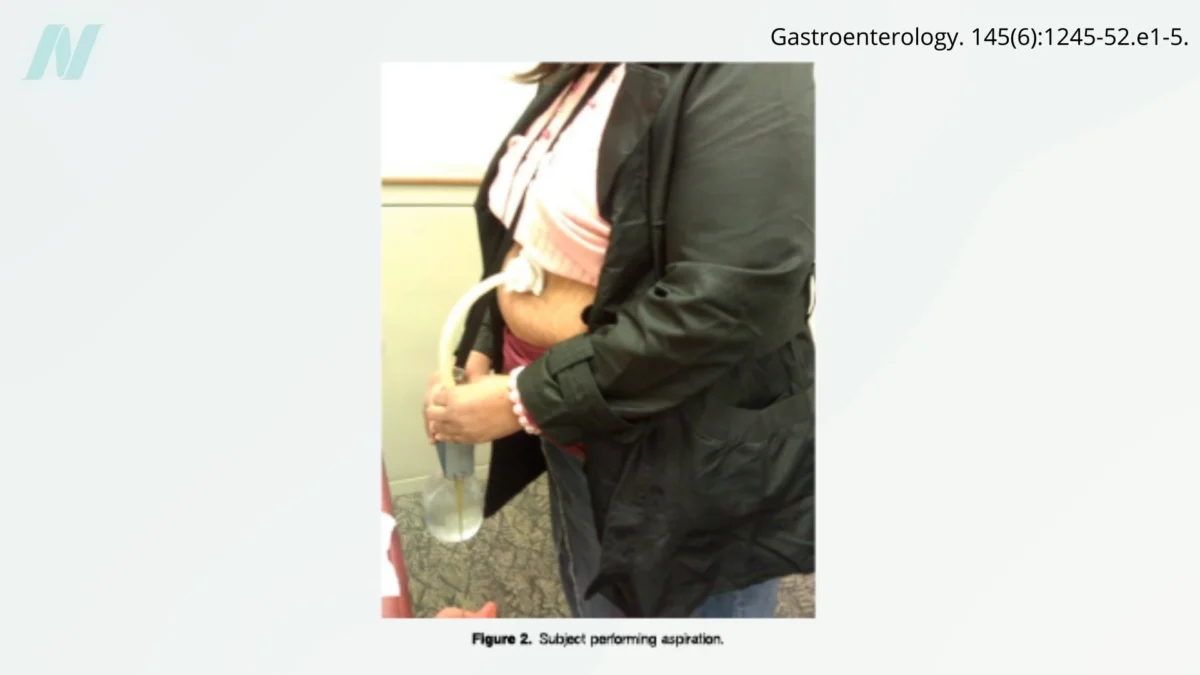
One such intervention that has garnered significant attention, and indeed controversy, is the AspireAssist siphon assembly. This device, classified as a percutaneous gastrostomy, involves a surgically created opening in the stomach, a fistula tunneled through the abdominal wall. Post-meal, users can attach a suction device to this opening to drain a portion of their stomach contents. The process essentially allows individuals to consume food and then mechanically remove a significant percentage of it before it can be fully digested and absorbed.
The theoretical underpinning of the AspireAssist is straightforward: reduce the net caloric intake by expelling food. However, the practical implications are far more complex. Reports suggest that patients using the device can indeed lose weight. Several factors may contribute to this: the physical presence of the fistula might influence gastric wall relaxation, potentially leading to earlier feelings of fullness. Furthermore, the protocol often necessitates the consumption of substantial amounts of water and thorough chewing, habits that can independently aid in weight management by promoting hydration and slowing the eating process. Perhaps most significantly, patients have reportedly begun making healthier food choices to avoid the visually unappealing prospect of aspirating less healthy foods. The clear tubing of the device reportedly makes fried foods, in particular, appear quite unappetizing when expelled.
However, the AspireAssist is not without its drawbacks and risks. A critical concern is the potential for nutritional deficiencies. The aspiration process can remove essential nutrients, including potassium, necessitating supplementation to prevent deficiency, a complication also observed in individuals with bulimia. While serious adverse effects like abdominal abscesses are reported as rare, minor wound complications are more common. The device’s primary appeal, according to its proponents, is that it does not alter the fundamental anatomy of the gastrointestinal tract. In the often unregulated landscape of weight-loss procedures, this distinction is presented as a significant advantage.
The Duodenal-Jejunal Bypass Liner: An Invasive Approach to Calorie Malabsorption
Another intervention that bypasses traditional surgical alterations of the gastrointestinal tract is the duodenal-jejunal bypass liner. This approach draws inspiration from the principles of gastric bypass surgery, which reroutes food away from a portion of the small intestine to limit calorie absorption. Instead of extensive surgery, the duodenal-jejunal bypass liner involves inserting a flexible plastic tube, approximately two feet in length, to line the walls of the small intestine.
The challenge with this method lies in its secure placement. The liner must be anchored within the digestive tract, a process that utilizes ten barbed hooks. These hooks are associated with a high incidence of adverse effects, reportedly causing lacerations and contributing to the vast majority of the 891 adverse events documented in a study of 1,056 patients – a staggering rate of nearly 9 out of 10 individuals experiencing some form of complication. More severe outcomes, such as penetrating trauma leading to esophageal perforation or liver abscesses, while rarer, occur in approximately 1 in 27 patients, highlighting the significant risks associated with this procedure.
Intestinal Ablation: A Radical Intervention for Calorie Absorption
Beyond mechanical interventions, more drastic measures have been explored, including procedures aimed at altering the absorptive capacity of the intestines. While the "palatability" of stomach pumping devices like AspireAssist has been questioned, even more unsettling endoscopic interventions have emerged. One such procedure, referred to as intestinal "resurfacing," involves a more aggressive approach than simply lining the intestines with plastic. This method entails "thermally ablating the superficial duodenal mucosa," essentially burning off the intestinal lining. The rationale is to reduce the surface area available for nutrient absorption. This radical procedure, which literally involves destroying and regenerating the intestinal lining, raises profound questions about long-term health consequences and the ethical boundaries of weight-loss interventions.
Botulinum Toxin (Botox) Injections: A Failed Pharmaceutical Approach
In the pharmaceutical realm, interventions have also been attempted with limited success. Researchers have explored injecting Botulinum toxin (Botox) into the stomach walls of obese individuals. The theory was that this would partially paralyze the gastric muscles, slowing stomach emptying and inducing a prolonged feeling of fullness, thereby facilitating weight loss. However, clinical trials have largely demonstrated that this method is ineffective, failing to produce the desired weight-loss outcomes.

Corsets and Tapeworms: Historical Echoes and Persistent Myths
The history of weight loss is replete with methods that are now considered unscientific or even dangerous. The use of corsets, for instance, was explored in a study where participants were instructed to wear them for extended periods daily over nine months. The study concluded that the method was ineffective, primarily because participants found the corsets uncomfortable and did not adhere to the regimen. This echoes a common theme in many extreme weight-loss attempts: the difficulty of long-term compliance with uncomfortable or impractical interventions.
Even more disturbing are historical accounts of "sanitized tapeworms" being advertised as weight-loss remedies as far back as the early 20th century. The notion of intentionally infesting oneself with parasites for weight loss is a chilling reminder of the desperation that can drive individuals to seek unconventional solutions. Evidence of living tapeworms being discovered during bariatric surgery operations suggests that such parasitic infestations are not only ineffective but also pose significant health risks.
The Psychology of Disgust: A Novel Approach to Appetite Control
In a more nuanced and psychologically oriented approach, research has explored "harnessing the power of disgust" to reduce the appeal of high-calorie foods. One study employed implicit priming techniques, where subliminal messages were used to influence food preferences. Before presenting images of healthy foods, participants were briefly shown positive images, such as kittens, to create a positive association. Conversely, before displaying images of high-calorie foods like ice cream, negative scenes, including cockroaches on pizza, vomit, and burn wounds, were flashed for mere milliseconds. This rapid, subliminal exposure aimed to create an aversive response to unhealthy food cues. The findings indicated that subjects subsequently reported a reduced desire for high-calorie foods, suggesting that leveraging disgust through subconscious priming could be a potential tactic to combat the pervasive influence of food cues that promote unhealthy eating habits.
Neuromodulation and Invasive Brain Stimulation: The Limits of Intervention
The pursuit of weight loss has even extended into the realm of the brain. Researchers have investigated methods involving electrical stimulation, both within the digestive system and directly in the brain, to influence appetite and food intake. Studies exploring implantable gastric stimulation, involving electrodes inserted into the stomach wall, and even colon electrical stimulation, have yielded limited success.
More dramatically, experiments have involved "repetitive electric brain stimulation" aimed at reducing food intake. While placing deep-brain electrodes is a high-risk surgical procedure, scientists have long pondered the possibility of modulating brain activity to curb appetite. In one study, holes were drilled into the skulls of five obese individuals, and wires were inserted into their brains for "electrostimulatory exploration." The objective was to identify specific brain regions that, when stimulated, could elicit hunger responses. Upon identifying these areas, researchers delivered electrical currents, intending to create electro-coagulatory lesions. While such techniques showed promise in animal models like cats and monkeys, the application to obese humans proved unsuccessful, with brain lesions not resulting in weight loss. This underscores the complexity of the brain’s role in appetite regulation and the significant risks associated with invasive neurological interventions.
The Broader Implications: A Call for Evidence-Based Solutions
The array of extreme and unconventional weight-loss methods examined—from the AspireAssist siphon and duodenal-jejunal bypass liners to intestinal ablation, Botox injections, and invasive brain stimulation—highlights a persistent, and at times desperate, search for rapid solutions to a complex health issue. While some interventions may achieve short-term weight reduction, they often come with substantial risks, ethical concerns, and a questionable long-term sustainability.
The international medical community often observes these "machinations" with a degree of bemusement, as evidenced by commentary titles such as "What Are the Yanks Doing?" in academic journals. This reflects a broader concern about the proliferation of unproven or high-risk procedures in the absence of robust scientific evidence and rigorous regulatory oversight.
The overarching implication is a critical need for a paradigm shift in how weight management is approached. The focus must firmly remain on evidence-based, sustainable strategies that prioritize overall health and well-being over rapid, potentially harmful transformations. As emphasized in authoritative resources like Dr. Greger’s book, "How Not to Diet," healthy and sustainable weight loss is not a matter of complex, invasive surgery or experimental neurological interventions. It is, rather, a journey rooted in informed lifestyle choices, balanced nutrition, and consistent physical activity.
Doctor’s Notes and Further Resources
For individuals considering interventions for weight management, a thorough understanding of available options is paramount. Medical professionals often recommend exploring less invasive and more scientifically validated approaches.
- Gastric Balloon Surgery: The safety and efficacy of gastric balloon surgery, another intervention aimed at reducing stomach capacity, are subjects of ongoing research and clinical evaluation. Information regarding these procedures is crucial for informed decision-making.
- Weight Loss Medications: The landscape of pharmaceutical interventions for weight loss is diverse, with various drugs available. However, their safety and effectiveness can vary significantly, necessitating careful consultation with healthcare providers. Resources detailing the safety and efficacy of weight-loss pills provide essential guidance.
Ultimately, the most effective and enduring path to weight management lies in adopting a holistic approach that emphasizes sustainable dietary habits, regular physical activity, and behavioral modifications. Resources dedicated to sustainable weight loss, such as comprehensive guides and scientific literature, are invaluable tools for individuals seeking to achieve and maintain a healthy weight. The pursuit of a healthier lifestyle should always be guided by evidence, safety, and a commitment to long-term well-being.