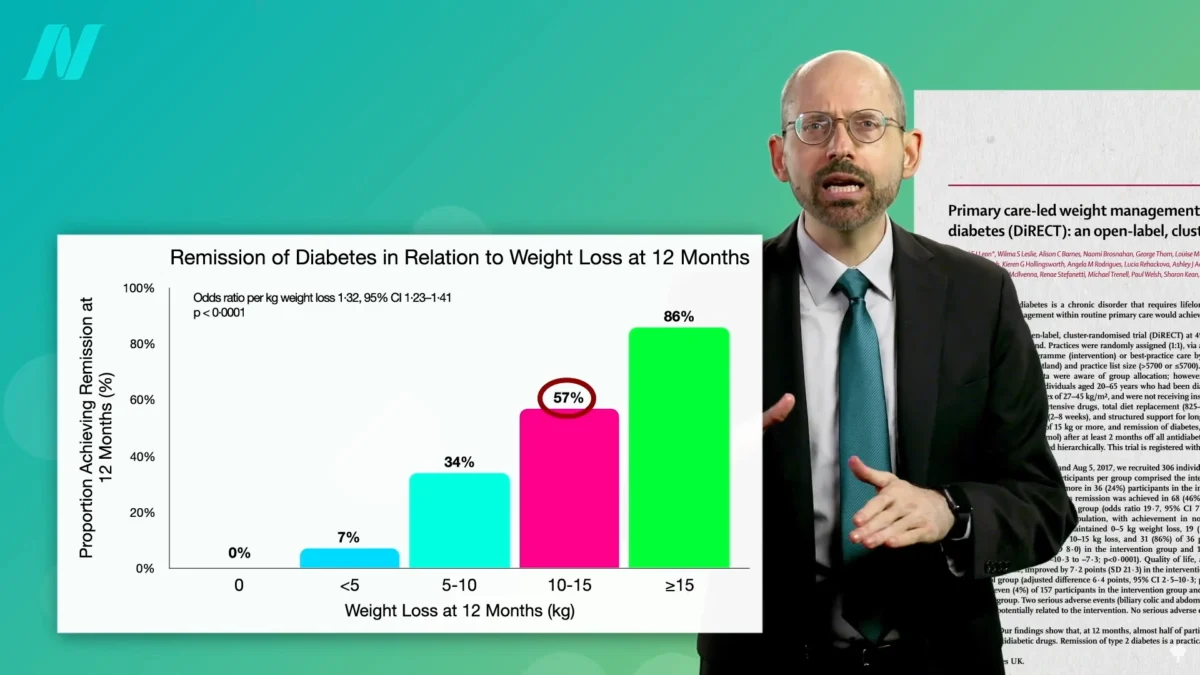
The burgeoning global epidemic of type 2 diabetes, a condition currently affecting over half a billion adults with projections indicating a 50% surge within a generation, is prompting a critical re-evaluation of treatment paradigms. Emerging scientific consensus and historical medical practices suggest a powerful, albeit often overlooked, pathway to remission: significant weight loss. Research indicates that for nearly 90% of individuals diagnosed with type 2 diabetes for less than four years, a reduction of just 15% in body weight can lead to the restoration of non-diabetic blood sugar levels. This figure dramatically contrasts with the outcomes of bariatric surgery, where even more substantial weight loss yields lower remission rates, underscoring the potent efficacy of dietary and lifestyle interventions.
The historical trajectory of diabetes management reveals a persistent, though often extreme, understanding of its link to dietary excess. Ancient Ayurvedic texts, dating back approximately 2,000 years, proposed radical approaches to managing diabetes, including prescriptions for intense physical exertion or severe dietary restriction. One such passage advised a diabetic to "live like a saint," walk immense distances, or subsist on minimal sustenance, reflecting an early recognition that reducing caloric intake could alleviate symptoms. This historical perspective is echoed in the stark realities of past medical practices. In 1797, Dr. John Rollo proposed a diet for diabetes that was not only restrictive but also unpalatable, featuring rancid meat and employing emetics to induce sickness and vomiting. While these methods, by causing severe discomfort and reduced food consumption, offered temporary relief by reducing food intake, they were far from sustainable or healthy.
The siege of Paris during the Franco-Prussian War inadvertently provided further evidence for the impact of caloric restriction on diabetes. Amidst extreme food shortages, individuals with diabetes experienced a reduction in their symptoms, leading to the widespread advice of "mangez le moins possible" – eat as little as possible. This empirical observation was later formalized into the "Allen starvation treatment," developed by Dr. Frederick M. Allen. For a significant period before the advent of insulin, the Allen treatment was considered a major advancement in diabetes management.
The Allen Treatment and the Concept of "Fat Toxicity"
Dr. Allen’s groundbreaking work in the early 20th century was influenced by clinical observations that severe diabetes cases often saw remission following debilitating "wasting conditions" such as tuberculosis or cancer. This led him to investigate the therapeutic potential of inducing a similar state of weight loss. His research demonstrated that even in the most severe forms of type 2 diabetes, urinary sugar could be eliminated within a matter of days through extreme caloric restriction. However, maintaining this remission proved challenging once patients resumed a more regular diet. Dr. Allen’s core principles for managing diabetes involved maintaining a low body weight and severely restricting dietary fat. He observed that the consumption of even small amounts of fat, such as butter or olive oil, could trigger a resurgence of diabetic symptoms.
This observation by Dr. Allen aligns remarkably with contemporary scientific understanding, which increasingly frames type 2 diabetes as a condition of "fat toxicity." Modern research utilizes advanced imaging techniques, such as high-tech MRI scanners, to demonstrate in real-time how the infusion of fat into the bloodstream, or consumption of high-fat diets, rapidly leads to the accumulation of fat within muscle cells. This intracellular fat buildup, occurring within hours or even a single day of high-fat intake, directly impairs the body’s ability to utilize insulin effectively, leading to insulin resistance. Even a single meal rich in fat can elevate insulin resistance within six hours, with acute dietary fat intake accelerating this process.

The implications of this fat accumulation are profound. Insulin resistance in muscle tissue, when coupled with an excessive caloric intake, can trigger a cascade of metabolic dysfunctions. This includes the buildup of fat in the liver, a condition known as hepatic steatosis, which further exacerbates insulin resistance. Subsequently, fat can accumulate in the pancreas, directly impacting the function of insulin-producing beta cells. This progressive fat infiltration is now understood to be a primary driver of the development and progression of type 2 diabetes. Scientific literature posits that type 2 diabetes can be viewed as a state of excessive fat accumulation in the liver and pancreas, and critically, this condition remains reversible for a significant period, estimated to be at least 10 years in the majority of individuals.
The Power of Very Low-Calorie Diets and Weight Loss
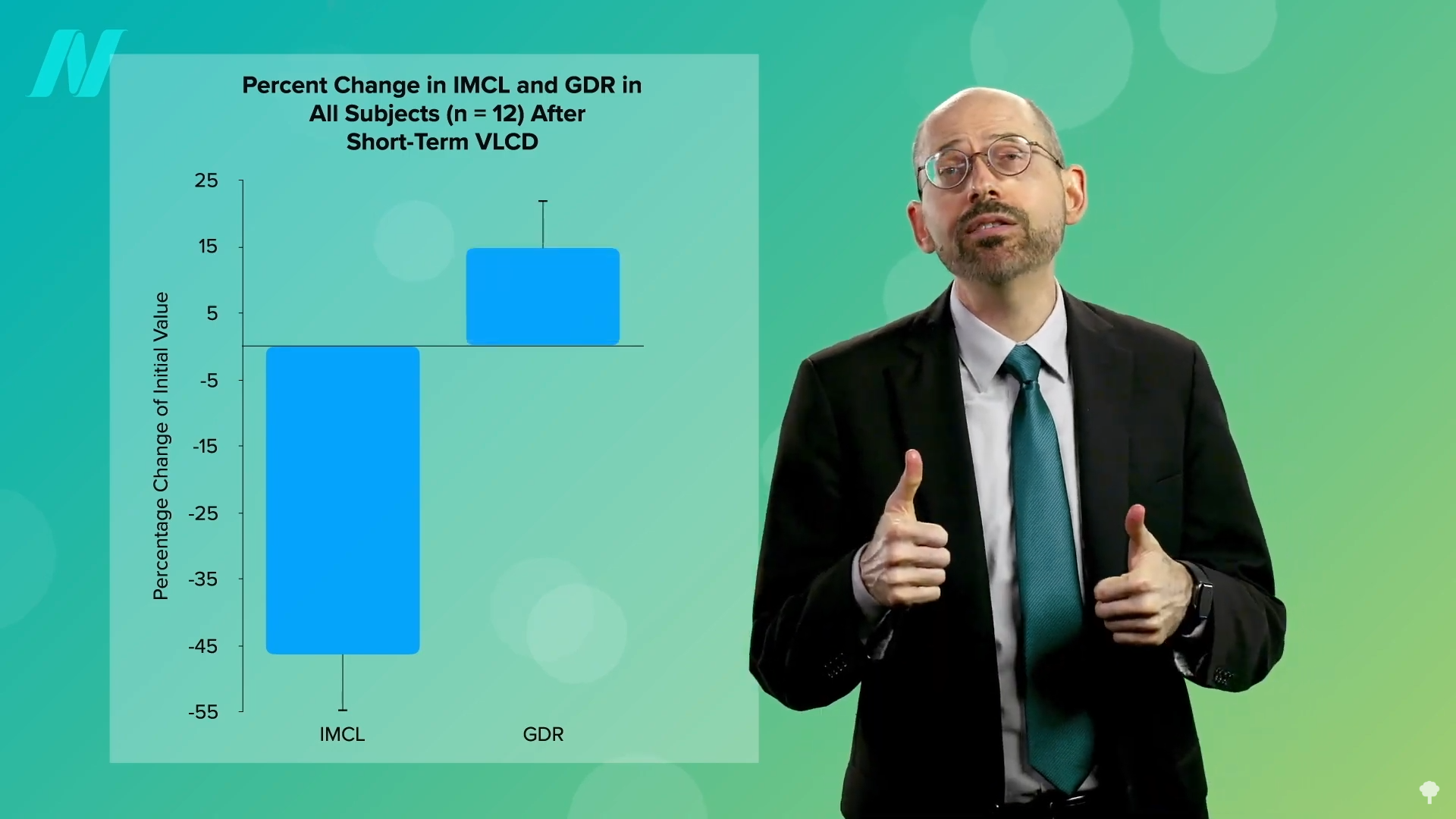
The mechanism by which weight loss achieves remission is rooted in the reduction of this cellular fat accumulation. When individuals embark on a very low-calorie diet, typically around 700 calories per day, the body begins to mobilize stored fat. This process leads to the depletion of excess fat from muscle cells, a phenomenon directly correlated with a significant improvement in insulin sensitivity. As the diet continues, the excess fat within the liver shows a substantial decrease. If the dietary intervention is sustained, the accumulated fat in the pancreas also begins to reduce. This reversal of fat accumulation in key metabolic organs is the cornerstone of achieving remission from type 2 diabetes.
The impact of weight loss on diabetes remission is particularly pronounced in individuals diagnosed more recently. Studies indicate that achieving a 15% body weight loss can lead to non-diabetic blood sugar levels in nearly 90% of individuals who have had type 2 diabetes for less than four years. This contrasts with those who have lived with the disease for longer periods; remission rates drop to approximately 50% for individuals with diabetes exceeding eight years.
Comparing Weight Loss Interventions: Diet vs. Surgery
The effectiveness of weight loss through dietary interventions is further highlighted when compared to surgical approaches. Bariatric surgery, while a powerful tool for significant weight reduction, has demonstrated comparatively lower remission rates. For instance, individuals undergoing bariatric surgery who achieve substantial weight loss have reported remission rates of 62% and 26% in different study groups, depending on the duration of their diabetes. This suggests that non-surgical methods, particularly those focused on dietary modification and sustained lifestyle changes, may offer a more robust and potentially more accessible pathway to diabetes remission for many. The adage that "your forks are better than surgeons’ knives" gains considerable weight in this context.
Further supporting this notion, research published in The Lancet indicates that individuals with type 2 diabetes diagnosed for an average of three years can achieve disease reversal after losing approximately 30 pounds. This translates to a significant portion of the body weight—often around 10-15%—that appears to be a critical threshold for metabolic recovery.
The Role of Fasting and Long-Term Maintenance
While extended periods of physician-supervised, water-only fasting can be a potent method for inducing rapid weight loss and achieving remission, the critical factor for sustained remission is the maintenance of that weight loss. Scientific literature has established with certainty that weight regain invariably leads to the recurrence of diabetes. Therefore, the focus must extend beyond the initial weight loss phase to encompass sustainable lifestyle changes that prevent weight regain.
Historical Context of Insulin and the Enduring Importance of Lifestyle
The discovery of insulin in 1921 was a monumental breakthrough, hailed as "medicine’s greatest miracle." It was literally life-saving for individuals with type 1 diabetes, who would otherwise succumb to the disease. However, for those with type 2 diabetes, while insulin could manage blood sugar levels, it proved insufficient in preventing long-term complications such as blindness, kidney failure, stroke, and amputations. This realization led to a renewed appreciation for the pre-insulin era’s emphasis on lifestyle management.
Elliott Joslin, a highly respected pioneer in diabetes care, advocated strongly for the central role of self-discipline in diet and exercise for managing diabetes, even after the availability of insulin. His perspective underscores that while pharmaceutical interventions play a role, the fundamental drivers of type 2 diabetes—overeating and a sedentary lifestyle—must be addressed through behavioral and dietary changes for lasting remission and prevention of complications.
The Underlying Cause: Fat Toxicity
The core of understanding type 2 diabetes lies in recognizing it as a disease of fat toxicity. Infusing fat into the bloodstream via intravenous means, or adopting a high-fat diet, demonstrably leads to fat accumulation within muscle cells and subsequent insulin resistance. This intracellular fat accumulation disrupts the normal signaling pathways of insulin, leading to a state where the body’s cells do not respond adequately to insulin’s signal to take up glucose from the blood.
Future Implications and Public Health Strategies
The growing body of evidence linking weight loss to type 2 diabetes remission has significant implications for public health strategies. It suggests that widespread public health initiatives focused on promoting healthy eating patterns, encouraging regular physical activity, and supporting individuals in achieving and maintaining a healthy weight could dramatically reduce the burden of type 2 diabetes. The focus on preventable aspects of the disease, as historically recognized, is paramount.
The increasing prevalence of type 2 diabetes necessitates a shift from a purely management-oriented approach to one that emphasizes reversal and prevention. Educational campaigns that highlight the reversibility of type 2 diabetes through lifestyle changes, particularly weight loss, can empower individuals to take control of their health. Furthermore, healthcare systems may need to adapt to support these lifestyle-based interventions more effectively, potentially through integrated care models that include nutritional counseling, exercise programs, and behavioral support.
The historical narrative of diabetes management, from ancient restrictive practices to modern scientific understanding of fat toxicity, converges on a powerful truth: the body’s metabolic health is profoundly influenced by dietary intake and body composition. While the journey to remission may require significant commitment, the scientific and historical evidence strongly supports the notion that type 2 diabetes, when diagnosed early, is a reversible condition, offering a hopeful outlook for millions worldwide. The ongoing research into optimal dietary strategies, including the potential role of various forms of intermittent fasting and plant-based diets, continues to refine the pathways to achieving and sustaining remission, emphasizing that the power to reverse this chronic disease often lies within accessible lifestyle modifications.