The effectiveness and safety of bariatric weight-loss surgery, a set of procedures designed to aid significant weight reduction, are increasingly understood to be profoundly influenced by the technical expertise of the performing surgeon. While these operations, such as sleeve gastrectomy and Roux-en-Y gastric bypass, offer a potent avenue for individuals struggling with severe obesity and related health conditions, a growing body of evidence highlights a critical variable often overlooked by patients: surgeon proficiency. The potential for complications, the need for revisional surgery, and even mortality rates appear to be directly correlated with the experience and skill level of the bariatric surgeon.
The Escalating Need for Bariatric Procedures and Their Associated Risks
Bariatric surgery has emerged as a significant medical intervention in the fight against the global obesity epidemic. For many individuals, these procedures represent a life-changing opportunity to improve health markers, reduce the burden of comorbidities like type 2 diabetes, hypertension, and sleep apnea, and enhance overall quality of life. However, the inherent complexity of these operations means they are not without risk. The data suggests that a substantial portion of patients who undergo bariatric surgery may require further surgical intervention.
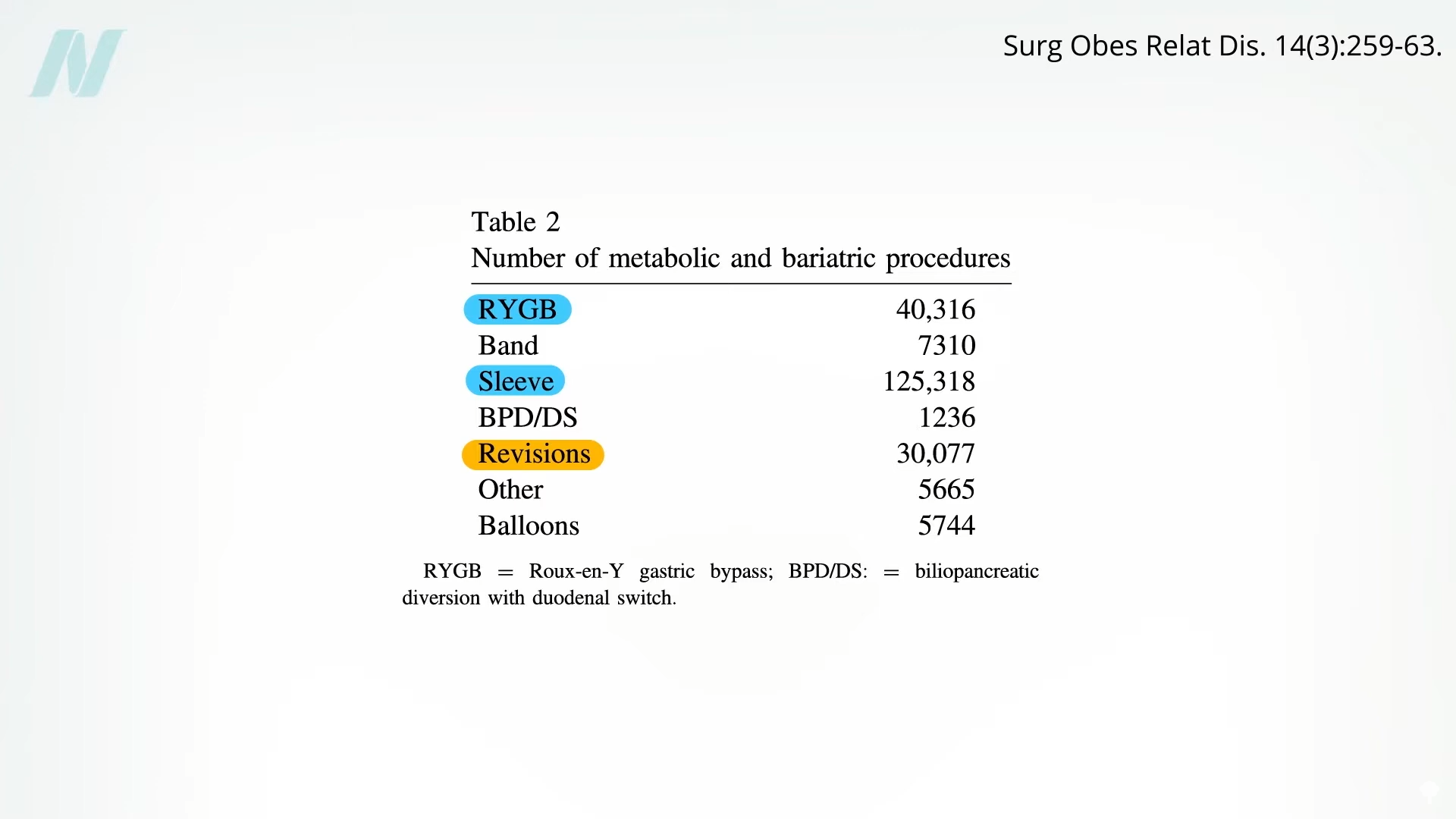
A striking statistic reveals that revision surgery to correct issues arising from an initial bariatric procedure is the third most common type of bariatric operation. This underscores a significant challenge within the field: a notable percentage of patients, estimated to be as high as 25%, find themselves returning to the operating room due to complications stemming from their first surgery. These subsequent reoperations carry an elevated risk profile, with mortality rates reportedly up to ten times higher than primary procedures. Furthermore, there is a stark lack of guarantee for success in these revision surgeries, meaning patients may endure further surgical interventions with no assured positive outcome.
The spectrum of complications associated with bariatric surgery is broad and can manifest in various forms. These include potentially life-threatening events such as leaks at the surgical site, the formation of abnormal connections between organs known as fistulas, the development of ulcers and strictures (narrowing) within the digestive tract, erosions of internal materials, blockages of the gastrointestinal system, and severe acid reflux. Each of these complications necessitates careful management and, in many cases, further surgical intervention, adding to the patient’s physical and emotional burden.
Surgeon Proficiency: A Determinant of Patient Safety and Success
The critical role of surgeon skill in mitigating these risks has become increasingly apparent. A seminal study published in The New England Journal of Medicine offered compelling insights into this phenomenon. In this research, bariatric surgeons voluntarily submitted video recordings of their surgical procedures. These videos were then meticulously reviewed and evaluated by a panel of their peers, assessing technical proficiency. The findings revealed a wide disparity in surgical skill among the participating surgeons.
Crucially, this variation in technical competence was directly linked to patient outcomes. The study established a clear correlation between a surgeon’s skill level and the rates of complications, hospital readmissions, the need for reoperations, and ultimately, patient mortality. Patients who were operated on by surgeons deemed less competent experienced a nearly threefold increase in complications and a fivefold higher rate of death compared to those treated by more skilled practitioners. This research provides robust, data-driven evidence that the surgeon’s hands-on ability is not merely a matter of preference but a significant determinant of patient safety and surgical success.
The Learning Curve: Experience as a Key Indicator
The analogy to highly skilled professionals like musicians or athletes has been drawn to explain the variation in surgical talent. While innate talent may play a role, the data strongly suggests that deliberate practice and extensive experience are paramount in achieving surgical mastery. Bariatric surgery, particularly procedures like gastric bypass, is exceptionally intricate. The learning curve for a surgeon to truly master these techniques is substantial, with estimates suggesting that it may require performing as many as 500 cases before a surgeon reaches a high level of proficiency.

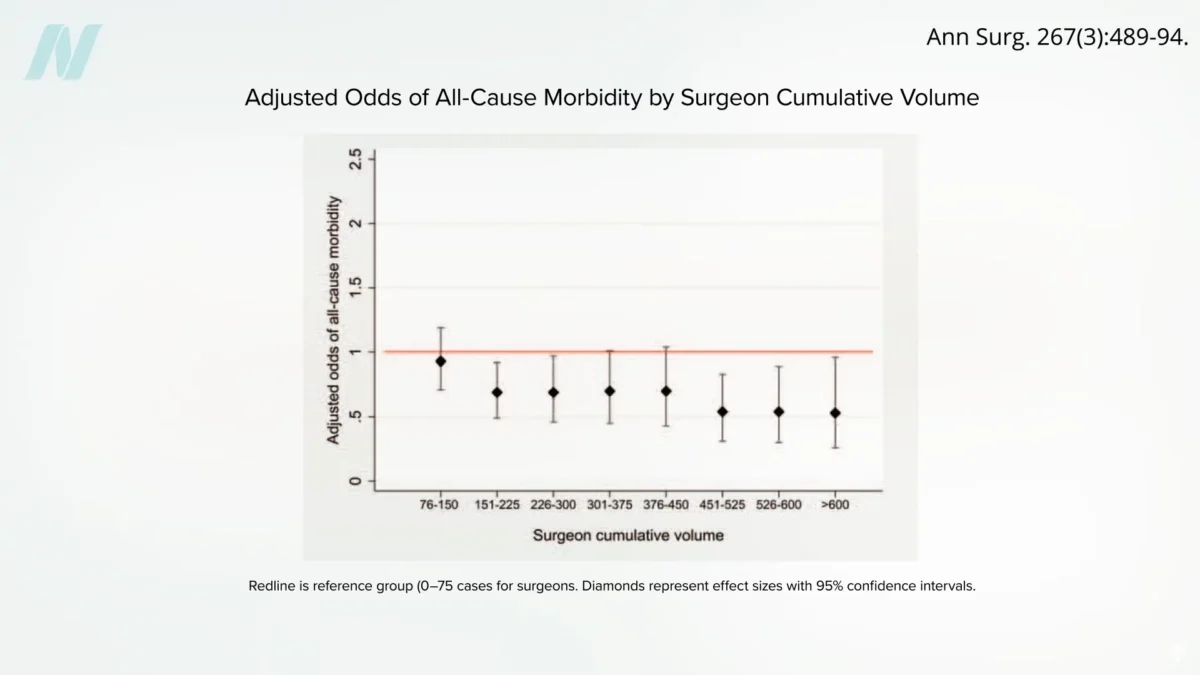
Evidence indicates that the risk of complications appears to plateau after a surgeon has completed approximately 500 procedures. Surgeons who have performed over 600 bypasses consistently demonstrate the lowest rates of complications. The implications for patient safety are profound: the odds of a fatal outcome are reportedly doubled when undergoing surgery with a surgeon who has performed fewer than 75 procedures compared to those who have completed more than 450. This data strongly supports the notion that experience, quantified by the number of procedures performed, is a critical factor in minimizing surgical risk.
Navigating the Landscape: Choosing a Center of Excellence
Given the significant impact of surgeon experience, prospective patients are strongly advised to be proactive in their surgical choices. A key recommendation is to inquire directly with potential surgeons about their procedural volume. Understanding how many bariatric surgeries a surgeon has performed can provide a valuable metric of their experience.
Beyond individual surgeon experience, seeking out accredited bariatric "Centers of Excellence" is another crucial step. These institutions are recognized for meeting rigorous standards of care, including surgeon training, patient selection, and post-operative management. Research indicates that surgical mortality rates at accredited Centers of Excellence are two to three times lower than those observed at non-accredited facilities. This suggests a systemic advantage to seeking care at centers that have demonstrated a commitment to high-quality bariatric surgical practice.
Beyond the Scalpel: Patient Factors and Post-Operative Management
While surgeon skill is a critical determinant of surgical outcomes, it is important to acknowledge that not all complications are solely attributable to surgical error. Patient behavior and adherence to post-operative instructions play a significant role in long-term success and complication avoidance.
A cautionary tale, cited in reports such as "The Dangers of Broccoli," illustrates this point. In one documented case, a woman three months post-gastric bypass surgery consumed large quantities of food at an all-you-can-eat buffet. While she chose healthy options, she reportedly failed to adequately chew her food. This led to the rupture of surgical staples and a medical emergency. Upon surgical exploration, her abdominal cavity contained undigested chunks of broccoli, whole lima beans, and other fibrous vegetables. This anecdote serves as a stark reminder that even with a technically flawless surgery, inadequate post-operative eating habits can lead to severe complications. While the anecdote highlights the importance of chewing, it also implicitly points to the need for a broader understanding of dietary modifications required after bariatric surgery, emphasizing the importance of nutrient-dense foods that are properly prepared and consumed.
The Lifelong Commitment: Nutritional Deficiencies and Their Consequences
Even when bariatric surgery proceeds without immediate complications, the long-term implications for patient health extend far beyond the surgical recovery period. These procedures fundamentally alter the digestive system, necessitating lifelong nutritional replacement and vigilant monitoring. Failure to adhere to this regimen can result in a spectrum of vitamin and mineral deficiencies, with potentially severe and life-threatening consequences.
The consequences of malabsorption are not limited to common issues like anemia, osteoporosis, or hair loss. In severe cases, patients can develop full-blown deficiencies of essential nutrients that can lead to debilitating and fatal conditions. These include beriberi (thiamine deficiency), pellagra (niacin deficiency), kwashiorkor (protein deficiency), and significant nerve damage. For instance, copper deficiency, if left untreated, can manifest as vision loss years or even decades after surgery.

A particularly tragic outcome has been observed with severe thiamine (Vitamin B1) deficiency. In reported cases, nearly one in three patients progressed to permanent brain damage before the condition was identified and treated. This highlights the critical importance of understanding the physiological changes induced by bariatric surgery and the absolute necessity of lifelong supplementation and medical follow-up.
The Mechanism of Weight Loss: Intentional Malabsorption and Behavioral Modification
Procedures like gastric bypass are designed to achieve weight loss through a combination of restricting food intake and intentionally impairing nutrient absorption. By surgically rerouting or removing segments of the intestines, the body’s ability to absorb calories is significantly reduced. However, this mechanism comes at the direct expense of absorbing essential nutrients.
Even restrictive procedures, such as gastric banding or sleeve gastrectomy, which primarily aim to reduce stomach size, can place patients at risk for life-threatening nutrient deficiencies. This is often due to persistent vomiting, a common side effect reported by up to 60% of patients following bariatric surgery. This vomiting is frequently attributed to "inappropriate eating behaviors," which essentially means attempting to eat in a manner that is incompatible with the altered anatomy of the digestive tract. The vomiting, while contributing to weight loss, functions as a potent deterrent to overeating, akin to the mechanism of drugs like Antabuse used in alcohol addiction treatment, which induce severe illness to discourage consumption.
Dumping Syndrome: A Designed Response to Food Intake
Another significant post-operative phenomenon is "dumping syndrome." A substantial percentage of gastric bypass patients experience symptoms such as abdominal pain, diarrhea, nausea, bloating, fatigue, and palpitations shortly after consuming calorie-rich foods. This occurs because the food bypasses the stomach too quickly and empties directly into the small intestine, overwhelming its capacity.
Surgeons often describe dumping syndrome not as an unwanted complication but as an intentional feature of the surgery. It is considered a desired component of the behavioral modification induced by gastric bypass. The unpleasant physiological response serves as a powerful disincentive for patients to consume high-energy, calorie-dense foods, thereby contributing to sustained weight management.
Conclusion and Future Directions
The landscape of bariatric surgery is complex, encompassing not only the surgical act itself but also the patient’s lifelong commitment to dietary management and nutritional supplementation. While the potential benefits for individuals struggling with severe obesity are substantial, the risks associated with these procedures necessitate careful consideration and informed decision-making. The critical role of surgeon skill and experience, coupled with the importance of choosing accredited centers of excellence, cannot be overstated. As research continues to illuminate the multifaceted aspects of bariatric surgery, a comprehensive understanding of these factors is essential for optimizing patient outcomes and ensuring the long-term success of this powerful weight-loss intervention.
This article is the second in a four-part series exploring the intricacies of bariatric surgery. The preceding installment, "The Mortality Rate of Bariatric Weight-Loss Surgery," provided an overview of the risks associated with these procedures. Future articles will delve into "Bariatric Surgery vs. Diet to Reverse Diabetes" and "How Sustainable Is the Weight Loss After Bariatric Surgery?" These discussions aim to equip individuals with a thorough understanding of bariatric surgery as they consider their options for sustainable health improvement. Resources such as the book How Not to Diet offer further in-depth guidance on achieving lasting weight loss through evidence-based strategies.