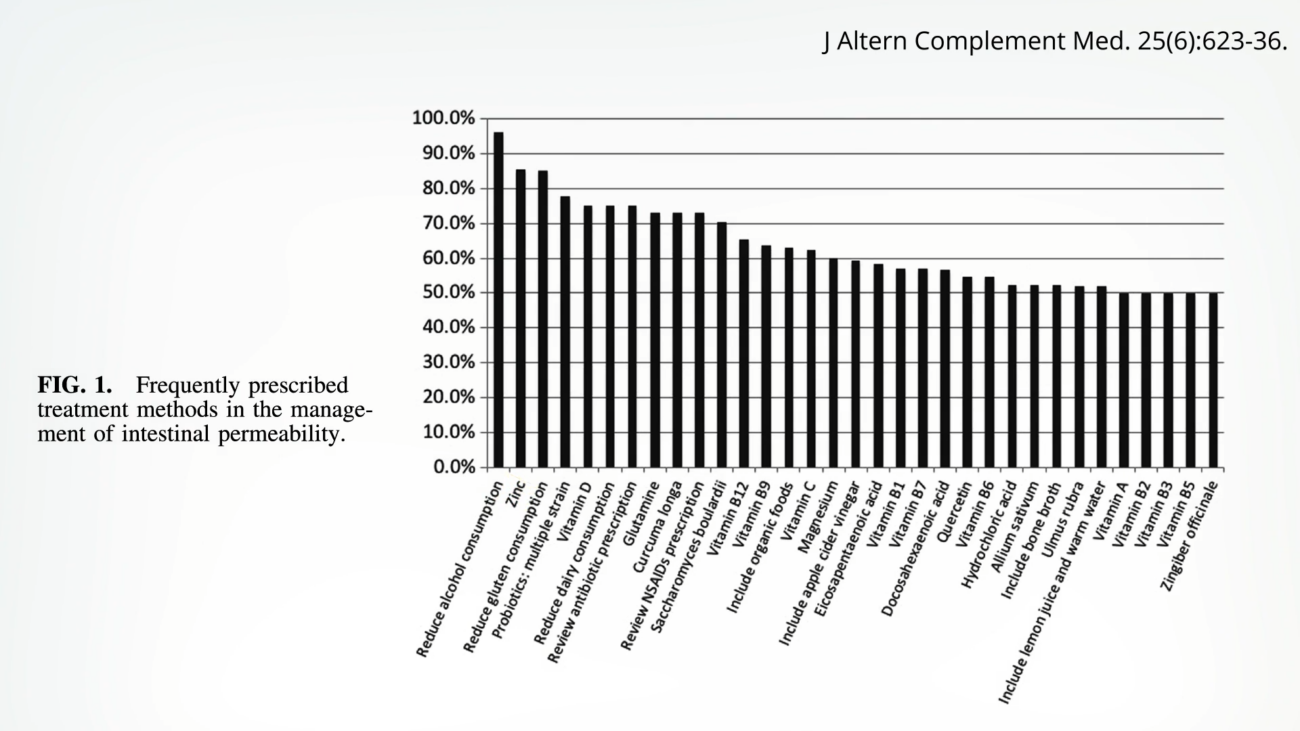
The human intestinal tract stands as our primary, most extensive barrier against the external environment. While our skin acts as a physical shield, the gastrointestinal system is a constant gateway for nourishment, making its integrity paramount. Normally, the entire digestive tract functions as a highly selective filter, meticulously controlling the passage of substances into the body. However, a range of factors, with diet being a chief culprit, can compromise this delicate balance, leading to what is commonly referred to as a "leaky gut." This condition, characterized by increased intestinal permeability, allows undigested food particles, microbes, and toxins to enter the bloodstream, potentially triggering chronic systemic inflammation. Understanding the dietary components that fortify this vital barrier is crucial for maintaining overall health.
The Western Diet and the Rise of Gut Dysbiosis
The prevalent Western or standard American diet, often rich in processed foods, unhealthy fats, and refined sugars, has been increasingly linked to gut dysbiosis. This disruption of the gut microbiome, the complex ecosystem of microorganisms residing in our intestines, can create an environment conducive to inflammation. When the intestinal lining becomes inflamed and permeable, the tight junctions—the specialized protein structures that seal the cells together—loosen. This compromised barrier allows unwanted substances to "leak" into the bloodstream, initiating a cascade of inflammatory responses throughout the body. This chronic inflammation is now recognized as a contributing factor to a wide array of health issues, from autoimmune diseases to metabolic disorders.
The Power of Plants: A Vegetarian Diet’s Impact on Gut Health
Emerging research strongly suggests that a predominantly vegetarian diet, characterized by a high intake of plant-based foods, can significantly bolster intestinal barrier function. The gut bacteria found in individuals who adhere to vegetarian diets are consistently associated with a balanced microbiome, exhibiting greater bacterial biodiversity and enhanced integrity of the intestinal lining. This dietary pattern is linked to a marked reduction in the production of uremic toxins, such as indole and p-cresol, which are byproducts of protein fermentation in the gut.
A cornerstone of this protective effect lies in dietary fiber. Fiber serves as the primary fuel source for beneficial gut bacteria. When these bacteria ferment fiber, they produce short-chain fatty acids (SCFAs), such as butyrate, propionate, and acetate. SCFAs play a critical protective and nourishing role for the cells lining the gut, known as enterocytes. They are essential for maintaining the energy supply to these cells and for preserving the integrity of the intestinal barrier. Studies indicate that increased SCFA production, driven by adequate fiber intake from plant-based foods, helps ensure the preservation and proper functioning of the intestinal lining. Therefore, plant fiber is of paramount importance in maintaining the structural and functional integrity of our gut barrier.
Evidence from Clinical Studies: Quantifying the Impact of Fiber
The impact of dietary fiber on gut health has been a subject of rigorous scientific investigation. One notable study involved individuals diagnosed with non-alcoholic fatty liver disease (NAFLD). For a period of six months, participants were placed on a diet rich in whole grains, beans, lentils, fruits, vegetables, nuts, and seeds. The results demonstrated a significant reduction in zonulin levels among these individuals.

Zonulin is a protein that plays a key role in regulating the tight junctions between intestinal cells. It is widely considered the only measurable biomarker that directly reflects impairment of the intestinal barrier. Elevated zonulin levels are a strong indicator of a "leaky gut." The observed decrease in zonulin in the NAFLD patients following a plant-rich diet suggests that incorporating these whole foods, particularly those high in fiber, contributes to maintaining the proper structure and function of the intestinal barrier.
While this study provided compelling observational data, researchers acknowledged the need for more direct evidence to establish a causal link between fiber intake and improved gut permeability. The absence of a control group in the initial NAFLD study meant that while the trend was positive, it was difficult to definitively attribute the improvement solely to fiber. Scientists emphasized that further randomized, controlled trials, ideally double-blind and crossover studies, would be necessary to isolate the effects of fiber from other beneficial compounds present in whole plant foods.
The Randomized Controlled Trial: Confirming Fiber’s Protective Role
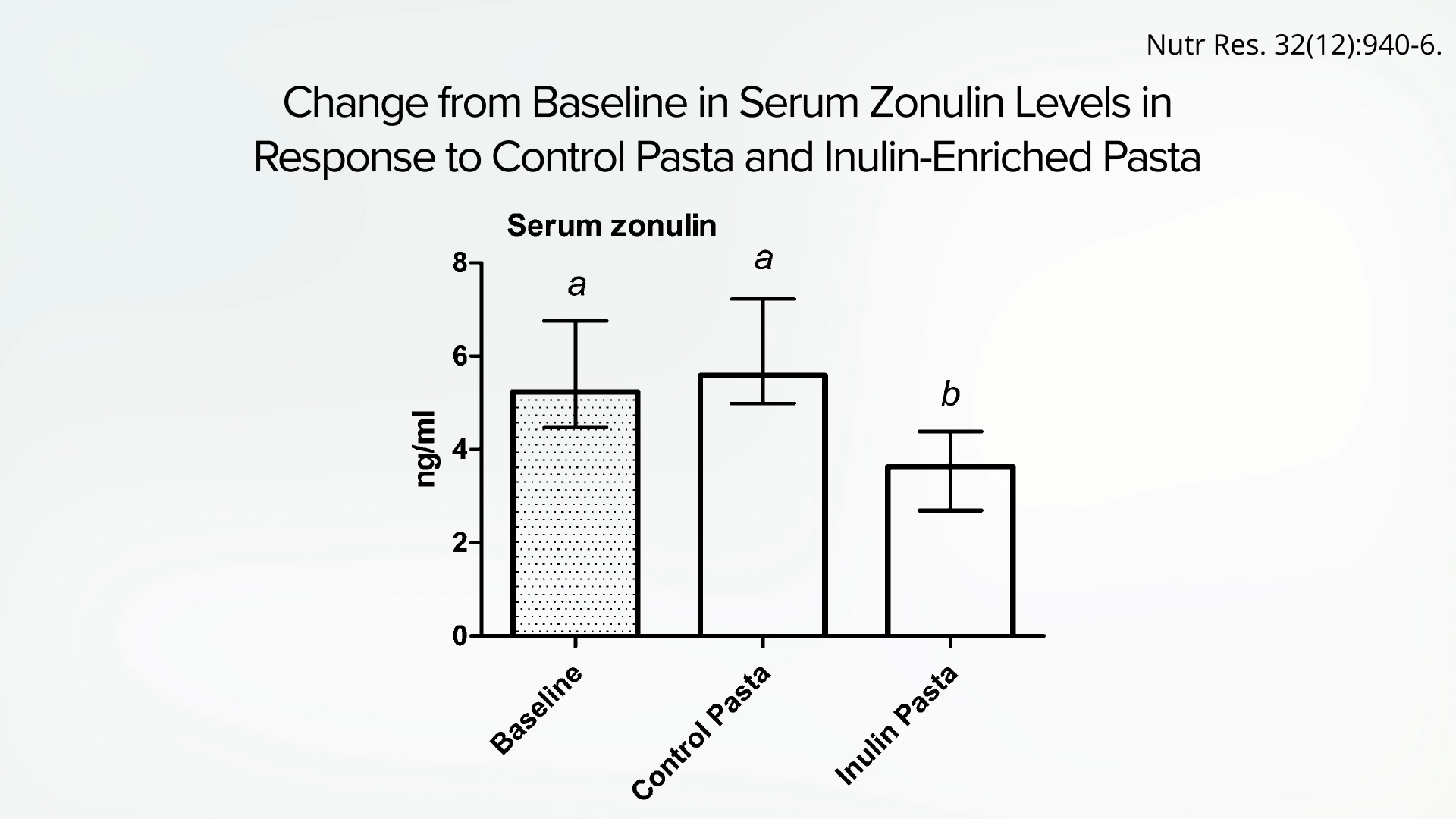
Fortunately, such a study did emerge, providing robust evidence for fiber’s direct impact on gut permeability. In a randomized, double-blind, crossover trial, a group of healthy young men was assigned to consume pasta with or without added fiber. The findings were significant: participants who consumed pasta with added fiber exhibited a notable decrease in zonulin levels compared to their pre-intervention levels and to the control group that did not receive the fiber supplement. This research definitively demonstrated that dietary fiber can indeed improve "gut leakiness," reinforcing the importance of fiber-rich foods in supporting intestinal health.
Beyond Fiber: Specific Plant Compounds with Protective Properties
While fiber is a primary driver of gut barrier health, certain plant-derived compounds also exhibit promising therapeutic potential. Curcumin, the vibrant yellow pigment found in turmeric, has been investigated for its ability to protect the intestinal lining. In animal studies, curcumin has shown efficacy in preventing intestinal damage induced by non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen.
Similarly, sulforaphane, a compound found in cruciferous vegetables such as broccoli, has demonstrated protective effects against intestinal damage in animal models. While direct human studies on broccoli’s impact on gut permeability are still limited, research involving turmeric has yielded encouraging results. A human study involving the consumption of turmeric, equivalent to approximately two to three teaspoons per day for three days, revealed a reduction in markers of gastrointestinal barrier damage and inflammation caused by strenuous exercise, when compared to a placebo group. This suggests that even moderate amounts of turmeric can offer protective benefits, though further research is needed to establish optimal dosages and long-term effects.
The Role of Zinc in Gut Barrier Function
Beyond plant compounds, the mineral zinc has also gained attention for its role in supporting intestinal health. Many alternative medicine practitioners list zinc as a primary intervention for leaky gut, often alongside recommendations to reduce alcohol consumption.
Scientific inquiry has supported this practitioner insight. In animal models, zinc has been shown to protect against drug-induced intestinal damage, akin to its effects observed with curcumin and sulforaphane. More importantly, randomized controlled trials in humans have corroborated these findings. One study administered a potent NSAID, indomethacin, to healthy adults for five days, which predictably resulted in a threefold increase in gut permeability. However, when participants concurrently took zinc supplements, this rise in permeability was significantly blunted, strongly suggesting a protective effect on the small intestine.
While the initial human trial utilized a very high dose of zinc (75 mg per day), which is nearly twice the tolerable upper daily intake, subsequent research has indicated that even much lower doses can be effective. A study found significant improvements in gut leakiness with a supplement of just 3 mg of zinc. This suggests that relatively modest zinc supplementation may be sufficient to exert a protective effect. For context, consuming one cup (approximately 200 grams) of cooked lentils can provide an additional 3 mg of zinc to the daily diet, highlighting how dietary choices can contribute to adequate zinc intake.
Implications for Public Health and Individual Well-being
The growing body of scientific evidence underscores the profound impact of diet on the integrity of our intestinal barrier. The shift from a standard Western diet to one rich in plant-based foods, emphasizing whole grains, legumes, fruits, vegetables, nuts, and seeds, appears to be a cornerstone strategy for preventing and treating leaky gut. The understanding of fiber’s role in SCFA production and the specific protective properties of compounds like curcumin and sulforaphane, along with the essential mineral zinc, provides a comprehensive dietary framework for improving gut health.
The implications of this research extend to public health initiatives aimed at combating chronic inflammatory diseases. By promoting dietary patterns that fortify the gut barrier, healthcare professionals can empower individuals to take proactive steps towards preventing a wide range of conditions linked to intestinal permeability. Further research into the precise mechanisms of action of various dietary components and their synergistic effects will undoubtedly continue to refine our understanding and guide the development of effective, evidence-based dietary interventions for promoting a healthy gut and, by extension, overall well-being.
Doctor’s Note: For further exploration of strategies to prevent gut dysbiosis and leaky gut, readers are encouraged to consult resources such as "Flashback Friday: Gut Dysbiosis: Starving Our Microbial Self" and "Avoid These Foods to Prevent a Leaky Gut," which offer additional insights and actionable advice.