The concept of personalized nutrition (PN) has rapidly gained traction, promising tailored dietary advice and food products designed to meet the unique biological makeup of each individual. Rooted in the intuitive notion that "one size does not fit all," this approach taps into a deep-seated human desire to feel special and uniquely understood. This inherent appeal, amplified by sophisticated marketing strategies, has fueled the growth of personalized food innovations, including advancements in 3D food printing, which are presented as ideal candidates for mass customization.
However, beneath the surface of this enticing promise lies a complex scientific and ethical landscape. While undeniable biological differences exist that necessitate tailored nutritional strategies for specific individuals, a critical examination of the current evidence suggests that for the majority of the population, the benefits of truly personalized nutrition are overstated, potentially overshadowing the profound impact of fundamental lifestyle choices.
The Scientific Basis and Commercialization of Personalized Nutrition
Personalized nutrition is often framed as a branch of the broader movement towards personalized medicine, also known as precision medicine. This paradigm shift is driven by a "massive cultural allure" of personal control over health outcomes, encompassing diagnosis, treatment, and prevention. The commercialization of this concept has been rapid, with a proliferation of direct-to-consumer genetic testing companies offering personalized nutrition advice. These companies often leverage genetic variants to suggest individualized micronutrient optimization, despite evidence indicating that many such variants explain only a small fraction of the variance in nutrient levels between individuals.
The scientific underpinnings of PN are complex. It acknowledges that variations in genetics, the microbiome, lifestyle, and environmental exposures can influence how individuals respond to different nutrients. For instance, certain genetic predispositions, such as a peanut allergy or celiac disease, clearly necessitate specific dietary restrictions. Similarly, lactose intolerance, common in populations of Asian descent, requires avoidance of dairy products.
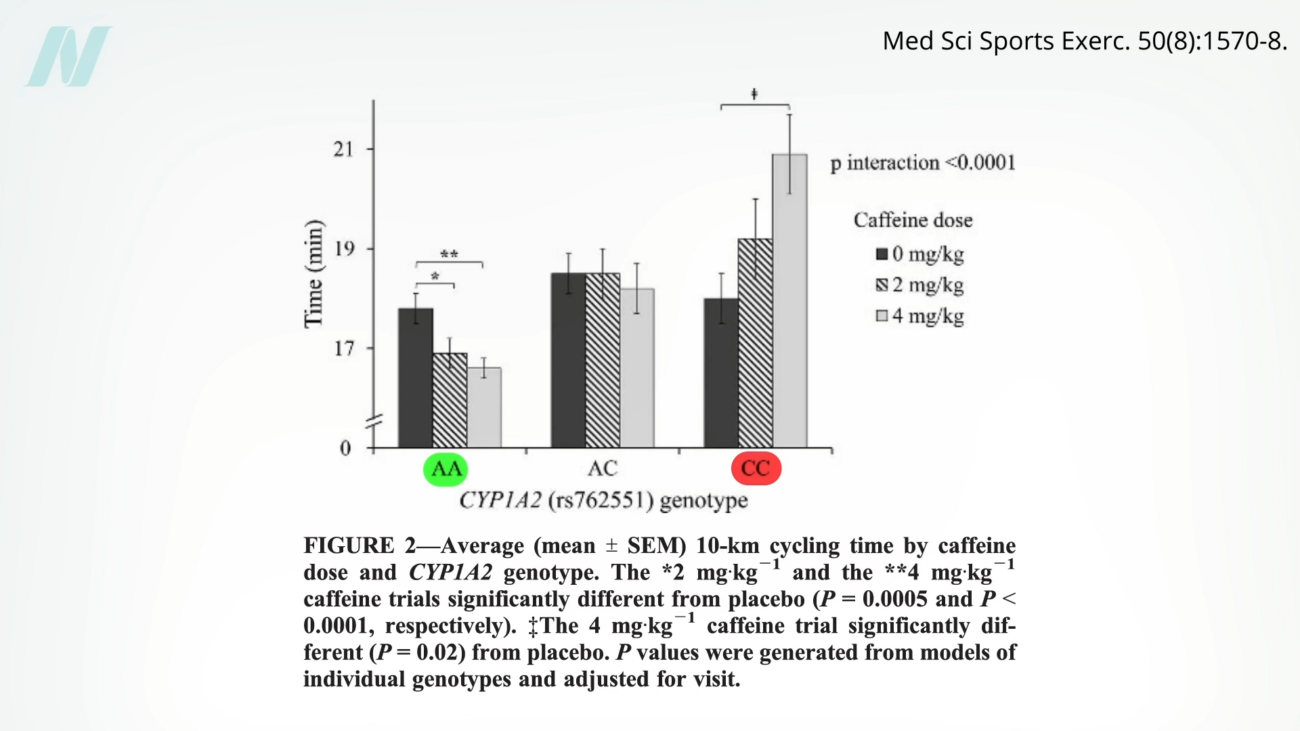
A compelling example of genetic influence on nutrient metabolism comes from research on caffeine. Studies have identified variations in the CYP1A2 gene, which encodes the enzyme responsible for metabolizing caffeine. "Fast metabolizers" of caffeine can experience ergogenic (performance-enhancing) benefits, with studies showing significant improvements in athletic performance, such as shaving over a minute off a 10-kilometer cycling time. Conversely, "slow metabolizers" may experience no benefit or even a performance decrement, with caffeine adding two minutes to their cycling time. This highlights how genetic makeup can dictate the efficacy of a common dietary component.
The Reality: More Similarities Than Differences
Despite these demonstrable individual differences, a significant body of research suggests that for the vast majority of people, in most common health contexts, we are more alike than we are different. The human genome, while intricate, shares a high degree of similarity across individuals. Many common diseases and health conditions are not caused by single gene mutations, as seen in rare monogenic disorders like hemophilia or sickle cell anemia. Instead, they arise from a complex interplay of multiple genes, environmental factors, and, crucially, lifestyle choices.
The challenge in realizing truly personalized medicine, including nutrition, lies in this polygenic and multifactorial nature of disease. For example, adult stature, a highly heritable trait, is influenced by at least 40 identified chromosomal locations. While parental genes account for approximately 80% of the difference in height between individuals, the dozens of identified genes collectively explain only about 5% of this variation. This illustrates that even for traits with strong genetic components, our understanding of the precise genetic architecture and its predictive power at an individual level remains limited.
Genome-wide association studies (GWAS), a common tool used to identify genetic links to diseases, scan entire chromosomes for statistical associations between diseases and DNA segments. While these studies are invaluable for understanding broad genetic predispositions, companies marketing genetic susceptibility tests often reinterpret these findings to imply direct individual risk prediction. However, the reality is that these identified genetic associations typically represent modest increases in risk, with far less predictive power than well-established lifestyle factors.

The Overstated Promise and the Neglected Fundamentals
The current practice of using an individual’s DNA to predict disease risk has been critically assessed as providing "little to no useful information" for actionable health decisions in many cases. The enthusiasm for personalized genetic advice, particularly from direct-to-consumer testing companies, often outpaces the scientific evidence. These companies may promote supplement use based on genetic variants that explain only minor variations in nutrient levels, creating a market for unproven interventions.
Consider a hypothetical scenario where an individual’s genetic analysis suggests a slightly elevated risk for a particular chronic condition compared to their ancestral group. The advice typically provided in such instances is invariably sound: exercise regularly, maintain a healthy weight, moderate alcohol consumption, and consume a diet rich in fruits, vegetables, and whole grains. This advice, while beneficial, is not novel. It represents the bedrock of public health recommendations that have been established through decades of research on lifestyle interventions.
The critical disconnect lies in the widespread failure to implement these fundamental, universally beneficial strategies. Nationwide surveys consistently reveal that a staggering majority of the population in developed countries, including the United States, does not adhere to even the most basic dietary guidelines. Reports indicate that nearly every individual in the United States consumes a diet that falls short of recommended standards, with findings suggesting that "almost no one in the United States is eating a healthy diet."
The Implications: A Misplaced Focus?
This widespread non-adherence to foundational health practices raises a crucial question: when the majority of the population struggles to adopt universally recognized healthy lifestyle behaviors, does focusing on highly personalized, often complex, and sometimes unsubstantiated nutritional strategies constitute a misplaced emphasis?
The allure of personalization, driven by commercial interests and a desire for individual solutions, may inadvertently distract from the urgent need to address population-level health behaviors. The "massive cultural allure" of personal control, while understandable, can become an illusion if it leads individuals to overlook the proven efficacy of fundamental health principles.
The implications are significant. By emphasizing the intricacies of individual genetic makeup and the potential for hyper-specific nutritional interventions, the discourse around health can shift away from accessible, evidence-based lifestyle changes. This can create a perception that complex genetic testing and tailored products are necessary for good health, potentially making healthy living seem unattainable or exclusive for those who cannot afford or access such services.
The Path Forward: Re-emphasizing Personal Responsibility
The future of health and nutrition likely lies in a balanced approach. While acknowledging and investigating genuine biological individualities—such as allergies, intolerances, and specific metabolic differences—the focus for the broader population should undoubtedly pivot back to personal responsibility for health. This means:
- Prioritizing Foundational Health Behaviors: Emphasizing the critical importance of a balanced diet rich in whole foods, regular physical activity, adequate sleep, stress management, and avoiding tobacco and excessive alcohol consumption. These are the cornerstones of disease prevention and well-being, supported by an overwhelming body of scientific evidence.
- Promoting Health Literacy: Educating the public about evidence-based nutrition and lifestyle choices, demystifying complex health information, and fostering critical thinking regarding health claims, especially those from commercial entities.
- Supporting Accessible Interventions: Focusing public health efforts and resources on creating environments and policies that make healthy choices easier and more accessible for everyone, regardless of their genetic profile or socioeconomic status.
- Responsible Innovation: Encouraging the development of personalized nutrition technologies and services that are rigorously validated by scientific evidence, ethically marketed, and truly address unmet needs beyond what is achievable through fundamental lifestyle changes.
The narrative around personalized nutrition needs to be recalibrated. While the science behind individual biological responses is fascinating and holds potential for specific therapeutic applications, it should not overshadow the profound and universally applicable power of personal responsibility for health. The most personalized and impactful approach to health for the vast majority of people remains the consistent and dedicated application of well-established, fundamental lifestyle principles. The challenge is not in finding a unique genetic code for optimal health, but in empowering individuals to live healthier lives through informed, consistent choices.
The accompanying video, "Friday Favorites: Do the Health Benefits of Coffee Apply to Everyone?", further elaborates on the nuanced differences in how individuals metabolize common dietary components like caffeine, underscoring the scientific basis for some personalization while reinforcing the need for a broader understanding of health.