The quest for a slimmer physique has led individuals and medical professionals down a rabbit hole of increasingly inventive, and often alarming, weight-loss strategies. From the superficially restrictive to the surgically invasive and downright bizarre, the spectrum of interventions aimed at shedding pounds is vast and, at times, deeply concerning. This article delves into the safety and efficacy of several such methods, highlighting the scientific evidence, potential risks, and the underlying motivations driving these extreme approaches.
The Calorie Conundrum: Exercise vs. Indulgence
At the heart of weight management lies the fundamental principle of energy balance: calories consumed versus calories expended. While seemingly straightforward, the practical application can be disheartening. For an individual of moderate obesity engaging in moderately intense physical activity, such as brisk walking or cycling, approximately 350 calories might be burned in an hour. However, the ease with which high-calorie, processed foods and beverages are consumed presents a stark contrast. A mere minute of consuming snacks or sugary drinks can easily account for 70 calories (293 kJ). This means that a full hour of dedicated exercise can be entirely negated by just five minutes of casual indulgence. This stark disparity underscores the immense challenge many face in achieving weight loss through diet and exercise alone, creating fertile ground for more drastic interventions.
The AspireAssist Siphon: A Direct Approach to Calorie Removal
Emerging as a technologically driven, albeit invasive, solution to this calorie imbalance is the AspireAssist siphon assembly. This device represents a significant departure from traditional weight-loss methods. It involves a percutaneous gastrostomy, a surgical procedure where a stoma, or opening, is created in the abdominal wall, leading directly into the stomach.
Procedure and Mechanism
The surgical implantation of the AspireAssist device is a multi-step process. Initially, a small incision is made in the abdomen. A gastrostomy tube is then inserted into the stomach, and a portion of it is tunneled through the abdominal wall to create an external opening, often referred to as a stoma. This creates a direct conduit from the stomach to the exterior of the body.
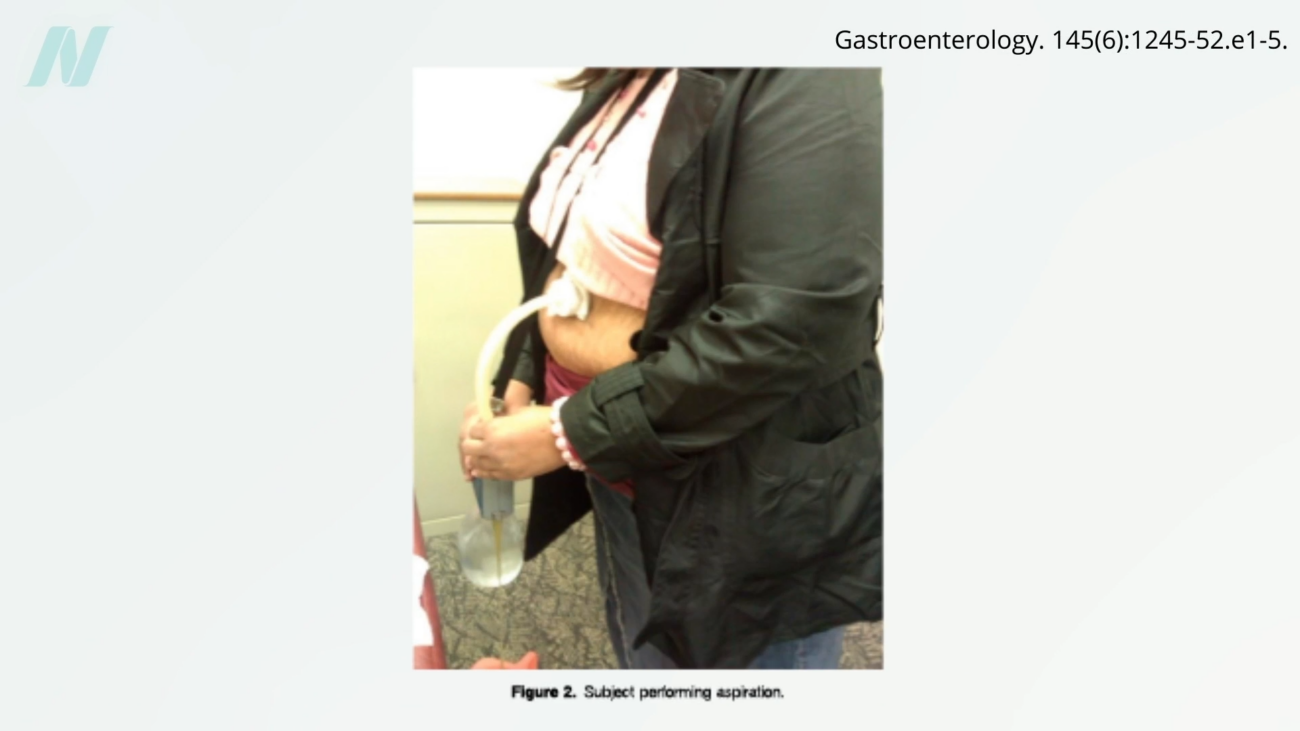
Following this procedure, individuals can attach a specialized suction device to the stoma after consuming a meal. This device allows for the direct aspiration, or siphoning, of a significant portion of the stomach’s contents – typically 25-30% of the food consumed – typically within 5 to 10 minutes of eating. This effectively bypasses the normal digestive process for a portion of the ingested calories.
Efficacy and Patient Experience
Studies have indicated that patients utilizing the AspireAssist system do experience weight loss. The precise mechanisms contributing to this efficacy are multifaceted. Beyond the direct removal of calories, the presence of the fistula, or the surgically created passage, may influence the stomach’s ability to relax and accommodate food, potentially leading to earlier feelings of fullness. Furthermore, the regimen often requires patients to drink substantial amounts of water and chew their food thoroughly, both of which are known to aid in weight management by promoting hydration and slowing the eating rate.
Anecdotal evidence suggests that the visual reality of aspirating gastric contents can also serve as a powerful deterrent. Patients report a shift towards healthier food choices to avoid the unappealing appearance of undigested, unhealthy foods being removed, particularly fried items which are described as visually unpleasant when extracted.
Risks and Considerations
Despite its efficacy in weight reduction, the AspireAssist system is not without its risks. A primary concern is the potential for nutrient deficiencies. The aspiration process removes not only calories but also essential nutrients, including potassium, which is leached from the stomach juices. Consequently, patients are required to supplement their diet with potassium to prevent deficiency, a complication that can mirror those seen in individuals with bulimia.
While serious adverse events such as abdominal abscesses are reported to be rare, minor wound complications related to the stoma are more common. The device’s primary selling point, that it does not alter the gastrointestinal tract’s anatomy, is presented as a benefit, especially within the context of a rapidly evolving and sometimes unregulated landscape of bariatric procedures.
The Duodenal-Jejunal Bypass Liner: A Less Invasive Surgical Alternative
The duodenal-jejunal bypass liner, exemplified by devices like the EndoBarrier, represents another approach that seeks to mimic the effects of more invasive bariatric surgery without extensive anatomical alteration. Traditional gastric bypass surgery involves surgically removing or rerouting a portion of the small intestine to reduce calorie absorption.
Mechanism of Action
Instead of major surgery, the duodenal-jejunal bypass liner utilizes a flexible, tube-like device, typically a few feet in length, made of plastic. This liner is endoscopically inserted into the small intestine and is designed to line the walls of the duodenum and jejunum. The intention is to create a barrier that prevents the direct contact of food with the intestinal lining, thereby reducing the absorption of calories and nutrients.
Adverse Events and Complications
The primary challenge with this method lies in its anchoring within the digestive tract. The EndoBarrier, for instance, is secured using a system of barbed hooks, reportedly 10 in number. These hooks are designed to grip the intestinal wall but are also responsible for a significant number of adverse events. In a study involving 1,056 patients, 891 adverse effects were reported, with nearly 90% of participants experiencing some form of complication. These can range from minor irritations to severe and life-threatening conditions, including penetrating trauma leading to esophageal perforation or liver abscesses, which occurred in approximately 1 in 27 patients.
Intestinal "Resurfacing": A Controversial Endoscopic Intervention
Further pushing the boundaries of invasive weight-loss procedures is the concept of intestinal "resurfacing." While the AspireAssist focuses on removing food, and bypass liners aim to impede absorption, resurfacing techniques target the very lining of the intestines.
Thermal Ablation of Duodenal Mucosa
One such method involves the "thermal ablation of the superficial duodenal mucosa." In layman’s terms, this procedure entails intentionally burning off, or "resurfacing," the inner lining of the duodenum. The rationale behind this is to alter the intestinal lining in a way that may reduce nutrient absorption, similar in principle to how surgical bypasses function, but through a less invasive endoscopic approach.
The "palatability" of the AspireAssist pump has been a subject of discussion, but the concept of intentionally damaging the intestinal lining raises significant ethical and safety concerns. The long-term consequences of such procedures on the digestive system’s integrity and function remain a critical area of investigation, with the potential for severe complications stemming from the intentional tissue destruction.

Botulinum Toxin (Botox) Injections: A Failed Pharmaceutical Approach
In a departure from surgical and endoscopic interventions, researchers have explored pharmaceutical agents for weight management. One such avenue involved the injection of Botulinum toxin (Botox) into the stomach walls of obese individuals. The hypothesis was that Botox, known for its muscle-paralyzing properties, could partially immobilize the gastric muscles. This, in turn, was expected to slow down stomach emptying, leading to prolonged feelings of fullness and, consequently, reduced food intake and weight loss.
However, clinical trials have demonstrated that this approach is largely ineffective. Studies have failed to show a significant impact on weight loss, indicating that the intended mechanism of action does not translate into tangible results for obese patients. This highlights the complexity of gastric physiology and the limitations of applying localized pharmaceutical interventions to a systemic issue like obesity.
Corsets and Tapeworms: Historical Oddities and Persistent Myths
The history of weight-loss endeavors is replete with methods that, in retrospect, appear more like historical curiosities than viable medical treatments.
The Corset Experiment
In the early 2000s, researchers in Sweden conducted a study to assess the efficacy of wearing corsets for weight management. Participants were instructed to wear corsets for extended periods – 12 to 16 hours a day, seven days a week, for nine months. The underlying assumption was that the physical restriction imposed by the corset would limit food intake and promote a slimmer silhouette.
The study, however, yielded predictable results: it failed. The participants found the corsets to be "uncomfortable" and largely did not adhere to the prescribed wearing schedule. This underscores the fundamental flaw in relying on external physical constraint for sustainable weight loss, which requires internal behavioral change and physiological adaptation.
The Tapeworm Diet: A Dangerous Delusion
The notion of "sanitized tapeworms" as a weight-loss remedy has circulated since the early 20th century. The purported mechanism was that the tapeworm, residing in the digestive tract, would consume a portion of the ingested food, thereby reducing the host’s caloric intake.
The practice, which involved ingesting tapeworm eggs, carries severe health risks. Living tapeworms have been discovered during bariatric surgery procedures, suggesting that deliberate infestation with these parasites is not only ineffective but also poses a significant health hazard. Infections can lead to malnutrition, abdominal pain, intestinal obstruction, and neurological complications. This method represents a dangerous and unscientific approach to weight management, preying on desperation and misinformation.
Harnessing Disgust: A Psychological Approach to Calorie Control
In contrast to physically invasive or parasitic methods, recent research has explored psychological interventions. One intriguing study, titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming," investigated the use of subliminal messaging to alter food preferences.
Subliminal Priming and Food Aversion
The experimental design involved exposing participants to rapidly flashed images, too brief for conscious perception. Before presenting images of healthy foods, participants were shown positive stimuli, such as kittens, to create a favorable association. Conversely, before displaying images of high-calorie foods like ice cream, negative imagery was presented. These negative stimuli included unsettling visuals such as a cockroach on a pizza, vomit in a bathroom, and a burn wound.
The findings suggested that this subliminal priming could be effective. Participants reported a reduced desire for high-calorie foods after the experiment, although direct measurement of consumption was not conducted. The researchers concluded that this technique of inducing subliminal revulsion could potentially serve as a tactic to counteract the pervasive environmental cues that promote unhealthy eating habits. This approach, while non-invasive, raises questions about long-term effectiveness and potential unintended psychological consequences.
International Perspectives on American Weight-Loss Innovations
The proliferation of extreme weight-loss methods in the United States has not gone unnoticed by the international medical community. Commentaries and research papers from abroad have expressed bemusement and concern regarding these "American machinations." Titles such as "Don’t Let Them Eat Cake! A View from Across the Pond" and "What Are the Yanks Doing?" reflect a sense of bewilderment at the lengths to which some are going to achieve weight loss.
Exploring Electrical Stimulation
Beyond the more widely publicized methods, research has also delved into the application of electrical stimulation for weight management. Studies have examined the implantation of electrodes into the muscular layer of the stomach wall, a technique aimed at influencing gastric motility and satiety. When this proved ineffective, the focus shifted to colon electrical stimulation.
More controversially, scientists have investigated the use of repetitive electric brain stimulation. The premise was that by placing electrodes within the brain, it might be possible to reduce food intake. This involved drilling holes into the skulls of obese individuals and inserting wires to stimulate specific brain regions associated with hunger. While some success was observed in animal models, attempts to induce weight loss in humans through this method, which involved creating electro-coagulatory lesions in the brain, ultimately proved unsuccessful. The researchers found that while electrical stimulation could elicit hunger responses, burning holes in people’s brains did not lead to significant weight reduction.
The Unanswered Question: What Constitutes Sustainable Weight Loss?
The sheer variety and often extreme nature of these weight-loss methods underscore a critical challenge in the field: the distinction between temporary weight reduction and sustainable, healthy weight management. While many of these interventions may lead to a decrease on the scale, they often come with significant health risks, ethical concerns, and a failure to address the underlying behavioral and lifestyle factors contributing to obesity.
As Dr. Greger emphasizes in his book, How Not to Diet, true sustainable weight loss is not a matter of complex surgical procedures or experimental neurological interventions. It is rooted in evidence-based dietary principles and consistent lifestyle modifications. The pursuit of rapid weight loss through extreme and unproven methods often diverts attention from the proven strategies that promote long-term health and well-being.
Further Exploration
For those seeking to understand the safety and efficacy of other weight-loss interventions, resources such as discussions on gastric balloon surgery, the risks and benefits of weight-loss pills, and comprehensive guides to sustainable weight loss are available. The ongoing dialogue and research within the medical community continue to shed light on the most effective and responsible approaches to tackling the complex issue of obesity.