The surgical community has increasingly advocated for bariatric surgery, often rebranding it as "metabolic surgery" to emphasize its physiological benefits beyond mere weight reduction. Proponents highlight remarkable remission rates for type 2 diabetes following these procedures, suggesting that the anatomical alterations induce significant hormonal changes that positively impact metabolic health. This perspective challenges earlier characterizations of bariatric surgery as simply a drastic measure for behavioral modification. However, emerging research and comparative studies are prompting a deeper examination of whether these outcomes are solely attributable to the surgical intervention itself or if significant portions can be attributed to the rigorous dietary regimens that accompany and follow such procedures.
The Promise of Metabolic Surgery and Early Observations
Bariatric surgery, which involves significant rearrangements of the gastrointestinal anatomy, has been associated with substantial improvements in type 2 diabetes. Studies have indicated that approximately 50% of obese individuals with diabetes, and as many as 75% of those classified as "super-obese," can achieve remission. This remission is defined by the normalization of blood sugar levels, allowing patients to discontinue diabetes medication and adhere to a regular diet. Crucially, these improvements can manifest rapidly, sometimes within days of the surgery. Long-term follow-up data has also shown sustained benefits, with around 30% of patients remaining diabetes-free 15 years post-surgery, a figure that significantly outpaces the approximately 7% remission rate observed in non-surgical control groups over comparable periods.
These impressive statistics have fueled the perception that bariatric surgery offers a unique, surgically-induced metabolic advantage. The rationale often presented is that the altered digestive tract influences gut hormones, leading to enhanced insulin sensitivity and glucose regulation. However, the intensive pre- and post-operative dietary protocols are also a critical component of patient management, and their role in achieving these metabolic improvements has become a focal point of scientific inquiry.
The Pre-Surgical Hurdle: Liver Fat and the Importance of Weight Loss
A significant challenge in performing bariatric surgery, particularly for individuals with obesity, is the presence of a large, fatty liver. This condition not only complicates the surgical procedure itself, increasing the risk of liver injury and bleeding, but it can also necessitate a transition from less invasive laparoscopic techniques to more extensive open surgery. Such transitions are associated with larger scars, increased risk of wound infections, and prolonged recovery times.
The management of fatty liver is a key consideration for bariatric surgeons. It is well-established that even a modest weight loss of 5% of total body weight can lead to a notable reduction in liver fat, often by as much as 10%. This principle underpins the pre-operative dietary recommendations given to patients awaiting bariatric surgery. These diets are designed to reduce liver size and improve overall metabolic status, thereby optimizing the patient for the surgical procedure and potentially mitigating surgical risks. Following surgery, patients are typically placed on extremely low-calorie liquid diets for an extended period, a measure intended to promote rapid weight loss and further support metabolic recovery.

This rigorous dietary intervention raises a fundamental question: To what extent are the observed improvements in diabetes remission due to the surgical alteration of anatomy, and to what extent are they a direct consequence of severe caloric restriction? Researchers have sought to disentangle these factors through controlled studies.
Disentangling Surgical Effects from Caloric Restriction: A Comparative Study
To investigate the independent contributions of surgical intervention and caloric restriction to diabetes remission, researchers at a bariatric surgery clinic at the University of Texas embarked on a distinctive study. Patients scheduled for gastric bypass surgery who also had type 2 diabetes volunteered to participate. The study involved two phases, meticulously matched for each individual.
In the first phase, participants were admitted to the hospital for 10 days and adhered to an extremely low-calorie diet (less than 500 calories per day). This diet was identical to the one they would typically follow pre- and post-surgery, but importantly, they did not undergo the surgical procedure itself. Following this initial phase, participants would return to their regular lives.
Months later, after regaining some of the weight lost during the initial dietary period, the same patients underwent the planned gastric bypass surgery. Subsequently, they repeated the exact same 10-day extremely low-calorie diet regimen, matched day-for-day with their initial experience. This innovative design allowed researchers to directly compare the effects of severe caloric restriction both with and without the concurrent anatomical changes of gastric bypass surgery, using the same individuals as their own controls. The hypothesis was that if the anatomical rearrangement provided unique metabolic benefits, these patients would demonstrate superior outcomes after surgery compared to their pre-surgical dietary phase.
Findings: Caloric Restriction’s Potent Impact
The results of this carefully designed study offered a compelling challenge to the prevailing narrative that bariatric surgery alone is the primary driver of diabetes remission. The findings revealed that the caloric restriction phase, independent of surgery, yielded significant improvements in blood sugar levels, pancreatic function, and insulin sensitivity. These improvements were comparable to, and in some critical aspects, even superior to those observed following the surgical intervention.
Remarkably, several key measures of diabetic control demonstrated more substantial improvement in the group that underwent caloric restriction without surgery. This suggested that, in some metabolic parameters, the surgery might even impose a slight disadvantage compared to diet alone. This outcome directly questioned the extent to which the anatomical changes inherent to bariatric surgery were essential for achieving these metabolic benefits, particularly in the context of type 2 diabetes.
Understanding the Mechanism: Fat Mobilization and "Personal Fat Threshold"
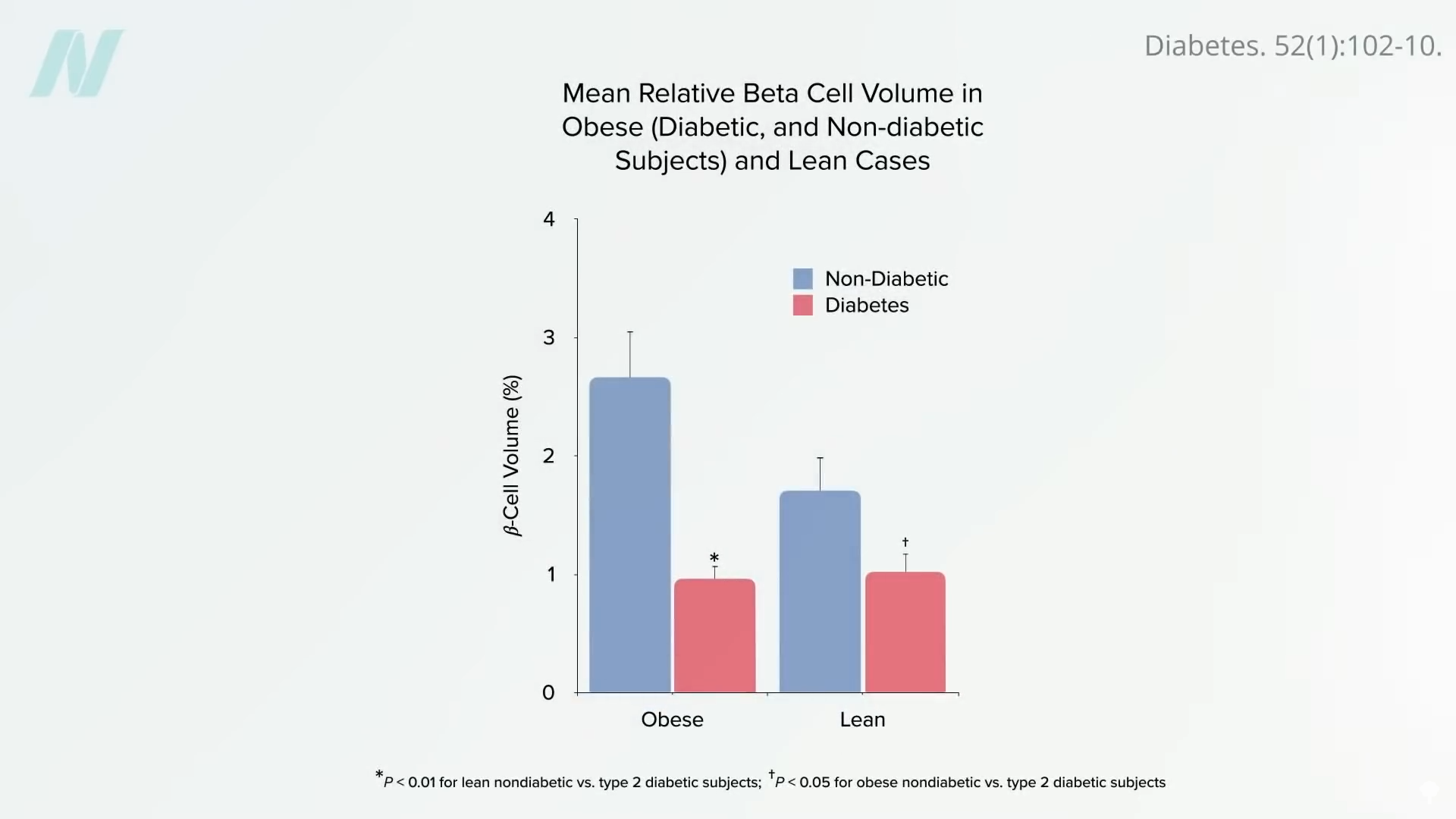
The study’s findings align with a growing understanding of the pathophysiology of type 2 diabetes, which is increasingly linked to the accumulation of excess fat, particularly in the liver. Type 2 diabetes is often conceptualized as a condition where the body’s capacity to safely store fat is overwhelmed. When individuals exceed their "personal fat threshold," excess fat begins to deposit in organs like the liver. This ectopic fat accumulation in the liver can impair its ability to respond to insulin, leading to insulin resistance.
In an attempt to cope with this overload, the liver may offload some of this fat by packaging it into very-low-density lipoproteins (VLDL) for transport. However, if these are not efficiently processed or utilized, this fat can accumulate in other organs, such as the pancreas. The presence of fat within the pancreas can be toxic to the insulin-producing beta cells, leading to their dysfunction and eventual destruction. By the time type 2 diabetes is diagnosed, it is not uncommon for a significant proportion of these vital insulin-producing cells to have already been damaged or destroyed.
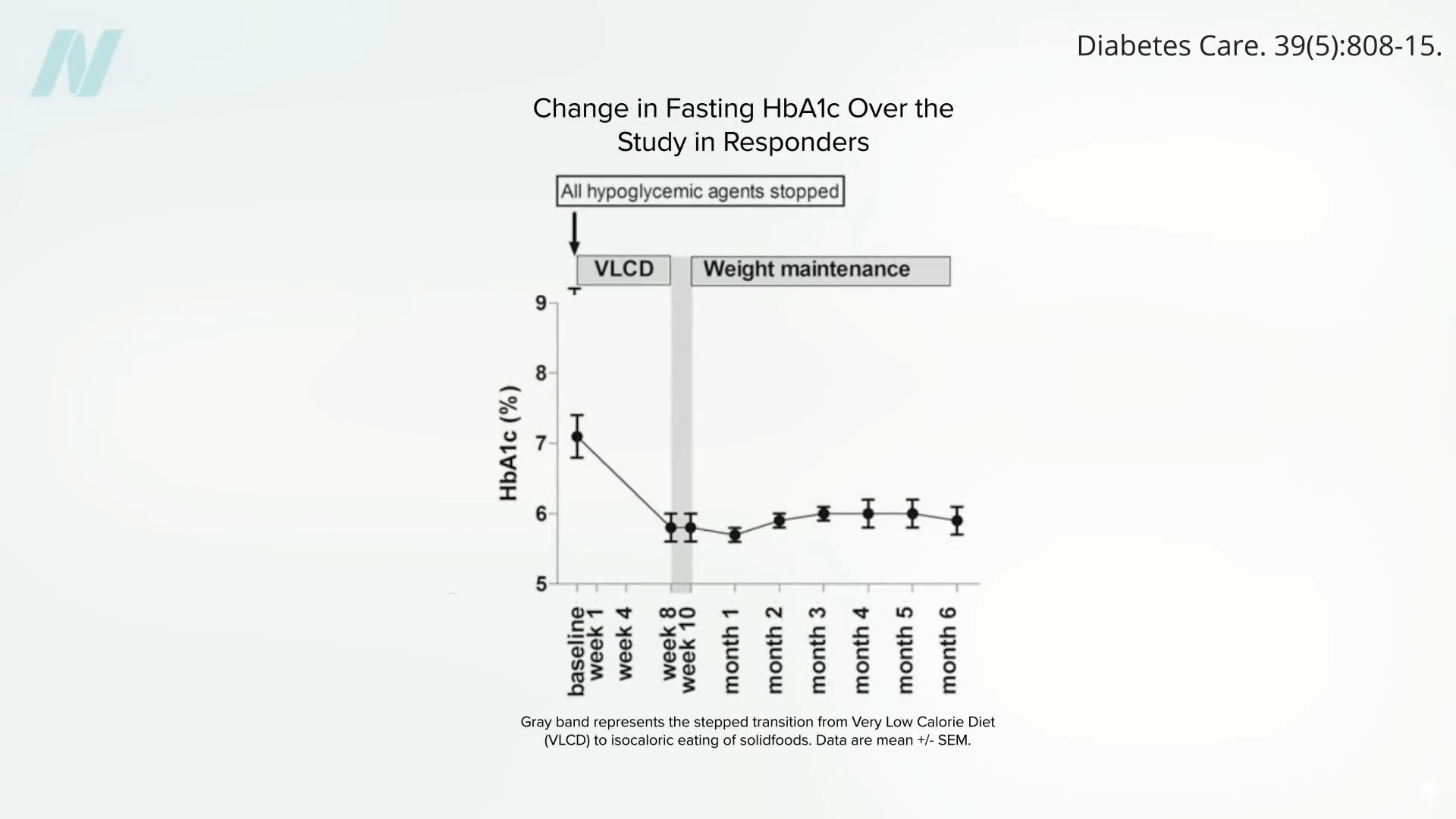
The research indicates that a sufficiently large caloric deficit, achieved through dietary interventions, can effectively reverse this pathological process. Within approximately seven days of a profound calorie deficit, a significant reduction in liver fat can be observed, leading to a rapid restoration of liver insulin sensitivity. Sustained caloric restriction for around eight weeks can further decrease liver fat to a level that helps normalize pancreatic fat content and function. Once an individual drops below their personal fat threshold, their body becomes more efficient at managing fat storage, potentially allowing them to resume a normal caloric intake while maintaining diabetes remission.
Long-Term Remission Rates: Diet vs. Surgery
The implications of these findings extend to the long-term sustainability of diabetes remission. While bariatric surgery has historically shown impressive remission rates, especially in the short to medium term, the evidence suggests that sustained weight loss through diet alone can also achieve significant and lasting benefits.
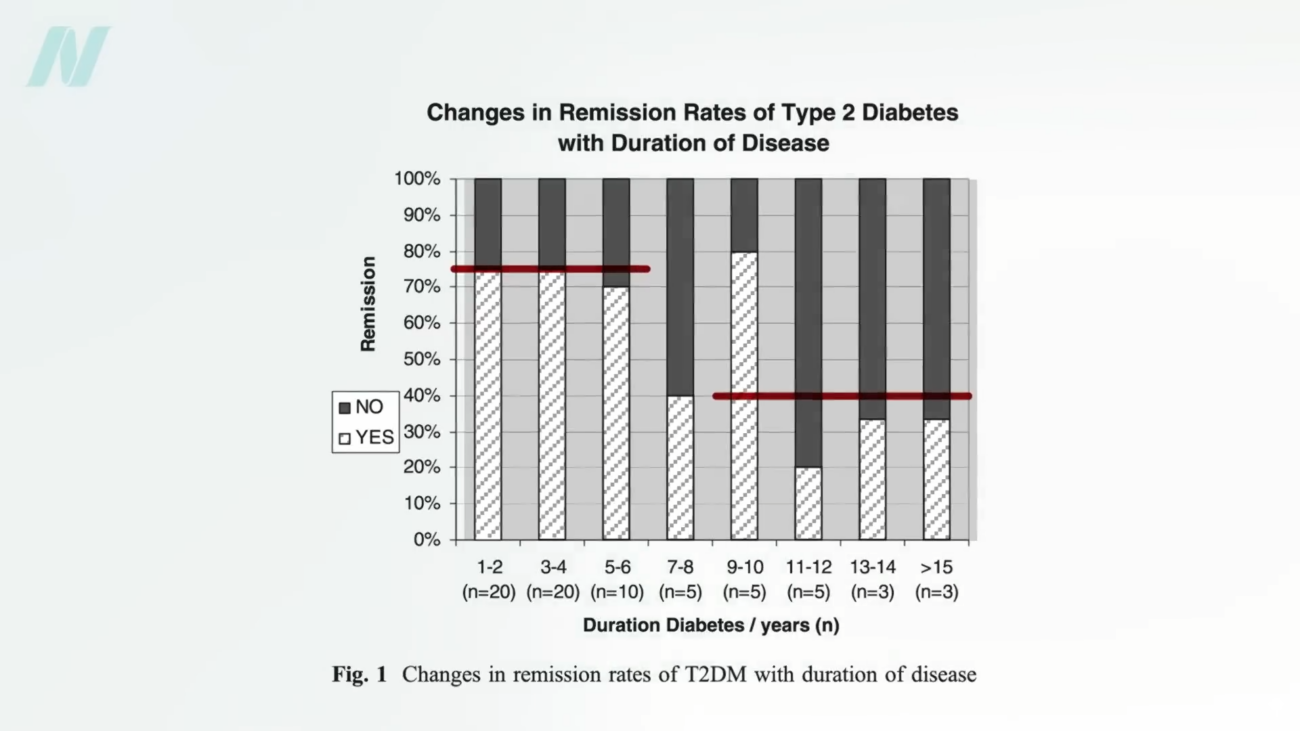
For individuals who have had type 2 diabetes for less than four years, losing approximately 30 pounds (13.6 kilograms) through dietary changes alone can lead to non-diabetic blood sugar levels in nearly 90% of cases, indicating a high likelihood of remission. However, for those who have lived with diabetes for eight years or longer, the success rate for remission through diet alone drops to around 50%.
When comparing these outcomes with bariatric surgery, the picture becomes more nuanced. While surgery can achieve remission in about 75% of individuals with diabetes of up to six years’ duration, this figure declines to approximately 40% for those who have had the disease for longer periods. This suggests that while surgery can be highly effective, particularly for those with less established diabetes, the duration of the disease plays a significant role in the potential for remission, regardless of the intervention method. Crucially, the comparative study indicated that the weight loss achieved through diet alone in the study participants resulted in metabolic improvements that were, in some respects, superior to those seen after surgery.
Broader Health Implications: Inflammation and Complications
Beyond blood sugar control, weight loss through diet alone may offer additional advantages in managing systemic inflammation, a known contributor to various chronic diseases. Studies have shown that individuals with diabetes who lose weight through dietary changes can significantly improve markers of systemic inflammation, such as tumor necrosis factor. In contrast, when a similar amount of weight is lost through bariatric surgery, these inflammatory markers have been observed to worsen. This finding suggests that the quality of weight loss, influenced by dietary composition, might be as important as the quantity.
Furthermore, the impact of these interventions on long-term diabetic complications warrants careful consideration. While reversing diabetes through bariatric surgery can improve kidney function, evidence suggests it may not necessarily prevent the onset or progression of diabetic vision loss. This could be attributed to the fact that surgery primarily addresses the quantity of food consumed rather than the quality of the diet itself. This observation echoes findings from large-scale studies, such as one published in The New England Journal of Medicine, which randomized thousands of individuals with diabetes to an intensive lifestyle program focused on weight loss. While this program led to significant weight reduction, it did not demonstrate a reduction in mortality or heart attacks over ten years. Researchers hypothesized that this might be because participants, while eating less, were still consuming the same heart-clogging dietary patterns.
Conclusion: A Balanced Perspective on Weight Management and Diabetes
The ongoing discourse surrounding bariatric surgery highlights a critical need to differentiate between the effects of surgical intervention and the impact of the stringent dietary regimens that are inextricably linked to these procedures. While bariatric surgery has demonstrated undeniable success in facilitating weight loss and achieving diabetes remission for many individuals, emerging research strongly suggests that significant portions of these metabolic improvements may be attributable to severe caloric restriction.
The study comparing caloric restriction with and without surgery provides compelling evidence that dietary intervention alone can yield substantial benefits for type 2 diabetes, potentially even surpassing surgical outcomes in certain metabolic markers. This underscores the profound power of diet in reversing the underlying mechanisms of type 2 diabetes, particularly by reducing liver and pancreatic fat.
As the medical community continues to refine its understanding of metabolic diseases, a balanced approach that emphasizes evidence-based strategies for sustainable weight loss through diet is paramount. For individuals with type 2 diabetes, especially those diagnosed early in the disease progression, a well-structured dietary intervention may offer a viable, less invasive path to remission, potentially with broader health benefits than previously recognized. Continued research is essential to further clarify the distinct contributions of surgical anatomy and dietary quality to long-term health outcomes and to empower patients with the most effective and personalized treatment strategies.
This article is the third in a four-part series exploring the nuances of bariatric surgery. Previous installments include "The Mortality Rate of Bariatric Weight-Loss Surgery" and "The Complications of Bariatric Weight-Loss Surgery." For further insights into sustainable weight loss strategies, readers are encouraged to consult resources such as the book "How Not to Diet," which focuses exclusively on evidence-based approaches to achieving and maintaining a healthy weight.