The pursuit of rapid and significant weight loss has, throughout history, driven individuals to explore an array of methods, some bordering on the extreme and ethically questionable. While the allure of a quick fix is potent, a closer examination of these unconventional approaches reveals a landscape fraught with potential dangers, questionable efficacy, and a stark contrast to scientifically validated, sustainable weight management strategies. This article delves into a spectrum of these methods, from invasive surgical interventions and ingeniously designed devices to historical curiosities and even the unsettling incorporation of biological organisms, critically assessing their safety, effectiveness, and the underlying science, or lack thereof.
The Caloric Imbalance: A Foundation for Extreme Measures
Understanding the fundamental principle of weight management—the caloric balance—is crucial to contextualizing the appeal of drastic measures. The human body functions on a delicate equilibrium of energy intake and expenditure. For individuals seeking to lose weight, this typically involves reducing calorie consumption and increasing calorie expenditure. However, the modern food environment presents a significant challenge to this balance. A moderately obese individual engaging in moderate physical activity, such as brisk walking or cycling, might burn approximately 350 calories per hour. In stark contrast, the consumption of calorie-dense, processed foods and sugary beverages can easily negate these efforts. A mere five minutes spent consuming snacks or drinks averaging 70 calories per minute can entirely offset an hour of strenuous exercise, highlighting the sheer scale of the caloric deficit required for meaningful weight loss through conventional means. This overwhelming disparity often fuels the search for more potent, albeit riskier, solutions.
The AspireAssist Siphon: A Direct Approach to Calorie Removal
One of the more technologically driven and invasive methods to emerge in recent years is the AspireAssist siphon system. This device represents a radical departure from traditional weight-loss interventions. It involves a surgical procedure to create a percutaneous gastrostomy, essentially a surgically created opening in the stomach wall. From this opening, a fistula is tunneled through the abdominal wall, allowing for direct access to the stomach.
Mechanism of Action and Ethical Considerations
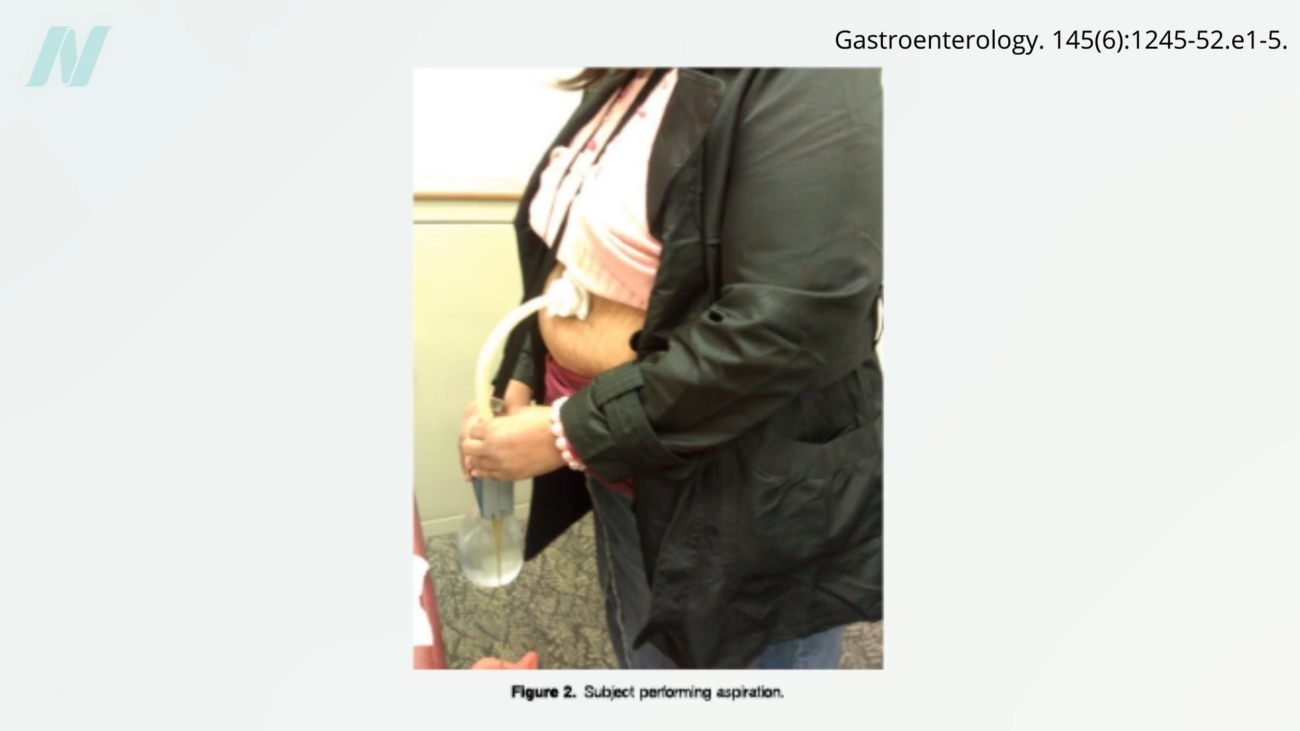
The AspireAssist system functions by enabling individuals to attach a portable suction device to the gastric port after consuming a meal. This device then drains a significant portion of the stomach’s contents—typically 20 to 30 percent—directly into a disposal bag. The stated purpose is to reduce the number of calories absorbed by the body. Proponents argue that this method allows individuals to consume food and then physically remove it, bypassing the typical digestive process and calorie absorption.
The implications of such a device are profound and raise significant ethical and psychological questions. The ability to "gorge on donuts, spew them out through the hole in your stomach, then gorge on more donuts" paints a disturbing picture of a potential cycle of disordered eating. While the device facilitates weight loss, it does so by essentially creating a mechanism for purging consumed food, a behavior historically associated with severe eating disorders like bulimia nervosa.
Clinical Outcomes and Patient Experiences
Clinical studies have indicated that patients using the AspireAssist system do experience weight loss. Several contributing factors are believed to be at play beyond the direct removal of calories. The presence of the gastric fistula may interfere with the stomach’s natural relaxation response during eating, potentially leading to earlier feelings of fullness. Furthermore, the protocol for using the AspireAssist requires patients to drink substantial amounts of water and chew their food thoroughly, both of which can contribute to satiety and slow the eating process. Perhaps more significantly, patients often report a psychological shift: the unpleasant visual of gastric aspirate from unhealthy foods, such as fried items appearing particularly unappetizing when pumped out, can motivate individuals to make healthier dietary choices to avoid the unappealing sight.
However, the system is not without its drawbacks and potential complications. Patients are required to supplement their diet with potassium, as it is leached out in the stomach juices, risking deficiency. While serious adverse effects like abdominal abscesses are reported as rare, minor wound complications are more common. The primary "selling point" often cited is that the siphon device does not alter the fundamental anatomy of the gastrointestinal tract, a distinction that, in the current landscape of weight-loss procedures, is presented as a significant advantage.
The Duodenal-Jejunal Bypass Liner: A Less Invasive Surgical Alternative?
Another intervention that bypasses significant portions of the digestive tract without major surgery is the duodenal-jejunal bypass liner, often referred to by its brand name, EndoBarrier. Traditional gastric bypass surgery involves physically altering the digestive system by removing or bypassing parts of the stomach and small intestine to reduce calorie absorption. The EndoBarrier offers a less surgically intensive approach by inserting a flexible tube, approximately two feet in length, that lines the duodenal and jejunal walls of the small intestine.
Mechanism and Risks
The intention behind the EndoBarrier is to create a physical barrier that prevents food from coming into direct contact with the intestinal lining, thereby inhibiting calorie and nutrient absorption. While this approach avoids the extensive anatomical changes of gastric bypass surgery, it introduces its own set of significant risks. The liner must be anchored within the digestive tract, a process that typically involves the use of ten barbed hooks. These hooks are designed to secure the device but are responsible for the majority of reported adverse effects. In a study involving 1,056 patients, nearly 90% experienced adverse events, primarily due to lacerations caused by the anchoring hooks. More severe complications, such as esophageal perforation or liver abscesses, though rarer, have been reported in approximately 1 in 27 patients, highlighting the substantial risks associated with this seemingly less invasive procedure.
Intestinal Resurfacing: A Radical Approach to Nutrient Absorption
Pushing the boundaries of intervention even further, the concept of "intestinal resurfacing" emerges as a particularly alarming prospect. While the EndoBarrier lines the intestine, resurfacing involves a more aggressive alteration of the intestinal lining itself. The described procedure, "thermally ablating the superficial duodenal mucosa," essentially means burning off the superficial layer of the intestinal lining. The intent is to reduce the capacity of the intestine to absorb nutrients. This method, euphemistically termed "resurfacing," involves intentionally damaging the delicate intestinal tissue, raising serious concerns about long-term digestive health, nutrient absorption, and the potential for irreversible harm.
The Era of Botulinum Toxin and Corsetry: Questionable Non-Invasive Methods
Beyond the realm of invasive devices and surgical alterations, researchers have explored less conventional, seemingly non-invasive methods, often with disappointing results.

Botox Injections: A Misguided Application
In an attempt to leverage the muscle-paralyzing properties of Botulinum toxin (Botox), some researchers have explored injecting it into the stomach walls of obese individuals. The hypothesis was that partially paralyzing the gastric muscles would slow stomach emptying, induce a prolonged feeling of fullness, and consequently lead to weight loss. However, clinical trials have demonstrated that this approach is ineffective. The physiological mechanisms governing satiety and gastric emptying are complex, and the localized application of Botox in this manner failed to achieve the desired weight-loss outcomes.
Corsets: A Return to Victorian Methods
In a study conducted in Sweden, researchers investigated the efficacy of wearing corsets for extended periods—12 to 16 hours a day, seven days a week, for nine months. The rationale behind this approach, while not explicitly detailed in the original abstract, likely stemmed from the historical perception that corsets physically restrict the stomach and abdomen, leading to reduced food intake. The study’s findings were predictably negative. Participants found the corsets to be uncomfortable and largely failed to adhere to the prescribed wearing schedule, rendering the intervention ineffective. This underscores a fundamental challenge in many weight-loss strategies: the need for sustained compliance, which is often hampered by discomfort or impracticality.
The Tapeworm Diet: A Perilous Parasitic Solution
Historically, one of the most notorious and dangerous weight-loss fads has been the "tapeworm diet." Advertised since the early 1900s, this method involved intentionally ingesting tapeworm eggs or larvae with the belief that the parasites would reside in the digestive tract, consuming a portion of the ingested food and thus reducing the host’s calorie intake.
Biological Hazards and Lack of Efficacy
The scientific community unequivocally condemns this practice due to its extreme health risks. Tapeworms, once established in the human body, can grow to several feet in length and can migrate to various organs, including the brain, liver, and lungs, causing severe and potentially fatal organ damage. The ingestion of "sanitized tapeworm cysts" was a dubious claim, as the parasites are inherently dangerous. Evidence suggesting the presence of live tapeworms discovered during bariatric surgery operations further indicates that this method is not only ineffective but poses a grave threat to human health.
Harnessing Disgust: A Psychological Approach to Appetite Control
In a more recent and psychologically driven approach, researchers have explored the power of disgust to curb cravings for unhealthy foods. A study titled "Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming" investigated the use of subliminal messaging to alter food preferences.
The Science of Subliminal Priming
The experimental design involved briefly flashing positive images (e.g., kittens) before presenting images of healthy foods, aiming to create a positive association. Conversely, before displaying images of high-calorie foods like ice cream, researchers flashed negative, aversive scenes such as a cockroach on pizza, vomit, or a burn wound. These negative images were presented for mere milliseconds, too short for conscious recognition but intended to trigger an implicit sense of revulsion.
Promising Results and Future Implications
The results of this study suggested that this technique could be effective. Participants reported a reduced desire to consume high-calorie foods after the priming sessions, although direct testing of actual food consumption was not conducted. The researchers concluded that subliminal aversion could be a viable tactic to combat the pervasive influence of food cues that promote unhealthy eating habits. This approach, while not directly altering the body’s physiology, taps into the brain’s associative learning mechanisms, offering a novel, albeit still experimental, avenue for appetite management.
International Perspectives on American Weight-Loss Innovations
The often unconventional and sometimes extreme nature of weight-loss pursuits in the United States has not gone unnoticed by the global medical and scientific community. Commentaries and academic papers have emerged from across the Atlantic, expressing bewilderment and critical analysis of these American "machinations." A paper published in the journal Obesity Surgery, provocatively titled "What Are the Yanks Doing?", reviewed the U.S. experience with implantable gastric stimulation. This involved inserting electrodes into the muscular layer of the stomach wall, a technique that ultimately proved unsuccessful. Following this, attempts were made with colon electrical stimulation, further illustrating a pattern of exploring invasive electrical interventions with limited success.
Brain Stimulation: The Ultimate Frontier of Appetite Control
Perhaps the most audacious and concerning area of research has been the exploration of direct brain stimulation for appetite control. Studies have investigated "Repetitive electric brain stimulation" as a means to reduce food intake in humans. Despite the inherent risks associated with deep-brain electrode implantation, which is considered a complication-prone operation, scientists have long pondered whether direct intervention in the brain could effectively reduce food consumption.
Experimental Procedures and Unfulfilled Promises
In one notable series of experiments, holes were drilled through the skulls of obese individuals, and wires were inserted into their brains for "electrostimulatory exploration." The objective was to identify specific brain regions that, when stimulated, could elicit hunger responses. Once these spots were located, researchers delivered electrical currents to create electro-coagulatory lesions, essentially burning out targeted areas of brain tissue. While similar techniques had shown some promise in animal models, such as cats and monkeys, the researchers found that this invasive procedure did not result in significant weight loss in obese human subjects. The profound ethical implications and the lack of efficacy render this approach a stark reminder of the dangers of pursuing extreme interventions without robust scientific validation.
The Path Forward: Sustainable Weight Management
The overwhelming narrative emerging from the examination of these extreme weight-loss methods is one of high risk, questionable efficacy, and a fundamental disconnect from established principles of health and nutrition. While the desire for rapid weight loss is understandable, the pursuit of such goals through invasive surgery, dangerous devices, parasitic infestations, or direct brain manipulation carries severe consequences.
As articulated in comprehensive works on the subject, such as Dr. Greger’s book How Not to Diet, truly sustainable and healthy weight loss is not a matter of complex surgical procedures or extreme physiological manipulation. It is, instead, rooted in consistent, evidence-based dietary habits, regular physical activity, and a holistic approach to well-being. The focus must shift from quick fixes to long-term lifestyle changes that prioritize health over rapid, and often unsustainable, weight reduction. The exploration of less invasive alternatives, such as gastric balloon surgery and various weight-loss medications, also warrants careful consideration, with a thorough understanding of their respective safety profiles and effectiveness, as detailed in supplementary medical resources. Ultimately, the journey to a healthier weight is best navigated through informed choices and a commitment to sustainable practices, rather than succumbing to the allure of the extreme.