The global health landscape is grappling with an escalating crisis of diabetes, with current projections indicating a substantial rise in adult cases over the next generation. Amidst this challenge, a significant breakthrough in understanding and potentially reversing Type 2 diabetes has emerged, centered on the potent impact of weight loss. Emerging research suggests that achieving remission of Type 2 diabetes is attainable for a vast majority of individuals diagnosed within the last four years, provided they achieve a modest 15% reduction in their body weight. This finding offers a beacon of hope and a paradigm shift in how this chronic condition is managed and perceived.
The sheer scale of the diabetes epidemic cannot be overstated. More than half a billion adults worldwide currently live with diabetes, a number projected to surge by approximately 50% in the coming decades. This burgeoning crisis places an immense strain on healthcare systems and profoundly impacts the quality of life for millions. While extensive research has focused on various dietary interventions, the latest insights point towards a more fundamental approach: addressing the root cause of excess weight and its metabolic consequences.
Historical Perspectives on Fasting and Diabetes
The notion that profound dietary restriction, including fasting, could combat diabetes is not a new one. Historical accounts reveal that over a century ago, fasting was recognized for its potential to rapidly halt the progression of diabetes and, in some instances, eliminate its symptoms within days or weeks. While the extreme application of such methods, akin to starvation, poses inherent dangers and is unsustainable, these early observations laid a groundwork for understanding the body’s response to calorie restriction. The critical question that has long lingered is whether the weight lost through drastic measures can be maintained and whether the underlying metabolic dysfunction can be truly reversed, rather than temporarily suppressed.
The historical understanding of Type 2 diabetes has long been intertwined with the concept of "excess." It was once considered a disease primarily affecting the affluent, those whose lifestyles afforded them the luxury of overconsumption without the necessity of strenuous physical activity. This perspective, however, overlooks the complex interplay of genetic predisposition, environmental factors, and lifestyle choices that contribute to its development. The preventable nature of diabetes, coupled with its increasing prevalence, naturally leads to the question of its treatability. If overeating contributes to its onset, could strategic undereating offer a path to recovery?
Ancient texts offer intriguing parallels to modern approaches. An Ayurvedic text, dating back approximately 2,000 years, proposed a regimen for individuals with diabetes that included extreme physical exertion or severe dietary restriction, even humorously suggesting consumption of cow dung and urine as a last resort. While these historical recommendations are stark and unscientific by today’s standards, they underscore a persistent recognition of the link between caloric intake, physical activity, and diabetes management.
Later, in 1797, Dr. John Rollo proposed a diet for diabetes that, while extreme, reflected an understanding that making patients sick could reduce food intake and thus alleviate symptoms. His regimen, which included rancid meat and emetics to induce vomiting, aimed to decrease food consumption. The unintended consequence of such harsh methods was a reduction in calorie intake, which temporarily lessened diabetic symptoms. This historical anecdote highlights a recurring theme: the direct correlation between reduced food intake and improved diabetic control, even when achieved through medically questionable means.
The siege of Paris during the Franco-Prussian War inadvertently provided further evidence for this connection. During this period of extreme scarcity, individuals with diabetes experienced improvements in their condition. This led to the popular advice of "mangez le moins possible" – "eat as little as possible." This principle was later formalized into the "Allen starvation treatment," developed by Dr. Frederick M. Allen. For a period, the Allen treatment was considered a significant advancement in diabetes management before the advent of insulin.
The Dawn of Insulin and the Legacy of the Allen Treatment
The discovery of insulin in 1921 revolutionized diabetes care, offering a life-saving intervention, particularly for those with Type 1 diabetes. However, its impact on Type 2 diabetes management was more nuanced. While insulin could manage blood glucose levels, it did not inherently address the underlying metabolic issues that led to the disease. The initial euphoria surrounding insulin’s discovery gradually gave way to the realization that it was not a panacea for Type 2 diabetes. Complications such as blindness, kidney failure, stroke, and amputations continued to affect individuals with Type 2 diabetes, even when their blood sugar was controlled with insulin.
Dr. Frederick M. Allen, a prominent figure in the pre-insulin era, observed that severe diabetes cases sometimes resolved following the onset of wasting illnesses like tuberculosis or cancer. This observation led him to investigate the therapeutic potential of severe caloric restriction. His research demonstrated that even in the most severe forms of diabetes, he could achieve the clearance of sugar from urine within ten days through strict dietary control. Allen’s approach centered on two core principles: maintaining a low body weight and restricting dietary fat. He noted that even small amounts of fat, such as butter or olive oil, could trigger a resurgence of diabetic symptoms in patients who had temporarily achieved symptom-free status. This highlighted a critical insight: fat intake played a significant role in the manifestation and persistence of diabetes.

This historical context is crucial for understanding the contemporary research. The early recognition of the link between excess and diabetes, the historical use of severe dietary restriction, and the understanding of fat’s role in exacerbating the condition all converge in current scientific investigations.
Type 2 Diabetes: A Disease of Fat Toxicity
Modern scientific inquiry has solidified the understanding that Type 2 diabetes is, in essence, a disease of "fat toxicity." Research utilizing advanced imaging techniques, such as high-tech MRI scanners, has provided compelling evidence of this phenomenon. By infusing fat into the veins of individuals or placing them on high-fat diets for even short periods, scientists have observed a rapid accumulation of fat within muscle cells. This intracellular fat buildup is directly correlated with an increase in insulin resistance. The body’s cells become less responsive to insulin, the hormone responsible for regulating blood glucose.
The speed at which this occurs is remarkable. Studies have shown that insulin resistance can increase within hours of fat infusion, within three days of a high-fat diet, and even after a single high-fat meal. This acute dietary fat intake has a rapid and detrimental effect on insulin sensitivity. The implications of this are profound: when muscle cells become insulin resistant in the context of excessive calorie intake, the liver begins to store excess fat. This hepatic fat accumulation can then lead to fat accumulation in the pancreas, ultimately culminating in the full manifestation of Type 2 diabetes.
As one prominent study suggests, Type 2 diabetes can now be understood as a condition characterized by an excess of fat in the liver and pancreas. Crucially, this condition remains reversible for at least ten years in most individuals, offering a window of opportunity for intervention.
The Power of Weight Loss and Caloric Restriction
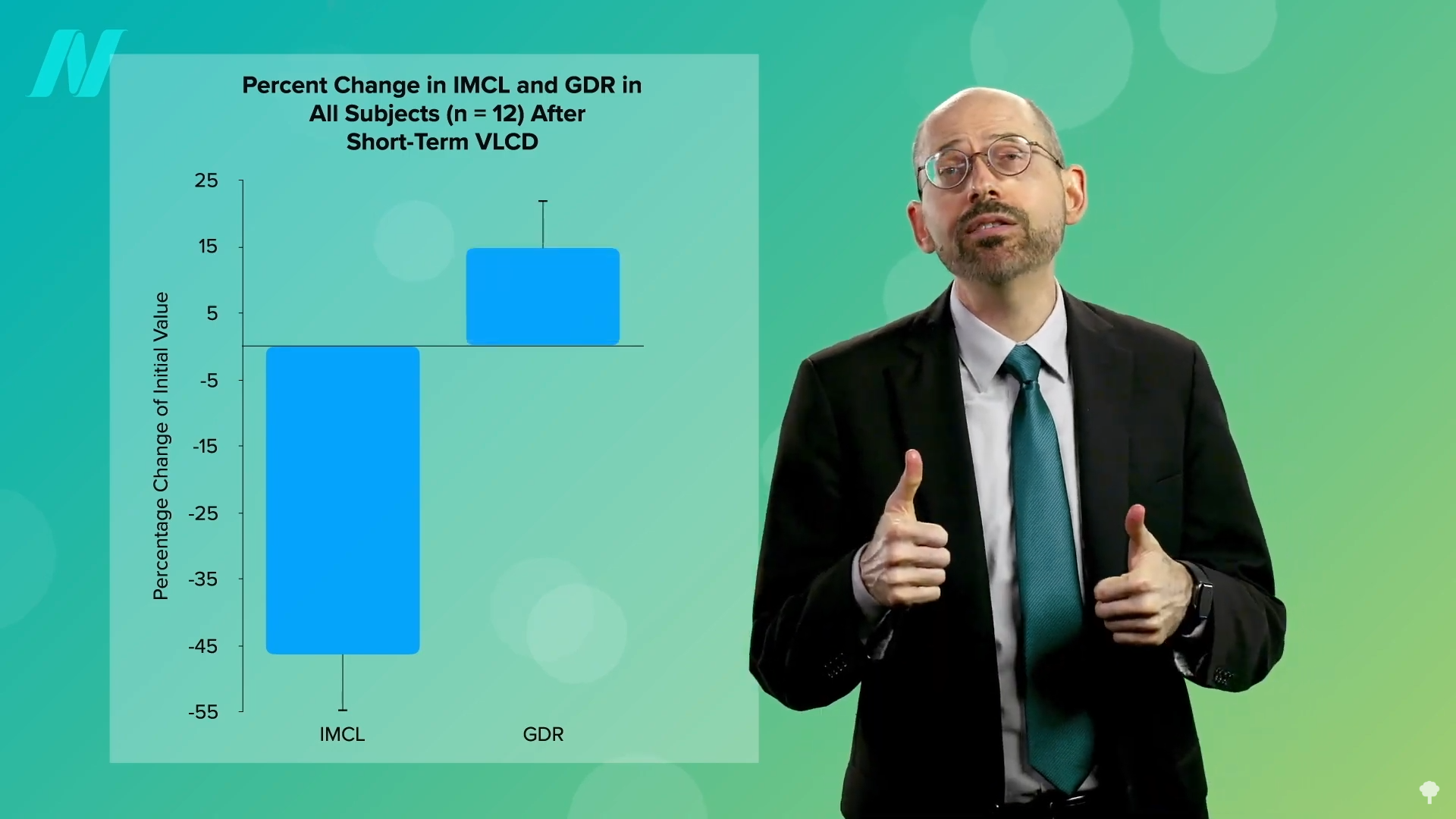
The reversal of Type 2 diabetes is intricately linked to the reduction of excess fat within the body, particularly in the liver and pancreas. When individuals are placed on very low-calorie diets, typically around 700 calories per day, a significant shift occurs. Fat is mobilized and removed from muscle cells, leading to a corresponding enhancement in insulin sensitivity. This process, visualized through scientific studies, demonstrates the body’s capacity to regain metabolic health when the burden of excess fat is reduced.
The subsequent reduction in liver fat is a critical step. If the dietary intervention is sustained, the excess fat within the pancreas also diminishes. This reduction in pancreatic fat is believed to be a key factor in restoring insulin production and improving insulin signaling. For individuals diagnosed with Type 2 diabetes, particularly in its earlier stages, this metabolic reset can lead to sustained healthy blood sugar levels without the need for medication.
Achieving Remission: The 15% Weight Loss Threshold
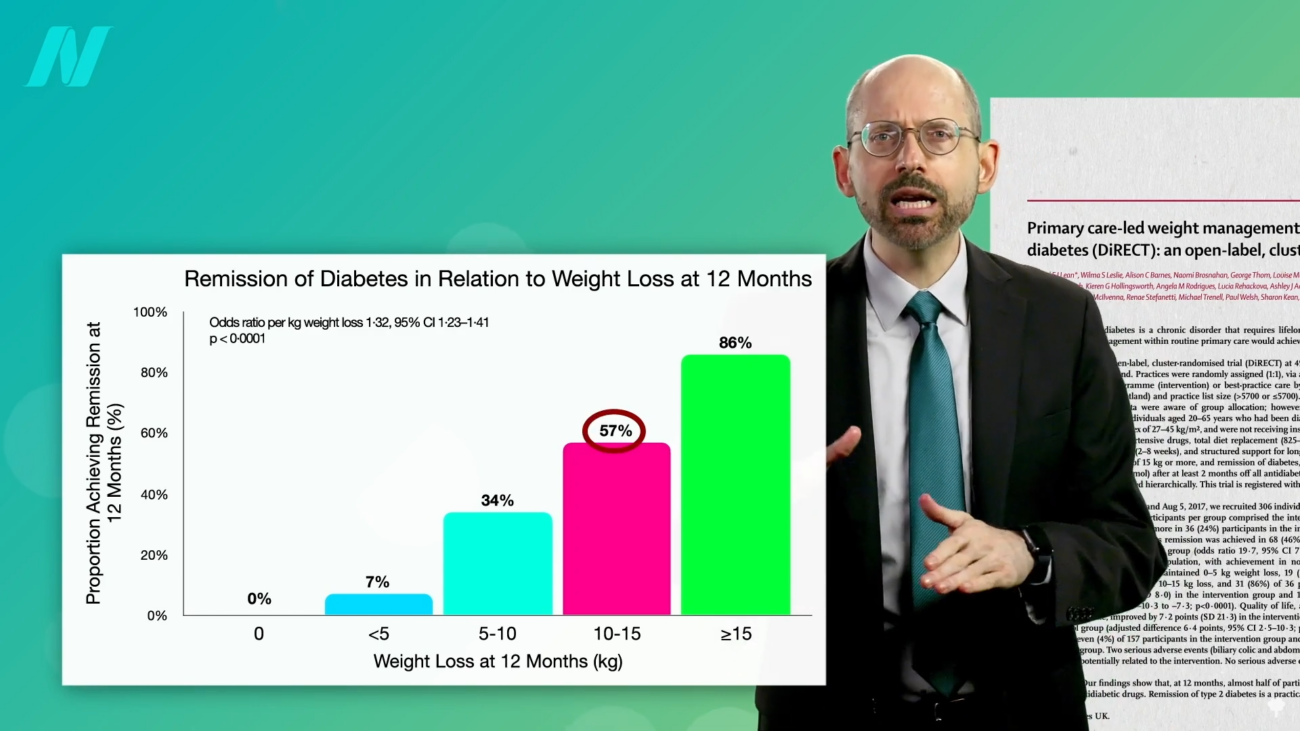
The breakthrough finding that underpins much of the current optimism is the correlation between weight loss and diabetes remission. Research indicates that individuals who have had Type 2 diabetes for less than four years and achieve a 15% reduction in their body weight have a remarkable success rate in achieving remission. For this group, nearly 90% can attain non-diabetic blood sugar levels. This means their bodies can regulate glucose effectively, mirroring the metabolic state of individuals without diabetes.
The implications of this finding are particularly significant when compared to other interventions. For instance, bariatric surgery, a more invasive procedure aimed at significant weight loss, has shown lower remission rates. Studies comparing the two interventions reveal that even with greater weight loss achieved through surgery, remission rates for Type 2 diabetes are considerably lower, approximately 62% for those losing more weight, compared to the 90% achieved through a 15% body weight reduction. This suggests that a less invasive, lifestyle-based approach can be more effective in achieving diabetes remission.
Furthermore, the duration of the disease plays a crucial role. For individuals who have lived with Type 2 diabetes for longer periods, the prognosis for remission becomes more challenging. While those with a diagnosis of less than four years show a nearly 90% remission rate with a 15% weight loss, the success rate drops to around 50% for individuals who have had the disease for more than eight years. This underscores the importance of early intervention and diagnosis.
Evidence suggests that for many, losing approximately 30 pounds can be sufficient to reverse Type 2 diabetes, especially when the diagnosis has been relatively recent, averaging around three years. This translates to a powerful message: lifestyle changes, particularly those focused on achieving and maintaining a healthy weight, can be more effective than surgical interventions in many cases. The adage of "your forks are better than surgeons’ knives" gains significant traction in this context.
Sustaining Remission: The Importance of Long-Term Lifestyle Changes
While achieving remission is a significant milestone, the long-term management of Type 2 diabetes requires sustained commitment to healthy lifestyle choices. The body’s capacity to regain metabolic health is dependent on maintaining the weight loss achieved. Historical observations and contemporary research both concur on a critical point: weight regain often leads to the re-emergence of diabetes.
Extended periods of physician-supervised, water-only fasting have been shown to facilitate significant weight loss and can lead to diabetes remission. However, the key to sustained remission lies in the individual’s ability to maintain this weight loss through ongoing healthy eating habits and regular physical activity. The metabolic improvements observed during fasting periods must be translated into sustainable lifestyle changes to prevent the recurrence of the disease.
The emphasis on diet and exercise as central pillars of diabetes management, as advocated by pioneers like Elliott Joslin, remains profoundly relevant today. Even with the advent of life-saving medications like insulin, the fundamental principles of a healthy lifestyle are paramount for preventing long-term complications and achieving lasting remission in Type 2 diabetes.
Broader Implications and Future Directions
The findings regarding weight loss and Type 2 diabetes remission have profound implications for public health strategies, clinical practice, and individual patient empowerment.
1. Shifting Treatment Paradigms: The research challenges the traditional view of Type 2 diabetes as an irreversible, progressive condition. It highlights the potential for reversal through lifestyle modifications, shifting the focus from solely managing symptoms to addressing the root metabolic causes. This could lead to a greater emphasis on weight management programs, nutritional counseling, and behavioral interventions in diabetes care.
2. Patient Empowerment: Understanding that significant weight loss can lead to remission empowers individuals with Type 2 diabetes to take an active role in their health. It offers a tangible goal and a clear pathway towards regaining control over their metabolic health, moving beyond a passive reliance on medication.
3. Public Health Initiatives: The global diabetes epidemic necessitates scalable and effective interventions. The 15% weight loss threshold for remission suggests that accessible and sustainable weight management strategies could have a substantial impact on reducing the burden of Type 2 diabetes worldwide. Public health campaigns could focus on promoting healthy eating habits, increasing physical activity, and raising awareness about the reversibility of the disease.
4. Research and Development: Continued research is vital to further elucidate the precise mechanisms by which weight loss impacts pancreatic and hepatic fat accumulation. Understanding these pathways could lead to the development of targeted therapies and more personalized treatment approaches. Further investigation into the optimal duration and composition of dietary interventions for sustained remission is also warranted.
5. Addressing Health Disparities: The rising prevalence of Type 2 diabetes disproportionately affects certain socioeconomic and ethnic groups. Future research and interventions must consider these disparities to ensure that the benefits of weight loss-driven remission are accessible to all populations.
In conclusion, the scientific evidence strongly suggests that Type 2 diabetes, when diagnosed within its earlier stages, is a highly reversible condition. Achieving a modest yet significant weight loss of 15% of body weight can lead to remission for a vast majority of individuals. This understanding marks a pivotal moment in diabetes management, offering a hopeful and actionable path towards reclaiming metabolic health and mitigating the global impact of this pervasive disease. The journey from diagnosis to remission is increasingly viewed not as an endpoint, but as a testament to the body’s remarkable capacity for healing when supported by appropriate lifestyle choices.