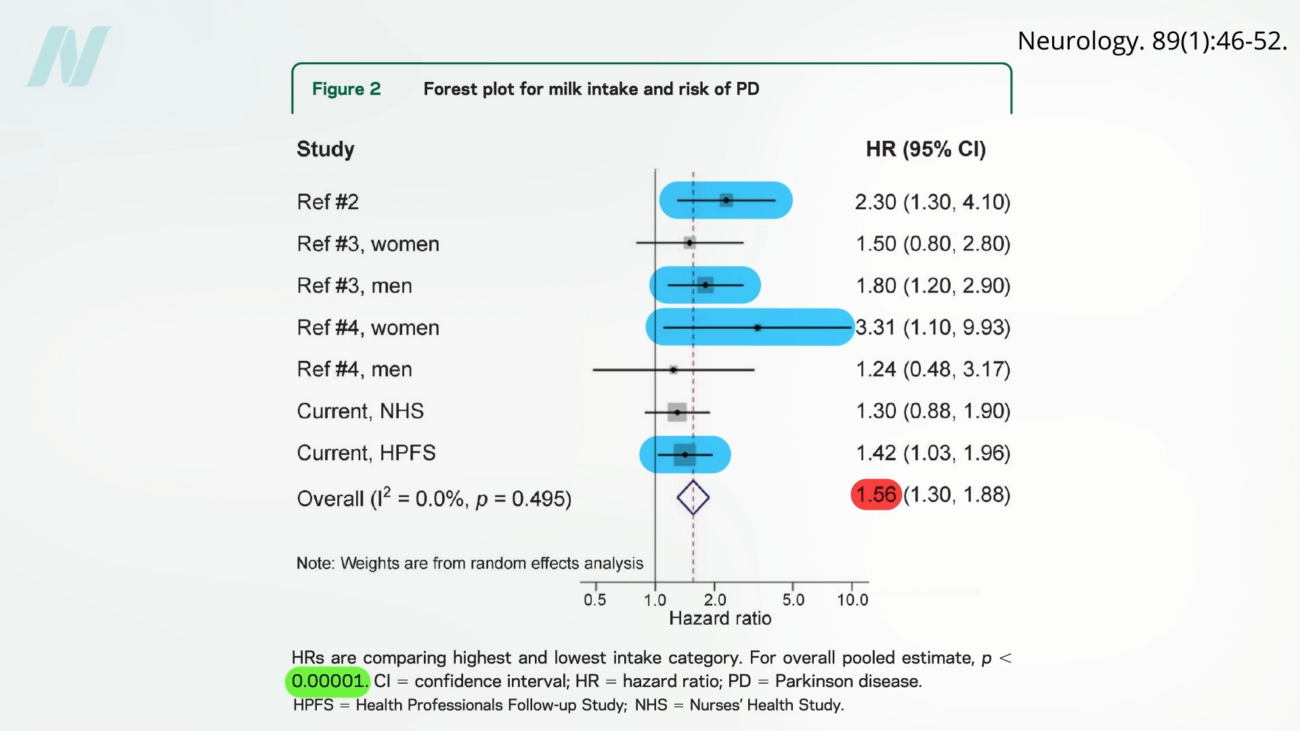
Parkinson’s disease is a relentless neurodegenerative disorder that impacts millions worldwide, characterized by the progressive loss of dopamine-producing neurons in the brain. While the exact genesis of this debilitating condition remains a complex puzzle, mounting scientific inquiry has consistently pointed to dairy consumption as a significant dietary factor associated with an elevated risk of developing Parkinson’s disease. Indeed, dairy products stand out as the only food group with a persistent and robust link to an increased likelihood of Parkinson’s. This association is not an isolated observation but has been corroborated by five extensive prospective studies, including the landmark Harvard cohorts: the Nurses’ Health Study and the Health Professionals Follow-up Study. These influential studies, collectively tracking over 100,000 individuals for decades, represent the most comprehensive analysis to date of dairy intake and Parkinson’s disease, meticulously examining more than 1,000 newly diagnosed cases. The findings across these studies have been remarkably consistent, revealing a link between dairy consumption and Parkinson’s disease, with a majority reporting a statistically significant association. On average, individuals who consumed the highest amounts of milk exhibited approximately a 50% increase in their risk of developing Parkinson’s compared to those who consumed the least. This level of statistical significance, evidenced by a p-value below 0.00001, indicates an extremely low probability that such an extreme finding could occur by random chance – less than a 1 in 100,000 likelihood.
The Search for a Causal Mechanism
Despite the clear and consistent epidemiological links between milk consumption and Parkinson’s disease incidence, the underlying biological mechanisms have long eluded definitive explanation. One review published a few years prior to a significant breakthrough noted, "Despite clear-cut associations between milk intake and incidence of Parkinson’s, there is no rational explanation." However, a pivotal study conducted a year later offered a crucial clue, with its title succinctly stating: "Midlife milk consumption and substantia nigra neuron density at death." This research delved into the direct impact of dairy intake on the very brain structures affected by Parkinson’s.
Parkinson’s disease is primarily driven by the degeneration of a specific type of nerve cell, known as dopaminergic neurons, located in a vital brain region called the substantia nigra. Symptoms of Parkinson’s typically manifest only after a substantial proportion of these critical neurons have already been lost. The study in question meticulously tracked the milk consumption habits of participants during their middle adult years – specifically their 40s, 50s, and 60s. Subsequently, upon the participants’ passing, their brains were examined through autopsy, and the density of these crucial substantia nigra neurons was quantified. The results were striking: across all examined brain quadrants, neuron density was consistently highest in individuals who had consumed no milk and lowest in those who had been the heaviest milk drinkers.
Even after excluding participants diagnosed with Parkinson’s disease, the correlation remained significant. Those who consumed approximately two cups (473 mL) of milk daily showed up to a 40% reduction in nerve cell density in most quadrants of this critical brain area. This observation raised a pressing question: what component within milk could be responsible for this observed neuronal depletion?
Unmasking the Suspects: Heptachlor Epoxide and Galactose
One compelling hypothesis emerged from the examination of brain tissue. Among the individuals who reported the highest milk consumption, residues of the banned pesticide, heptachlor epoxide, were found in an astonishing 9 out of 10 brains. Heptachlor, a potent organochlorine pesticide, was widely used in agriculture but was banned in many countries due to its environmental persistence and potential health risks. Its metabolite, heptachlor epoxide, is known to be toxic and can accumulate in fatty tissues, including the brain. The prevalence of these pesticide residues in the brains of heavy milk drinkers offered a plausible pathway through which milk consumption could be causally linked to an increased risk of Parkinson’s disease. The logic suggested that the milk itself might act as a vehicle for this neurotoxic substance, leading to the gradual destruction of dopaminergic neurons.
However, the scientific investigation into the milk-Parkinson’s link did not stop with pesticide residues. Another significant contender for explaining the observed brain damage has emerged: galactose, a simple sugar that is a fundamental component of lactose, the primary sugar found in milk. When lactose is consumed, it is broken down in the digestive system into glucose and galactose. Research has indicated that galactose plays a role in the aging process of the brain. In experimental settings, galactose has been used to induce aging-like changes in the brain.

The mechanism proposed is that ingested galactose is readily absorbed by the brain within a few hours. For doses exceeding 100 mg/kg of body weight, studies suggest that galactose can trigger pathological alterations within brain cells that bear a striking resemblance to those observed in Parkinson’s disease. This critical dose can be easily reached and surpassed by consuming just two glasses (473 mL) of milk per day, which are a primary dietary source of galactose. Notably, dopaminergic neurons, the very cells crucial for preventing Parkinson’s, appear to be particularly vulnerable to galactose-induced damage. This heightened susceptibility is attributed to their increased vulnerability to oxidative stress, a cellular process that galactose can exacerbate.
Galactose’s Broader Implications for Health
The potential role of galactose extends beyond just Parkinson’s disease, offering explanations for other observed health correlations with milk consumption. For instance, studies have linked higher milk intake with increased mortality rates. While saturated fat in dairy products might intuitively be blamed, this association has been observed even with skim milk, which is fat-free but still contains lactose and, consequently, galactose. This suggests that the impact of milk on mortality may be independent of its fat content.
The question then arises: can simply opting for lactose-free milk circumvent these risks? Products like Lactaid milk have the lactase enzyme added, which pre-breaks down lactose into glucose and galactose. However, this process simply shifts the breakdown of lactose from the gut to the carton. Therefore, individuals consuming these "lactose-free" alternatives are still ingesting the same amount of galactose. This may explain why increased milk intake in midlife has also been associated with a greater rate of cognitive decline. Researchers have extensively utilized D-galactose, a metabolic derivative of lactose, in animal models to simulate cognitive aging, primarily through inducing oxidative stress. Studies comparing individuals who rarely consume milk with those who drink more than one glass (237 mL) daily indicate a higher likelihood of experiencing a decline in global cognitive function among the latter group. This research underscores the potential neurotoxic effects of galactose, particularly on cognitive processes and neuronal health over time.
A Multifaceted Inquiry into Parkinson’s Etiology
The investigation into the precise cause of milk-related Parkinson’s risk is ongoing and multifaceted. While the presence of banned pesticides like heptachlor epoxide in the brains of heavy milk drinkers provides a compelling environmental contaminant explanation, the metabolic effects of galactose offer an intrinsic dietary factor hypothesis. Both pathways, though distinct, point towards milk consumption as a significant modifiable risk factor for a devastating neurological disease.
The implications of these findings are far-reaching. For individuals concerned about their risk of Parkinson’s disease, or those seeking to optimize their cognitive health, understanding these potential links is crucial. Public health recommendations and dietary guidelines may need to evolve to reflect the growing body of evidence linking dairy consumption to neurodegenerative outcomes. Further research is warranted to definitively disentangle the contributions of pesticides and galactose, and to explore potential interventions that could mitigate these risks.
The research into the connection between milk and Parkinson’s disease is a dynamic field. Earlier explorations, such as those documented in "Could Lactose Explain the Milk and Parkinson’s Disease Link?", laid the groundwork for understanding the role of lactose and its breakdown products. Additionally, other dietary factors, like uric acid levels, have also been investigated for their potential role in Parkinson’s pathology, as explored in "Parkinson’s Disease and the Uric Acid Sweet Spot," highlighting the complex interplay of various dietary components and their influence on neurological health.
The scientific community’s ongoing efforts to elucidate the mechanisms behind the milk-Parkinson’s link underscore the importance of a critical examination of our dietary habits and their long-term consequences for brain health. The persistent association, coupled with plausible biological explanations, necessitates continued scientific scrutiny and may eventually lead to significant shifts in public health messaging and individual dietary choices.